Clear Sky Science · en
A preliminary study on oral health status and unmet dental needs in patients with home-based psychiatric services
Why Teeth Matter When Mental Health Care Comes Home
For many people living with serious mental illness, getting to a dentist can be far harder than getting to a doctor. This study looks inside the homes—and mouths—of patients in Tokyo who receive psychiatric care at home, asking a simple but overlooked question: what is happening to their teeth and gums? The answer reveals hidden pain, infection risks, and financial pressures that rarely show up in routine mental health visits, but that can strongly affect comfort, nutrition, and quality of life.
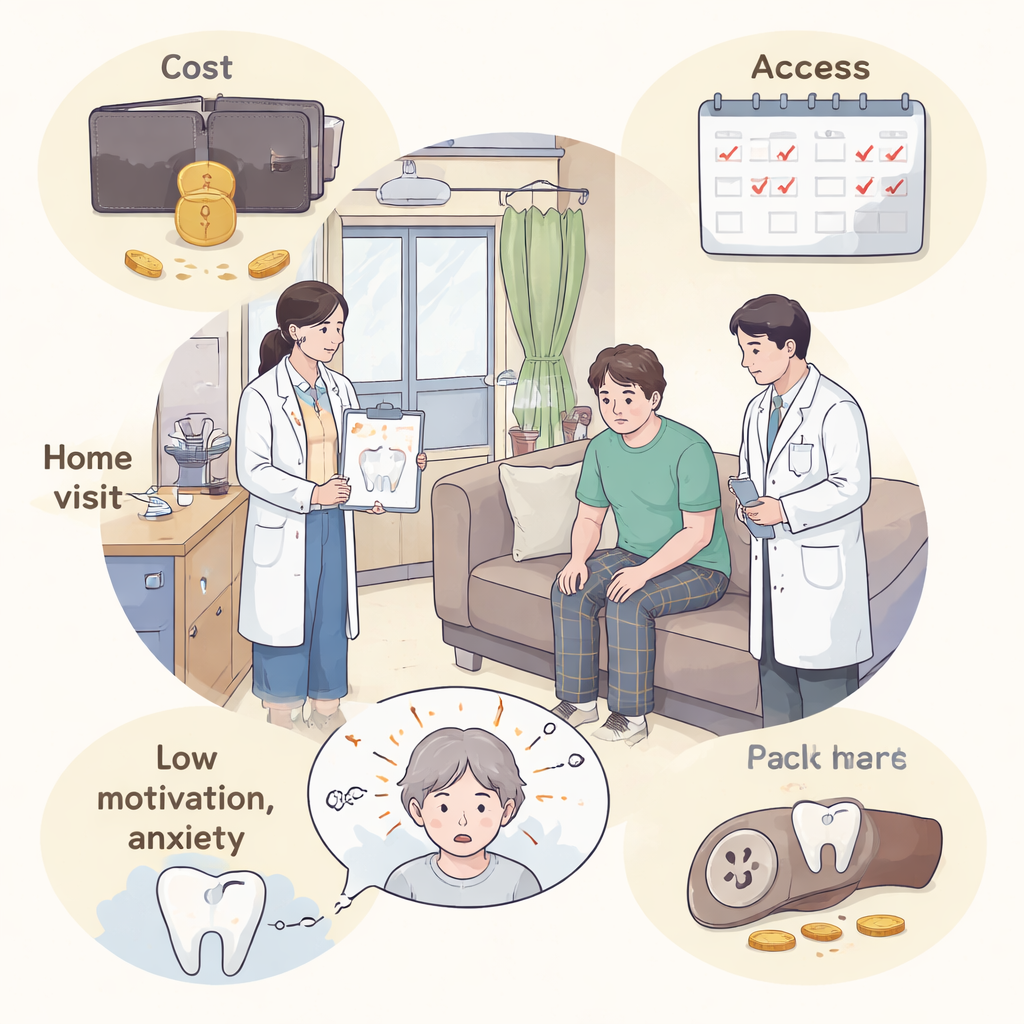
A Hidden Dental Problem Behind Closed Doors
The researchers visited 22 adults who were already receiving regular home-based psychiatric care from a community clinic in Tokyo. Instead of asking these patients to come to a dental office, a dentist joined the psychiatric team during routine home visits and carried out free oral examinations on the spot. The team recorded how many teeth each person had, how many were decayed, missing, or filled, and used several simple scoring tools to judge gum health, cleanliness, and tongue coating. They also reviewed the medical records to understand each person’s diagnosis, medications, living situation, smoking habits, and use of public assistance.
What the Dentist Saw at the Kitchen Table
On paper, these patients had about as many teeth as the average middle-aged Japanese adult. But the condition of those teeth was far worse. Many had multiple untreated cavities, severely decayed “residual roots” left in place instead of being removed, and thick layers of plaque and hardened tartar. Tongue and tooth-surface scores showed that roughly a third of patients had very poor oral hygiene. Compared with other groups—such as elderly people served by visiting nurses or patients treated for gum disease in hospitals—the home-based psychiatric group scored consistently worse on almost every oral health index the researchers used.
Money Worries, Low Energy, and Fear of the Chair
The study helps explain why these problems build up. Nearly seven in ten participants were living on public assistance, and many others had low or unstable income. In Japan, people on public assistance pay nothing for insured dental services, including home visits. Those who are not covered must pay a fee for each home dental visit—a cost some participants said they simply could not afford. One patient stopped treatment because of these charges, while another delayed care until finances improved. Beyond money, many participants had not seen a dentist in years, and more than 40% only agreed to an exam because a family member or psychiatrist pushed for it. The symptoms of mental illness—such as low motivation, fear of new situations, and difficulty organizing daily tasks—made it easy to skip toothbrushing and avoid appointments. Powerful psychiatric drugs often dry out the mouth, further increasing the risk of decay and infection.
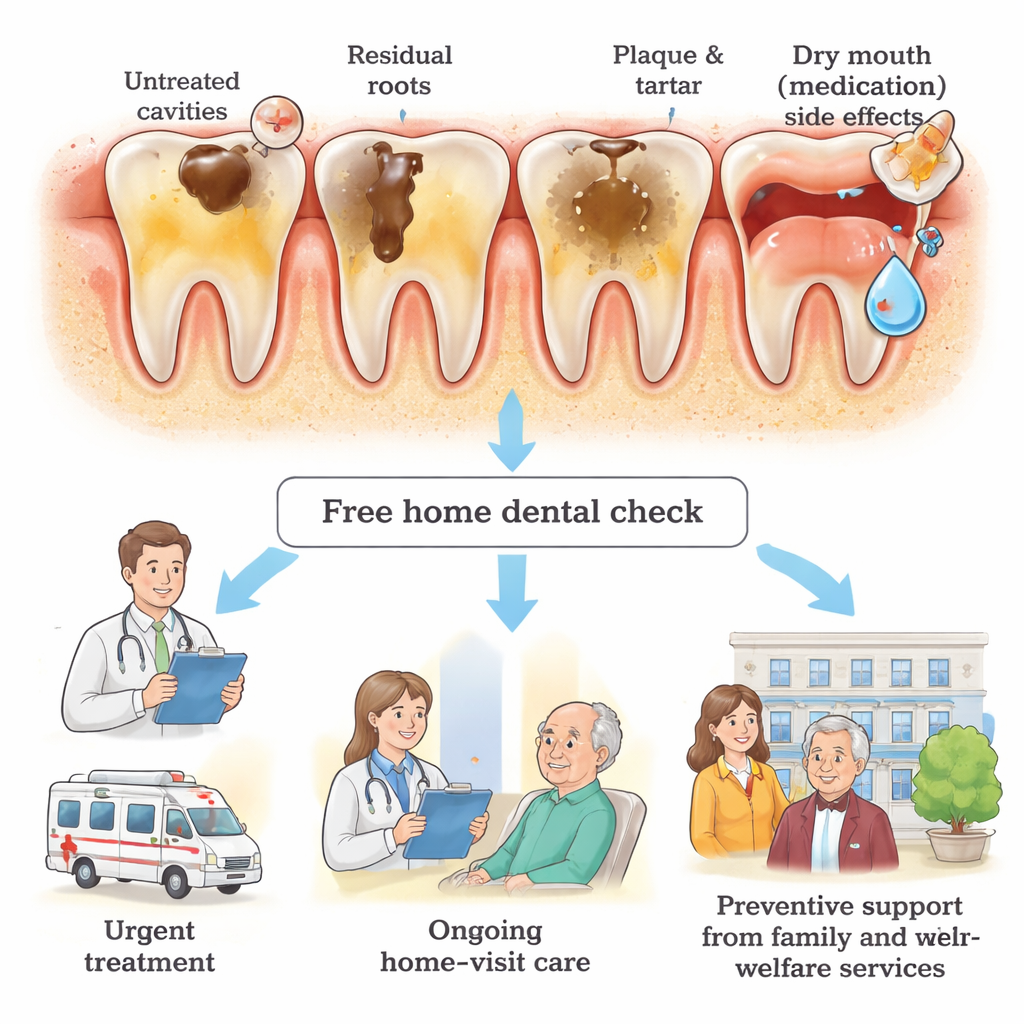
The Quiet Power of Families and Home Visits
When family or other caregivers were closely involved, patients were more likely to move from a free checkup to actual treatment. By mid-2025, seven participants had gone on to receive home-visit dental care; almost all had family present during visits, and all had some form of financial support that removed out-of-pocket costs. The authors argue that teaching families simple daily tasks—like checking the mouth, supervising toothbrushing, and helping arrange appointments—could greatly improve oral health for people who cannot manage these steps alone. They also highlight a promising treatment approach called atraumatic restorative treatment, which uses hand tools and special filling materials to repair cavities gently at home, with less stress for anxious or medically fragile patients.
What Needs to Change to Protect These Smiles
Although this was a small, single-clinic pilot project, its message is clear: every patient in this group had untreated decay and poor oral hygiene. For people whose mental health already makes everyday life difficult, tooth pain, infections, and trouble chewing add an extra, avoidable burden. The authors call for stronger links between psychiatry, dentistry, and social welfare so that oral health checks become a standard part of home visits, and referrals to home-visit dentists are easy and routine. They argue that expanding financial support for home dental services, offering regular free screenings, and building caregiver education programs could prevent small problems from becoming crises. In plain terms, taking care of the mouth should be seen as a basic part of taking care of the mind—especially for those who rarely leave home.
Citation: Suga, T., Tu, T.T.H., Gamo, Y. et al. A preliminary study on oral health status and unmet dental needs in patients with home-based psychiatric services. Sci Rep 16, 4919 (2026). https://doi.org/10.1038/s41598-026-35661-9
Keywords: oral health, serious mental illness, home-based care, dental access, public assistance