Clear Sky Science · en
Clinical implications of systolic blood pressure for diabetic retinopathy across HbA1c levels in a Japanese population
Why your blood pressure matters to your eyesight
For people living with diabetes, keeping blood sugar under control is often the main focus. But this study from Japan suggests that another familiar number—your upper blood pressure reading, or systolic blood pressure—may quietly shape your risk of vision loss, even when your blood sugar looks good. Understanding how these two everyday clinic measurements work together could help patients and doctors better protect sight.
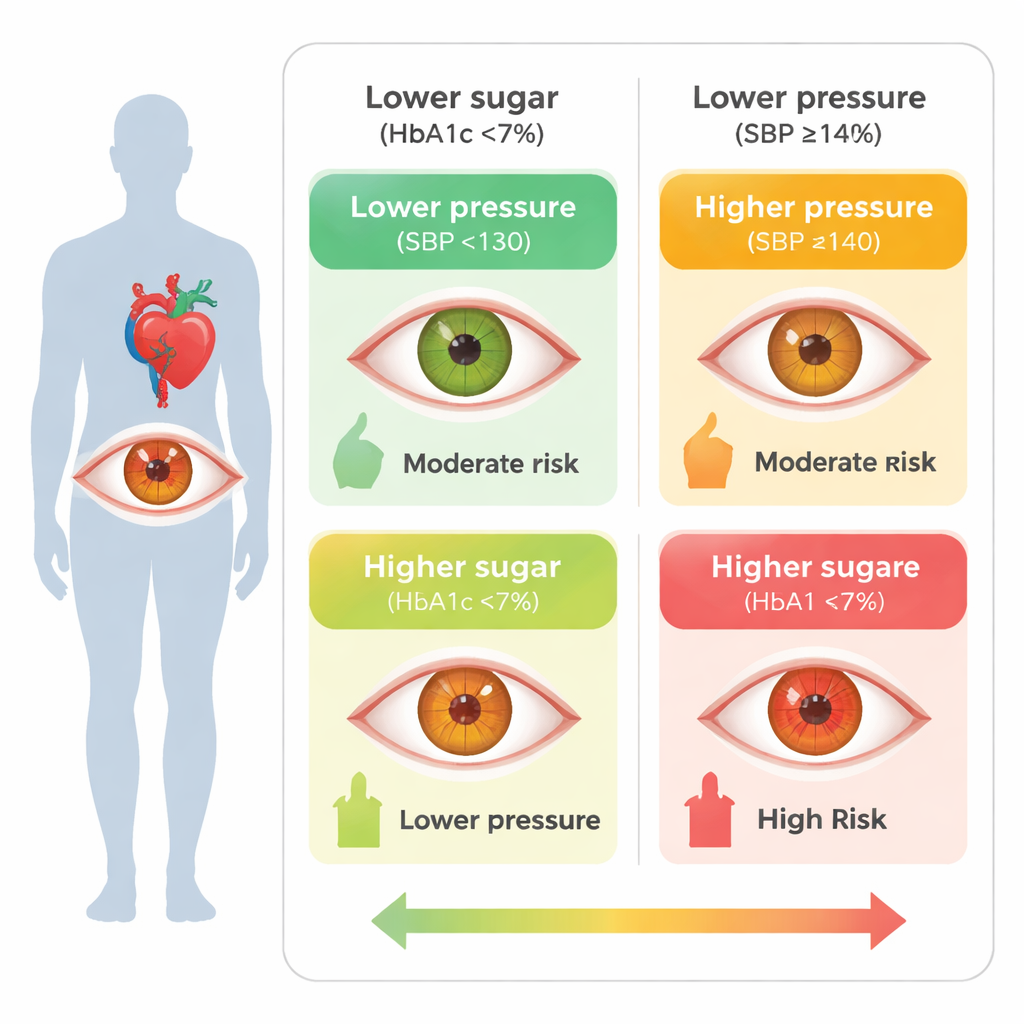
Looking at eyes in a real-world community
Researchers examined 1,049 adults aged 40 and older with diabetes who took part in health and eye screenings in Chikusei City, Japan. Each person had photographs taken of the back of the eye to check for diabetic retinopathy, a condition in which tiny blood vessels in the retina are damaged and can eventually lead to vision loss. The team also measured blood pressure and blood tests, including HbA1c, a marker of average blood sugar over several months. Participants were then sorted into four groups based on whether their blood sugar was relatively well controlled (HbA1c under 7%) or higher (7% or above), and whether their systolic blood pressure was below 140 mmHg or at least 140 mmHg.
How common was diabetic eye damage?
Overall, 13% of the people with diabetes in this study had some degree of diabetic retinopathy. About 8% had early-stage disease—called mild to moderate nonproliferative diabetic retinopathy—where changes are present but may not yet affect vision. Just over 5% had more serious forms, including severe nonproliferative or proliferative diabetic retinopathy, which carry a higher risk of vision loss. On average, people with more advanced eye damage had higher HbA1c levels and slightly higher systolic blood pressure than those without retinopathy, reflecting a heavier burden of long-term diabetes-related stress on the blood vessels in the eye.
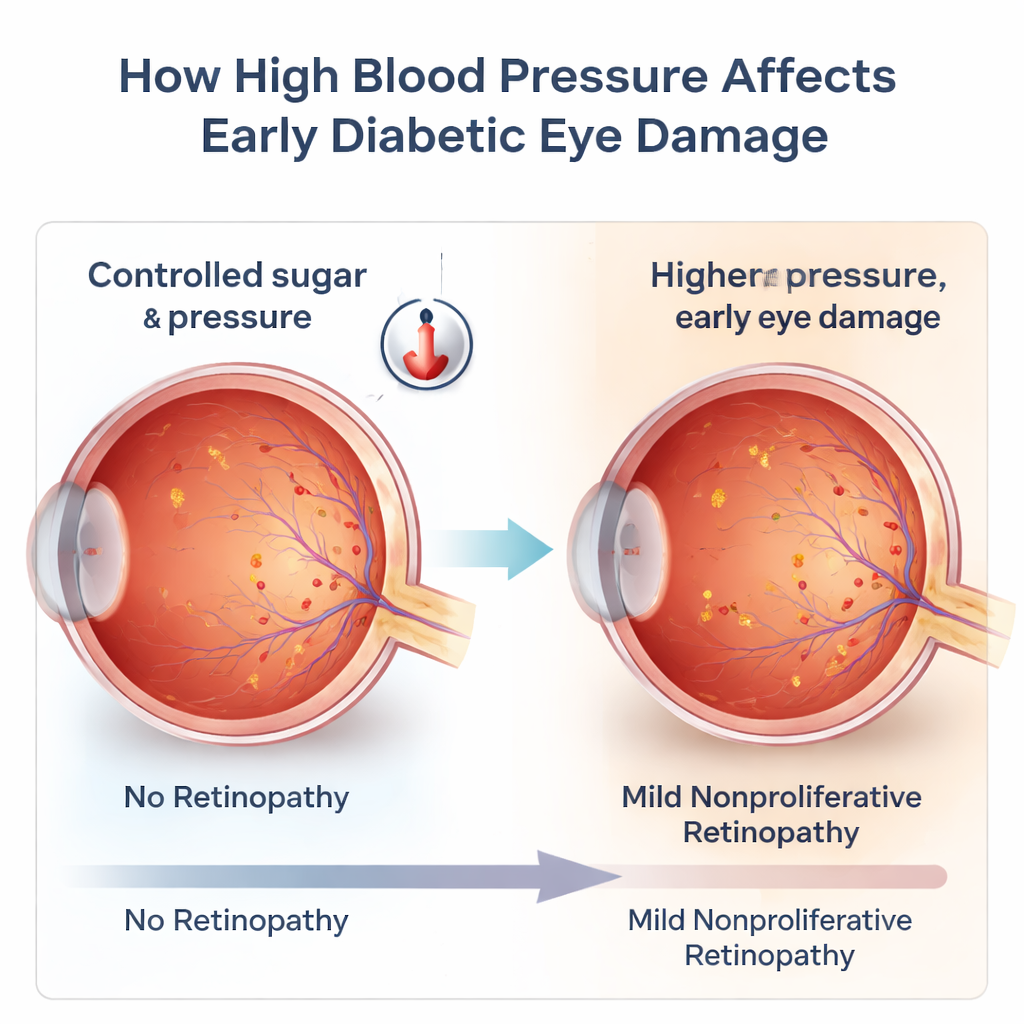
Blood pressure still counts when sugar looks good
The central question was whether systolic blood pressure carries different weight depending on how well blood sugar is controlled. Using statistical models that accounted for age, sex, cholesterol problems, kidney function, smoking, and medications, the researchers compared people with higher and lower systolic blood pressure inside each blood sugar category. Among participants with HbA1c under 7%, those with systolic pressure of at least 140 mmHg had more than double the odds of having diabetic retinopathy compared with those whose pressure was below 140 mmHg. This pattern held particularly for early-stage changes in the retina. In other words, even among people meeting a common blood sugar target, higher blood pressure appeared to push the retina toward damage.
When sugar is high, it may overshadow pressure
Among people whose HbA1c was 7% or higher, diabetic retinopathy was already common, regardless of blood pressure level. Both the lower- and higher-pressure groups in this high-sugar category had about five to six times the odds of retinopathy compared with those who had lower HbA1c and lower systolic pressure. Within this high-sugar group, however, having higher versus lower systolic pressure did not clearly change the odds of retinopathy. This suggests that, once blood sugar is poorly controlled, its damaging effects on the eye may be so strong that additional pressure from higher blood pressure is harder to detect in this kind of snapshot study.
What this means for everyday care
The findings point to a simple but powerful message for people with diabetes and their clinicians. Keeping HbA1c under 7% remains important, but it may not be enough on its own to guard against diabetic eye disease. In those with reasonably controlled blood sugar, letting systolic blood pressure drift into the hypertensive range could still double the chance of early eye damage. While this study cannot prove cause and effect or fully clarify the impact on advanced disease, it strongly supports a two-pronged strategy: manage both blood sugar and blood pressure carefully, and have regular eye exams so that any retinopathy is caught and treated as early as possible.
Citation: Sasaki, M., Ofuji, Y., Hanyuda, A. et al. Clinical implications of systolic blood pressure for diabetic retinopathy across HbA1c levels in a Japanese population. Sci Rep 16, 6093 (2026). https://doi.org/10.1038/s41598-026-35660-w
Keywords: diabetic retinopathy, blood pressure, HbA1c, eye health, type 2 diabetes