Clear Sky Science · en
Five-variable nomogram including PR interval and left atrial appendage flow velocity predicts atrial fibrillation recurrence after cryoballoon ablation
Why heart rhythm relapses matter
Atrial fibrillation is a common heart rhythm problem that raises the risk of stroke and heart failure. One modern treatment, called cryoballoon ablation, uses extreme cold to block faulty electrical pathways in the heart. Yet up to half of patients see the irregular rhythm return within a year. This study asks a simple but crucial question: can doctors tell in advance who is most likely to have atrial fibrillation come back after the procedure?
Looking beyond basic checkups
Most current risk scores for atrial fibrillation focus on age, blood pressure, and other general health conditions. While helpful, they often ignore how the upper chambers of the heart actually look and behave in detail. The researchers followed 757 patients who had their first cryoballoon ablation between 2017 and 2023. All had careful assessments before treatment, including standard heart tracings (electrocardiograms) and ultrasound scans of the heart, with a special focus on the left atrium and its small pouch, the left atrial appendage. The team then tracked which patients stayed free of atrial fibrillation and which had the rhythm problem return over the next two years.
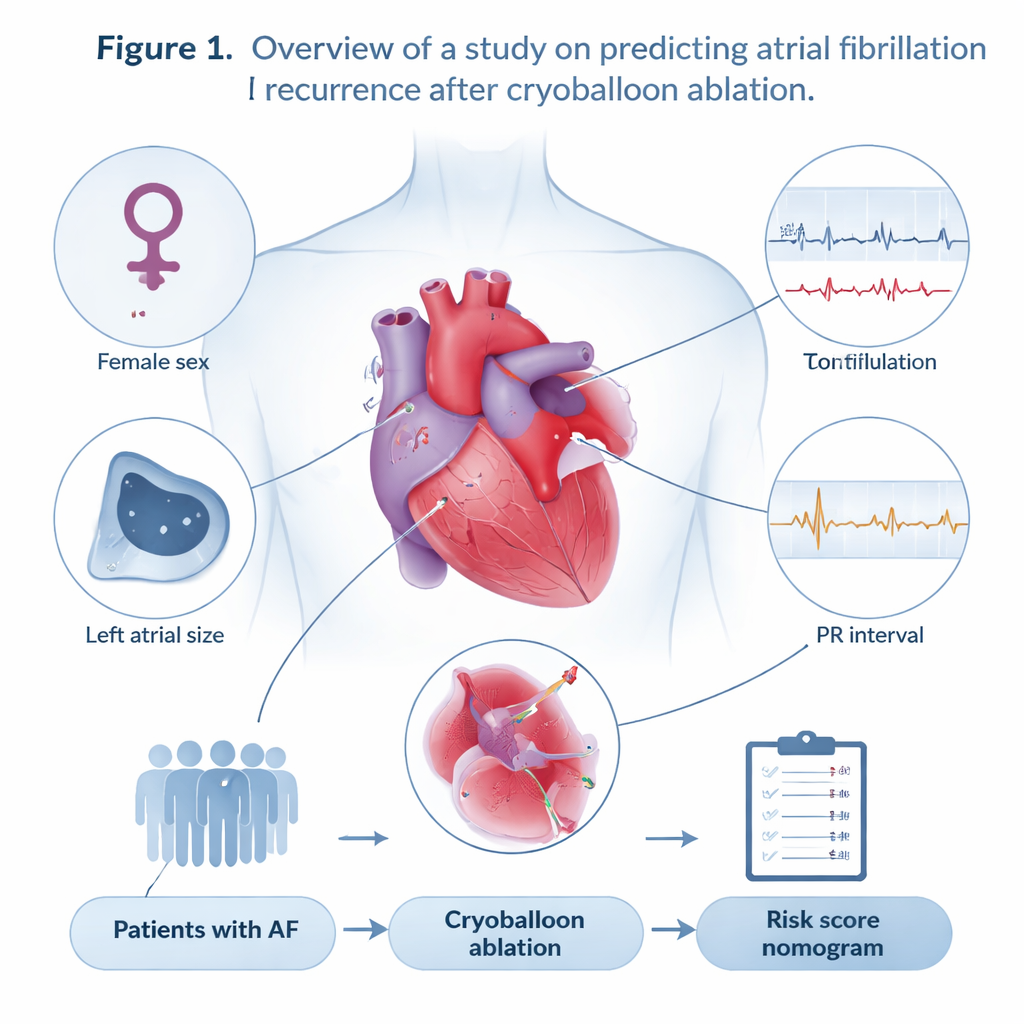
Five simple clues from the heart
From an initial set of 124 possible measurements, the investigators used advanced statistical methods to narrow down the most informative predictors. They found that just five features were enough to build a powerful risk tool. Two were basic clinical traits: being female and having persistent, rather than occasional, atrial fibrillation. Three came from heart tests: the PR interval on the electrocardiogram, which reflects how long electrical signals take to travel from the upper to lower chambers; the size of the left atrium; and the speed of blood flow leaving the left atrial appendage, a measure of how strongly that pouch squeezes. Longer PR intervals, a larger left atrium, and slower flow speeds were all linked to a higher chance that atrial fibrillation would return.
A bedside score for personal risk
Using these five pieces of information, the authors built a “nomogram,” a visual calculator that converts each factor into points and sums them into a personal risk score. Higher scores mean a lower chance of remaining in normal rhythm after ablation. When they tested the model, it correctly separated patients into low-, medium-, and high-risk groups. Over 24 months, about four out of five people in the low-risk group stayed free of atrial fibrillation, compared with less than half in the medium group and only about one in five in the high-risk group. The model’s accuracy, measured by statistical tools called ROC curves, remained high in both the original group of patients and a separate validation group, suggesting the tool is reliable rather than overfitted to one dataset.
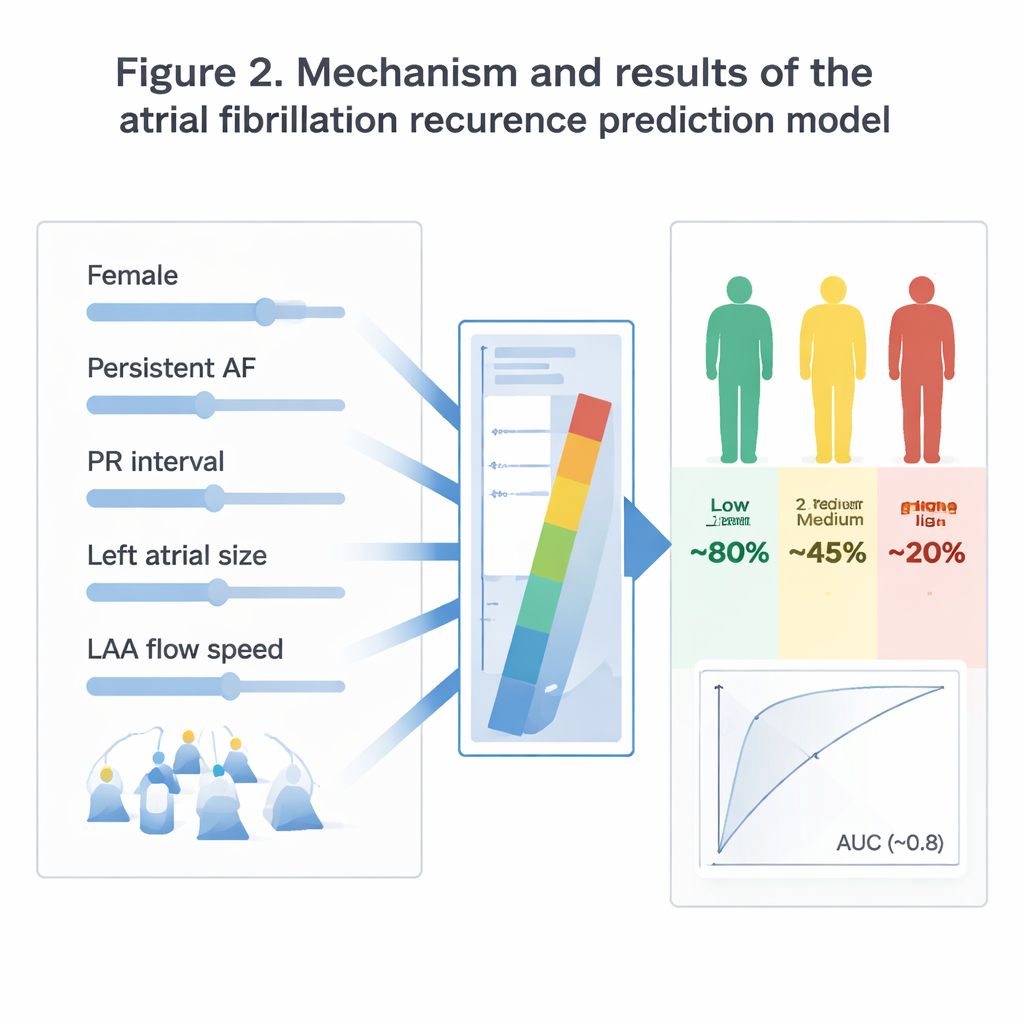
Beating older prediction tools
The new five-factor score was also tested head-to-head against several existing risk scores that doctors sometimes use after ablation. In every comparison, at both one and two years after the procedure, the new model better distinguished between people who would remain in normal rhythm and those who would relapse. This advantage likely comes from incorporating both the structure and function of the left atrium, as well as the subtle electrical delay captured by the PR interval, rather than relying only on age and common medical conditions. Decision analyses suggested that using this tool to guide follow-up—such as closer rhythm monitoring for high-risk patients—could provide more benefit than simply treating everyone the same way.
What this means for patients
For people considering or recovering from cryoballoon ablation, this research offers a clearer picture of what to expect. By combining sex, the type of atrial fibrillation, and three straightforward heart measurements, doctors may soon be able to give patients a personalized estimate of how likely their rhythm problem is to return. Those at lower risk might avoid unnecessary extra tests, while high-risk patients could be monitored more closely or offered additional treatments sooner. The study was done at a single hospital, so larger multi-center trials are still needed, but it points toward a future in which heart rhythm care after ablation is tailored to each person’s unique cardiac fingerprint rather than a one-size-fits-all approach.
Citation: Jie, Q., Qian, W., Jia, H. et al. Five-variable nomogram including PR interval and left atrial appendage flow velocity predicts atrial fibrillation recurrence after cryoballoon ablation. Sci Rep 16, 5644 (2026). https://doi.org/10.1038/s41598-026-35653-9
Keywords: atrial fibrillation, cryoballoon ablation, risk prediction, heart rhythm, echocardiography