Clear Sky Science · en
Molecular insights into macrolide resistant Mycoplasma pneumoniae isolates from outpatient clinics in Tehran, Iran
Why a “walking pneumonia” germ matters
Many people think of pneumonia as a hospital illness, but a tiny germ called Mycoplasma pneumoniae often causes a milder, so‑called “walking pneumonia” in otherwise healthy people. Doctors usually treat it with a common family of antibiotics called macrolides, such as azithromycin. This study from Tehran, Iran, shows that these drugs are increasingly failing against this germ, and explains how researchers tracked the rise of drug‑resistant strains and what it means for patients and public health.
Tracking a stubborn lung infection
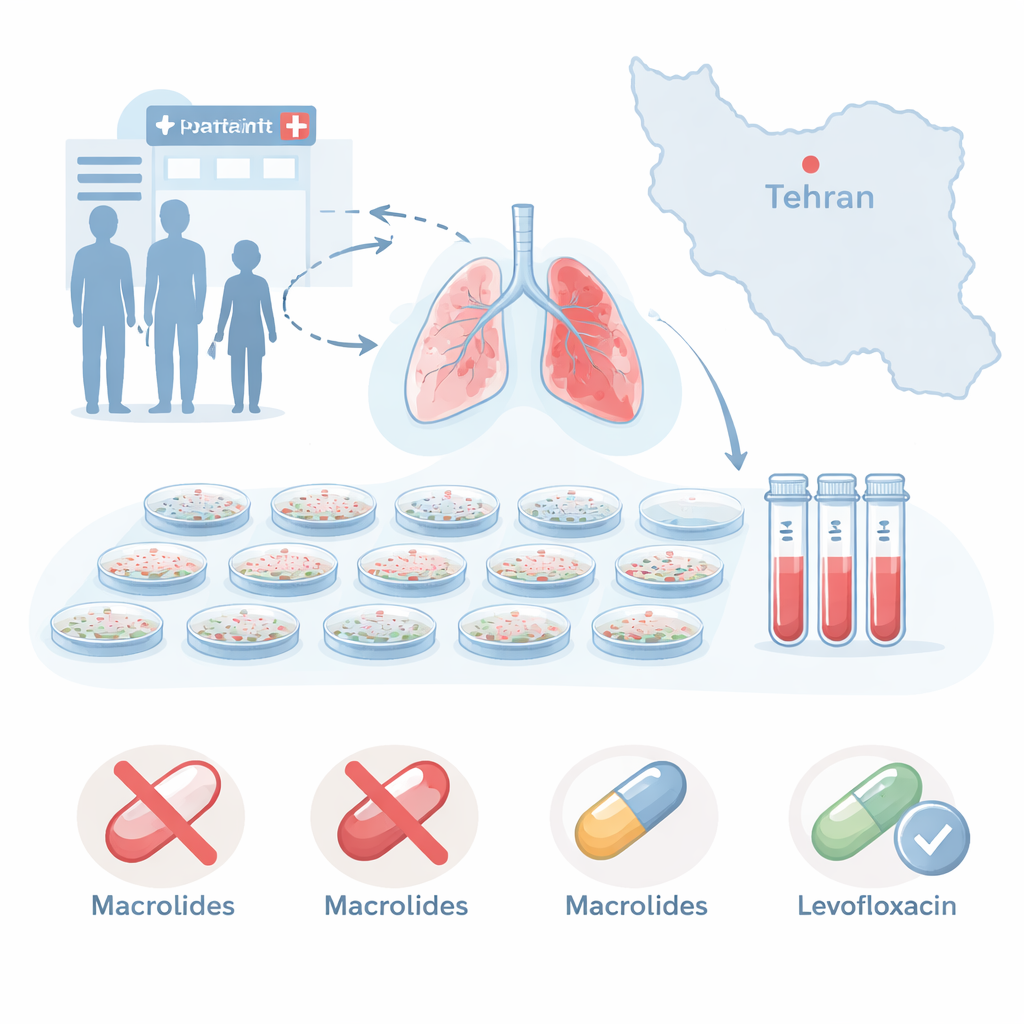
The researchers focused on 270 adults with “atypical pneumonia” seen at four outpatient clinics in Tehran. These patients typically had a dry cough, chest pain, and trouble breathing, but less often had high fever or thick sputum. Lab tests confirmed Mycoplasma pneumoniae infection in 54 of them. Because this microbe lacks a cell wall, the antibiotics used for more typical bacterial pneumonia do not work, so doctors rely heavily on macrolides, especially for community cases treated outside the hospital.
Common antibiotics losing their punch
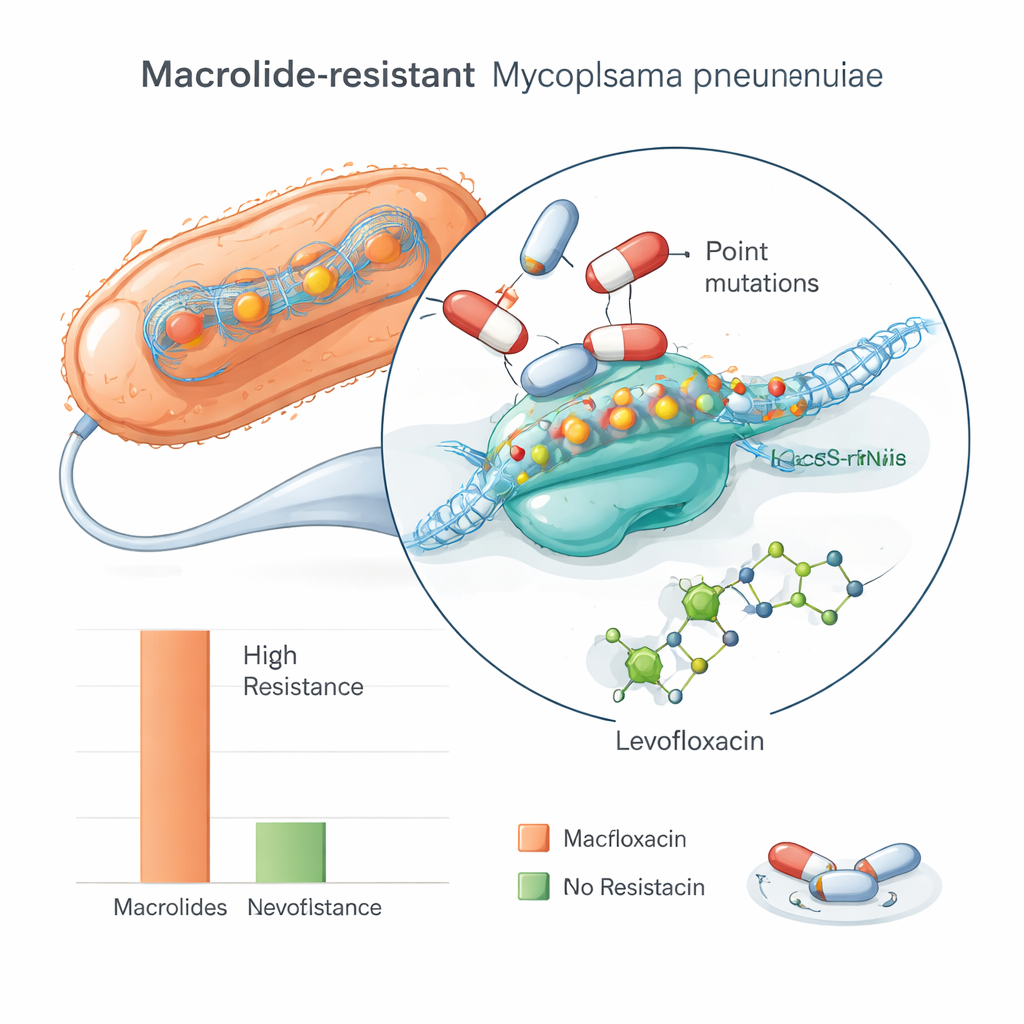
The team tested how well several antibiotics could stop the growth of each Mycoplasma sample in the lab. The results were striking: about 85 percent of the isolates were resistant to two frontline macrolides, erythromycin and azithromycin, meaning it took very high drug levels to slow them down. Some samples showed reduced response to other drugs such as tetracycline or clindamycin, but these rates were much lower. In contrast, every isolate remained sensitive to levofloxacin, a different type of antibiotic often reserved for more serious infections. In real‑world terms, this pattern suggests that the usual first‑line drugs may fail in many Iranian patients, forcing doctors toward second‑line options with more side effects and age limits.
Clues from the germ’s “family tree”
To understand how these resistant strains were spreading, the scientists used a genetic fingerprinting method called multilocus sequence typing. By reading sections of eight housekeeping genes, they identified eight distinct genetic types among 20 randomly chosen resistant samples. One type, called ST3, made up half of all resistant isolates, and most belonged to a broader “family” of closely related strains known as clonal complex 1. Computer‑generated family trees and network diagrams showed that the Tehran strains fell into three main clusters, mirroring patterns seen in East Asian countries where resistant Mycoplasma has become common.
Connecting local findings to a global picture
When the Tehran data were compared with a global online database of Mycoplasma types, the same ST3 lineage again stood out as dominant worldwide, especially among resistant strains. However, Iran showed a relatively higher share of a few other types, such as ST2 and ST14, hinting at regional twists in how the germ evolves and spreads. Most clinical symptoms did not reliably distinguish resistant from non‑resistant infections, underscoring that doctors cannot guess resistance from how sick a patient looks; they need access to good laboratory testing and up‑to‑date local data.
What this means for patients and doctors
For lay readers, the message is clear: a familiar “walking pneumonia” germ is learning to dodge some of our most trusted antibiotics in parts of the world, including Iran. This study shows that macrolide‑resistant Mycoplasma pneumoniae is already very common in Tehran and is dominated by a few successful genetic families, especially one called ST3. While another drug, levofloxacin, still works well in the lab, it cannot be used freely in all age groups and must be prescribed carefully. The authors argue that continued genetic and drug‑sensitivity monitoring, along with more cautious antibiotic use, are essential to keep treatment options effective and to slow the spread of these hardier strains.
Citation: Arfaatabar, M., Sadeghi, Y., Goodarzi, N.N. et al. Molecular insights into macrolide resistant Mycoplasma pneumoniae isolates from outpatient clinics in Tehran, Iran. Sci Rep 16, 7432 (2026). https://doi.org/10.1038/s41598-026-35614-2
Keywords: antibiotic resistance, Mycoplasma pneumoniae, macrolides, pneumonia, molecular typing