Clear Sky Science · en
Multiparametric comparative assessment of surgical efficacy in patients with SUI and POP versus normal controls
Why Pelvic Support Matters
Millions of women leak urine when they cough, laugh, or exercise, and many also feel a heavy bulge in the vagina. These problems, called stress urinary incontinence and pelvic organ prolapse, can disrupt work, intimacy, and daily life, yet they are often suffered in silence. This study used advanced MRI scanning to look inside the body before and after a modern combined operation, showing in clear images how surgery can rebuild the body’s natural “hammock” of support and help women regain control.
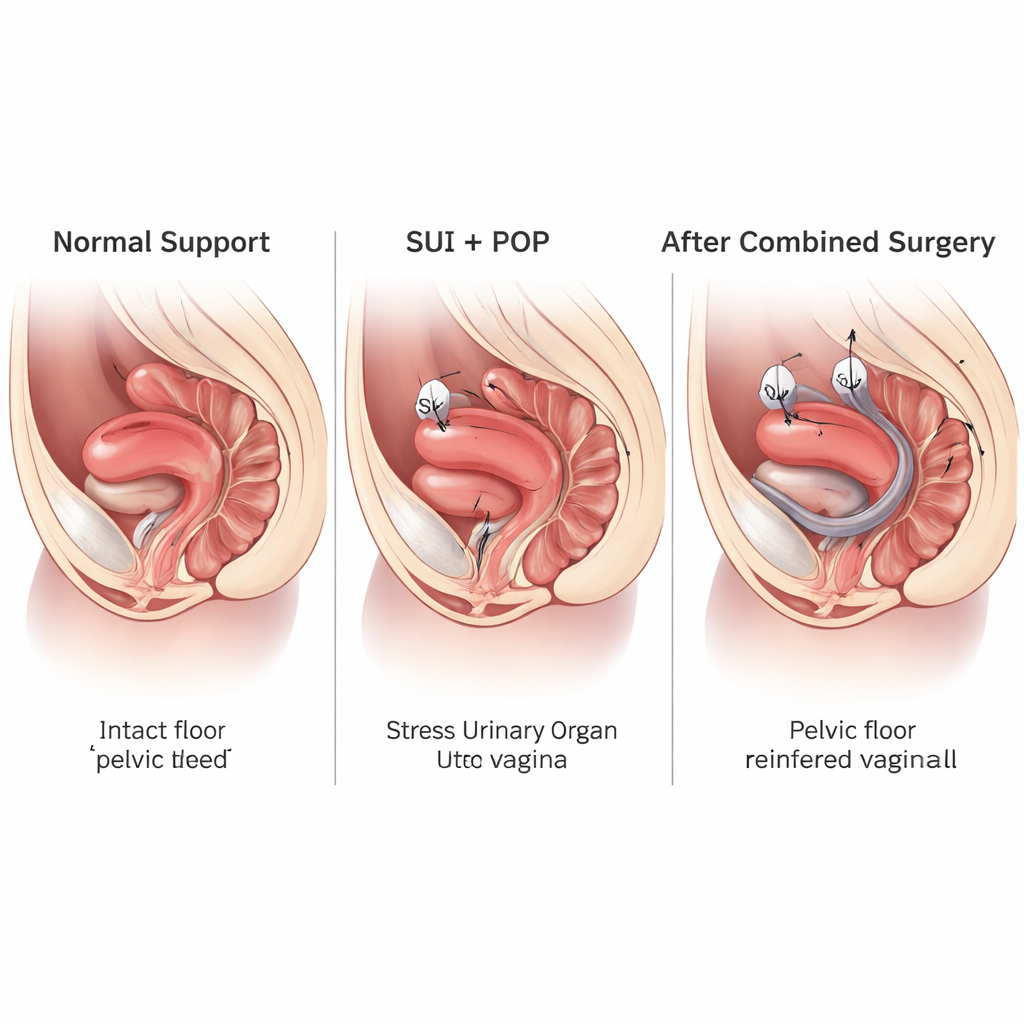
The Hidden Hammock Inside the Pelvis
Deep in the pelvis, muscles, ligaments, and connective tissue act like a flexible hammock. They hold up the bladder, uterus, and bowel and help close the urethra so urine does not leak during physical effort. When this support is damaged by childbirth, aging, or long-term strain, organs can sag downward. This sagging stretches the pelvic floor opening, shifts the angle of the vagina and uterus, and weakens the body’s natural self-locking system, leading to both urine leakage and pelvic organ prolapse.
Who Was Studied and How
The researchers analyzed 50 women with moderate prolapse and stress urinary incontinence who all had the same combined operation: a transobturator sling under the mid-portion of the urethra plus a reconstruction of the back wall of the vagina and the perineal body, the firm tissue between the vagina and anus. They also enrolled 10 healthy women of similar age and childbirth history as a comparison group. All participants had high-resolution MRI scans, and in the surgical group these scans were repeated six months after surgery. Using special software, the team measured the size of the pelvic floor opening, the length and position of the urethra, and the angles and coordinates of key points along the uterus and vagina in a standardized internal “map” of the pelvis.
What Changed After Surgery
Before surgery, women with prolapse had a smaller and weaker perineal body, a shortened urethra, and a widened pelvic floor opening compared with healthy women. The axis of the vagina was bent and shifted forward, showing that the organs had slipped out of their ideal alignment. After the combined operation, MRI showed that the perineal body area nearly doubled, the urethra became longer, and the opening in the pelvic floor narrowed back toward normal. The angles between different parts of the vagina, and the plotted positions of landmarks such as the top of the vagina and the vaginal opening, moved back into the same region as those of the healthy controls. In other words, the organs were lifted and re-centered, and the internal “geometry” of the pelvis was largely restored.
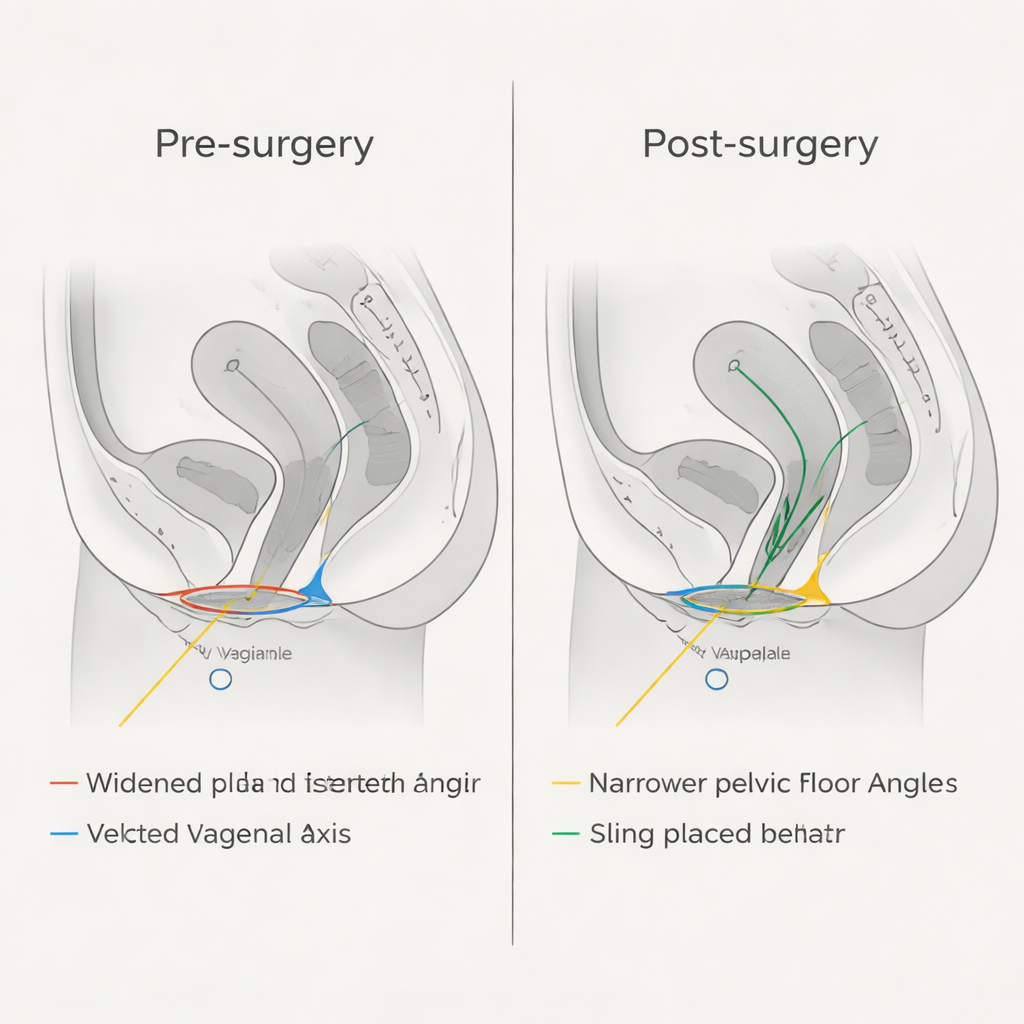
Rebuilding Balance, Not Just Lifting Organs
The authors interpret these changes as more than simple tightening. By reconstructing the perineal body and back wall of the vagina and adding a supportive sling under the urethra, the surgery reestablished a balanced system of forces. When a woman stands or strains, pressure is once again directed toward the strong tissues at the back of the pelvis rather than straight down toward the vaginal opening. The repaired tissues and repositioned organs recreate a functional bending angle in the vagina and a stable “hammock” under the bladder and urethra. This biomechanical reset helps explain why previous clinical work from the same team found high cure and satisfaction rates and low reoperation rates with the combined procedure.
What This Means for Patients
To a lay reader, the message is encouraging: modern pelvic floor surgery can do more than patch a problem area. Using careful imaging, this study shows that a combined sling and posterior repair can rebuild the underlying support system so that the bladder, uterus, and vagina work together again as they should. While the research has limits—such as a modest number of patients and focus on anatomy rather than detailed symptom scores—it provides strong visual evidence that the operation restores both structure and balance. For women living with leakage and prolapse, it suggests that well-planned surgery, guided by an understanding of pelvic mechanics, can offer durable relief and a return to confident everyday life.
Citation: Tian, D., Luo, Q., Wang, X. et al. Multiparametric comparative assessment of surgical efficacy in patients with SUI and POP versus normal controls. Sci Rep 16, 5274 (2026). https://doi.org/10.1038/s41598-026-35587-2
Keywords: pelvic floor, urinary incontinence, pelvic organ prolapse, pelvic surgery, MRI imaging