Clear Sky Science · en
Non-reassuring fetal heart rate and associated factors among laboring mothers at southern public hospitals in Ethiopia: a poisson regression model
Why a Baby’s Heartbeat in Labor Matters
When a woman is in labor, one of the most closely watched signs is her baby’s heartbeat. Changes in this rhythm can warn doctors and midwives that the baby is not getting enough oxygen and may be in trouble. This study from public hospitals in Southern Ethiopia looks at how often worrisome heartbeat patterns occur during childbirth and which everyday factors—like clinic visits, alcohol use, and pregnancy complications—raise the risk. Understanding these links can help improve care for mothers and babies both in Ethiopia and in other low‑resource settings.
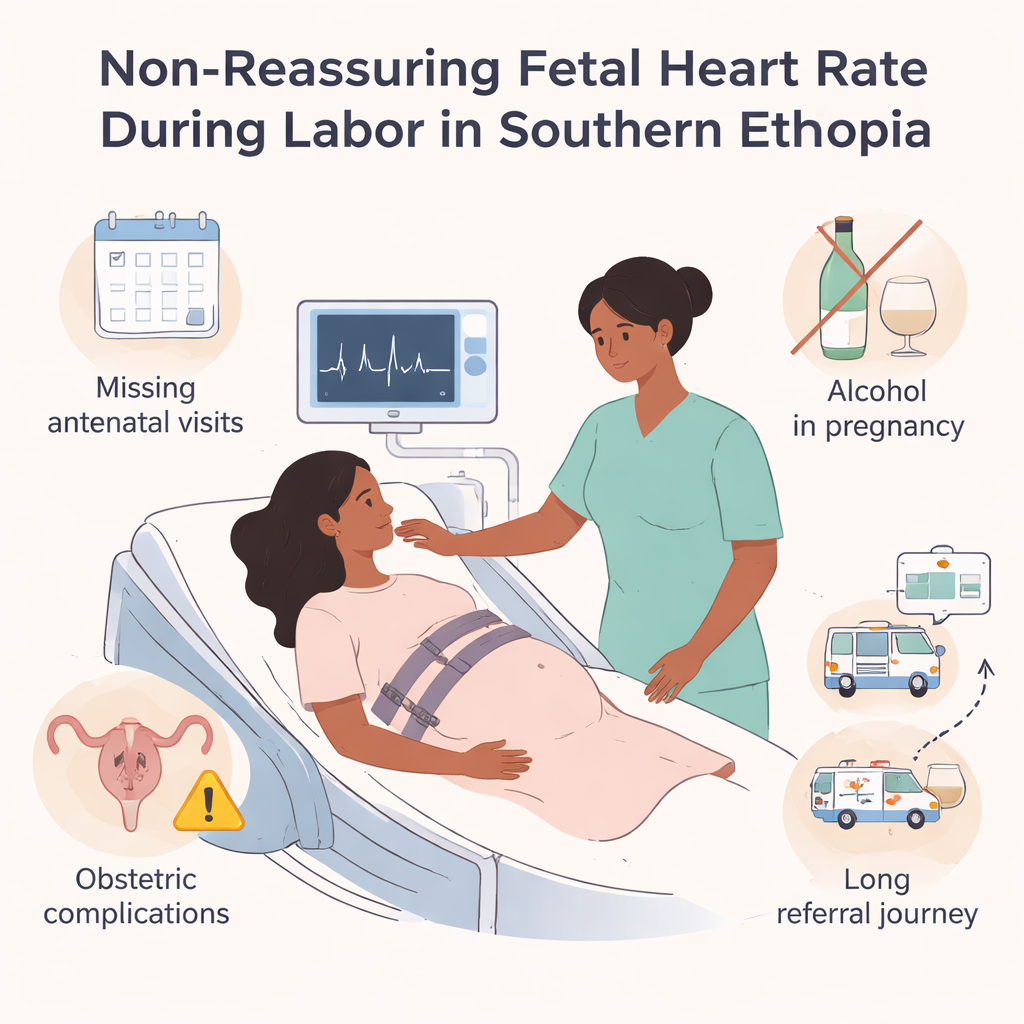
What Doctors See on the Monitor
During labor, caregivers regularly check the baby’s heartbeat using a machine called a cardiotocograph or a handheld device. A healthy pattern shows a steady rate with gentle ups and downs as the baby moves and the uterus contracts. A pattern called “non‑reassuring fetal heart rate” appears when the heartbeat is too fast, too slow, or loses its usual variability, or when it repeatedly drops during or after contractions. These signals suggest that the baby may not be getting enough oxygen and may soon develop serious problems such as brain injury or even death if no action is taken.
A Close Look at Births in Southern Ethiopia
The researchers carried out a cross‑sectional study in three public hospitals in the South Omo zone of Southern Ethiopia between June and November 2023. They included 448 women who came in labor and met specific criteria, excluding those whose babies already had severe problems like major birth defects or death before admission. Trained midwives interviewed the mothers, reviewed their medical charts, and continuously tracked the babies’ heart rates during labor. The team then used a statistical approach called Poisson regression to identify which maternal and birth‑related factors were linked to non‑reassuring heart rate patterns.
How Often the Warning Signs Appeared
The study found that non‑reassuring fetal heart rate patterns were strikingly common: they occurred in about two out of every five births (41.5 percent). This rate is higher than what has been reported in many high‑income countries and in some earlier studies from other parts of Ethiopia and Africa. The authors suggest several reasons, including differences in how referrals work, how carefully fetal heart monitoring is used and interpreted, and the overall health and risk profiles of the mothers who reach these hospitals. Regardless of the cause, such a high rate means that a large share of babies are exposed to possible oxygen shortage during birth.
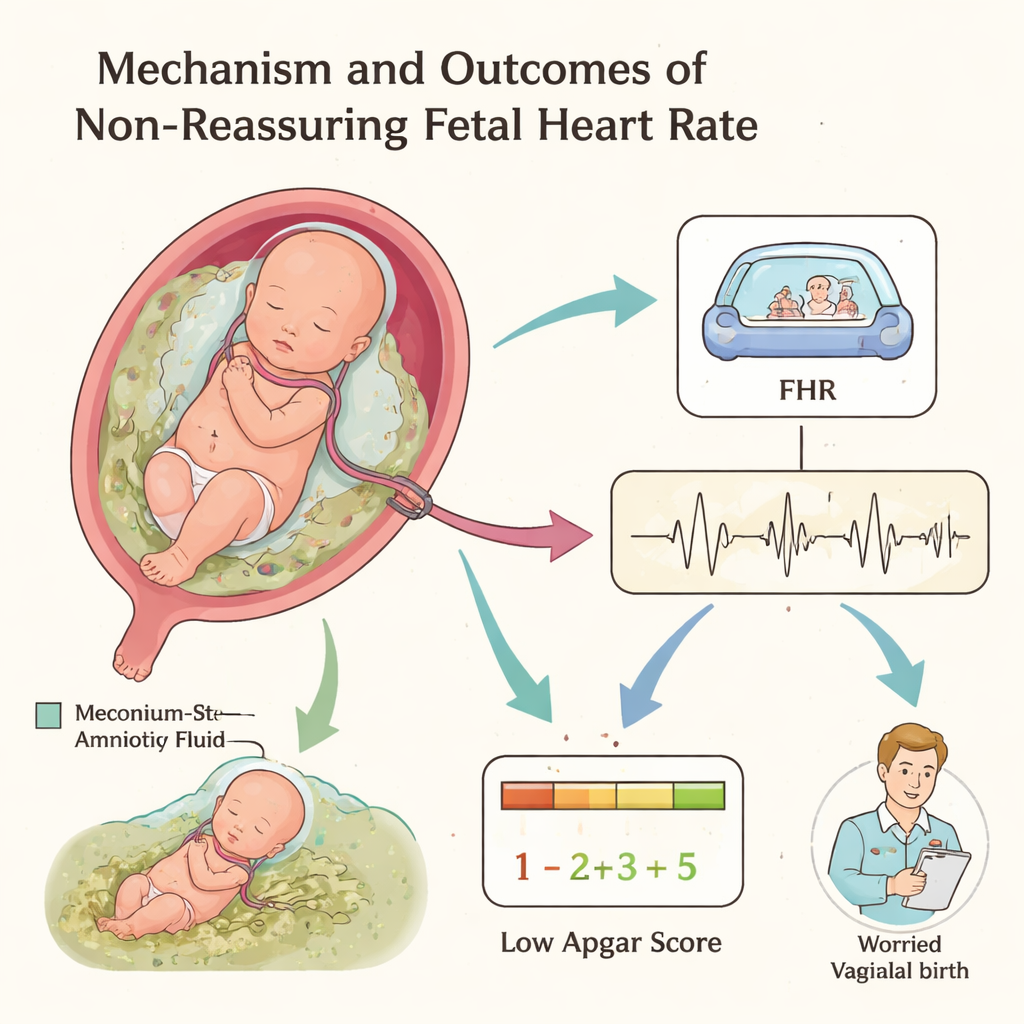
Everyday Factors That Raise the Risk
Several clear risk factors stood out. Mothers who had no antenatal care visits were more than three times as likely to have a baby with a non‑reassuring heart rate compared with those who attended checkups. Women with pregnancy‑related complications—such as high blood pressure or bleeding—also had a much higher risk. Drinking alcohol during pregnancy, being transferred from another health facility (often after a long and complicated labor), and the presence of meconium‑stained amniotic fluid (when the baby has passed stool into the fluid) all increased the chance of dangerous heart rate patterns. Another strong factor was a nuchal cord, when the umbilical cord is wrapped around the baby’s neck, which can squeeze the cord and reduce blood and oxygen flow during contractions.
What This Means for Mothers and Babies
For a layperson, the message is straightforward: problems during pregnancy and labor often show up first as changes in the baby’s heartbeat. In this Ethiopian setting, many babies showed warning patterns, especially when their mothers lacked regular prenatal visits, drank alcohol, had complications, or arrived late after being referred. The study suggests that simple steps—such as encouraging early and repeated antenatal care, discouraging alcohol use, improving transport and referral systems, and closely monitoring labor with prompt action when fluid is stained or the cord is around the neck—could greatly improve the chances that babies are born healthy and breathing well.
Citation: Asnake, A.B., Desalew, A., Meseret, F. et al. Non-reassuring fetal heart rate and associated factors among laboring mothers at southern public hospitals in Ethiopia: a poisson regression model. Sci Rep 16, 5192 (2026). https://doi.org/10.1038/s41598-026-35575-6
Keywords: fetal heart rate, labor and delivery, antenatal care, perinatal outcomes, Ethiopia