Clear Sky Science · en
A pragmatic approach to identifying postextubation dysphagia in critically ill surgical patients using the water swallow test
Why swallowing matters after the breathing tube comes out
Many people leave the operating room or intensive care unit (ICU) with a breathing tube that helped them survive a critical illness. But once that tube is removed, a hidden problem can appear: some patients suddenly have trouble swallowing safely. This study asked a simple question with big consequences for recovery—can a quick bedside water drinking test reliably flag which surgical ICU patients are at risk for swallowing trouble and serious complications like pneumonia?
A simple bedside test for a complex problem
After breathing tubes are removed, some patients develop postextubation dysphagia—difficulty swallowing that can send food or liquid into the lungs instead of the stomach. That misdirection, called aspiration, can trigger pneumonia, repeated need for breathing support, and longer hospital stays. Specialized tests using X‑rays or tiny cameras through the nose can precisely measure swallowing, but they require equipment, trained staff, and time. The team at a large Thai hospital wanted a more practical way to screen many surgical ICU patients quickly. They chose a structured water swallow test, in which a just‑extubated patient first drinks small spoonfuls of water and then a larger amount while a clinician watches closely for signs of choking, coughing, voice changes, or a drop in oxygen levels.
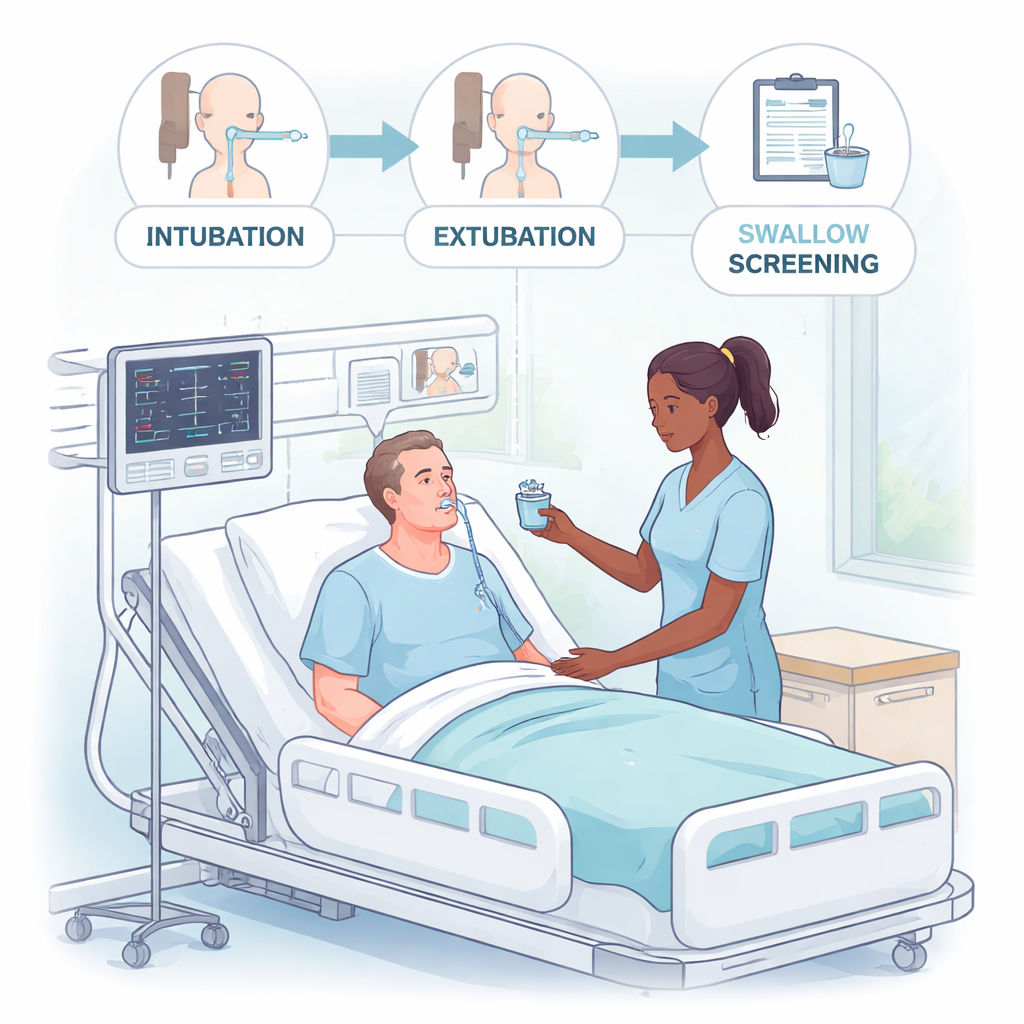
Who was tested and what happened
Over nearly two years, 123 adult patients in a surgical ICU who had been on a breathing machine for at least 12 hours, were awake, stable, and able to follow commands took the water swallow test a few hours after their breathing tubes were removed. Patients with obvious reasons for swallowing trouble—such as head and neck surgery, major brain problems, or long periods without any food by mouth—were excluded so the study could focus on the impact of the tube itself and critical illness. If a patient did poorly on the water test, they were sent for a more detailed examination with a flexible camera (a fiberoptic endoscopic evaluation of swallowing) at the bedside to confirm whether they truly had dysphagia.
How often swallowing trouble occurred
Most patients—114 out of 123—appeared to pass the water swallow test without obvious signs of difficulty. Thirteen patients failed the bedside test; ten of them went on to the camera‑based exam. In that group, eight were confirmed to have swallowing problems. Overall, that meant about 1 in 15 patients (6.5%) in this carefully selected surgical ICU group had confirmed postextubation dysphagia. Those with swallowing trouble tended to be older, slimmer, and more severely ill. They had been on the breathing tube much longer—typically about six days compared with a day and a half—and more often had needed to be re‑intubated, meaning the breathing tube had to be put back in after an earlier removal attempt.
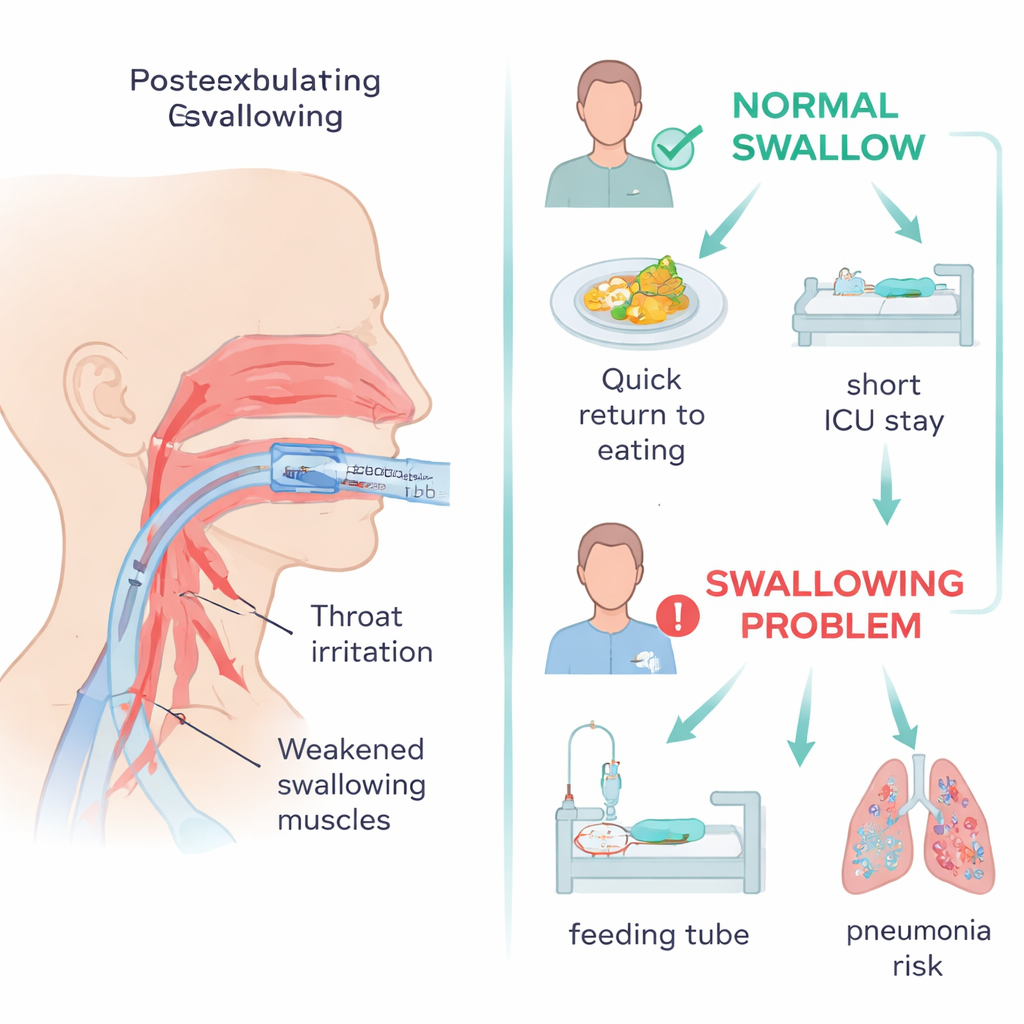
Riskier paths and slower recoveries
The study also tracked what happened to patients after the test. Those with swallowing problems took much longer to eat by mouth again and relied on feeding tubes for days to weeks instead of a day or two. They stayed longer in the ICU and in the hospital overall and were more likely to need the breathing tube reinserted within a month. Certain features stood out as warning signs for dysphagia: a history of reintubation, more days on medicines to support blood pressure, higher levels of blood urea nitrogen (a marker that can reflect illness severity and kidney strain), and longer time spent intubated. These factors likely reflect both direct injury and irritation to the throat from the tube, and the broader weakness and nerve changes that come with severe critical illness.
What this means for patients and care teams
For patients and families, the study’s message is both reassuring and cautionary. In this surgical ICU, most carefully screened patients did not have serious swallowing trouble once the tube came out, and aspiration pneumonia was rare. At the same time, a small but important group did develop significant difficulties that slowed their recovery. The quick water swallow test proved to be a practical, nurse‑friendly way to spot many of these high‑risk patients early, even though it can miss “silent” aspiration that causes no obvious coughing. The authors conclude that ICUs should routinely screen for swallowing problems after extubation, pay special attention to older, long‑intubated, or reintubated patients, and closely monitor any patient starting to drink or eat again. Doing so may help prevent pneumonia, reduce the need for repeat intubation, and get patients home sooner and safer.
Citation: Yuyen, T., Intusut, M., Phothikun, N. et al. A pragmatic approach to identifying postextubation dysphagia in critically ill surgical patients using the water swallow test. Sci Rep 16, 5253 (2026). https://doi.org/10.1038/s41598-026-35533-2
Keywords: swallowing problems, breathing tube removal, intensive care, aspiration pneumonia, water swallow test