Clear Sky Science · en
A mixed methods assessment of disaster management perceptions among healthcare practitioners in Qatar
Why this matters for everyday life
When disasters strike—whether a pandemic, a political crisis, or a massive sporting event that strains local services—the strength of a community’s healthcare system can mean the difference between chaos and control. This study from Qatar asks a simple but vital question: how ready are the doctors, nurses, pharmacists, and other healthcare workers we depend on when things go very wrong, and what helps or hinders their ability to respond?
Taking the pulse of a health system under stress
The researchers surveyed over 400 healthcare practitioners from major public institutions in Qatar and held online group discussions with 41 of them. Participants came from hospitals, primary health centers, and the Ministry of Public Health, and included a wide mix of professions. The team used a detailed questionnaire to probe five areas: what people know about disasters, how they feel about their roles, how often they actually practice key skills, how willing they are to keep working during crises, and how well they think their organizations manage such events. They also listened closely to workers’ own stories of recent emergencies, including the COVID-19 pandemic, the 2017 Gulf diplomatic crisis that disrupted supply chains, and the FIFA World Cup 2022, which acted as a large-scale stress test for the health system.
Strong confidence, but limited hands-on practice
On paper, the results were reassuring. Most healthcare workers rated their knowledge of disaster roles, reporting lines, and basic life-saving actions as good. They strongly supported having national and institutional disaster plans and were generally willing to work extra hours and continue their duties in difficult conditions. Many felt their organizations had solid plans, adequate supplies, and recognized staff contributions. However, when it came to real-world practice, gaps emerged. Participation in drills, simulations, and plan updates was only moderate, and a substantial share of staff reported that they rarely or only occasionally took part in activities like improving disaster plans or supervising volunteers. Frontline workers often described disaster training as too theoretical, with practical exercises focused on managers rather than the broader workforce.
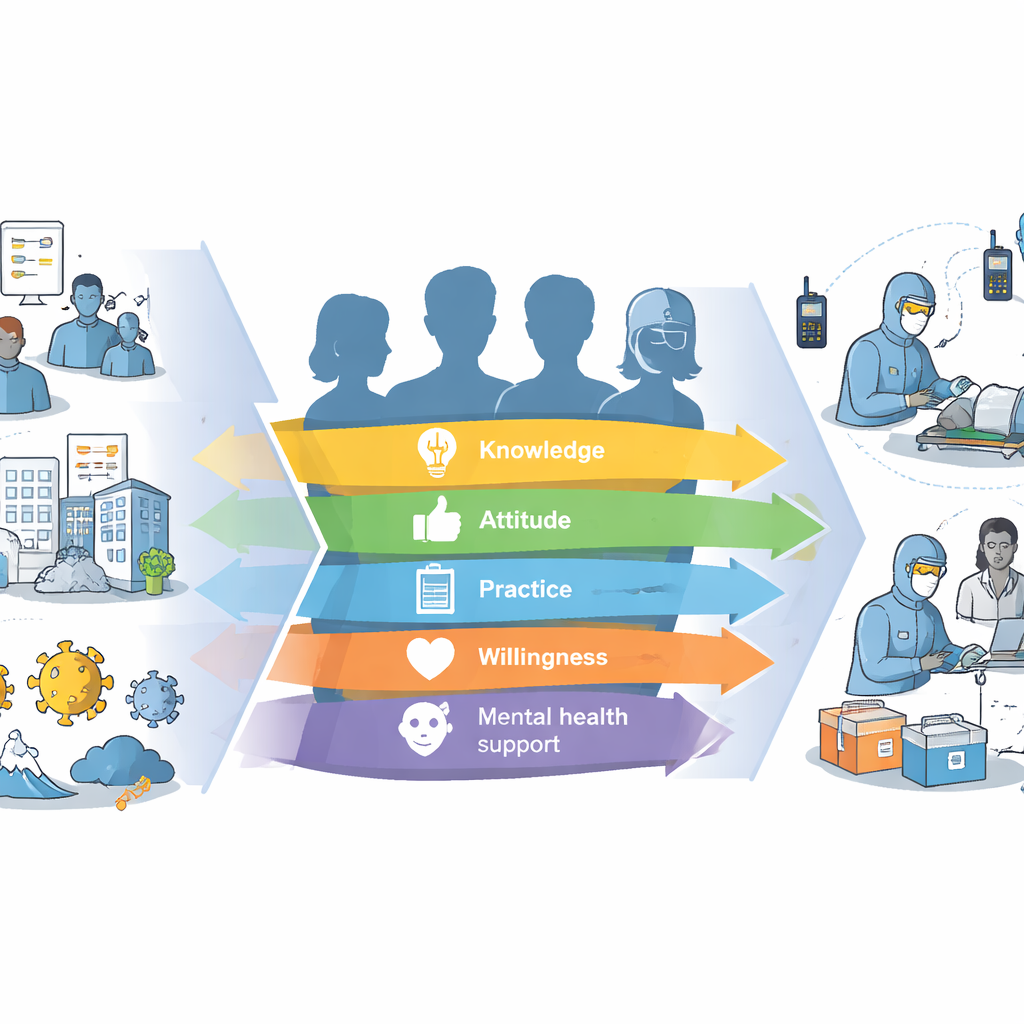
What really boosts readiness
Two factors stood out as especially powerful: training and lived experience. Staff who had taken disaster courses, held administrative roles, or worked through major events like COVID-19 or the 2017 blockade consistently reported higher confidence in their knowledge, skills, and their organization’s management. Focus group discussions fleshed this out with vivid detail: workers spoke of large-scale mock crises, mass vaccination campaigns, new command centers, and rapid expansions of services. They also highlighted more modern tools—telemedicine, risk registries, mobile apps, and even artificial intelligence—as emerging supports for earlier detection, better coordination, and safer care during emergencies. At the same time, they described emotional strain, burnout, and fear for themselves and their families, underscoring the importance of mental health support, peer solidarity, and compassionate leadership.
Teamwork, technology, and the wider community
Beyond individual skills, the study shows that disaster readiness is a team sport. Healthcare workers emphasized how much they rely on clear communication, shared plans, and smooth collaboration between hospitals, clinics, ministries, universities, and even volunteers. They pointed to both successes—such as daily briefings and well-run command centers—and weaknesses, including mixed messages, fragmented digital systems, and confusion about who does what across professions. Workers also saw the public as a crucial partner. The pandemic, in particular, raised general awareness of basic protection measures and showed that families can shoulder more responsibility when equipped with good information, testing tools, and clear guidance. Yet outreach efforts were often reactive, and mistrust or hesitancy about measures like vaccination remained obstacles.
What this means for the future
For a layperson, the message is both hopeful and cautionary. Qatar’s healthcare workforce feels broadly knowledgeable, motivated, and backed by strong national plans—important foundations for any future crisis. But the study exposes a gap between having plans and living them: too many staff are still on the sidelines when it comes to hands-on drills, decision-making, and using lessons learned to refine procedures. The authors argue that making disaster training practical, frequent, and mandatory, involving frontline workers in planning, strengthening mental health support, improving communication systems, and engaging the wider community are all essential steps. In simple terms, being ready for the next disaster is less about having a thick manual on the shelf and more about making preparedness part of everyday work and everyday life.
Citation: Elshami, S., Abdel-Rahman, M.E., Abdul Rahim, H. et al. A mixed methods assessment of disaster management perceptions among healthcare practitioners in Qatar. Sci Rep 16, 8864 (2026). https://doi.org/10.1038/s41598-026-35518-1
Keywords: disaster preparedness, healthcare workforce, Qatar health system, emergency training, public health resilience