Clear Sky Science · en
Colorimetric loop-mediated isothermal amplification for the rapid and visual detection of hepatitis B virus
Why a Simple Color Change Matters
Hepatitis B virus (HBV) is a leading cause of liver failure and liver cancer, especially in low- and middle-income countries where many people cannot access sophisticated laboratory tests. The study behind this article introduces a low-cost, electricity-light test that can spot high levels of HBV by nothing more than a visible color change in a small tube. This kind of easy-to-read test could help clinics without advanced machines quickly find people at greatest risk and connect them to care.
A Fast Test Built for Real-World Clinics
The researchers focused on a method called loop-mediated isothermal amplification, or LAMP, which copies viral DNA at a single, steady temperature instead of cycling through many temperatures like conventional PCR machines do. They paired LAMP with a pH-sensitive dye called cresol red in a carefully tuned chemical mix. When HBV DNA is present and amplified at 65 °C for 50 minutes, the reaction releases protons, the solution becomes more acidic, and the dye changes from pink to yellow. If there is no HBV DNA, the color stays pink. This design means that a health worker needs only a basic heater and their own eyes to read the result: pink for negative, yellow for positive.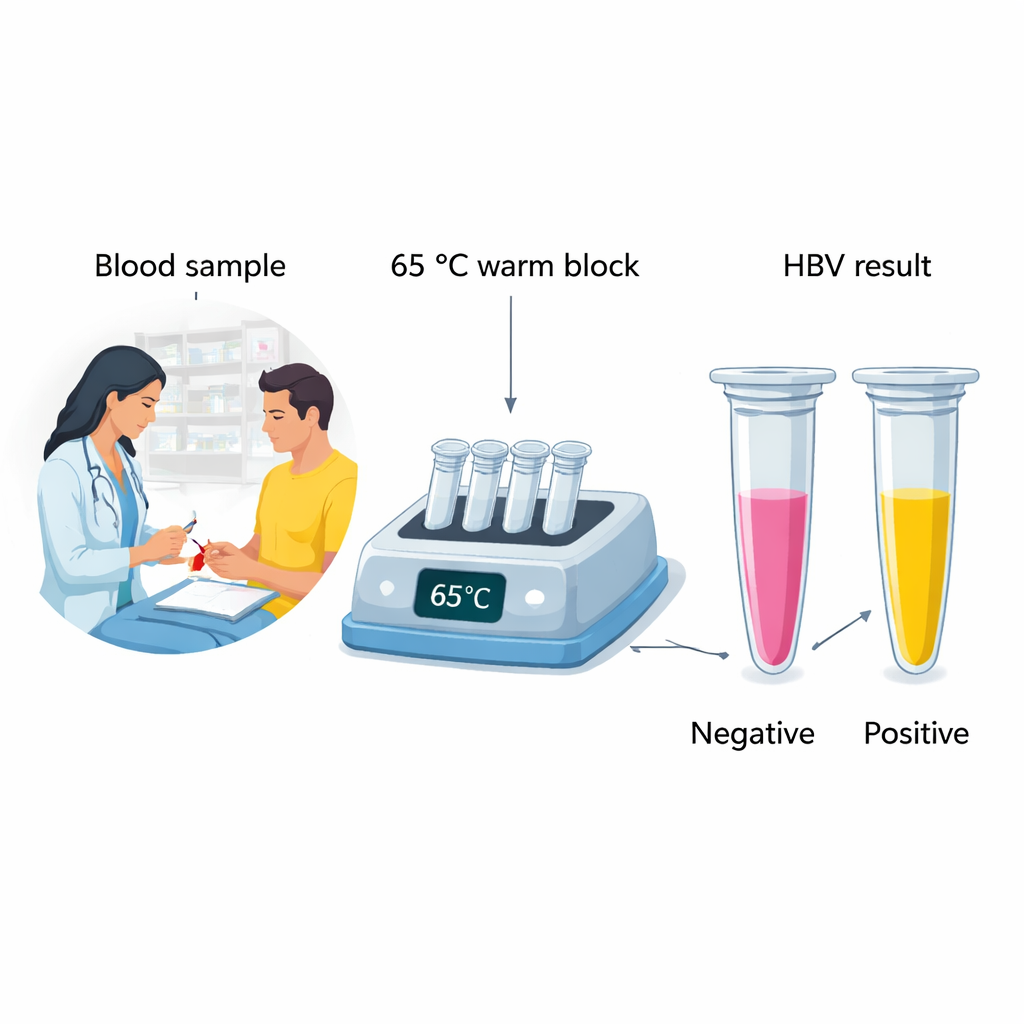
Checking That the Test Hits the Right Target
To be useful, the test must react only to HBV and not to other common blood-borne viruses. The team extracted genetic material from patient samples containing HBV, as well as from samples with HIV and hepatitis C virus (HCV), and from blood known to be virus-free. In the color-change LAMP assay, all HBV-positive samples turned yellow, while the HIV, HCV, and virus-free samples remained pink. When the researchers examined the reaction products on agarose gels, the telltale ladder-like pattern of LAMP products appeared only in HBV-positive tubes. These experiments showed that the assay was highly specific: it did not generate false positives from related infections.
How Little Virus the Test Can Detect
The study next asked how small an amount of HBV DNA the method could reliably pick up. Using serial dilutions of purified HBV DNA, the researchers tested concentrations from 100 down to 0.001 nanograms per microliter. Each level was run three times, and the outcome was judged both by eye (pink versus yellow) and by gel electrophoresis. The color change and gel bands were consistently present down to 10 nanograms per microliter, but not below. This value was defined as the limit of detection. In practical terms, this means the test is best suited for samples where the virus is present at moderate to high levels, which often coincide with active infection and a higher risk of spreading the virus to others.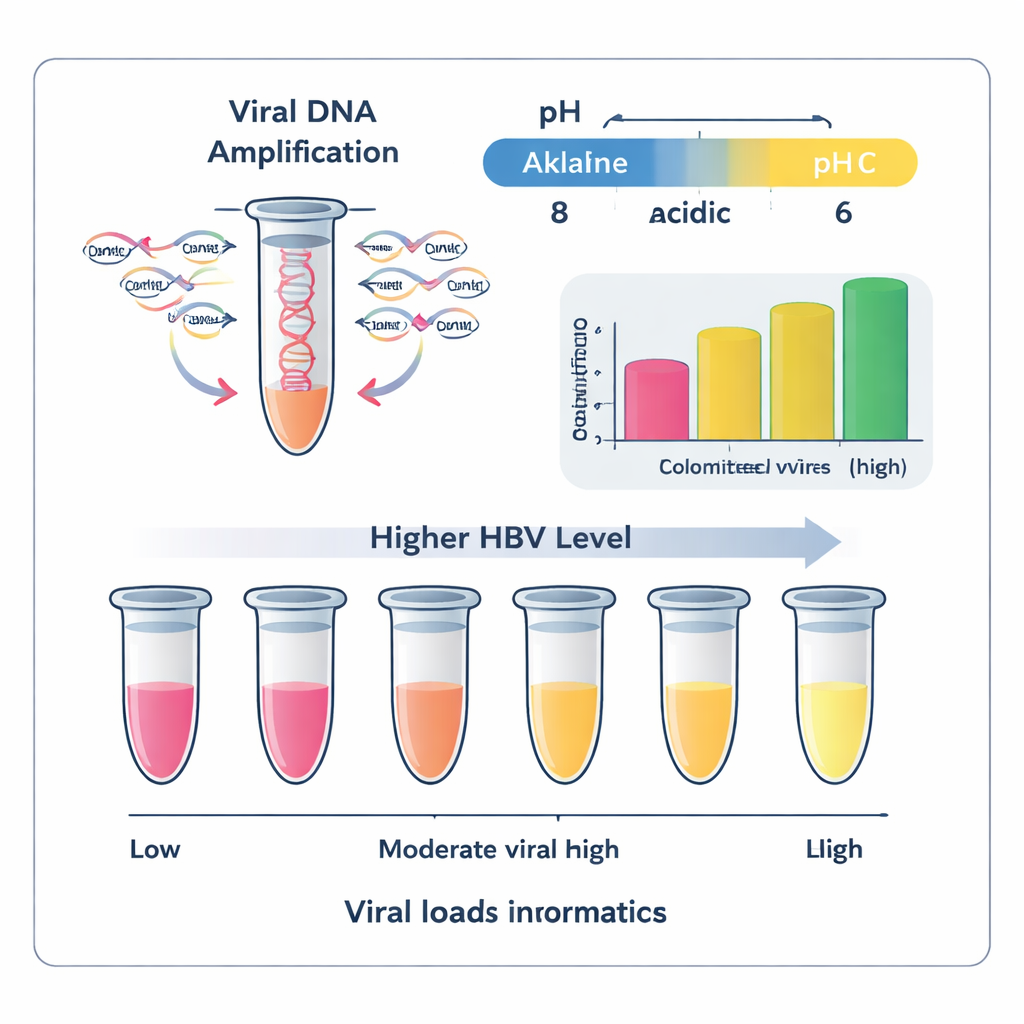
Performance in Real Patient Samples
To understand how the assay would perform in real-world screening, the team evaluated 200 plasma samples already confirmed as HBV-positive by a commercial real-time PCR system and 20 confirmed negative donor samples. Overall, the color-change LAMP detected 124 of the 200 positive cases, for a sensitivity of 62%, and correctly identified all 20 negative samples, for a specificity of 100%. When the data were broken down by viral load, a clearer picture emerged. For samples with very high viral loads, above 10,000 IU per milliliter, the test caught more than 90% of infections. Detection dropped sharply for samples with lower viral loads, reflecting the assay’s fixed detection limit. The high positive predictive value—every yellow tube corresponded to a true infection—means that a positive result can be trusted, while a negative result at low viral loads should still be double-checked by more sensitive methods where available.
What This Means for Patients and Health Systems
From a lay perspective, this work shows how a simple pink-to-yellow color shift in a plastic tube could help frontline clinics identify the people most likely to become seriously ill from hepatitis B or to pass the virus on. The test is inexpensive, runs in under an hour, and requires only a simple heater instead of large, costly machines and highly trained staff. While it does not replace sophisticated laboratory tests—especially for detecting very low levels of virus—it offers a practical way to expand HBV screening and monitoring in places that currently lack such tools. Wider use of this approach could support earlier diagnosis, guide treatment decisions for those with high viral loads, and ultimately aid efforts to reduce the global burden of hepatitis B.
Citation: Khan, S.J., Khamai, L., Kham-Kjing, N. et al. Colorimetric loop-mediated isothermal amplification for the rapid and visual detection of hepatitis B virus. Sci Rep 16, 2625 (2026). https://doi.org/10.1038/s41598-026-35503-8
Keywords: hepatitis B, rapid testing, point-of-care diagnostics, LAMP assay, colorimetric detection