Clear Sky Science · en
Automatic diagnosis of age-related macular degeneration using machine learning and image processing techniques
Why this matters for your eyesight
As people live longer, more of us face age-related macular degeneration (AMD), a disease that slowly erodes central vision and can make reading, driving, or recognizing faces difficult or impossible. Eye doctors can spot early warning signs in photographs of the back of the eye, but doing this by hand for thousands of patients is time‑consuming and requires specialized experts. This study explores how a transparent, machine‑learning–based tool can help catch AMD early from routine eye photos, without relying on fragile, hard‑to-explain deep‑learning "black boxes."
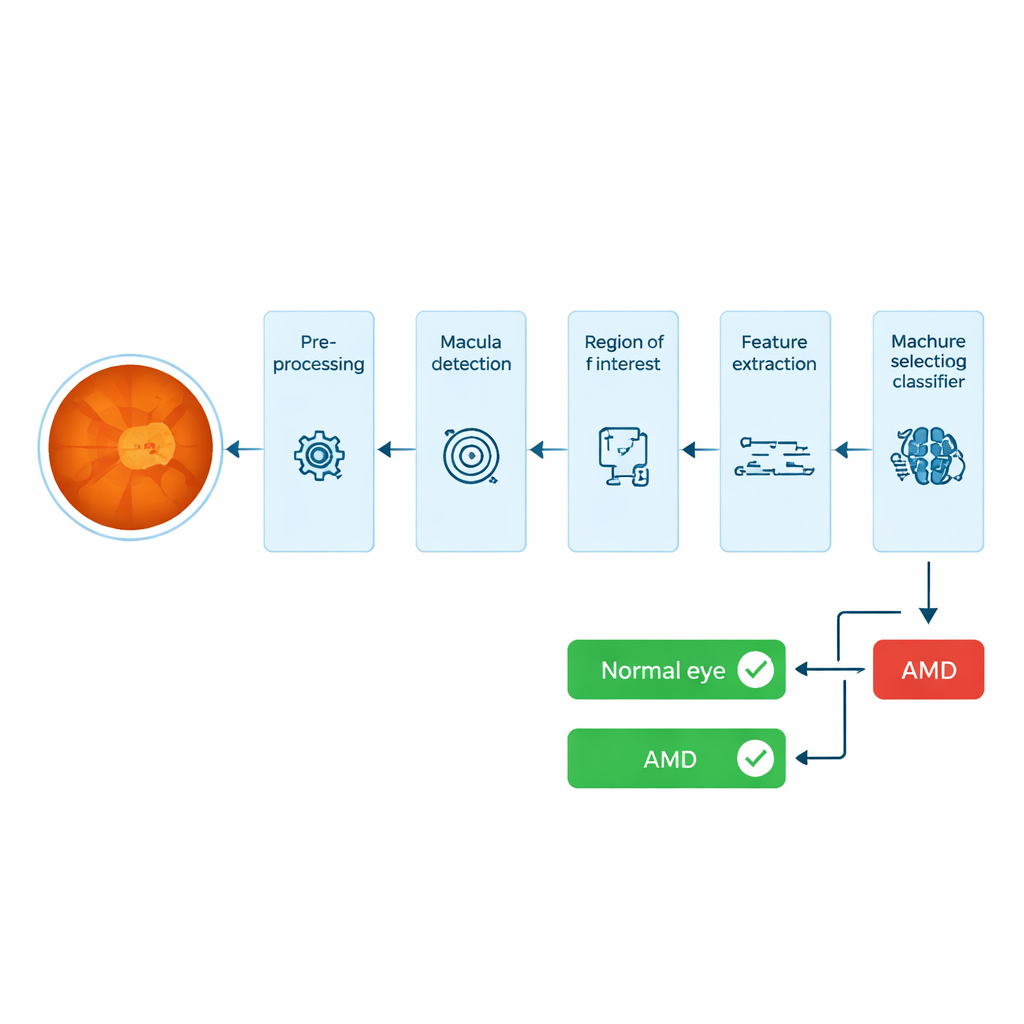
Looking for trouble in the eye’s sharp‑vision zone
AMD attacks the macula, a small dark spot near the center of the retina that provides sharp, detailed vision. Many automated systems try to find tiny fatty deposits called drusen in full‑eye images, but drusen can be easily confused with other bright spots such as small bleeds, and they vary a lot in shape and size. That makes them tricky to detect reliably by computer, and even experts must spend time carefully checking the results. The authors take a different route: instead of hunting directly for drusen across the whole retina, they focus on the macular region itself and measure how its texture and color change when AMD is present.
From raw photograph to the macula’s "fingerprint"
The system starts with a color photograph of the back of the eye, called a fundus image. It first enhances contrast using standard image‑processing steps so that dark and bright areas are easier to distinguish. Next, it automatically locates the optic disc—the bright circular area where nerves exit the eye—and uses its known geometric relationship to the macula to search along a narrow strip of the image for the darkest region that fits the expected size and position of the macula. Around this point, the system crops a small rectangle: this is the region of interest, containing the tissue most likely to reveal early AMD‑related damage.
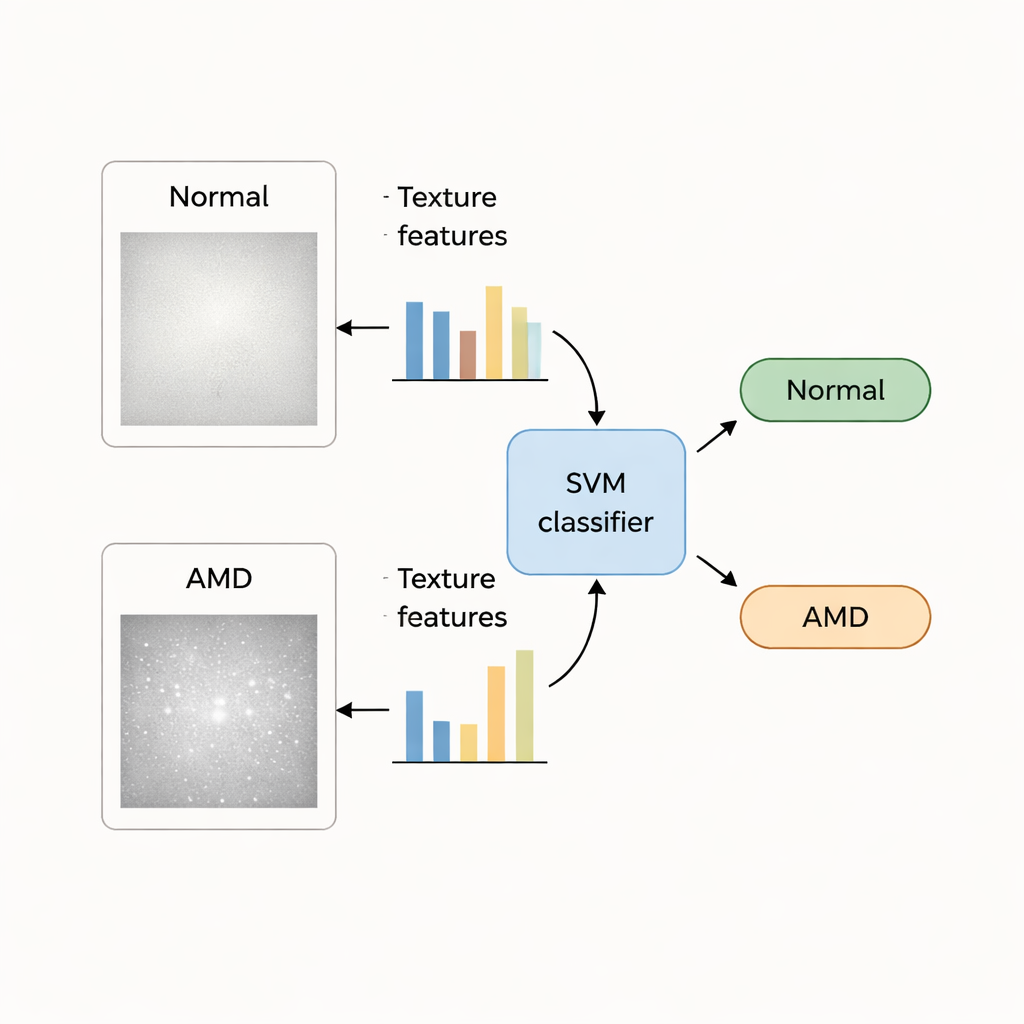
Turning patterns and colors into numbers
Within this macular patch, the researchers compute a large set of numerical descriptors, or "handcrafted features." Texture features capture how pixel intensities are arranged—whether the surface looks smooth, mottled, or irregular—while color features capture shifts in brightness and hue that may reflect changes in pigment and tissue health. In total, 140 texture and 48 color values are measured for each eye image. Because not all of these numbers are equally useful, the team applies statistical tests and a feature‑ranking method to select a smaller subset that best separates healthy and AMD eyes, trimming away redundant or noisy measurements.
Training the machines to say "AMD" or "normal"
With these selected features in hand, the authors train several well‑known machine‑learning classifiers—Support Vector Machine (SVM), k‑Nearest Neighbor, Naïve Bayes, and a simple neural network—to learn the difference between normal and AMD‑affected eyes. They use two public collections of retinal images: the STARE dataset, which includes 35 normal and 74 AMD images, and the larger ODIR dataset, with hundreds of labeled cases. To test reliability, they repeatedly split each dataset into training and testing portions, rotating through the images so that every eye serves as a test at least once, and then measure accuracy, error rate, and how often AMD is correctly detected.
Clear results and clearer reasoning
Across all tests, the SVM classifier using texture features from the macular region stands out. On the STARE dataset, it correctly distinguishes AMD from normal eyes nearly 99% of the time; on ODIR, accuracy is about 95%. Texture information proves more powerful than color alone, and combining both types of features does not surpass the performance of texture by itself. While some deep‑learning systems in the literature achieve comparable or slightly higher scores, they require large amounts of labeled data and offer little insight into what image cues they rely on. In contrast, the handcrafted texture and color features in this study correspond to recognizable structures in the retina, making the system more interpretable for clinicians.
What this means for patients
In everyday terms, the study shows that a relatively simple, transparent computer program can look at a standard eye photo, zoom in on the macula, and—with very high reliability—flag whether AMD is likely present, without first trying to trace every tiny deposit. Such a tool could help eye clinics and screening programs quickly sort large numbers of images, ensuring that patients with early disease are seen by specialists sooner, while also giving doctors a clearer view of which visual patterns the machine is using to make its call.
Citation: Agarwal, D., Bhargava, A., Alsharif, M.H. et al. Automatic diagnosis of age-related macular degeneration using machine learning and image processing techniques. Sci Rep 16, 5037 (2026). https://doi.org/10.1038/s41598-026-35428-2
Keywords: age-related macular degeneration, retinal imaging, machine learning, early disease detection, medical image analysis