Clear Sky Science · en
Diagnostic and immunological roles of leptin gene rs7799039 polymorphism and cytokines in COVID-19, HCV, and dual infection
Why your body’s fat hormone matters in viral infections
Why do some people get much sicker from viruses like COVID-19 or hepatitis C than others with similar age and weight? This study looks at a surprising part of the answer: a hormone made by body fat called leptin, along with three powerful immune signals in the blood. By tracking these molecules in people with COVID-19, hepatitis C virus (HCV), or both at once, the researchers searched for early warning markers that might flag high-risk patients and reveal how obesity and immunity are intertwined.
Connecting fat tissue, immunity, and two major viruses
Leptin is best known for telling the brain how much fat the body stores, helping control appetite. But leptin also behaves like an immune messenger, pushing the body toward a more inflammatory state. A common variation in the leptin gene, called rs7799039, changes a single DNA letter (from G to A) and can alter how much leptin the body makes. At the same time, other immune messengers—including interleukin-6 (IL-6), tumor necrosis factor‑alpha (TNF‑α), and interferon‑gamma (IFN‑γ)—are central players in how the body fights viruses and, when overproduced, how it damages its own tissues. The team set out to see how these signals and the leptin gene variant behave in people fighting COVID‑19, chronic HCV, or both infections together.
How the study was carried out
The researchers examined 228 adults in Egypt, divided into four equal groups: people with COVID‑19 only, people with chronic HCV only, people infected with both viruses, and healthy controls. All participants were broadly similar in age, sex, and body mass index; most were overweight or obese, which makes leptin particularly relevant. Each person gave a nasopharyngeal swab to test for COVID‑19 and a blood sample for HCV viral load, routine lab tests, and measurement of IL‑6, TNF‑α, and IFN‑γ. The leptin gene variant rs7799039 was determined from blood DNA, classifying people into three genotypes: GG, GA, or AA. The team then used statistical models to ask which blood markers best distinguished sick individuals from healthy ones and how genotypes were distributed across groups.
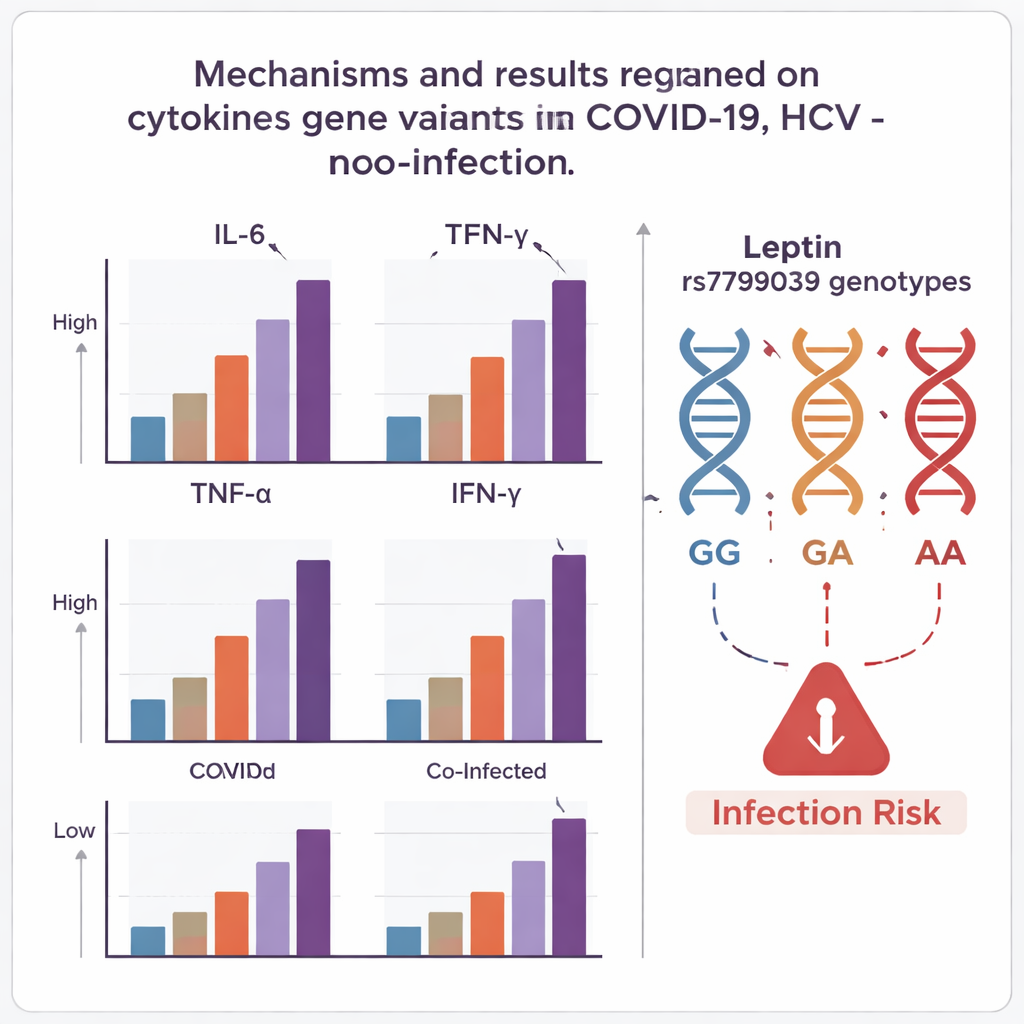
What the immune signals revealed
Levels of all three cytokines—IL‑6, TNF‑α, and IFN‑γ—were noticeably higher in every infected group than in healthy controls, and highest of all in people carrying both HCV and COVID‑19. IL‑6, a key driver of the so‑called “cytokine storm,” reached very high values in co‑infected and COVID‑19 patients, completely separating them from controls in this dataset. TNF‑α and IFN‑γ also rose, especially in co‑infected individuals, and TNF‑α in particular showed strong ability to distinguish patients from healthy people across all three diseases. Interestingly, the relationships among these cytokines differed by infection type: in HCV alone, they moved largely independently, but in co‑infection, TNF‑α and IFN‑γ rose and fell together, suggesting a stronger, more tightly linked inflammatory response when both viruses are present.
Leptin gene variants and who gets sick
The leptin gene told its own story. Across all participants, the GA genotype of rs7799039 was the most common. However, people with COVID‑19 or with both infections were more likely to carry at least one A version of the gene (GA or AA) than healthy controls. Those with the GG genotype—the form more often seen in the control group—appeared to be relatively protected, showing lower odds of having COVID‑19 or co‑infection. The AA genotype was somewhat more frequent in patients, but numbers were small and the link to disease was not statistically firm. Importantly, these genetic patterns held even after accounting for age, sex, and body weight, suggesting the leptin variant itself may shape susceptibility or the intensity of the immune response.
What this means for patients and care
Taken together, the findings point to TNF‑α as a consistently reliable blood marker that can help identify people with COVID‑19, HCV, or both, while IL‑6 and IFN‑γ provide additional clues that depend on the specific infection. The work also supports the idea that leptin—and the genes controlling it—links obesity with more intense inflammation during viral illness. For a layperson, the message is that your body’s fat hormone system and immune system are closely connected: certain leptin gene types and high inflammatory signals in the blood may help doctors spot who is at higher risk and who might benefit most from treatments that calm runaway inflammation, such as drugs targeting the IL‑6 pathway.
Citation: Sakr, A.A., Ahmed, A.E., Hasona, N.A. et al. Diagnostic and immunological roles of leptin gene rs7799039 polymorphism and cytokines in COVID-19, HCV, and dual infection. Sci Rep 16, 4361 (2026). https://doi.org/10.1038/s41598-026-35418-4
Keywords: COVID-19, hepatitis C, leptin, cytokines, genetic polymorphism