Clear Sky Science · en
Chronic spontaneous urticaria is associated with elevated serum zonulin levels
Why itchy hives might start in the gut
Many people live for months or even years with stubborn, unexplained hives that itch, burn, and disrupt sleep. This condition, called chronic spontaneous urticaria, can seriously reduce quality of life, yet doctors often cannot pinpoint a clear trigger. The study summarized here explores an emerging idea: that a "leaky" gut barrier and a gatekeeping molecule called zonulin may be part of the story behind these relentless rashes.
A common but mysterious rash
Chronic spontaneous urticaria (CSU) is defined by repeated outbreaks of itchy, raised wheals lasting longer than six weeks, sometimes accompanied by deeper swelling known as angioedema. Unlike hives caused by a clear allergy or physical trigger, CSU appears without an obvious cause and accounts for about two-thirds of chronic urticaria cases. It typically drags on for years and affects sleep, work, and everyday activities, creating a real emotional and financial burden for patients. Although immune cells in the skin called mast cells are known to be central players, the deeper reasons these cells become overactive remain poorly understood.
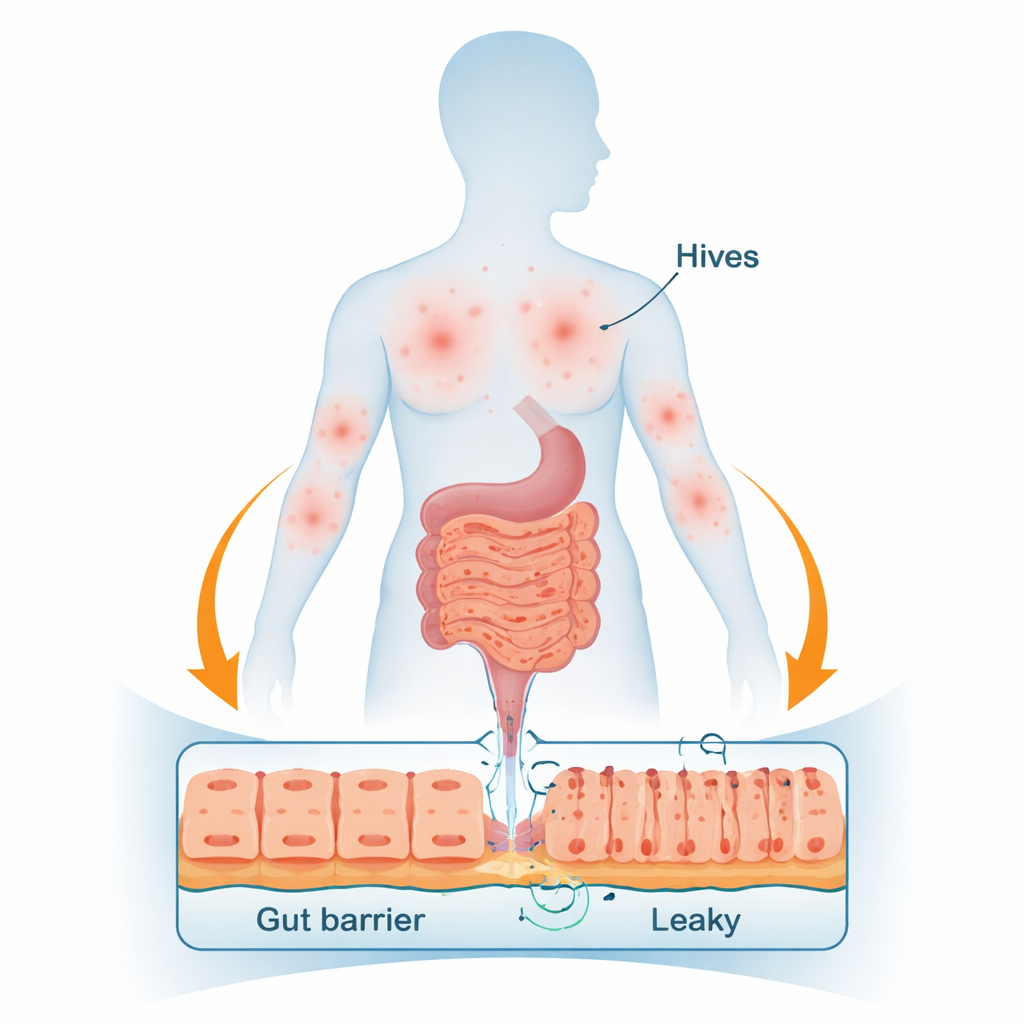
Linking a “leaky” gut to stubborn hives
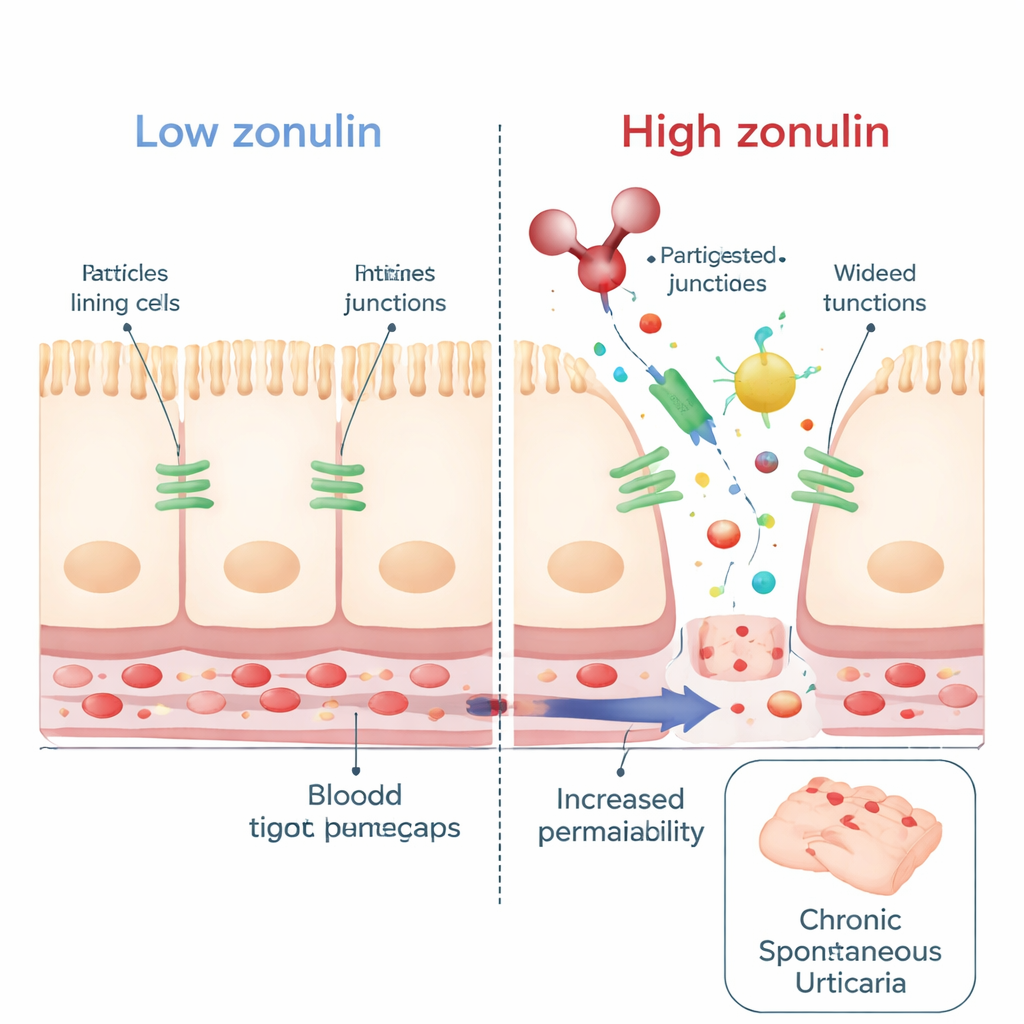
One leading theory is that CSU is, in many patients, an autoimmune condition: the immune system mistakenly targets parts of the body itself. Another piece of the puzzle is intestinal permeability—often nicknamed "leaky gut"—where the normally tight barrier lining the small intestine lets more substances slip into the bloodstream. Zonulin is a natural molecule that helps regulate the tight junctions between intestinal cells. Higher levels of zonulin in the blood have been linked to increased permeability and to autoimmune diseases such as celiac disease and type 1 diabetes. Because of this, the authors asked whether people with CSU might also show higher zonulin levels, hinting at a disturbed gut barrier that could feed into abnormal immune activity in the skin.
What the researchers actually measured
The team carried out a case–control study involving 65 adults with CSU and 65 healthy volunteers matched for age and sex. None of the participants had other known autoimmune or inflammatory diseases, major chronic illnesses, or recent infections, and they avoided factors that might confound gut health, such as recent antibiotic or probiotic use. Blood samples were collected after fasting and analyzed in the laboratory with a technique called ELISA to determine serum zonulin levels. For the patients, the researchers also recorded disease activity over a week using a standard urticaria activity score, along with information about weight, smoking, presence of angioedema, and whether they also had chronic inducible urticaria triggered by physical factors such as scratching (symptomatic dermographism).
Higher zonulin, but not necessarily worse symptoms
On average, people with CSU had clearly higher zonulin levels in their blood than healthy controls (about 132 vs 83 picograms per milliliter), a difference that was statistically strong. Within the CSU group, those who also had inducible forms of urticaria showed especially high zonulin levels compared with patients whose hives were purely spontaneous. However, zonulin levels did not track with how severe the hives were, how long the disease had lasted, or with other clinical factors such as body mass index, total IgE levels (a common allergy marker), smoking, or Helicobacter pylori infection. These findings suggest that altered intestinal barrier function may be more closely tied to certain subtypes or patterns of chronic hives than to day-to-day symptom intensity.
What this could mean for patients
The authors caution that zonulin is an imperfect stand-in for gut permeability, because common test kits detect a family of related proteins, not only the classic intestinal form. The study was also relatively small, and many patients were already on treatment, which might influence both symptoms and lab values. Even so, the consistent elevation of zonulin in CSU—particularly in those with inducible hives—adds weight to the idea that the gut barrier and skin inflammation are linked. Rather than proving that a leaky gut causes hives, the work points to a two-way relationship in which immune mediators released from skin mast cells could further loosen the gut barrier, and gut-derived signals might, in turn, fuel ongoing immune misfires in the skin.
Take-home message for non-specialists
For someone living with chronic, unexplained hives, this research offers a new angle on why the problem persists. People with CSU in this study had higher blood levels of zonulin, a molecule tied to how tightly the cells of the gut wall are sealed together. This supports the idea that, at least in some patients, the gut lining is more permeable than usual and may be involved in driving or maintaining the disease. While doctors are not yet ready to treat CSU by directly targeting zonulin or the gut barrier, future studies may explore whether adjusting intestinal permeability—through diet, medications, or other strategies—could become part of a more complete treatment plan for these difficult, long-lasting hives.
Citation: Solak Esen, B., Erkayman, M.H. Chronic spontaneous urticaria is associated with elevated serum zonulin levels. Sci Rep 16, 5812 (2026). https://doi.org/10.1038/s41598-026-35394-9
Keywords: chronic spontaneous urticaria, zonulin, intestinal permeability, leaky gut, autoimmune skin disease