Clear Sky Science · en
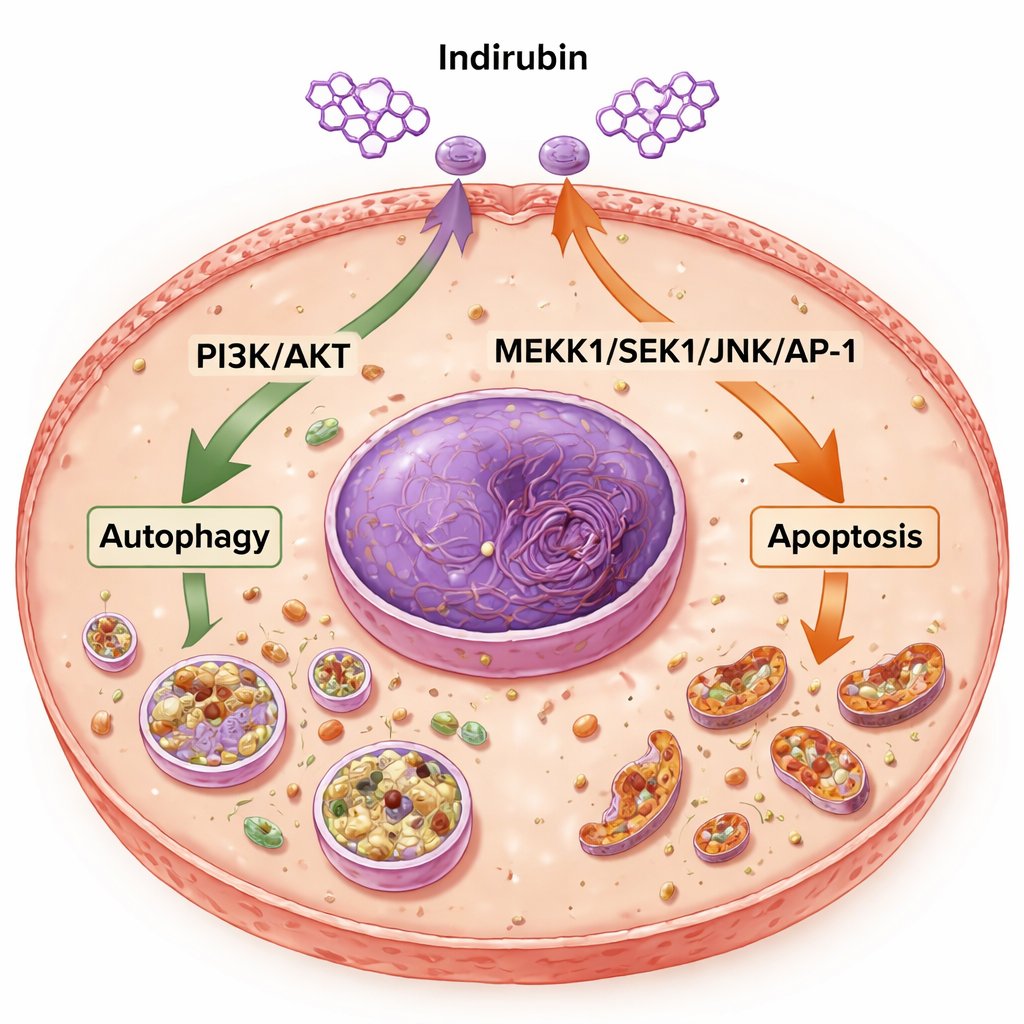
Indirubin treatment was associated with modulation of the PI3K/AKT and MAPK pathways and induction of apoptosis and autophagy
A new twist in cervical cancer treatment
Cervical cancer remains one of the leading causes of cancer death in women worldwide, and current treatments like surgery, chemotherapy and radiation can be harsh and sometimes ineffective in advanced disease. This study explores whether indirubin, a natural compound derived from a traditional Chinese medicine, can slow cervical cancer growth and kill cancer cells while acting through well-known cellular survival switches inside tumors. For readers, it offers a glimpse of how an old remedy might be reshaped into a modern, more targeted cancer therapy.
Why a plant pigment caught scientists’ attention
Indirubin is a pigment found in indigo naturalis, a preparation long used in traditional Chinese medicine. Earlier research showed it can curb the growth of several types of cancer cells, but how it works in cervical cancer was not well understood. The authors focused on two major control systems inside cells. One is the PI3K/AKT pathway, often described as a growth and survival “on switch” in many tumors. The other is part of the MAPK family of pathways, specifically a chain called MEKK1/SEK1/JNK/AP-1, which helps cells decide whether to adapt to stress or die. By examining these switches, the team hoped to see whether indirubin could push cervical cancer cells away from survival and toward self-destruction.
Testing indirubin in mice and human cancer cells
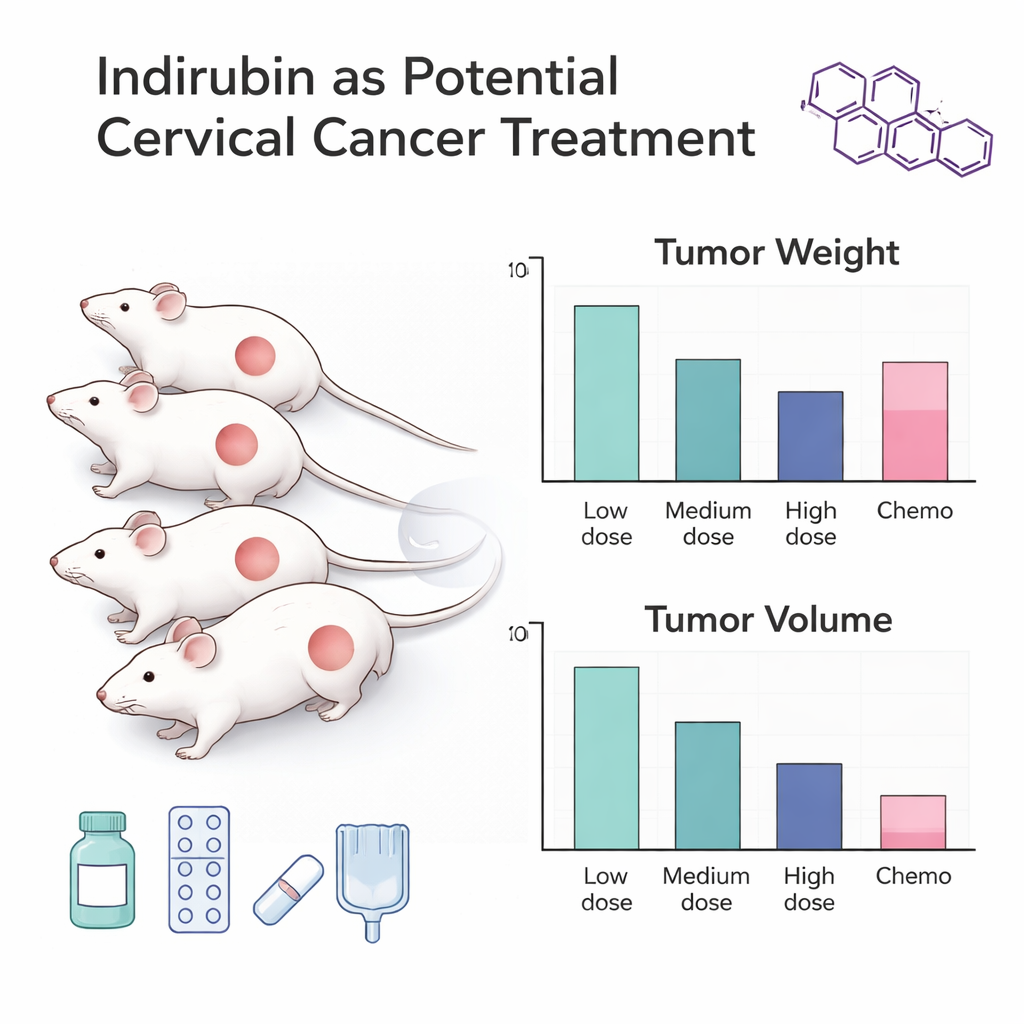
To probe indirubin’s effects, researchers ran two main sets of experiments. In mice, they implanted cervical cancer cells under the skin and treated the animals with different doses of indirubin or with standard chemotherapy drugs. In the lab, they treated HeLa cells—a well-established cervical cancer cell line—with increasing concentrations of indirubin and then measured how many cells survived, how many went into programmed cell death (apoptosis), and how well the cells activated their internal “self-cleaning” process, known as autophagy. They also tracked mouse weight and carefully followed animal welfare rules to ensure that any anti-tumor effects were not simply due to general toxicity.
Slowing tumors and triggering cell suicide
In mice, indirubin clearly shrank tumors in a dose-dependent fashion: higher doses led to much lighter and smaller tumors, yet the animals maintained normal body weight, suggesting the drug did not cause serious systemic harm. In cell culture, indirubin reduced the number of living HeLa cells over time and with rising doses. At its highest tested levels, indirubin killed more cervical cancer cells than standard chemotherapy agents such as cisplatin and ifosfamide. Flow cytometry, a technique that sorts and counts cells, revealed that indirubin-treated cells were much more likely to be in early or late stages of apoptosis, meaning the compound strongly encouraged cancer cells to undergo controlled self-destruction instead of continuing to divide.
Rewiring the cell’s survival circuits
Digging deeper, the team showed that indirubin changed the balance of key proteins that control cell fate. It boosted markers of autophagy, indicating the cells’ recycling machinery was more active, while reducing levels of p62, a protein that usually falls when this process ramps up. At the same time, indirubin dampened the activity of the PI3K/AKT pathway—both at the level of gene messages and through reduced phosphorylation, the chemical “on” signal on these proteins. The drug also lowered levels of BCL2, a protein that blocks cell death, and raised levels of Bax, a pro-death partner, tipping the scales toward apoptosis. In tumor tissues from mice, indirubin similarly suppressed the MEKK1/SEK1/JNK/AP-1 pathway, suggesting it was turning down another stress-response route that tumors exploit to survive and spread.
What this could mean for future patients
For non-specialists, the main message is that indirubin, a compound rooted in traditional medicine, was able to slow cervical cancer growth and push cancer cells toward self-cleaning and self-destruction by turning off powerful internal survival switches. It did this in both animal models and cultured cells, and it did so without obvious harm to the mice. While these findings are still preclinical and far from routine use in the clinic, they provide a scientific foundation for further studies and eventually human trials. If future research confirms its safety and effectiveness, indirubin or related compounds could one day join the toolbox of targeted treatments that make cervical cancer therapy more precise and less punishing.
Citation: Xie, X., Liu, C., Liu, X. et al. Indirubin treatment was associated with modulation of the PI3K/AKT and MAPK pathways and induction of apoptosis and autophagy. Sci Rep 16, 5155 (2026). https://doi.org/10.1038/s41598-026-35382-z
Keywords: cervical cancer, indirubin, traditional Chinese medicine, cell signaling pathways, apoptosis and autophagy