Clear Sky Science · en
Epidemiologic survey of ulcerative colitis and crohn’s disease in Japan using claim data
Hidden Patients Behind Everyday Stomach Troubles
Chronic gut diseases like ulcerative colitis and Crohn’s disease can turn daily life into a struggle with pain, urgent bathroom trips, and fatigue. In Japan, these illnesses are officially labeled “intractable,” meaning they are difficult to cure and demand long‑term care. Yet national statistics may be missing a large share of people quietly managed in neighborhood clinics rather than big hospitals. This study asks a simple but important question: how many patients are we overlooking, and what does that mean for understanding and planning care for these conditions?
Two Serious Gut Diseases in Focus
Ulcerative colitis and Crohn’s disease are long‑lasting inflammations of the digestive tract, grouped under the umbrella of inflammatory bowel disease. Ulcerative colitis mainly affects the lining of the large intestine, while Crohn’s disease can involve the entire digestive tract and often causes deeper damage, including narrowings and fistulas. Both lead to symptoms such as diarrhea, abdominal pain, and bloody stools, and many patients need ongoing medication and regular monitoring. Because they are designated as hard‑to‑treat conditions in Japan, the government runs periodic nationwide surveys to track how common they are.
Why National Counts May Fall Short
The official nationwide survey in 2014 estimated that roughly 220,000 people in Japan had ulcerative colitis and about 71,000 had Crohn’s disease. However, that survey collected information only from hospitals, based on the assumption that patients with serious, rare diseases would mainly be seen at large institutions such as university hospitals. As the number of patients has grown, though, more people have begun receiving care at smaller clinics closer to home. If these clinic‑only patients are not counted, national policies and funding may be based on an incomplete picture of how many people actually live with these illnesses.
Mining Insurance Records for a Clearer Picture
To fill this gap, the researchers turned to a large health insurance claims database covering about 8 million employees and their families—roughly 6% of Japan’s population. Claims records capture every insured visit to a hospital or clinic, along with diagnosis codes, tests, treatments, and drug prescriptions. By searching for specific international disease codes for ulcerative colitis and Crohn’s disease, the team estimated how many people were treated for each condition in 2014, 2016, 2018, and 2020. They also checked whether each person had visited a hospital, a clinic, or both, and compared the characteristics and yearly medical costs of ulcerative colitis patients who went only to clinics versus those who had hospital care.
Many Patients Rely Only on Clinics
The claims data showed that in 2014 there were 227.9 people with ulcerative colitis and 58.2 people with Crohn’s disease per 100,000 insured individuals—slightly higher than the national survey’s figures. Crucially, about one‑third of ulcerative colitis patients (around 32–35%, rising to nearly 38% by 2020) received care only at clinics, with no hospital visits at all. For Crohn’s disease, the share of clinic‑only patients was smaller, around 12%, and stayed fairly stable over time. When the researchers recalculated the ulcerative colitis rate using only patients who had hospital visits, the result closely matched the official survey. This suggests the earlier nationwide count was accurate for hospital‑treated patients but underestimated the total number of people living with ulcerative colitis by leaving out the clinic‑only group.
Who Are the Clinic‑Only Patients?
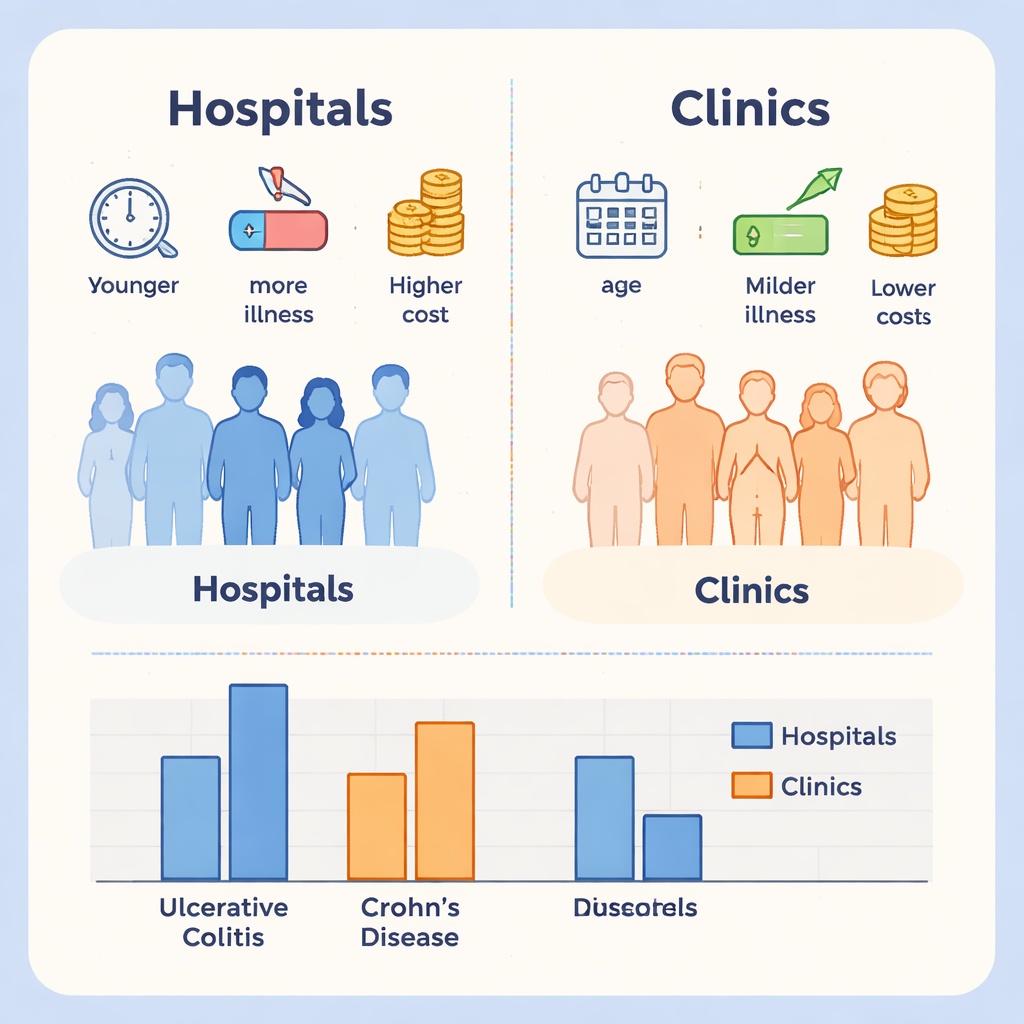
Looking more closely at ulcerative colitis patients in 2014, the study found that those treated only at clinics tended to be older, had fewer additional health problems, and incurred lower yearly treatment costs than patients seen at hospitals. This pattern fits with the idea that clinics often manage people with milder or more stable disease, while hospitals care for those needing intensive tests, complex treatments, or expensive drugs such as biologic therapies. The data also showed that very few patients were treated outside the main departments of internal medicine, surgery, and pediatrics, and that only a small fraction visited multiple departments, supporting the structure of existing national surveys.
What This Means for Patients and Policy
For people living with ulcerative colitis or Crohn’s disease, these findings underscore that many patients are managed in local clinics and may not be visible in headline national statistics. For ulcerative colitis in particular, the true number of patients in Japan is likely higher than official counts that focus only on hospitals. Recognizing this hidden population is important for planning specialist services, budgeting for medications, and ensuring that clinic‑based care is adequately supported. By tapping into routinely collected insurance claims, the study offers a more realistic view of how these chronic gut diseases are treated across the health system—and highlights the need to include clinics when measuring the full burden of intractable illnesses.
Citation: Shitara, Y., Maeda-Minami, A., Ishikawa, H. et al. Epidemiologic survey of ulcerative colitis and crohn’s disease in Japan using claim data. Sci Rep 16, 5158 (2026). https://doi.org/10.1038/s41598-026-35336-5
Keywords: ulcerative colitis, Crohn’s disease, Japan, epidemiology, claims data