Clear Sky Science · en
Assessment and treatment of metabolic acidosis in CKD: a registry-based study
Why acid balance matters for people with kidney trouble
People with chronic kidney disease often focus on blood pressure, sugar levels, and dialysis, but few hear about the body’s acid balance. This study shows that a subtle problem called metabolic acidosis—too much acid and not enough natural buffer in the blood—may be quietly harming many kidney patients in Japan, while rarely being checked or treated. Because fixing it can be as simple as changing diet or taking baking-soda–like tablets, understanding how often it is missed has real consequences for everyday care.
A quiet complication of failing kidneys
Healthy kidneys help keep our blood’s acidity within a narrow, safe range. When kidneys are damaged, they struggle to clear acids made by normal metabolism and modern diets rich in animal protein and low in fruits and vegetables. The result can be metabolic acidosis, which has been linked to weaker bones, loss of muscle and appetite, worse blood sugar control, and a faster slide toward kidney failure and heart problems. International and Japanese kidney guidelines now advise correcting low bicarbonate levels, the blood’s main “antacid,” once they drop below a certain threshold.
Using big data to take a nationwide snapshot
To see how well this advice is followed in real life, researchers analyzed records from the Japan Chronic Kidney Disease Database Extension, which gathers laboratory tests, diagnoses, and prescriptions from 21 university hospitals across the country. They focused on more than 179,000 adults with moderate to severe kidney disease (stages 3a to 4) seen between 2014 and 2021. The team asked four simple questions: How often is serum bicarbonate measured? Among those checked, how common is metabolic acidosis? And when acidosis appears on paper, how often is it formally diagnosed and treated?
Tests and treatment rarely reach most patients
The first striking finding was how seldom bicarbonate was measured at all. In any given year, fewer than one in ten patients had this test recorded, even though all had chronic kidney disease. Testing was somewhat more common in advanced disease, yet even in stage 4 only about one in five patients were checked annually. Among the 22,309 people who ever had bicarbonate measured, acidosis—defined as a level below 22 mEq/L—was surprisingly frequent: it appeared in about 44 percent overall, and in nearly two thirds of those with the worst kidney function (stage 4). Despite this, only 8.6 percent of patients with low bicarbonate carried a diagnostic code for metabolic acidosis, and just 7.5 percent received sodium bicarbonate tablets, the standard alkalizing treatment.
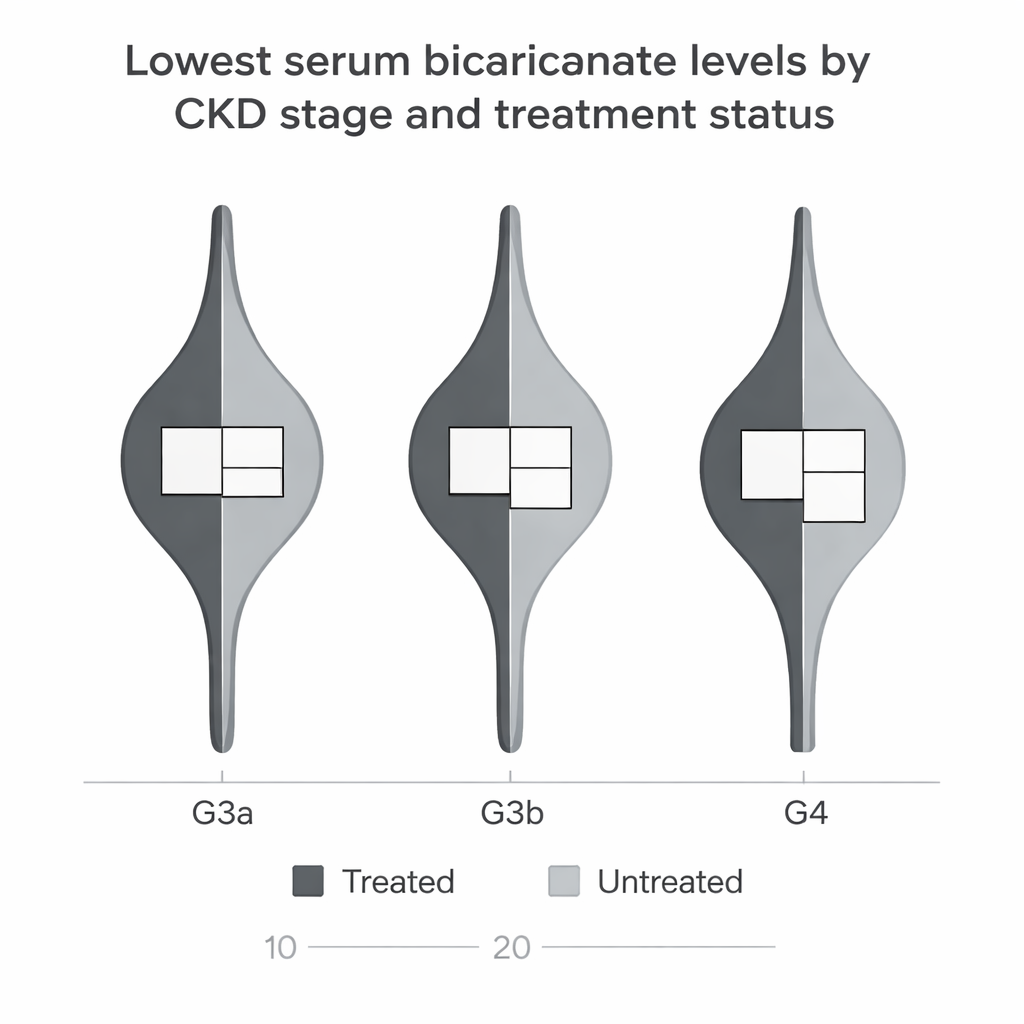
Who gets checked, and what the numbers reveal
Patients who had bicarbonate measured tended to be older, have poorer kidney function, more protein in their urine, and more other illnesses such as diabetes and heart failure. In other words, doctors appeared to reserve acid–base testing for more complex, fragile patients, not for the broader kidney population. Even within this high‑risk group, many with low bicarbonate were left untreated. Those who did receive alkali therapy had very low levels on average, close to the newest international guideline threshold at which doctors are urged to take action. This pattern suggests that treatment is often delayed until acidosis is quite severe, and milder cases—where intervention may slow kidney decline—are commonly overlooked.
What this means for patients and their care
The study concludes that metabolic acidosis is both common and under-recognized among Japanese people with chronic kidney disease. Simple blood tests to check bicarbonate are performed infrequently, and even clear-cut abnormalities seldom lead to a diagnosis or treatment. Yet a growing body of research indicates that correcting acid buildup, through diet rich in fruits and vegetables or through prescribed alkali tablets, can help preserve kidney function and may lower the risk of serious complications. For patients and clinicians alike, the message is straightforward: asking about and monitoring acid balance should become a routine part of kidney care, not an afterthought.
Citation: Tanaka, M., Hosojima, M., Kabasawa, H. et al. Assessment and treatment of metabolic acidosis in CKD: a registry-based study. Sci Rep 16, 5104 (2026). https://doi.org/10.1038/s41598-026-35335-6
Keywords: chronic kidney disease, metabolic acidosis, bicarbonate, kidney function decline, alkali therapy