Clear Sky Science · en
Investigation of thoracico-abdominal infrared thermal imaging characteristics in patients with cervical HR-HPV infection
Why body heat can reveal hidden cervical infections
Most people think of a fever thermometer when they hear about body temperature, but heat patterns on the skin can quietly reflect what is happening deep inside. This study explores whether a camera that “sees” infrared heat on the chest and belly can pick up subtle changes in women infected with high‑risk types of human papillomavirus (HPV), the virus responsible for nearly all cases of cervical cancer. If reliable patterns exist, this noninvasive approach could someday complement standard screening and help doctors better understand how the body reacts to HPV.
A closer look at HPV and women’s health
HPV is one of the most common viral infections in women worldwide; most women will encounter it at least once. A subset of “high‑risk” types, known as HR‑HPV, can lead to precancerous changes and cervical cancer if the infection persists. There is no medicine that simply clears HR‑HPV, so doctors rely on regular screening to catch early changes in cervical cells. The research team, working within both Western medicine and traditional Chinese medicine, wondered whether HR‑HPV might also leave a broader footprint on the body’s energy use and blood flow, especially in the pelvic area where the infection occurs. That idea led them to test medical infrared thermal imaging, a technology that converts invisible heat radiation from the skin into a color map of surface temperature.
How the thermal camera was used
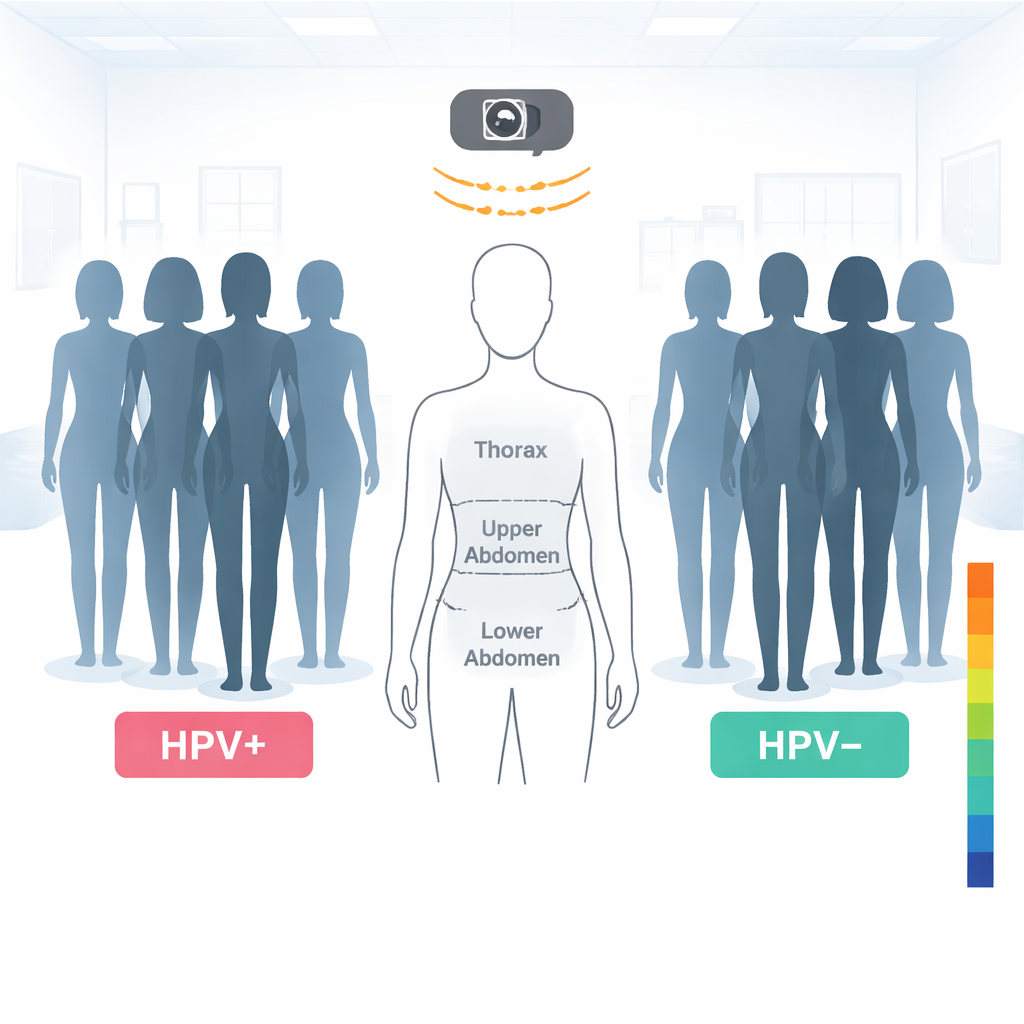
The investigators recruited two groups of women aged 25 to 60 from a hospital in Beijing: 68 women with confirmed high‑risk cervical HPV infection and 65 women whose cervical HPV tests were negative. All participants followed strict pre‑scan rules designed to keep temperature readings stable—for example, avoiding heavy exercise, hot or cold environments, and stimulants before the test, and resting quietly in a controlled room. During the exam, women removed clothing and accessories, stood in front of the infrared camera, and had images taken of the entire chest and abdomen. The researchers then divided each image into specific regions of interest: the thorax, upper abdomen, and lower abdomen, and within the lower abdomen three smaller zones, including a left lower area, an area over the uterus, and a right lower area. Using specialized software, they calculated the average temperature in each zone.
What the heat maps revealed
In women without HPV, the thermal images looked smooth and symmetrical, with a gentle decrease in temperature from the chest to the upper and then lower abdomen. In contrast, women with high‑risk HPV showed disrupted patterns. Their images displayed more uneven colors and visible “hot spots,” especially patches and clusters of higher temperature in the lower abdomen. When the team compared the numbers, the overall lower abdominal skin temperature was higher in HPV‑positive women than in healthy participants, even though the general chest‑to‑belly gradient was similar in both groups. The temperature difference was modest—on the order of a few tenths of a degree Celsius—but consistent enough to reach statistical significance, particularly in the lower left abdominal region.
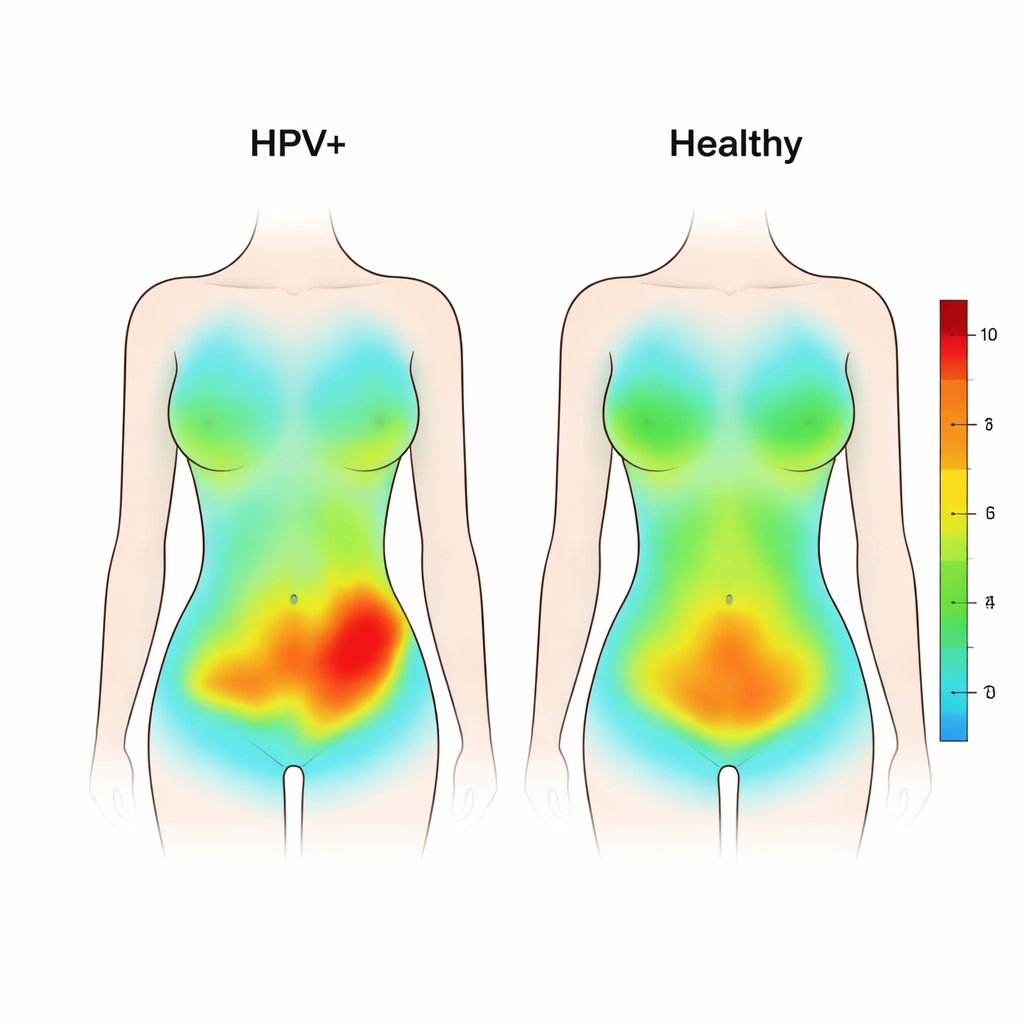
Uneven warmth and possible hidden processes
Looking more closely at the three sub‑areas of the lower abdomen, both groups showed a pattern where the left side tended to be slightly warmer than the right, and the area over the uterus was coolest. However, the left‑side warmth was noticeably greater in the HPV‑positive group, and the difference between the left and right sides of the lower abdomen was larger overall. This stronger left‑right imbalance suggests an underlying disturbance in local blood flow, metabolism or mild inflammation, although the study could not prove the exact cause. The authors note that nearby organs such as parts of the colon and small intestine also lie in this region, and they speculate that HPV‑related changes in immune responses or the local microbiome might help explain the altered heat patterns. At the same time, they caution that the absolute temperature changes remain within the normal range of human variation, so any clinical impact is still uncertain.
What this could mean for future care
For a layperson, the takeaway is that a special heat‑sensing camera can detect small but consistent differences in how warmth is distributed across the lower abdomen in women with high‑risk cervical HPV infection compared with women without the virus. These differences, especially the warmer and more irregular pattern on the lower left side, may reflect how the body’s circulation and metabolism respond to infection, even before serious disease develops. Infrared thermal imaging is painless and noninvasive, so with further research it might become a helpful companion tool alongside Pap tests and HPV testing, offering an additional, visual way to track treatment responses or study how different HPV subtypes affect the body. For now, it should be viewed as an early research tool rather than a stand‑alone test for diagnosis, but it opens an intriguing window into the subtle ways infections can reshape the body’s thermal landscape.
Citation: Li, X., Sun, L., Qiu, M. et al. Investigation of thoracico-abdominal infrared thermal imaging characteristics in patients with cervical HR-HPV infection. Sci Rep 16, 6500 (2026). https://doi.org/10.1038/s41598-026-35261-7
Keywords: cervical HPV, infrared thermography, cervical cancer screening, skin temperature, women’s health