Clear Sky Science · en
Clinical evaluation and comparative study of a fully automated erythrocyte osmotic fragility analysis system based on scatter turbidimetry
Why a blood test like this matters
Red blood cells carry oxygen to every corner of the body, and when they break apart too easily, people can develop serious forms of anemia. Doctors use a laboratory test called erythrocyte osmotic fragility to see how sturdy these cells are, but the classic version of this test is slow, hands-on, and tricky to standardize. This study reports on a new, fully automated system that performs the same check far more quickly and consistently, raising the prospect of faster, more reliable screening for hemolytic (cell-breaking) blood disorders in everyday hospitals and clinics.
A gentler stress test for red blood cells
The osmotic fragility test asks a simple question: how easily do red blood cells burst when placed in a watery, salt-poor solution? Healthy cells can swell without bursting right away, while fragile cells rupture sooner, spilling their contents. Doctors rely on this behavior to help diagnose conditions such as hereditary spherocytosis, autoimmune hemolytic anemia, and some forms of thalassemia and iron deficiency anemia. Traditionally, laboratory staff mix blood by hand into a series of salt solutions, wait for cells to burst, and then measure how cloudy the liquid becomes. This approach works but is time-consuming, requires careful technique, and can vary from one operator or lab to another.
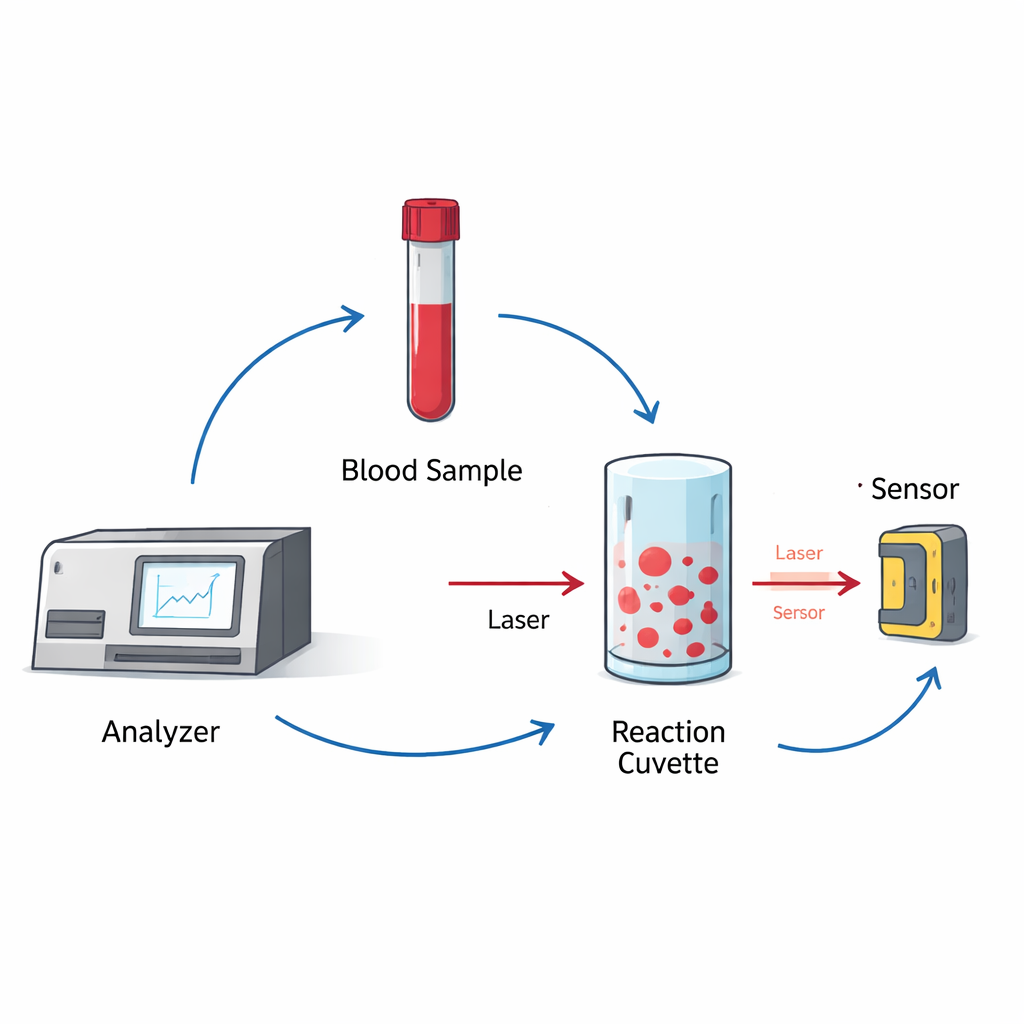
Turning light scattering into a push-button test
The new system, developed by Shenzhen Pumen Technology, replaces much of this manual work with optics and automation. A small volume of well-mixed whole blood is added to a specialized reagent in a reaction cup inside the analyzer. A focused laser beam passes through the mixture, and the red blood cells scatter the light in patterns that change as cells swell and burst. A light-sensitive detector captures these changes and converts them into electrical signals that the instrument’s software interprets as a measure of cell fragility. The device handles mixing, timing, and reading automatically and can process many samples per hour, cutting the per-sample time roughly in half compared with the older spectrophotometer-based method.
Putting the new machine to the test
To find out whether the automated system can stand in for the traditional one, the researchers tested 112 blood samples from people ranging in age from infancy to old age, including both healthy individuals and patients with different severities of anemia. Every sample was run on the new analyzer and on a well-established spectrophotometer method from a different manufacturer, under tightly controlled conditions and with routine quality checks. The team then used several statistical tools to see how closely the two sets of results matched—looking at simple correlation, whether the two methods classified samples the same way, and how large any differences were around clinically important decision points used by doctors.
Very close agreement with the old standard
The automated and traditional methods proved to be remarkably similar. When plotted against each other, measurements from the new device lined up almost perfectly with those from the reference system, with a correlation close to one and a regression line nearly identical to the ideal one-to-one line. In practical terms, the analyzer never disagreed with the traditional method about whether a result fell into a normal or abnormal range, giving a statistical agreement score (Kappa) of 1.00, which represents perfect consistency. A more detailed bias analysis showed that nearly all paired measurements fell within narrow, clinically acceptable limits, including around key thresholds that doctors might use to decide whether a patient needs further investigation or treatment.
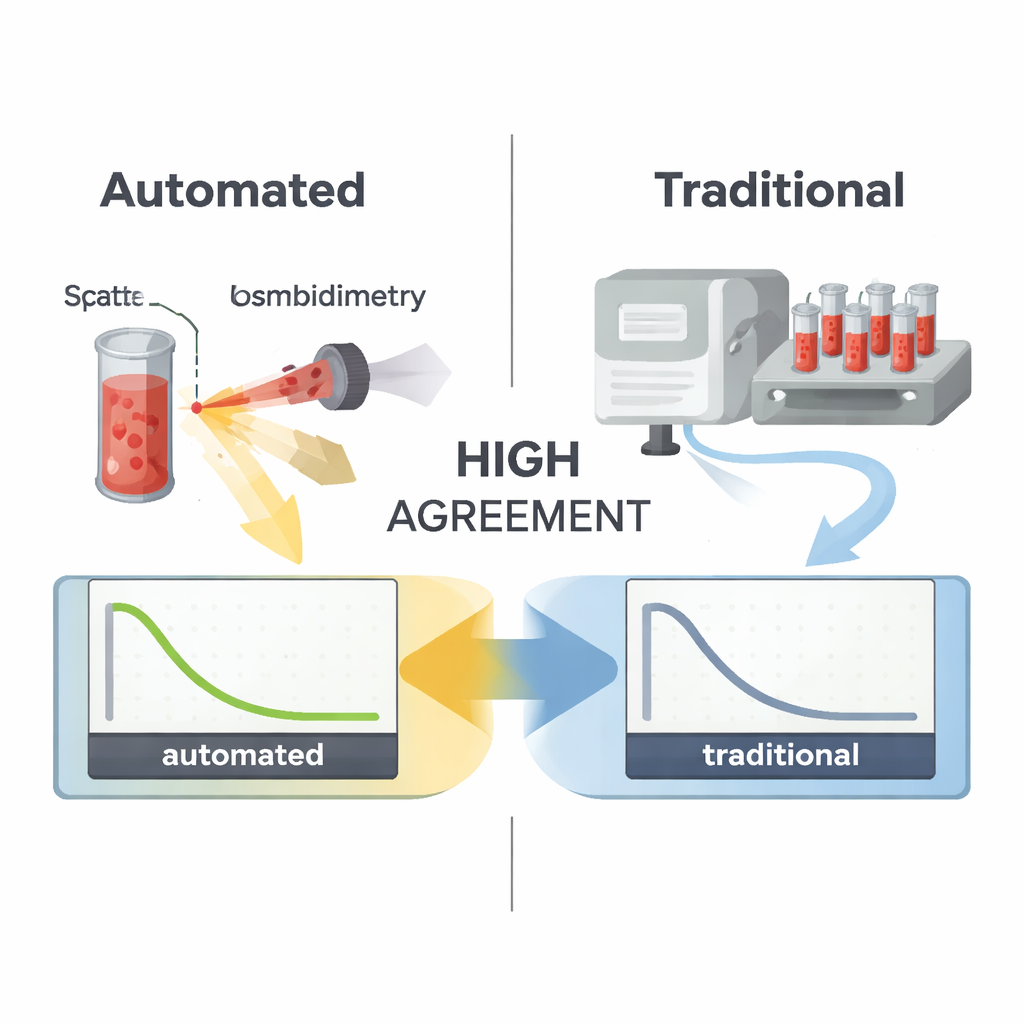
What this means for patients and clinics
For patients, the most important message is that a faster, more hands-off version of an established red blood cell test can deliver results that closely mirror the traditional gold standard. For busy laboratories, the new system’s automation can reduce human error, standardize results between operators, and boost throughput, making it especially useful for large-scale screening programs for anemia and hemolytic diseases. While the authors note that larger, multi-center studies and tests in rare blood disorders are still needed, their data suggest that this automated light-scattering approach is ready to move from research into routine use, helping clinicians diagnose red blood cell problems more efficiently and reliably.
Citation: Ma, L., Huang, Y., Chen, T. et al. Clinical evaluation and comparative study of a fully automated erythrocyte osmotic fragility analysis system based on scatter turbidimetry. Sci Rep 16, 4787 (2026). https://doi.org/10.1038/s41598-026-35163-8
Keywords: red blood cells, anemia screening, automated blood testing, hemolytic disorders, laboratory diagnostics