Clear Sky Science · en
Radiomics analysis of early pregnancy ultrasound images to predict viability at the end of first trimester
Why early answers in pregnancy matter
For many women, the first weeks of pregnancy are filled with both hope and anxiety. When an early ultrasound cannot yet show clearly whether a pregnancy will continue or end in miscarriage, doctors call it a “pregnancy of unknown viability.” This period of waiting—often one to two weeks before a repeat scan—can be emotionally exhausting. The study summarized here explores whether subtle patterns hidden inside routine ultrasound images, combined with simple clinical information, can help predict the eventual outcome earlier and more accurately.
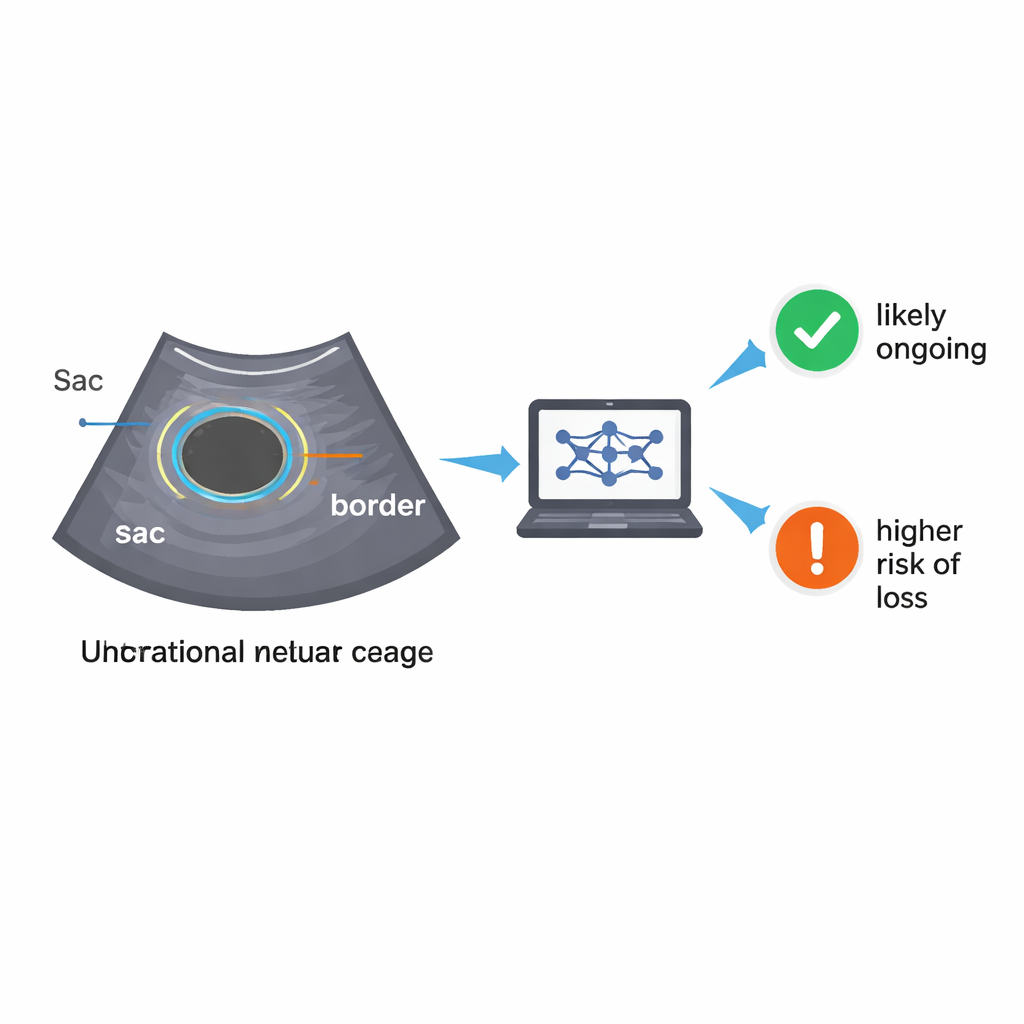
Looking beyond what the eye can see
Traditional ultrasound assessment relies on what clinicians can measure and see directly: the size and shape of the pregnancy sac, the presence of a yolk sac or tiny embryo, and whether a heartbeat is visible. Earlier research has used such features to build scoring systems, but their accuracy is limited and often depends on complete data. In this new work, researchers asked whether computers could pick up much finer details in the ultrasound images—details too subtle for the human eye—using an approach called radiomics. Radiomics turns images into thousands of numerical features that describe texture, brightness patterns, and small-scale structure, potentially capturing early signs of healthy or failing implantation.
Building an automated image pipeline
The team collected ultrasound scans from 500 women attending early pregnancy units in two London hospitals between 2021 and 2023. All had been told they had a pregnancy of unknown viability, and their final outcome—ongoing pregnancy or miscarriage by the end of the first trimester—was later recorded. To prepare the images for analysis, the researchers first taught a deep learning model to find two key regions on each scan: the gestational sac itself and a thin ring of surrounding uterine tissue. Using a neural network architecture designed for medical imaging, the system learned to trace these regions with high accuracy, closely matching expert manual outlines. This automated “segmentation” step is crucial, because it allows future scans to be processed without requiring additional time from specialist clinicians.
Turning patterns into predictions
Once the regions were identified, radiomics software extracted more than four thousand quantitative features from the ultrasound images. At the same time, the team gathered straightforward clinical information already recorded in routine care—such as the woman’s age, how many weeks pregnant she was by her last menstrual period, and how much bleeding and pain she had reported. Because not all of these variables are equally useful, the researchers tested a wide range of feature-selection methods and machine-learning algorithms to find the best combination. Their final model, called the Pregnancy of Unknown Viability Prediction Score (PUVPS), relied on a technique known as XGBoost and carefully chosen radiomic and clinical features. In testing, the model distinguished ongoing pregnancies from miscarriages with strong performance, including in data from an external hospital not used to train the system.
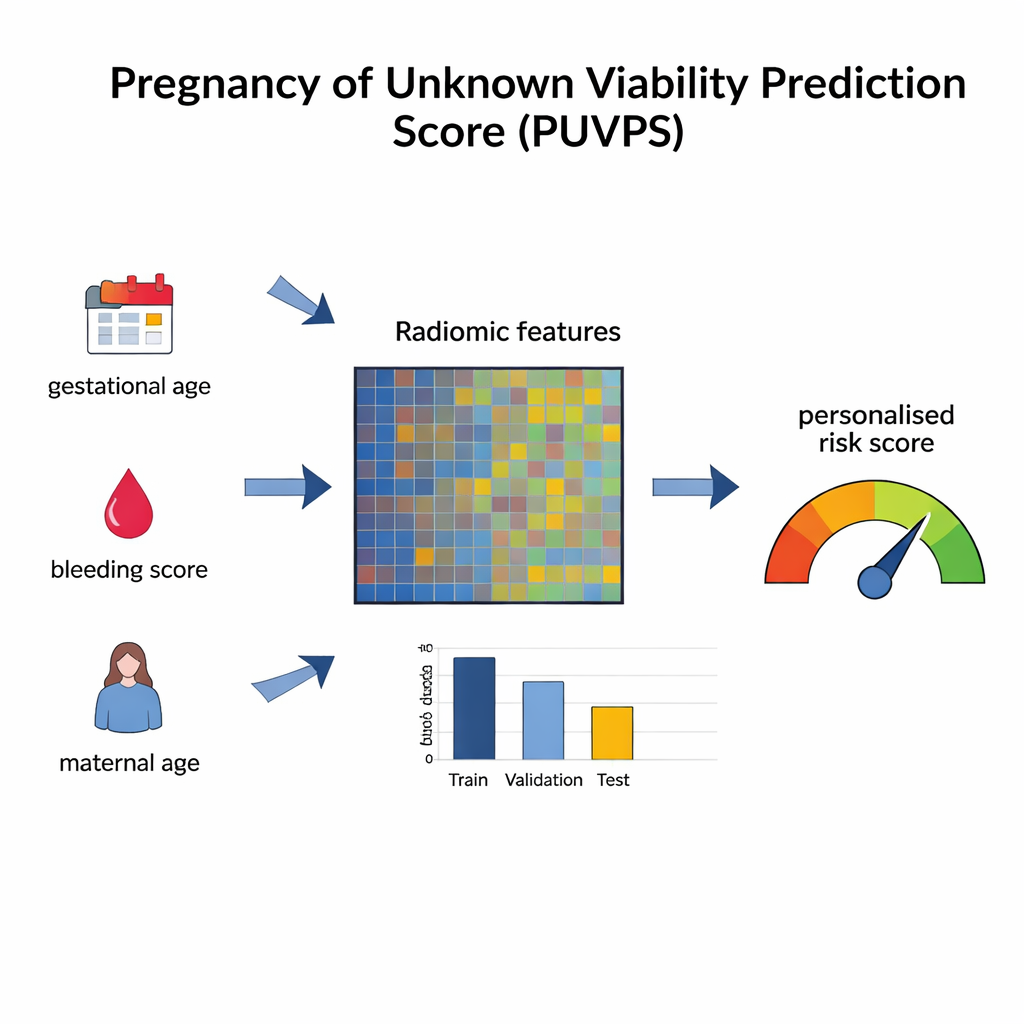
What the model is really using
Some of the most influential predictors turned out to be familiar clinical factors: how far along the pregnancy should be based on the last menstrual period, the severity of vaginal bleeding, and the mother’s age. But several radiomic texture measures from the sac and surrounding tissue also ranked highly. These capture how uniform or patchy the pixel intensities are and how bright regions are distributed, which may relate to how well the early placenta and supporting tissues are forming. Interestingly, the radiomic features also seemed to change with gestational age, hinting that they may be tracking real biological changes in early pregnancy development rather than random noise.
What this could mean for patients
The study has limitations, most notably the modest sample size, which can make any machine-learning model overly optimistic until it is tested in much larger and more diverse groups. Still, the results suggest that it may be possible to provide women facing a pregnancy of unknown viability with a personalized risk estimate based solely on the ultrasound they are already having, without extra blood tests or procedures. In the future, if validated in large multi-centre trials, a tool like PUVPS could sit quietly in the background of the ultrasound clinic, analyzing images in real time and offering a probability of ongoing pregnancy. Rather than replacing standard follow-up scans, it could help women and clinicians prepare emotionally and practically during a very uncertain waiting period.
Citation: Murugesu, S., Linton-Reid, K., Barcroft, J. et al. Radiomics analysis of early pregnancy ultrasound images to predict viability at the end of first trimester. Sci Rep 16, 5504 (2026). https://doi.org/10.1038/s41598-026-35158-5
Keywords: early pregnancy, miscarriage risk, ultrasound, radiomics, machine learning in medicine