Clear Sky Science · en
DMEK grafts prepared from corneas stored in TISSUE-C and CARRY-C (deswelling medium) show similar viable endothelial cell density
Why this matters for eyesight
For thousands of people each year, a corneal transplant is the only way to restore clear vision. Surgeons and eye banks work hard to prepare the donor tissue in ways that keep as many living cells as possible. This study asks a practical but crucial question: does a common step used to thin and “firm up” donor corneas before surgery actually harm the delicate cells that keep the cornea transparent, or is the apparent damage just an illusion created by how we measure those cells?
How surgeons fix a cloudy window of the eye
The cornea is the transparent front window of the eye. Its inner surface is lined with a single layer of pump cells that keep it clear by controlling water content. When these cells fail, the cornea swells and becomes cloudy, blurring vision. Modern surgery often replaces only this thin inner layer using a technique called DMEK, which transplants just the clear membrane and its living pump cells from a donor cornea. Because every extra living cell helps the transplant last longer, eye banks routinely count these cells to decide whether a cornea is suitable for use.
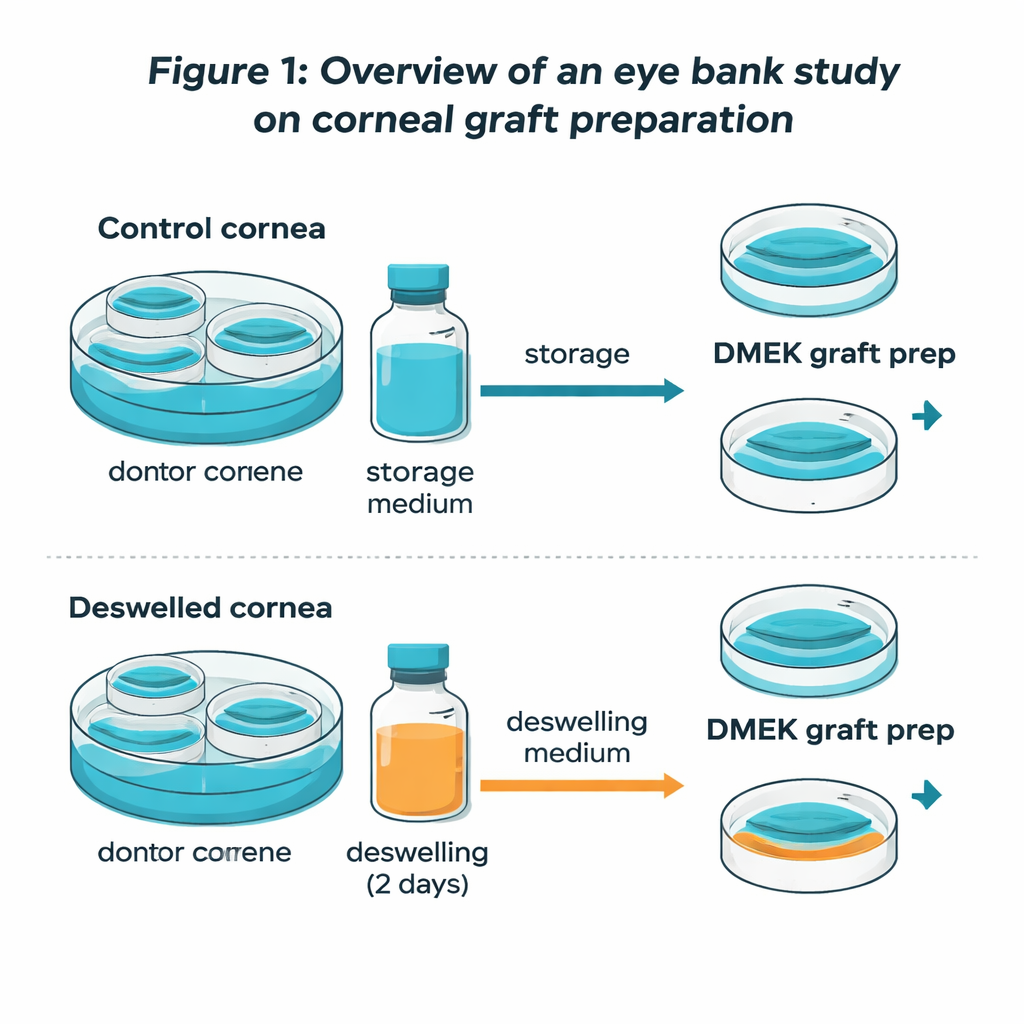
Why corneas are thinned before surgery
In many European eye banks, donor corneas are kept for days in a warm storage liquid so they can be tested before surgery. During this time they swell like a sponge in water, which creates folds on the inner surface and can make the surgical peeling step more difficult. To solve this, eye banks often move the cornea for a couple of days into a special “deswelling” liquid that contains a sugar-like compound called dextran. This draws out water and restores a more normal thickness. Older reports, however, suggested that such dextran-rich liquids might poison the pump cells, because cell counts looked lower afterward. Yet clinical studies in patients did not show worse long-term results, leaving a puzzle: was dextran really killing cells, or were the counts misleading?
A head‑to‑head test of paired donor corneas
To tackle this, the researchers used eight pairs of human donor corneas that were not suitable for transplantation but still valuable for research. Both corneas in each pair started in the same standard storage liquid and had nearly identical initial cell counts. Two weeks later, one cornea of each pair stayed in the original medium, while its partner spent two days in the dextran deswelling liquid before DMEK-type preparation. The team then used advanced fluorescent dyes and imaging to map where living cells were located across the central area and to calculate not just how tightly they were packed, but how many viable cells were present in total.

What the usual numbers were hiding
At first glance, the routine measurements appeared to confirm the old worries: after deswelling, the standard cell counts were about a quarter lower than in the corneas that stayed swollen. But when the scientists overlaid living-cell stains on the whole inner surface, a different picture emerged. Swollen corneas had many deep folds with bare, dead zones that did not show up in the routine counts, which only sample areas where cells can be clearly seen. Deswelled corneas, by contrast, had far fewer folds and a smoother surface. Neighboring cells had migrated to cover previously empty patches, spreading themselves more evenly. This made them slightly less crowded in any one spot, lowering the “cells per square millimeter” number, but the total pool of living cells across the transplant area—the measure that truly matters for graft survival—was essentially the same in both groups.
What this means for patients and eye banks
For patients waiting for sight-restoring surgery, these findings are reassuring. Short, two-day exposure to dextran-based deswelling liquid did not actually reduce the number of living corneal pump cells; it merely redistributed them over a larger, smoother area. The lower cell counts reported by standard methods turned out to be a measurement artifact, not genuine toxicity. By thinning the cornea and allowing cells to slide into previously folded, non-functioning regions, deswelling may even help prepare the tissue for a more even, healthy surface after transplantation. The study supports the continued use of dextran-containing deswelling media for DMEK grafts—and likely for full-thickness corneal grafts as well—provided exposure is short and carefully controlled.
Citation: Ninotta, S., Sagnial, T., Goin, P. et al. DMEK grafts prepared from corneas stored in TISSUE-C and CARRY-C (deswelling medium) show similar viable endothelial cell density. Sci Rep 16, 4803 (2026). https://doi.org/10.1038/s41598-026-35103-6
Keywords: corneal transplant, DMEK, eye bank, dextran deswelling, endothelial cell viability