Clear Sky Science · en
Brain-infiltrating CD8 T cells retain functional activity to protect against acute Zika virus infection
Why this research matters to you
Zika virus is best known for damaging the developing brains of fetuses, but it can also harm the brains of adults. Our bodies fight viruses using many tools, including killer immune cells called CD8 T cells. Until now, scientists did not know whether these cells help or hurt the brain during Zika infection. This study uses a mouse model that is highly vulnerable to Zika to show that brain‑invading CD8 T cells actually protect the brain, and that disrupting their activity can make disease much worse. Understanding this balance could guide safer vaccines and treatments for Zika and related mosquito‑borne viruses.
A closer look at Zika and the brain
Zika virus spreads mainly through mosquito bites but can also be passed through sex, blood transfusion, and from mother to fetus. Earlier outbreaks revealed that Zika can cross protective barriers in the body, including the blood–brain barrier, and infect brain cells. This can lead to inflammation, nerve damage, and conditions such as Guillain–Barré syndrome. In this study, researchers used mice lacking a key antiviral signaling pathway (type I interferon). These mice are especially sensitive to Zika and develop clear signs of brain infection, making them useful for probing how the immune system responds inside the central nervous system. 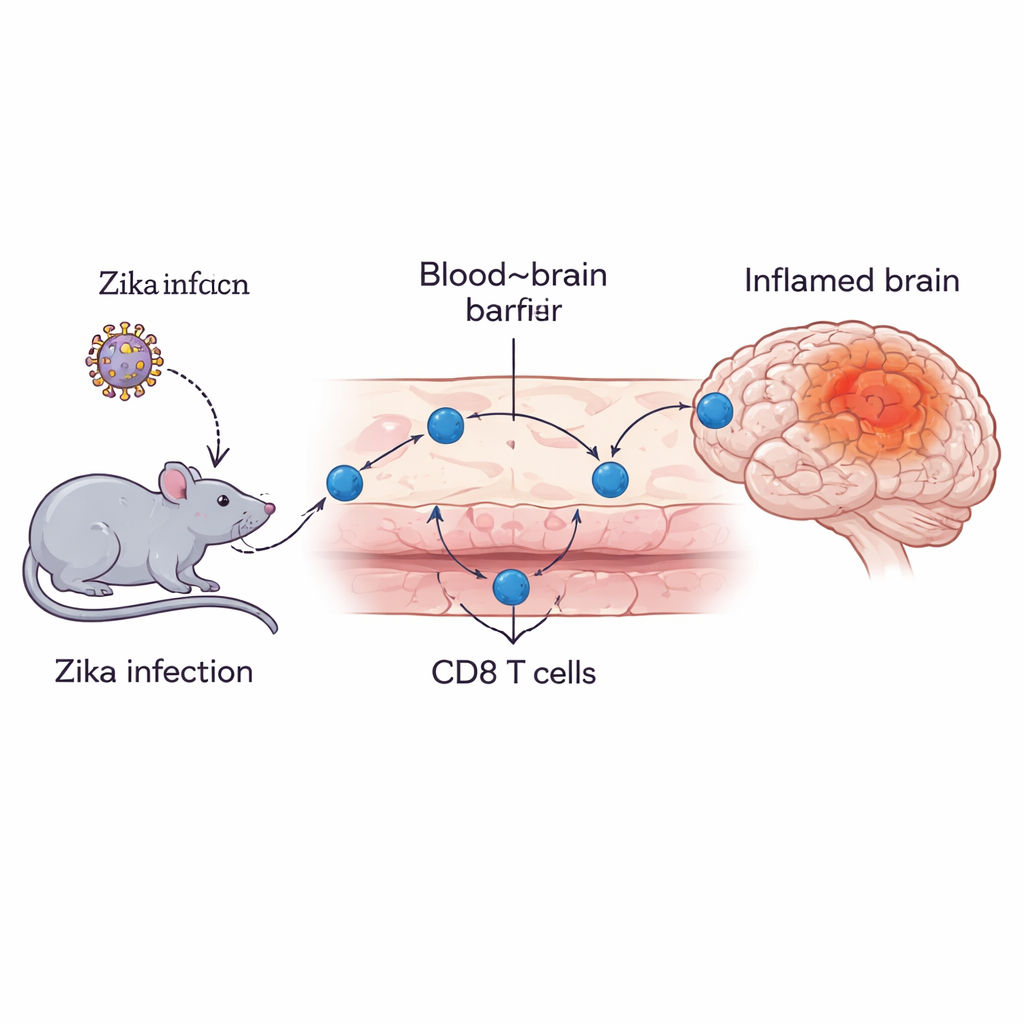
When the brain sounds the alarm
After infecting the mice with a clinical Zika strain, the team tracked weight loss, virus levels, and changes in brain tissue. Within a few days, viral genetic material appeared in the brain, and the animals began to lose weight and show signs of illness. The brain switched on many genes linked to inflammation and injury, including molecules associated with blood–brain barrier disruption and nerve damage. At the same time, genes tied to antiviral defense became more active, showing that the brain was mounting a strong response. Young mice carried more virus and got sick faster than adults, suggesting that age influences how vulnerable the brain is to Zika.
Killer T cells move into the brain
The scientists then asked which immune cells were entering the brain during infection. They found large numbers of CD8 T cells, a type of white blood cell that can recognize and kill virus‑infected cells. These CD8 cells in the brain mostly showed an "effector" profile, meaning they were primed for action rather than in a resting state. Markers on their surface indicated they had previously seen Zika and were not just bystanders. In the spleen, a major immune organ, Zika‑experienced CD8 T cells produced high levels of powerful antiviral molecules and were poised to move into tissues. Together, these findings suggested that the brain‑infiltrating CD8 cells were highly active fighters rather than exhausted or worn‑out cells.
Proving that CD8 T cells are protective
To test if these T cells were friends or foes, the team performed two key experiments. First, they transferred CD8 T cells from Zika‑infected donor mice into other infected mice. Animals that received these Zika‑experienced cells lost less weight and survived longer than those that received control cells, showing that the primed CD8 cells could actively limit disease. Second, the researchers used a drug, fingolimod, to trap T cells in lymph nodes and reduce their entry into the brain. When CD8 T cell infiltration was blocked, virus levels in the brain shot up and markers of inflammation and injury increased, indicating that fewer CD8 cells meant more damage. 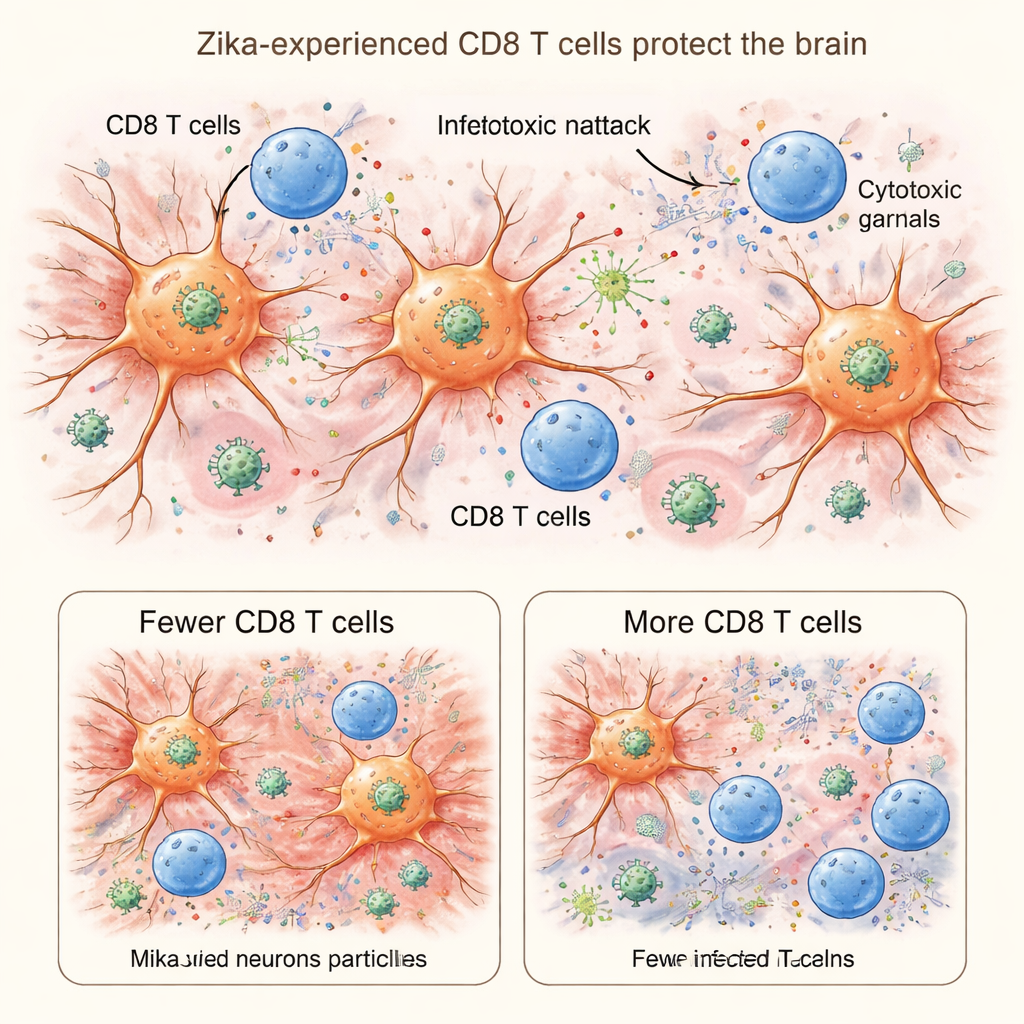
When blocking a brake makes things worse
Many therapies for cancer work by blocking PD‑1, a "brake" molecule on T cells that can signal them to slow down. In chronic infections and tumors, PD‑1 is often a sign that T cells are exhausted and need to be re‑energized. Here, however, most Zika‑experienced CD8 T cells in the brain expressed PD‑1 yet still functioned strongly. When the researchers treated infected mice with an antibody that blocks PD‑1, the animals actually fared worse: they lost more weight and died more often. This suggests that, during acute Zika infection in this model, PD‑1 marks active, helpful T cells and may help fine‑tune their response rather than shut it down completely.
What this means for future treatments
For non‑experts, the key message is that not all immune responses in the brain are harmful. In this vulnerable mouse model, CD8 T cells that invade the brain during acute Zika infection help clear the virus and limit inflammation, improving survival. Preventing these cells from reaching the brain, or interfering with their regulation through PD‑1, makes the disease worse. These findings caution against one‑size‑fits‑all immune therapies, such as blanket PD‑1 blockade, in viral brain infections. They also highlight CD8 T cells as promising targets for vaccines and treatments designed to protect the brain from Zika and possibly other related viruses.
Citation: Kim, J., Lee, W., Kim, D.Y. et al. Brain-infiltrating CD8 T cells retain functional activity to protect against acute Zika virus infection. Sci Rep 16, 4738 (2026). https://doi.org/10.1038/s41598-026-35079-3
Keywords: Zika virus, CD8 T cells, brain infection, neuroinflammation, antiviral immunity