Clear Sky Science · en
Shen-Shuai-II-Recipe inhibits aerobic glycolysis through SIRT1 in 5/6 ablation/infarction renal failure model
Why this kidney study matters
Chronic kidney disease affects millions of people worldwide and often leads to scarring of the kidneys, called fibrosis, that cannot be reversed. Current drugs slow the damage but rarely stop it. This study explores how a traditional Chinese herbal formula, Shen-Shuai-II-Recipe (SSR), might protect the kidneys by gently resetting how kidney cells use energy, offering clues to new ways of treating long‑term kidney damage.
Energy-hungry kidney cells under stress
Our kidneys are packed with tiny tubules that constantly filter blood and adjust salts and water. These tubular cells normally burn fat efficiently to get the energy they need. In chronic kidney disease, repeated injury pushes them into a different mode: they start breaking down sugar very quickly, a process called aerobic glycolysis. This emergency fuel strategy helps short-term survival but produces excess lactic acid and is closely linked to scarring of kidney tissue. The authors note that this metabolic switch appears in many forms of kidney injury and is now seen as a key driver of progressive fibrosis.
A traditional formula put to the test
To probe how SSR works, the researchers used a well-established rat model of severe kidney damage called the 5/6 ablation/infarction model, in which most kidney tissue is surgically removed or blocked. After the injury, rats were given SSR, the blood‑pressure drug losartan (a standard treatment), or no active treatment for eight weeks. Kidney function was tracked using common blood and urine tests, and kidney tissue was examined under the microscope and with protein measurements. Rats receiving SSR or losartan had lower levels of waste products in the blood and less protein in the urine than untreated rats, indicating better kidney function. Tissue staining showed less collagen buildup and fewer signs of fibrosis in the treated groups, with SSR clearly easing structural damage.
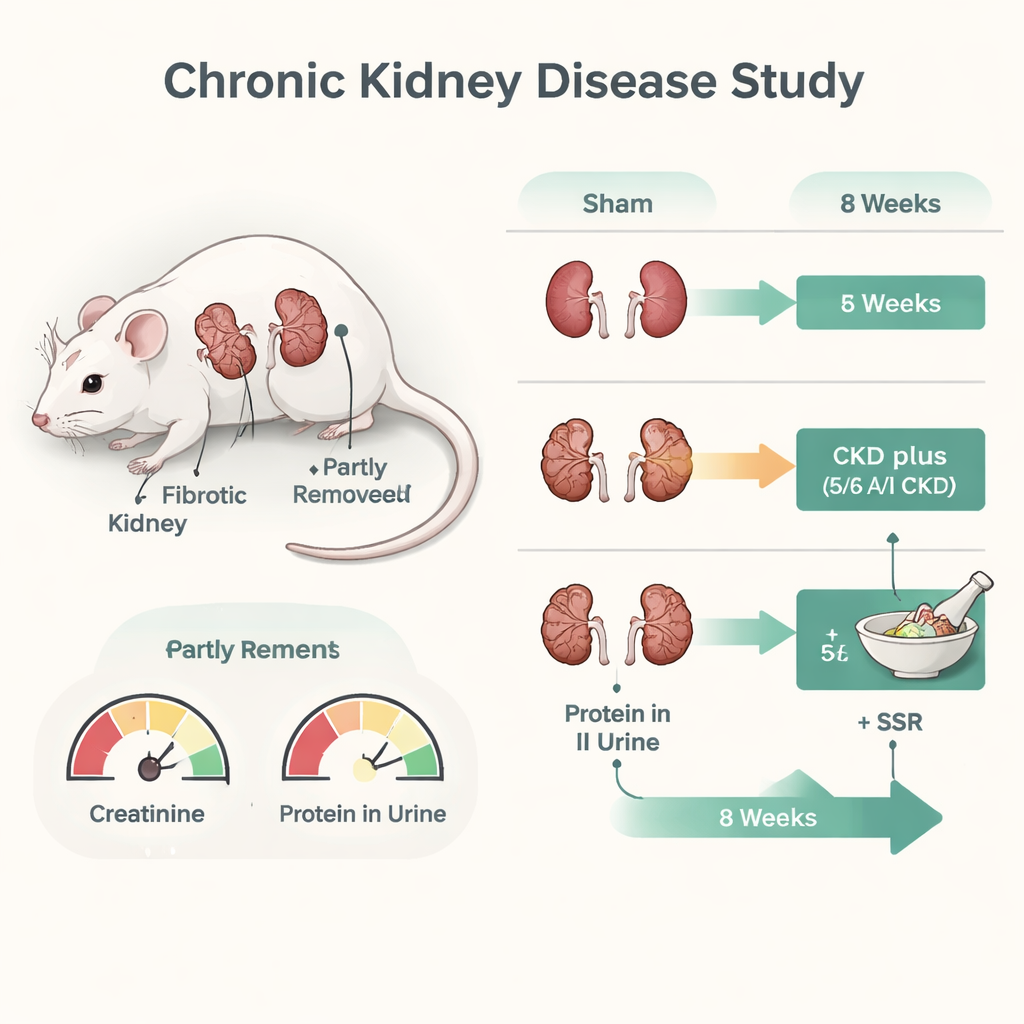
Dialing back sugar burning in damaged kidneys
The team then focused on energy metabolism inside kidney cells. In the damaged kidneys, levels of key glycolysis enzymes, such as HK2 and PFKFB3, were elevated, and lactic acid levels were higher while pyruvic acid was lower—hallmarks of overactive sugar burning. SSR treatment reversed these changes: glycolysis‑related enzymes dropped, lactic acid levels fell, and the balance of metabolites shifted toward a healthier state. Similar effects were seen in cultured rat kidney tubular cells exposed to low oxygen in the lab, which mimics the chronically oxygen‑poor environment of diseased kidneys. Under hypoxia, these cells became more fibrotic and glycolytic, but serum from SSR‑treated animals reduced fibrotic proteins, lowered glycolysis activity, and preserved glucose in the culture medium.
A molecular switch: SIRT1 and HIF‑1α
The researchers homed in on two molecular regulators that link oxygen levels to metabolism: SIRT1, an enzyme that senses the cell’s energy state, and HIF‑1α, a transcription factor that switches on glycolysis genes under low oxygen. In diseased rat kidneys and hypoxic kidney cells, SIRT1 levels fell while HIF‑1α rose. SSR treatment boosted SIRT1 and suppressed HIF‑1α, in parallel with reduced glycolysis and fibrosis. To test whether SIRT1 was essential for SSR’s benefits, the team used small interfering RNA to knock down SIRT1 in kidney cells. When SIRT1 was silenced, SSR could no longer decrease HIF‑1α, glycolysis enzymes, lactic acid buildup, or fibrotic markers. This indicates that SIRT1 is a central switch through which SSR exerts its protective effects.
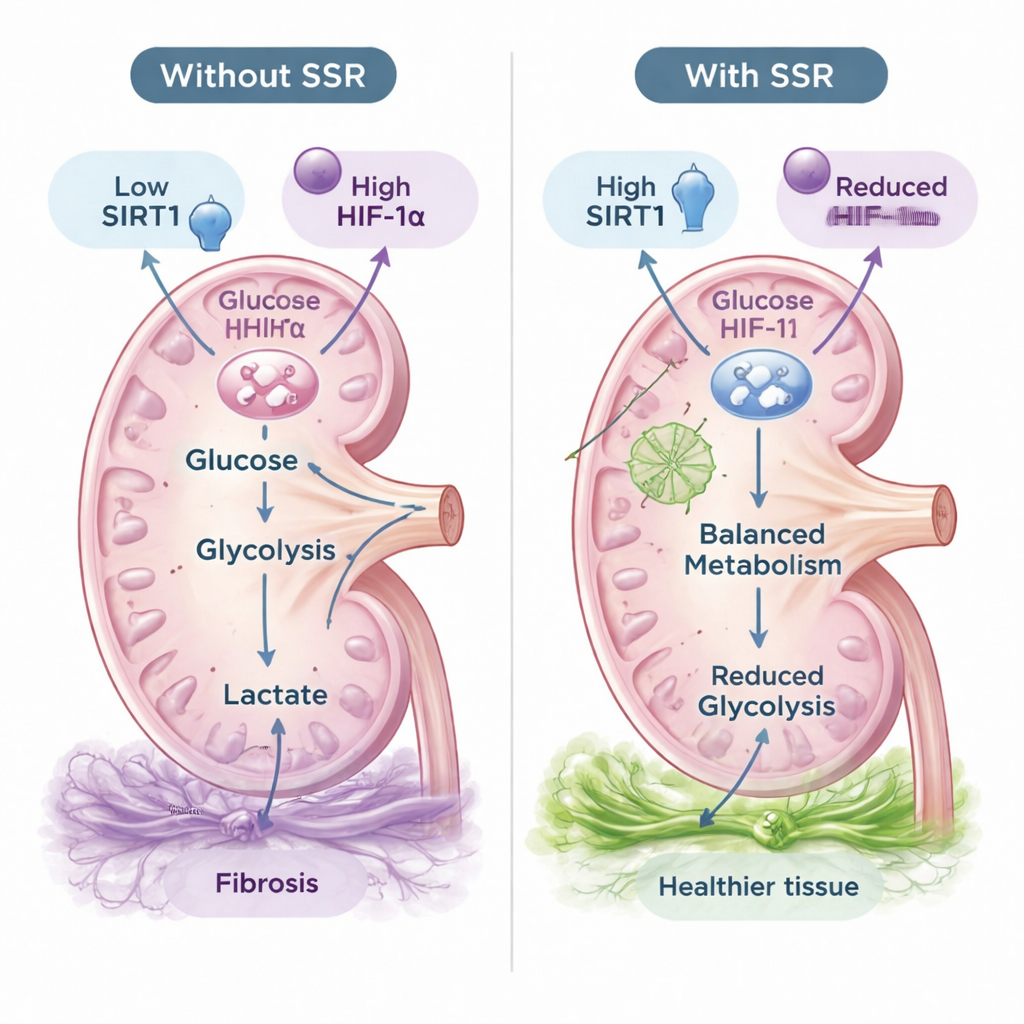
What this could mean for future treatments
The authors propose that SSR acts as a multi‑component “metabolic reprogrammer” for the kidney: by enhancing SIRT1 and keeping HIF‑1α in check, it prevents tubular cells from being locked into a damaging high‑glycolysis state and slows the buildup of scar tissue. Several known ingredients of SSR have already been linked individually to SIRT1 activation and to better control of sugar use in other organs. Together, they may work synergistically in the kidney. While this work was done in rats and cell cultures and does not yet prove clinical benefit, it highlights energy metabolism—and specifically the SIRT1/HIF‑1α axis—as a promising target. In plain terms, helping kidney cells burn fuel more wisely may be one of the keys to slowing, or someday halting, chronic kidney scarring.
Citation: Lan, T., Zhang, X., Lyu, X. et al. Shen-Shuai-II-Recipe inhibits aerobic glycolysis through SIRT1 in 5/6 ablation/infarction renal failure model. Sci Rep 16, 5022 (2026). https://doi.org/10.1038/s41598-026-35061-z
Keywords: chronic kidney disease, renal fibrosis, energy metabolism, aerobic glycolysis, traditional Chinese medicine