Clear Sky Science · en
Risk factors for electrographic seizures in infants after cardiac surgery and their association with outcomes: a retrospective cohort study
Why brain health after infant heart surgery matters
Each year, many babies born with heart defects need complex surgery in their first months of life. Thanks to advances in heart care, more of these children survive than ever before—but their brains may still be at risk. This study looks at “silent” seizures that do not cause visible shaking but show up on brain monitors, and asks two key questions: which babies are most likely to have them after heart surgery, and what do these hidden seizures mean for their short‑term health and brain injury risk?
Hidden brain storms after heart repair
Seizures in newborns and young infants are often invisible to parents and even to doctors at the bedside, especially when children are deeply sedated and on breathing machines. The research team followed 373 infants under one year of age who underwent surgery to correct or ease congenital heart defects. All received continuous brain monitoring after the operation using two tools: a full electroencephalogram (EEG), which records the brain’s electrical activity in detail, and a simpler bedside tracing called amplitude‑integrated EEG (aEEG). In this group, about 6 in 100 children developed electrographic seizures after surgery, and roughly half of those had very prolonged episodes, known as status epilepticus.
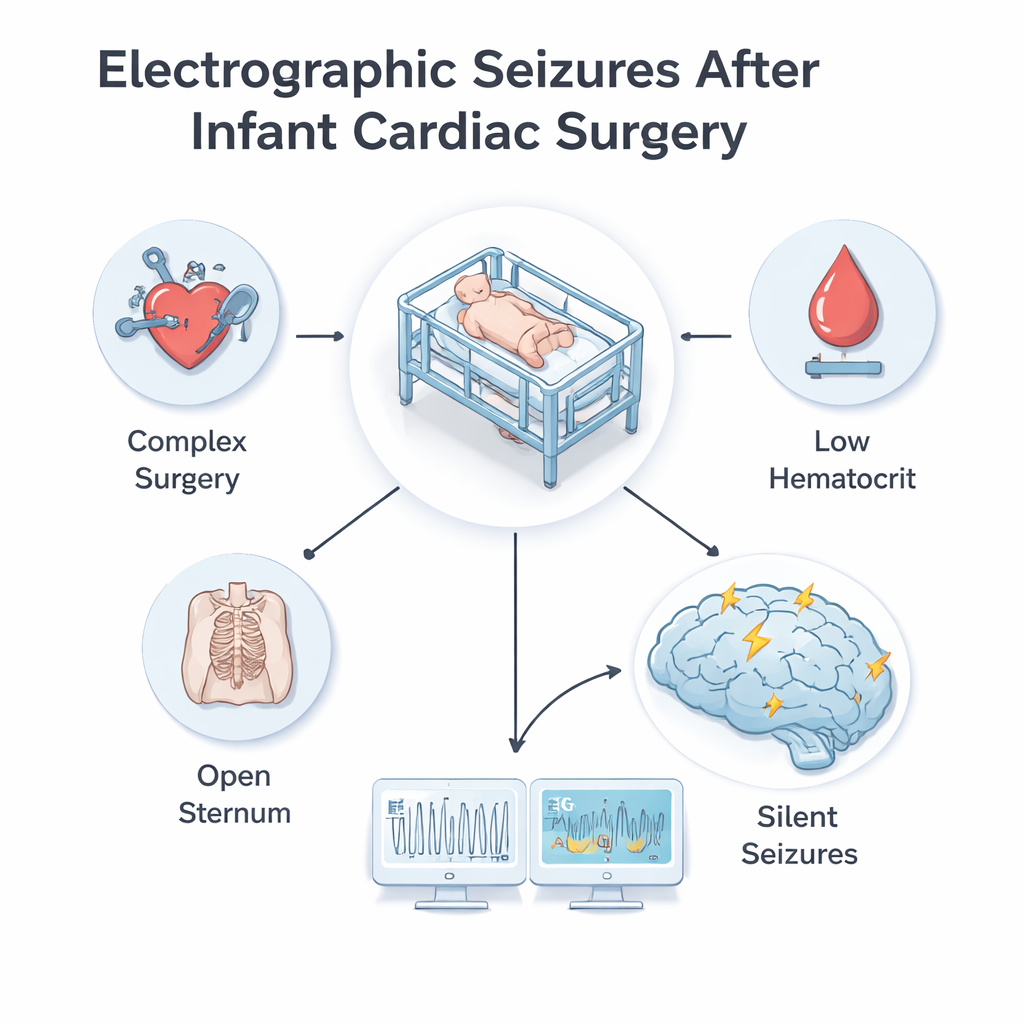
Pinpointing which babies are at highest risk
The authors examined dozens of factors collected before, during, and right after surgery to see which ones were linked to these silent seizures. Through statistical modeling, three stood out as independent risk markers. First was the overall complexity of the heart operation, measured by a standard score (RACHS‑2) that rises with more demanding procedures. Second was whether the child’s breastbone (sternum) was left open at the end of surgery—a common practice when the heart is swollen or weak and needs more room. Third was the level of red blood cells (hematocrit) in the blood on arrival in intensive care; lower levels mean the blood carries less oxygen. Together, these three measures formed a prediction model that could reliably separate higher‑risk from lower‑risk babies.
What silent seizures say about the brain
Next, the team asked how these electrographic seizures related to early complications. At first glance, babies with seizures seemed worse off in many ways: they had more major problems such as the need for a tracheostomy, repeat surgery, or support from an artificial heart‑lung machine, and they were more likely to die in the hospital. However, once the analysis adjusted for how complex the surgery was, how long the heart‑lung machine ran, and whether the sternum was left open, seizures on their own no longer predicted these broader complications. In contrast, the link with the brain itself remained strong. Infants with postoperative electrographic seizures had about eight times the odds of having a clear brain injury—such as stroke or coma—compared with those without seizures.
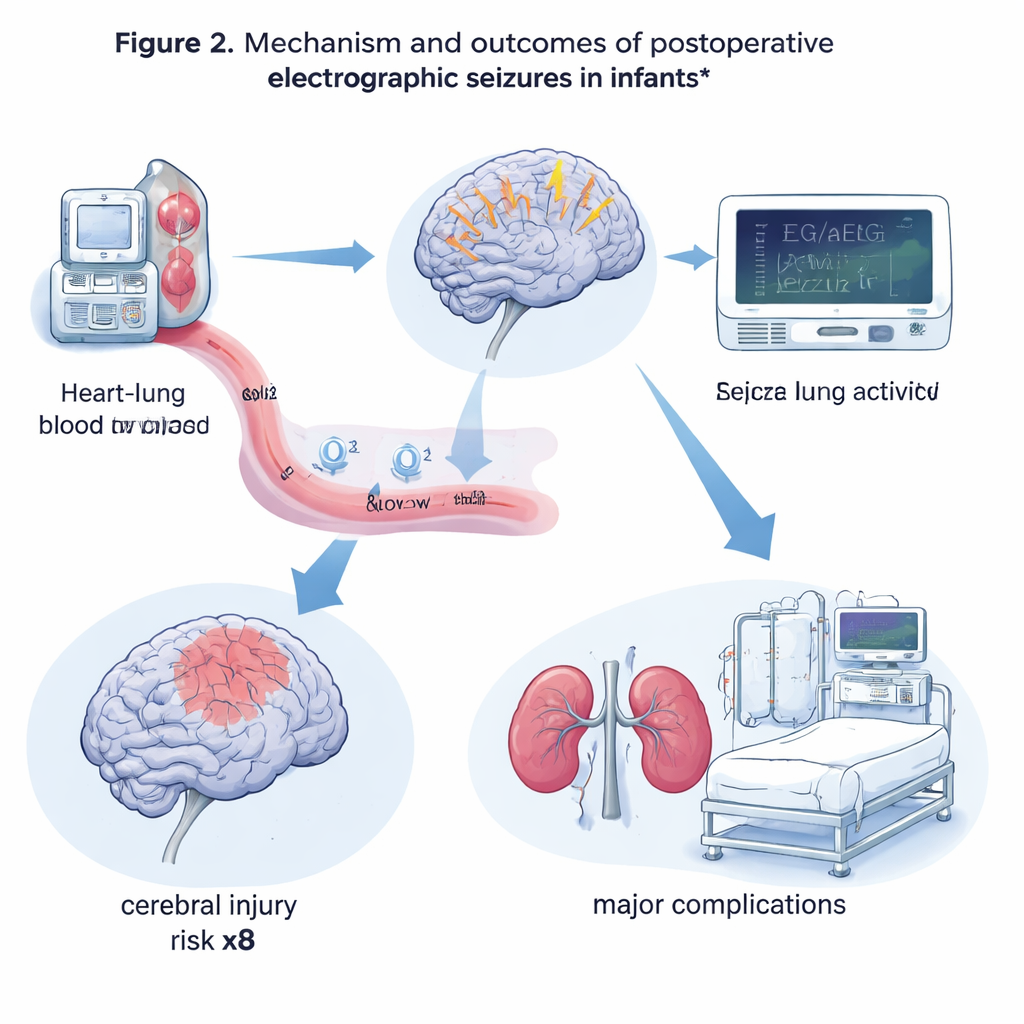
Using brain monitors wisely
Continuous EEG for every infant heart patient is expensive and technically demanding, and many hospitals cannot monitor all children all the time. This study suggests a more targeted approach: focus scarce EEG resources on babies whose surgery is very complex, whose chest must be left open, or whose blood oxygen‑carrying capacity is low right after surgery. In these situations, the brain is more likely to be under strain from reduced oxygen delivery, and seizures may be an early electrical warning sign of injury before any outward symptoms appear.
What this means for families and care teams
For families of infants needing heart surgery, the findings carry a mixed but practical message. On one hand, silent seizures after surgery are not simply a random event: they tend to appear in babies whose hearts and circulation are already under heavy stress. On the other hand, when they do occur, they are a powerful clue that the brain may have been hurt, even if the child looks calm and still. By identifying high‑risk children and watching their brain activity closely, doctors may be able to detect injury earlier, tailor treatments, and, in the future, test ways to better protect the developing brain during these lifesaving operations.
Citation: Ranucci, M., Mastrangelo, M., Sperandeo, F. et al. Risk factors for electrographic seizures in infants after cardiac surgery and their association with outcomes: a retrospective cohort study. Sci Rep 16, 4912 (2026). https://doi.org/10.1038/s41598-026-35059-7
Keywords: infant cardiac surgery, electroencephalography, silent seizures, brain injury, congenital heart disease