Clear Sky Science · en
Evaluating the impact of communicating high polygenic risk for coronary artery disease on the health behaviour of young overweight adults: a pragmatic randomised controlled trial
Why your genes and your heart are big news
Many people now send a tube of spit to a lab and get back long lists of genetic risks. One hope is that such reports will scare us—just enough—into eating better, moving more, and seeing the doctor in time. This study asked a simple but important question: if you tell young, slightly overweight adults that their genes put them at high risk for future heart disease, will they actually change their habits and improve their health?
A closer look at genetic heart risk
Coronary artery disease, a major cause of heart attacks, runs strongly in families. Scientists can now combine information from many small DNA changes into a single "polygenic risk score" that estimates a person’s inherited tendency to develop clogged heart arteries. The promise is that this score might identify younger adults who look healthy today but are quietly on a risky path. If these people knew their genetic risk early enough, they might be more motivated to lose weight, exercise, and control their blood pressure and cholesterol.
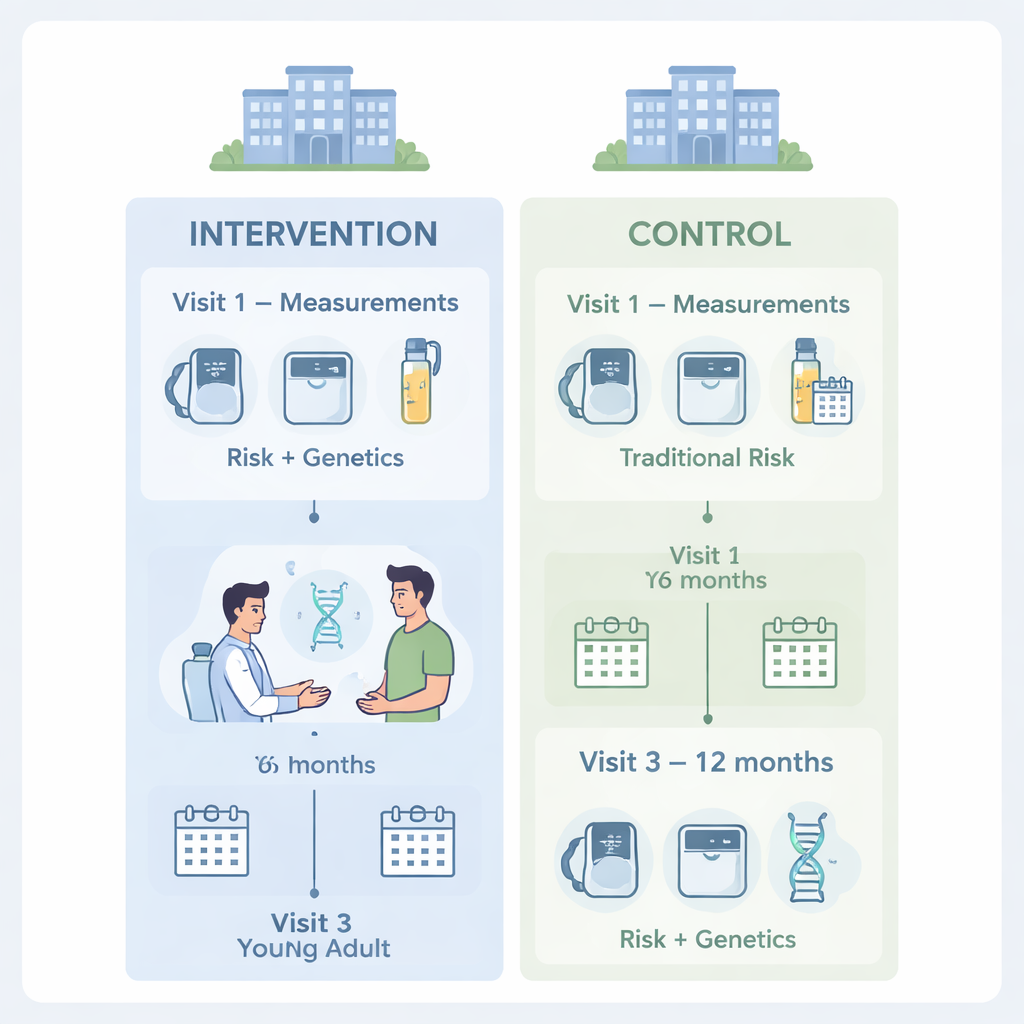
Putting genetic risk to the test in everyday clinics
To find out whether genetic risk information changes behavior, researchers in Estonia carried out a large, real-world trial in primary care. They recruited more than 1,000 adults aged 25 to 44 who were slightly overweight but did not yet have heart disease or diabetes. All had gene data from the Estonian Biobank. Everyone in the main comparison groups had a high genetic risk score for coronary artery disease, placing them in the top fifth of the population for inherited risk. Participants were randomly assigned either to an intervention group or a control group, and both groups saw their own family physicians for care over a year.
What information patients received
Both groups had their usual heart risk factors measured, including blood pressure, cholesterol, smoking, weight, and waist size. Doctors then estimated each person’s chance of developing heart disease within 10 years. For the intervention group, this calculation included genetic risk, and the results were shown as clear graphs: one compared their risk to that of their peers and illustrated how lifestyle changes could help; another displayed their genetic risk compared with the wider population. Doctors used these visuals to guide conversations and offer lifestyle advice and, when needed, preventive medicines such as cholesterol- or blood-pressure-lowering drugs. The control group received the same check-ups and counseling, but their genetic risk was not added to the calculations or shown to them until the end of the study.
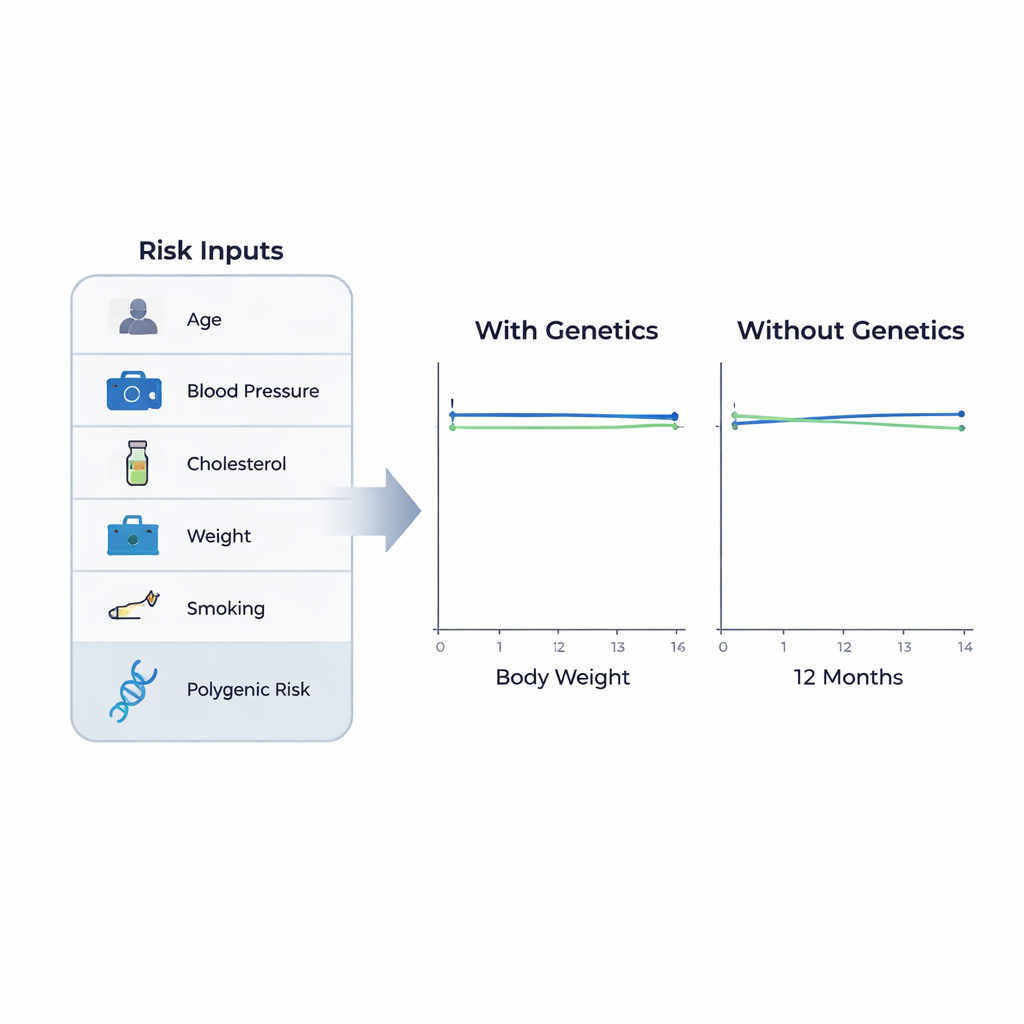
What changed—and what did not
After 12 months, the researchers compared the two groups. The main yardstick was body mass index, a common measure of weight relative to height. They also looked at blood pressure, cholesterol levels, blood sugar, waist size, smoking, drinking, diet, physical activity, and prescriptions or purchases of heart medicines. Across the board, there were no meaningful differences between those told about their high genetic risk and those who were not. Average weight, waist measurements, blood pressure, cholesterol, and estimated 10-year heart risk all stayed very similar in both groups. Self-reported habits—such as smoking, exercise, and fruit and vegetable intake—also showed no clear advantage for the group that received detailed genetic information.
Why the results matter for everyday health
The findings send a clear message: simply telling young adults that their genes put them at high risk for future heart disease does not, by itself, lead to noticeable improvements in weight or other key risk factors over a year. In this study, genetic risk behaved much like any other number on a risk chart—it was useful for doctors to know, but not powerful enough on its own to transform behavior. For genetic information to make a real difference, it likely needs to be combined with stronger, ongoing support, such as more frequent counseling, digital tools, and carefully targeted treatment. For now, the basics still matter most: staying active, eating well, not smoking, and working with a health professional to manage blood pressure and cholesterol, regardless of what your DNA says.
Citation: Põld, A., Toompere, K., Elken, A. et al. Evaluating the impact of communicating high polygenic risk for coronary artery disease on the health behaviour of young overweight adults: a pragmatic randomised controlled trial. Sci Rep 16, 4907 (2026). https://doi.org/10.1038/s41598-026-35027-1
Keywords: heart disease prevention, genetic risk scores, young adults health, primary care trials, lifestyle change