Clear Sky Science · en
A nationwide study of invasive Streptococcus agalactiae in the Faroe Islands from 2009 to 2024
Why this tiny island study matters
Group B Streptococcus is a common bacterium that many healthy people carry without knowing it, yet it can cause life‑threatening infections in newborns, pregnant women, older adults, and people with weak immune systems. This study followed all serious Group B Streptococcus infections in the Faroe Islands—a small, remote archipelago in the North Atlantic—over 15 years. By examining every case in an entire country, the researchers created a detailed picture of how this germ is changing, how well antibiotics still work, and how future vaccines might protect people, even in such a small and isolated community.
A remote laboratory in the North Atlantic
The Faroe Islands, with a population of only about 54,000, offer a rare chance to watch an infection across a whole nation where health care is centralized and well recorded. The researchers gathered data on all cases where Group B Streptococcus was found in normally sterile parts of the body, such as blood or spinal fluid, from 2009 to 2024. They identified 42 such invasive infections, mostly from blood samples. This might sound like a small number, but in a small population it reveals important shifts in how often the disease occurs and what kinds of bacterial strains are responsible.
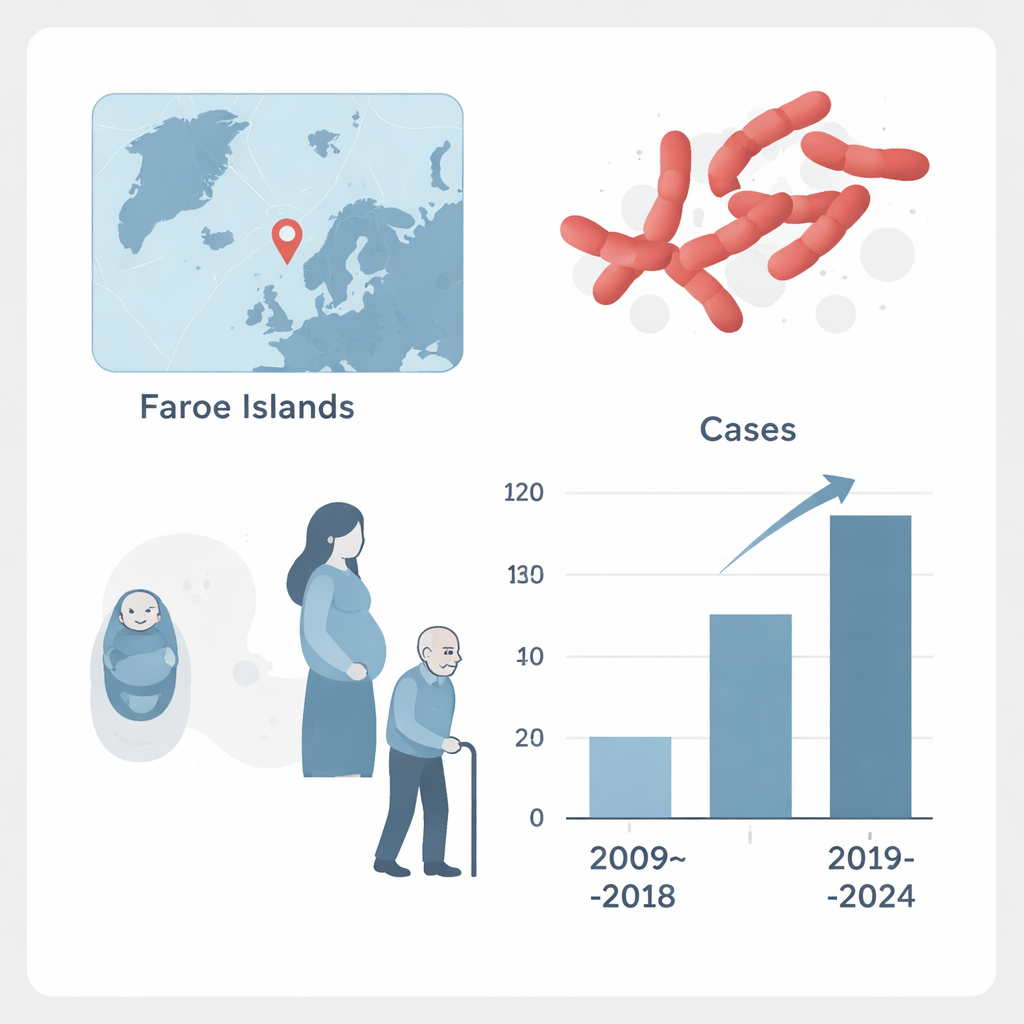
Infections on the rise, but still treatable
When the team adjusted for population size, they found that serious Group B Streptococcus infections became more common over time. On average, there were about 3.7 cases per 100,000 people each year from 2009 to 2018, rising to about 7.5 cases per 100,000 from 2019 to 2024—roughly a doubling of incidence. Unlike some other bacteria, this rise did not seem to dip during the COVID‑19 pandemic, suggesting that this germ is less affected by short‑term changes in social contact. The encouraging news is that every isolate tested remained fully sensitive to penicillin, the standard drug used to treat these infections, although a few showed resistance to backup antibiotics such as erythromycin and clindamycin.
Which bacterial “families” are circulating
To understand how similar or different the bacteria were, the scientists examined their outer sugar coats (called serotypes) and deeper genetic fingerprints. Among the 18 isolates available for detailed testing, the most common serotypes were II and V, followed by Ib and Ia, with a scattering of others and no sign of certain types that are strongly linked to severe disease in newborns. Using whole‑genome sequencing for the most recent 15 samples, they grouped the bacteria into genetic families known as clonal complexes. One family, called CC12, dominated the picture, with smaller contributions from several others. Notably, the so‑called hypervirulent CC17 lineage, often associated with neonatal meningitis, was not found, hinting that most cases in the Faroes likely occurred in adults rather than in babies.
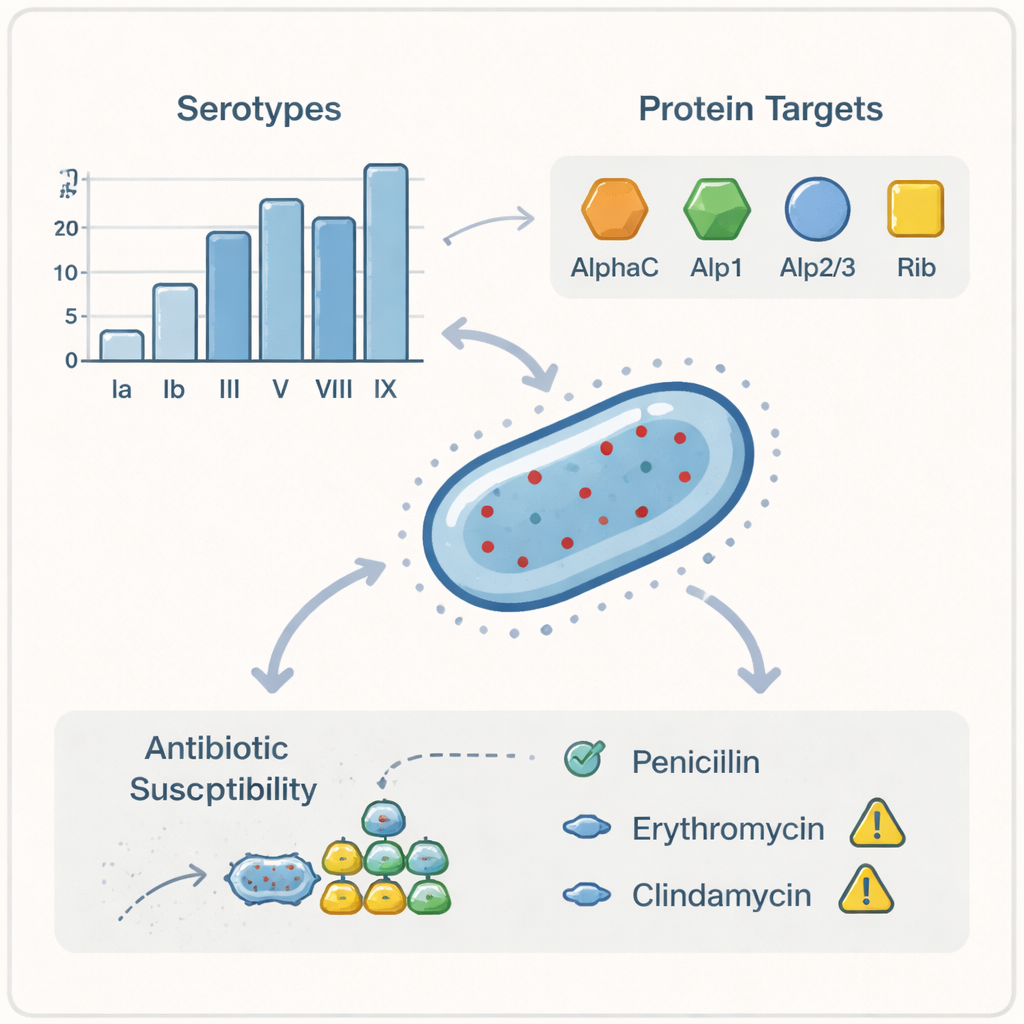
Clues for future vaccines
Because global health agencies are working toward vaccines against Group B Streptococcus, the team paid special attention to features that potential vaccines target. They showed that most of the invasive strains in the Faroe Islands belong to the same major serotypes that a leading sugar‑based vaccine candidate (known as GBS6) is designed to cover, although a few rare types fell outside its scope. They also looked for a set of surface proteins, called Alp family proteins, that form the basis of a different, protein‑based vaccine candidate. All of the sequenced strains carried at least one of these Alp proteins, suggesting that this second type of vaccine could also perform well in this setting. Other genetic markers tied to how the bacteria attach to human tissues and evade the immune system were found in nearly all strains, underlining that these are genuine disease‑causing variants.
What this means for patients and policy
By combining national surveillance with modern genetic tools, this study gives the Faroe Islands their first clear baseline for serious Group B Streptococcus disease. The rising infection rate signals that health services should stay alert, but the continued effectiveness of penicillin is reassuring. The mix of bacterial types suggests that current vaccine candidates would likely protect many people in this population, especially adults, if such vaccines are introduced. For a small, isolated country—and for similar regions elsewhere—ongoing genetic monitoring of these bacteria will be vital to track changes over time, spot any worrisome drug resistance, and guide decisions about if and when to roll out new vaccines.
Citation: Joensen, Ó., Krogfelt, K.A., Gaini, S. et al. A nationwide study of invasive Streptococcus agalactiae in the Faroe Islands from 2009 to 2024. Sci Rep 16, 5090 (2026). https://doi.org/10.1038/s41598-026-35025-3
Keywords: group B streptococcus, Faroe Islands, invasive infection, bacterial genomics, vaccine development