Clear Sky Science · en
Enhancing patient admission efficiency through a hybrid cloud framework for medical record sharing
Why faster hospital admissions matter
Anyone who has waited anxiously in an emergency room knows that every minute feels long. Yet doctors often start from scratch because a patient’s earlier tests, scans, or diagnoses are locked away in another hospital’s computer system. This paper explores a new way to connect hospitals through a shared but carefully controlled cloud setup, so staff can quickly find a patient’s history, cut down duplicate tests, and reduce the time people spend waiting for care.
The problem of scattered medical records
Modern hospitals store information electronically, but these systems usually stop at the hospital’s front door. When a patient shows up in an emergency department, staff may have no access to previous lab results, X-rays, or treatment notes from other facilities. Past efforts to fix this often relied on a single central database or cards and codes patients must carry. Those approaches can create security risks, single points of failure, and practical problems if a card is lost or damaged. The result is slower admissions, repeated procedures, and sometimes delays in urgent decisions.
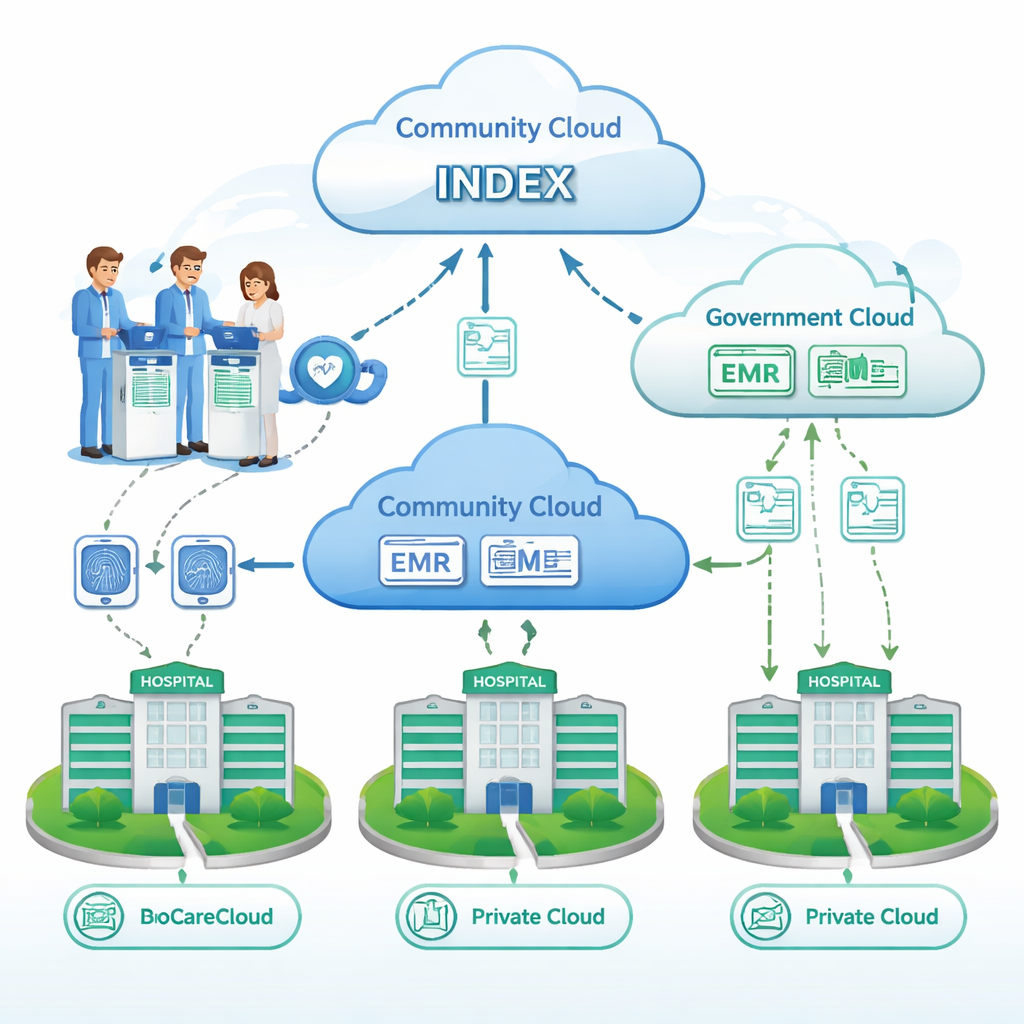
A layered cloud system built around the patient
The authors propose a framework called BioCareCloud that connects hospitals without forcing everyone’s data into one giant vault. Each hospital keeps its own records in a private cloud under its direct control. A shared community cloud never stores medical details; instead, it keeps a kind of index that answers one question: “Which hospitals have records for this patient?” A separate government cloud holds only basic demographic information, such as name and national ID, and helps automatically fill in registration details when a new record is created. Together, these three layers aim to give doctors the right information at the right time while limiting who sees what.
Fingerprints and smart bracelets instead of paper forms
To make admission smoother, the framework uses fingerprint readers at self-service kiosks instead of long registration forms or ID cards. The system does not keep raw fingerprint images; it converts each fingerprint into a scrambled digital code that cannot be turned back into a picture. That code is used to look for an existing record in the hospital and to ask the community cloud whether other hospitals have seen this patient before. At the same time, a disposable smart bracelet begins to track vital signs such as heart rate, temperature, and blood pressure. These measurements flow automatically into the hospital’s private cloud, so by the time the patient reaches the doctor, the latest vital signs are already on screen.
How the data moves during different patient journeys
The framework defines four typical situations. In the first, a person has never been seen anywhere before: the fingerprint is checked, the government cloud supplies basic details, and a brand-new record is created locally while the community cloud logs that this hospital now has information on the patient. In the second, the patient has only ever visited this hospital; the system confirms there are no outside records and simply updates the existing file. In the third and fourth situations, the community cloud reports that other hospitals also have records. The local hospital then securely requests those outside files and merges them with its own notes and the live bracelet data, giving the physician a more complete picture before examining the patient.
Testing the idea with real hospital data
Because installing such a system in working emergency departments is complex, the researchers used computer simulation to test its impact. They built a detailed model of three Saudi hospitals, using a week’s worth of real emergency department numbers for how many patients arrived each day, how long they waited, and how long treatment usually took. In this virtual environment they added biometric kiosks, the smart bracelets, and the three-layer cloud structure. They then ran many repeated simulations to see how patient flow changed while keeping the length of actual medical treatment the same.
What this could mean for patients
In the simulated hospitals, average waiting times dropped across all days of the week, and the number of patients treated per hour went up, even though doctors spent about the same amount of time with each person. The gains came from smoother admission—automatic identity checks, faster record finding, and early vital-sign collection—rather than from rushing the medical work itself. For patients, this could translate into shorter, less stressful waits and fewer unnecessary tests. For staff, it promises better use of existing resources and more complete information at the bedside, suggesting that a carefully designed hybrid cloud, combined with biometrics and simple wearable sensors, can make emergency care both faster and safer without sacrificing privacy.
Citation: Abughazalah, M., Alsaggaf, W., Saifuddin, S. et al. Enhancing patient admission efficiency through a hybrid cloud framework for medical record sharing. Sci Rep 16, 4926 (2026). https://doi.org/10.1038/s41598-026-35014-6
Keywords: electronic medical records, cloud healthcare, emergency department, biometric identification, IoT monitoring