Clear Sky Science · en
Comparison of human metabolome changes identified in a placebo-controlled amphetamine administration study versus those using forensic toxicology routine data
Why drug fingerprints in blood matter
When people take drugs such as amphetamine, they do not just change how they feel – they also leave subtle chemical fingerprints in their blood. These fingerprints, tiny molecules created or shifted by the body’s response to the drug, could one day help doctors and forensic scientists tell who has taken what, even when the drug itself is hard to detect. But carefully controlled human drug studies are rare and expensive, while forensic laboratories already sit on vast archives of real‑world blood samples. This study asks a simple but important question: can those routine forensic samples reliably stand in for gold‑standard clinical trials when we search for these hidden chemical clues?
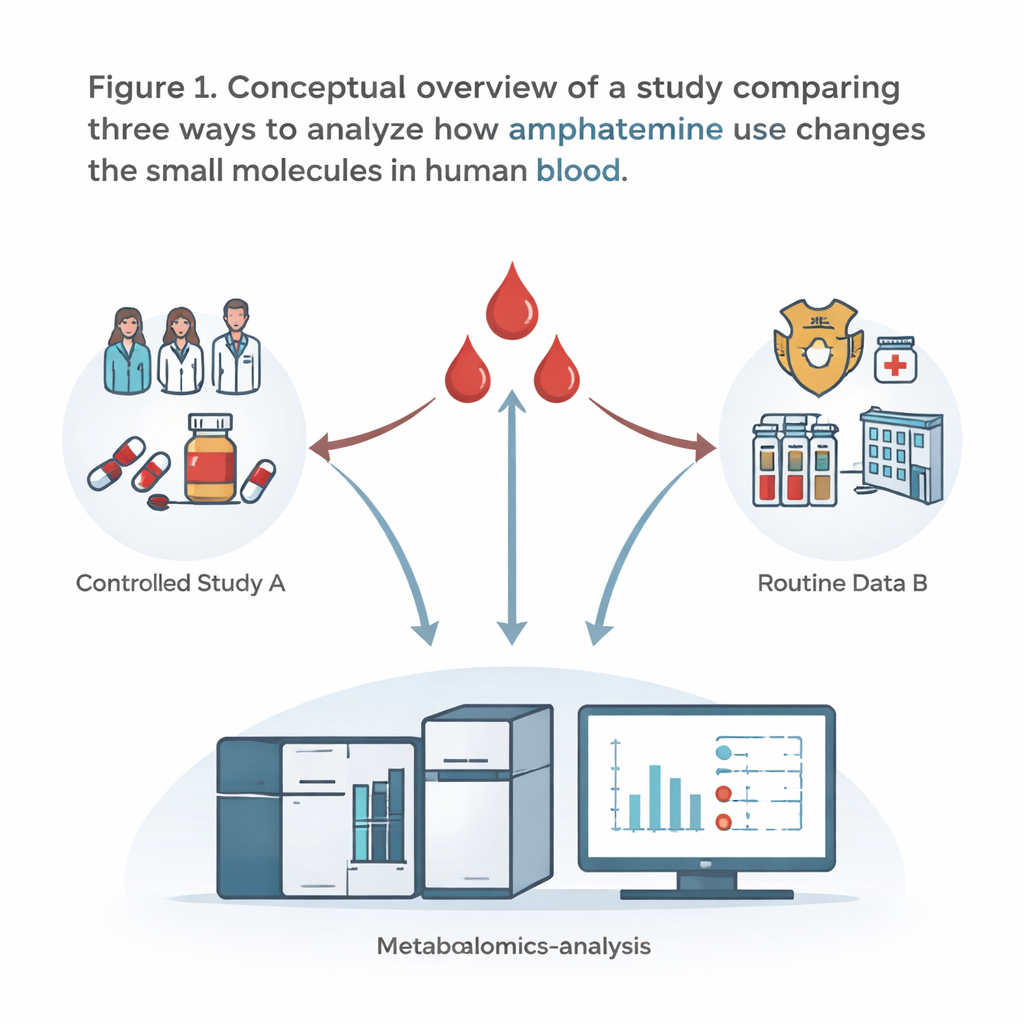
Three ways to look at amphetamine in the blood
The researchers focused on amphetamine, a common stimulant drug, and compared three different sources of human blood samples. In the first, the “controlled study,” healthy volunteers received a known dose of amphetamine or a placebo at a fixed time, and their blood was drawn exactly 3.5 hours later. In the second and third, the team used routine whole‑blood samples sent to a forensic toxicology lab by police and prosecutors in real legal cases. Some of these were positive for amphetamine, others negative. For one routine group, they re‑used the original measurement files; for the other, they thawed the same samples and re‑analyzed them together in a single run. This design let them directly compare tidy, well‑controlled research conditions with messy, everyday casework.
Reading the body’s chemical signals
Instead of targeting just a few known substances, the team used an “untargeted” technique called liquid chromatography–high‑resolution mass spectrometry. In practical terms, this instrument separates and weighs thousands of small molecules in each blood sample, then records their signal strength. Computer software pulls out individual “features” – distinct signals defined by their retention time and mass – and statistics are used to ask which ones differ between amphetamine‑positive and amphetamine‑negative samples. Because the identity of most signals is unknown at first, the comparison happens at the level of patterns rather than named compounds.
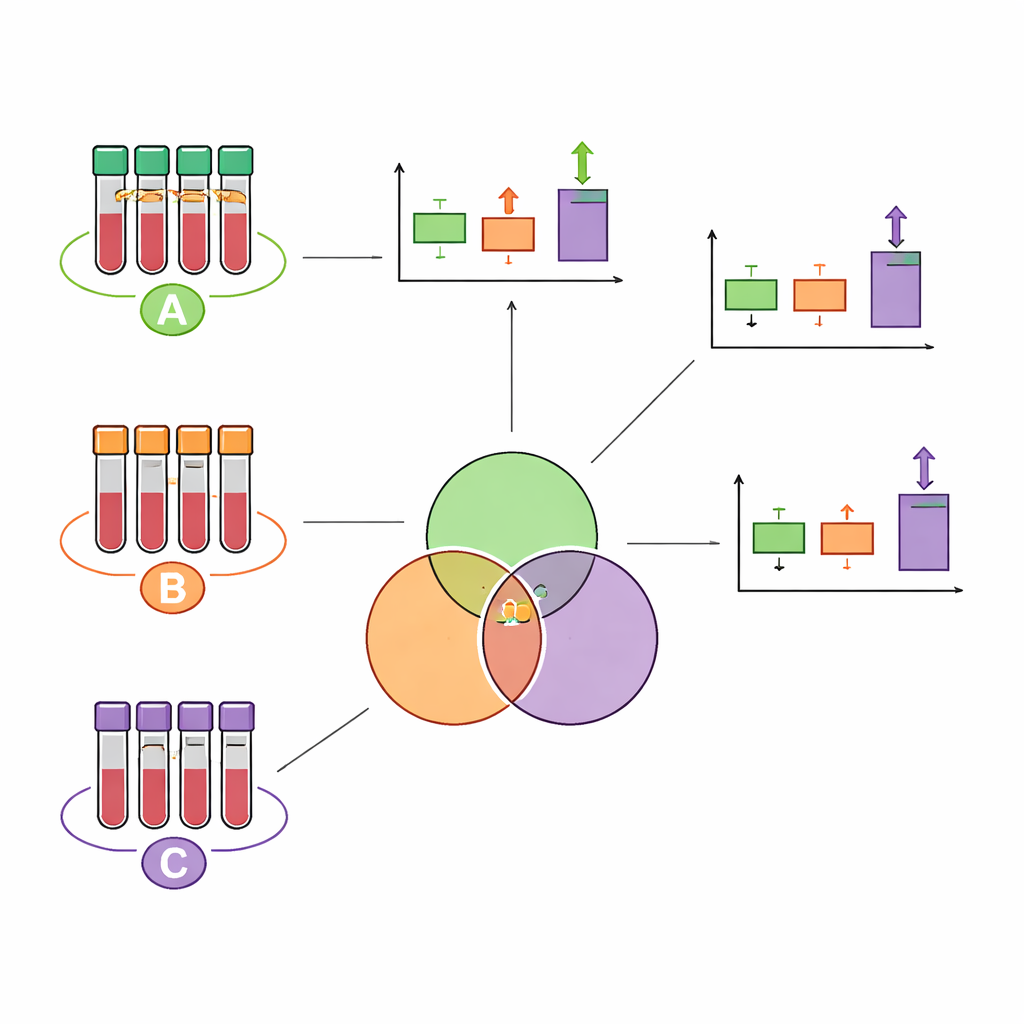
What matched and what did not
Across all three study types, more than 10,000 features passed quality filters, but only a small fraction showed statistically reliable differences between amphetamine‑positive and negative samples. In the tightly controlled clinical study, 31 features changed; in the two routine data sets, 130 and 75 features changed, respectively. Surprisingly, just three features were significant in all three study designs, and two of these turned out simply to be amphetamine itself and its main fragment in the instrument. Many features that shifted in the clinical trial did not do so consistently in the real‑world samples, and vice versa. Routine samples also showed much more scatter – likely caused by unknown drug doses, varying times since intake, different collection times of day, and additional lifestyle and medical factors that cannot be standardized in casework.
Strengths and limits of real‑world samples
Despite this patchy overlap, the study also revealed that routine forensic samples are not useless for metabolomics – far from it. Statistical checks with randomly grouped samples suggested that most of the detected differences were unlikely to be pure chance. Routine samples may even have advantages: people in real cases often take higher or repeated doses of amphetamine, which could amplify some biological changes that are weak or absent after a single controlled dose. However, to reliably see such effects amidst the noise, researchers will likely need larger groups of routine samples and careful matching on basic factors such as age, sex, and other drugs taken.
What this means for future forensic tools
For a layperson, the main message is that routine forensic blood samples can indeed help uncover chemical fingerprints of drug use, but they do not simply reproduce what is seen in clean clinical trials. The most robust common signal across all approaches remains the drug itself. More subtle changes in the body’s own chemistry are harder to pin down when many real‑world factors vary at once. The authors therefore see controlled, placebo‑based studies as the benchmark for understanding how a drug reshapes human metabolism, while large, carefully selected routine sample sets can complement this knowledge and bring it closer to everyday forensic practice.
Citation: Bovens, A., Leu, C., Brockbals, L. et al. Comparison of human metabolome changes identified in a placebo-controlled amphetamine administration study versus those using forensic toxicology routine data. Sci Rep 16, 4759 (2026). https://doi.org/10.1038/s41598-026-34985-w
Keywords: amphetamine, forensic toxicology, metabolomics, biomarkers, mass spectrometry