Clear Sky Science · en
Activation of M1mAChR’s improves spatial learning and memory deficits in rats exposed to chronic intermittent hypoxia
Why breathing at night matters for your memory
Many people with obstructive sleep apnea stop breathing over and over during the night, causing sharp drops in blood oxygen. Beyond loud snoring and daytime sleepiness, these brief suffocation-like episodes can quietly injure brain regions that support learning and memory. This study used a rat model to ask a simple but important question: can gently boosting one specific type of brain signal help protect memory circuits from the damage caused by repeated low-oxygen episodes?
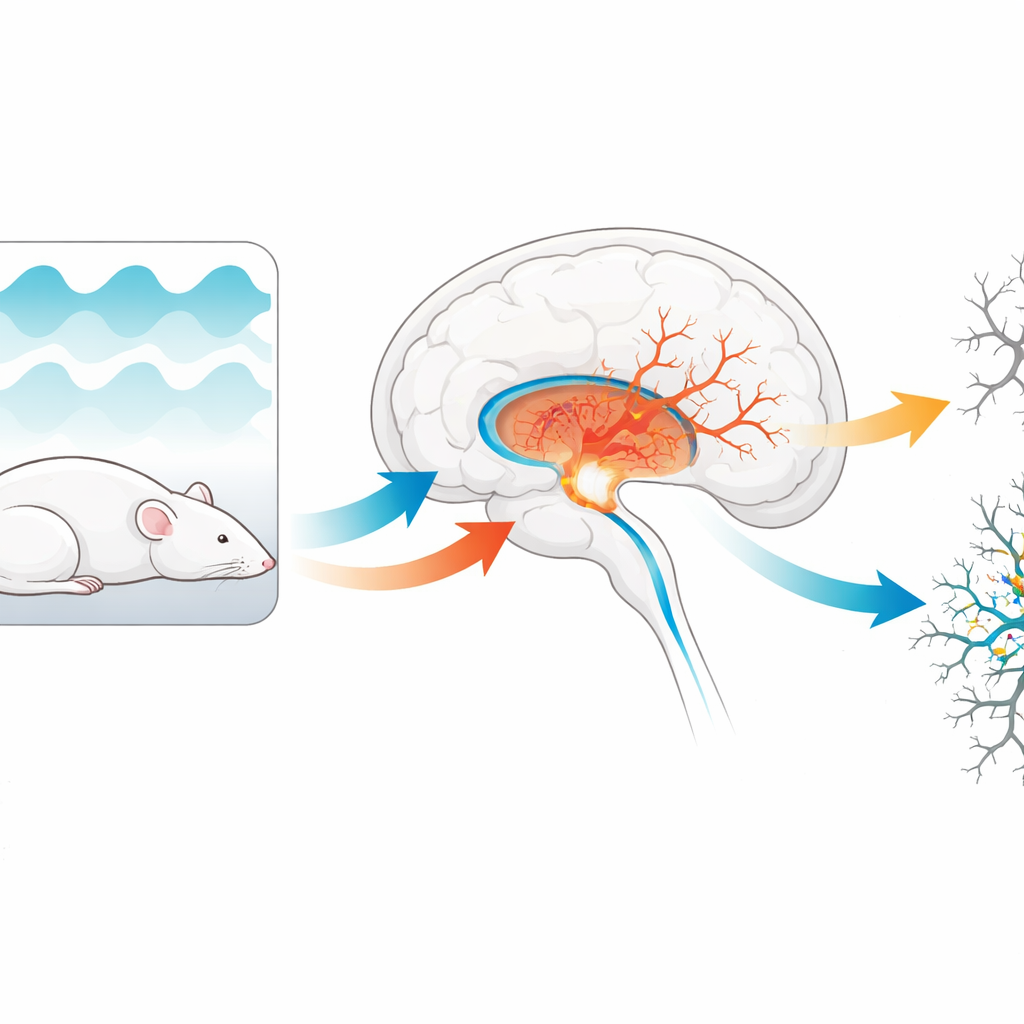
Sleep, oxygen dips, and a vulnerable memory center
Obstructive sleep apnea is marked by chronic intermittent hypoxia—rapid cycles of low and normal oxygen. The hippocampus, a deep brain structure crucial for forming spatial and everyday memories, is especially sensitive to such stress. Earlier work showed that apnea-like conditions can thin out neurons and disrupt the chemical conversations between them. Two signaling systems stand out in this story: a family of receptors that respond to the messenger acetylcholine (important for attention and memory) and an internal relay called the JAK2/STAT3 pathway that helps cells adapt and survive stress.
Testing apnea-like stress in the lab
To mimic sleep apnea, the researchers placed healthy rats in a chamber where oxygen levels repeatedly dropped and rose for eight hours a day over four weeks. Some animals only experienced this oxygen cycling, while others also received drugs that either blocked the JAK2/STAT3 relay or activated the M1 muscarinic acetylcholine receptor, a major acetylcholine-sensitive switch in the hippocampus. The team then measured how well the rats could learn the location of a hidden platform in a water maze and later remember where it had been. They also examined brain tissue to count neurons and to see how much of the key proteins M1 receptor and STAT3 were present.
What low oxygen did to learning and brain cells
Rats exposed to the apnea-like oxygen pattern struggled in the water maze. They took longer routes to find the platform and, when it was removed, spent less time searching in the correct area—signs of weakened spatial learning and memory. Under the microscope, their hippocampal neurons were fewer in number, more disorganized, and showed features of damage. At the molecular level, both total STAT3 and its active, switched-on form were reduced, as was the amount of M1 receptor in the hippocampus. In short, repeated oxygen dips dulled the very pathways thought to help neurons cope with stress and support memory.
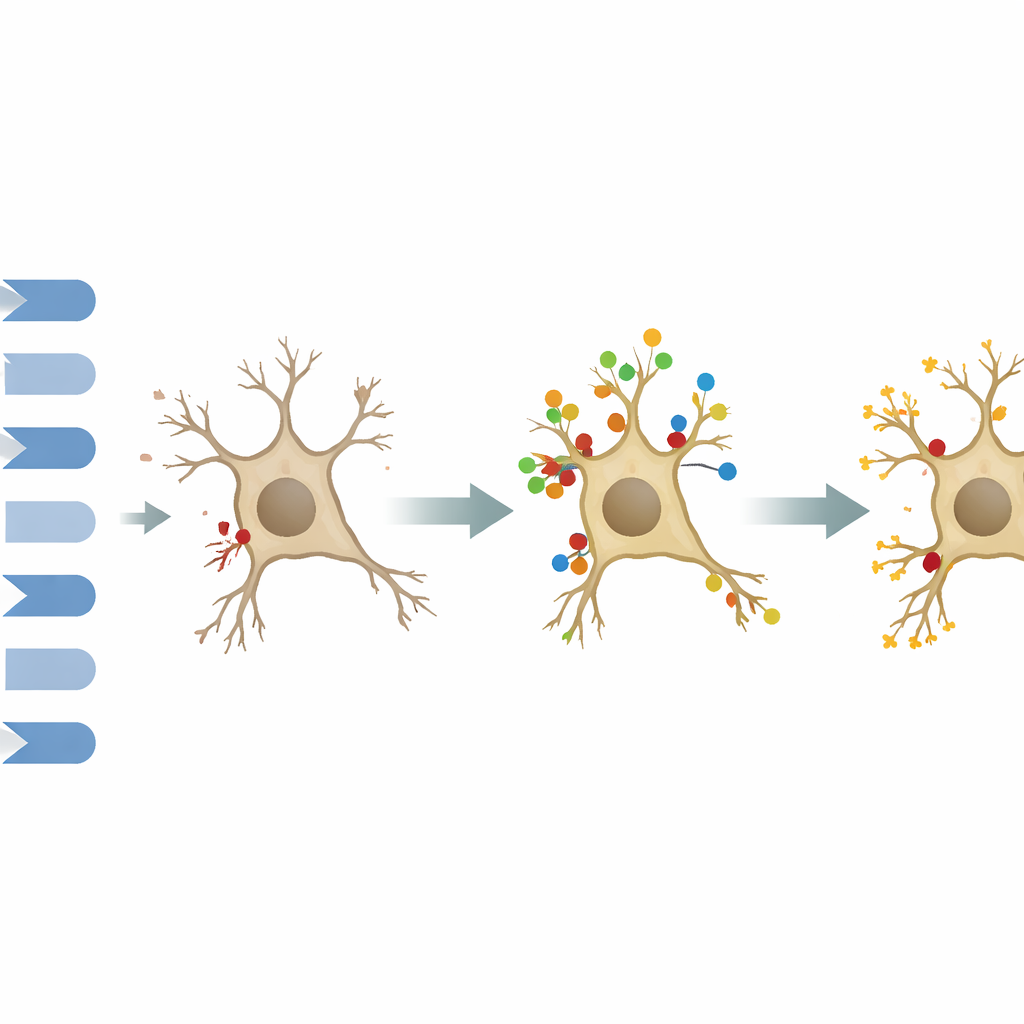
A protective switch with an important dependency
Turning on the M1 receptor with a selective drug, VU0364572, partly reversed these problems. Treated rats learned the maze more quickly and searched more accurately for the former platform location, and their hippocampal tissue showed better-preserved structure and higher M1 receptor levels. In contrast, blocking JAK2—a key upstream activator of STAT3—with the drug AG490 did not improve behavior and even erased the benefits of M1 activation when both drugs were given together. Interestingly, neither treatment restored STAT3 protein levels under these conditions, suggesting that what matters may be the integrity of the signaling route rather than its overall abundance.
What this means for people worried about snoring and memory
For a lay reader, the takeaway is that the brain’s response to oxygen swings during sleep is not fixed; it can be nudged toward injury or protection depending on which chemical switches are engaged. In this rat study, chronic intermittent low oxygen harmed memory circuits and reduced both a key surface receptor and an internal stress-response relay. Gently boosting the M1 receptor helped rats think and remember more clearly despite the oxygen stress, but only when the JAK2/STAT3 pathway was left intact. While this work is still far from a treatment for people, it highlights a promising strategy: pairing effective apnea care with drugs that shore up vulnerable memory networks, rather than targeting oxygen alone.
Citation: Huang, Q., Hu, C., Liu, H. et al. Activation of M1mAChR’s improves spatial learning and memory deficits in rats exposed to chronic intermittent hypoxia. Sci Rep 16, 8836 (2026). https://doi.org/10.1038/s41598-025-34689-7
Keywords: obstructive sleep apnea, intermittent hypoxia, hippocampus, learning and memory, acetylcholine receptors