Clear Sky Science · en
UV-induced immune modulation in the lung niche slows cancer progression
Sunlight and an Unexpected Cancer Clue
Most of us know that too much sun can cause skin cancer. This study turns that idea on its head by asking a surprising question: could a certain slice of sunlight—UVB radiation—actually help the body fight cancers that have spread to the lungs? By combining mouse experiments with data from thousands of people in the UK, the researchers explore how light on the skin can subtly tune the immune system inside the chest and potentially slow deadly tumors.
What the Scientists Wanted to Find Out
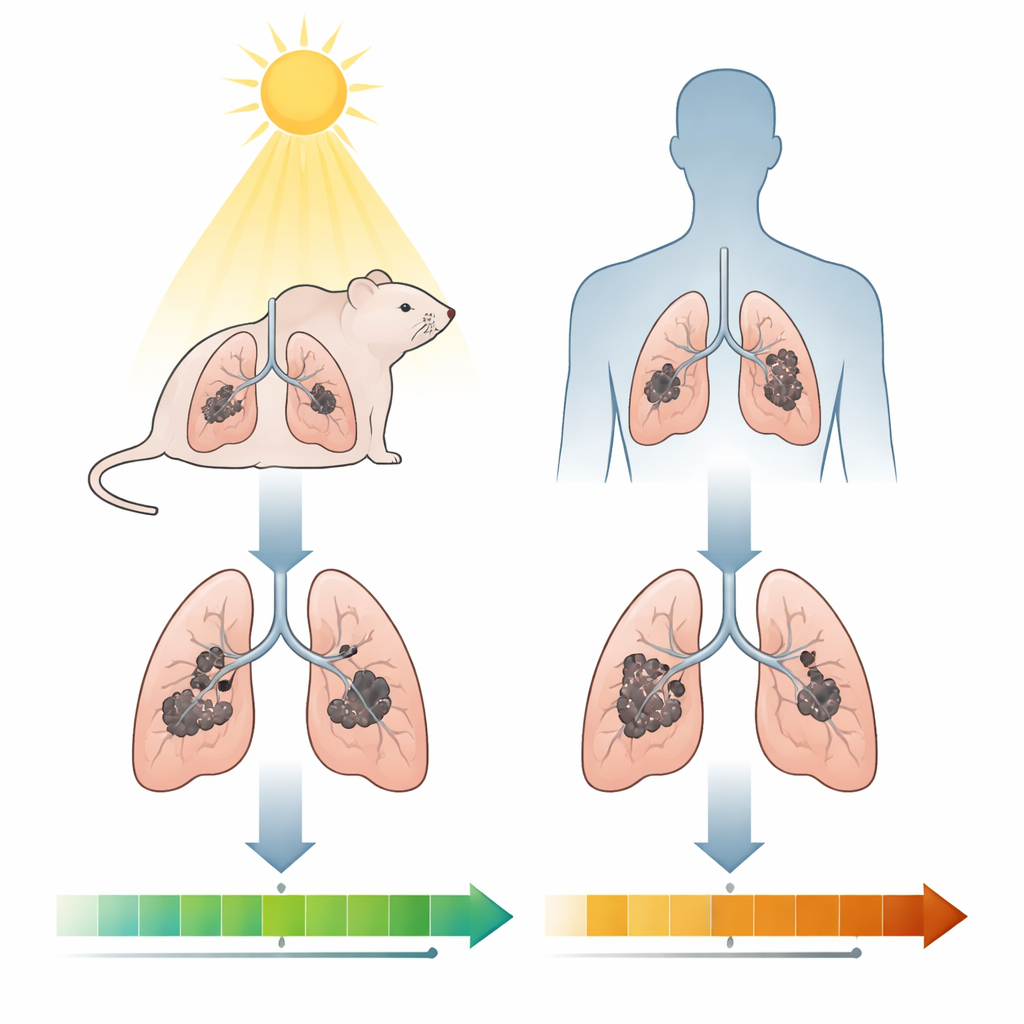
Ultraviolet B (UVB) light is notorious for burning skin and damaging DNA, but it also strongly shapes how immune cells behave. On the skin’s surface, UVB usually weakens protective immune reactions and can help melanomas grow. The big unknown was what happens in deep organs like the lungs, where immune cells constantly patrol for infections and stray cancer cells. The team asked whether controlled, repeated UVB exposure after melanoma cells had already seeded the lungs would make things worse—by further suppressing immunity—or might instead tilt the body toward a stronger anti-tumor response.
Testing Sunlight’s Effect in Mice
To explore this, the researchers injected melanoma cells into mice so the cells would travel through the bloodstream and form many small tumors in the lungs. A week later, once these microscopic colonies had started to grow, some mice were exposed to low doses of UVB light on their skin five times a week, while others went through the same handling without UVB. Over several weeks, the team tracked lung tumors using luminescent imaging and examined lung tissue under the microscope. Contrary to expectations based on skin cancer studies, the lung tumors in UVB-treated mice grew more slowly and remained smaller, and these mice lived somewhat longer than their non-irradiated counterparts.
How UV Light Reshapes Lung Immune Defenses
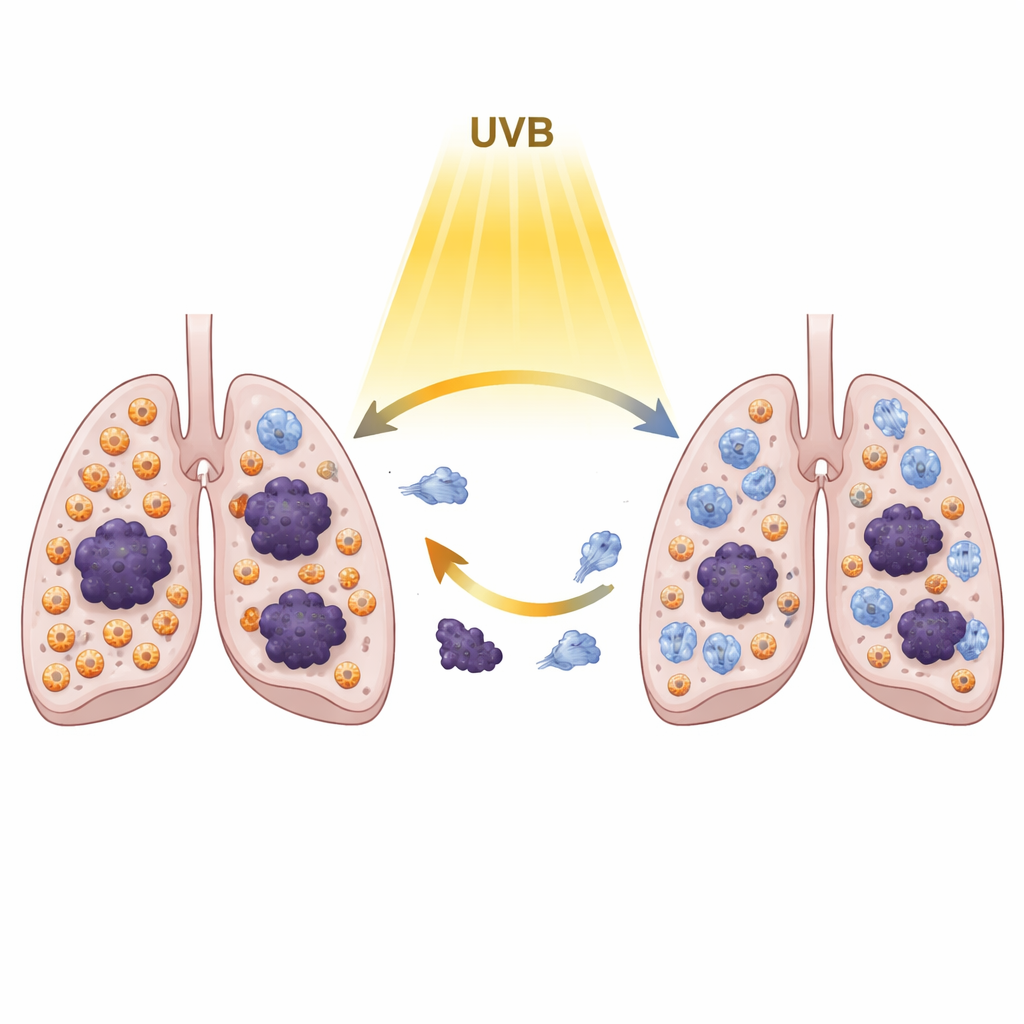
Slower tumor growth hinted that the immune “neighborhood” inside the lungs had changed. To see which cells were involved, the scientists isolated immune cells from lung tumors and analyzed them one by one using high-dimensional mass cytometry, a technique that tags dozens of markers on each cell. They found that UVB exposure did not boost classic suppressive T cells or checkpoint molecules that often shut down cancer-fighting responses. Instead, it shifted the balance among innate immune cells: there was a clear rise in a particular neutrophil population and a drop in certain inflammatory monocytes. Blood tests also showed lower levels of two signaling proteins, IL-6 and IL-10, which are often linked to cancer-promoting inflammation. Together, these changes suggest that UVB can quietly reprogram the lung environment so that it becomes less welcoming to metastases, even while UVB remains immunosuppressive in the skin itself.
Looking for Signals in Human Populations
Mouse experiments are powerful but controlled; people live in far more varied conditions. To see if a similar story might hold in humans, the researchers turned to the UK Biobank, a large study following hundreds of thousands of volunteers over many years. They focused on more than 3,000 individuals diagnosed with lung cancer and estimated how much solar radiation their home locations received on average each year. After accounting for factors such as age, smoking, body weight, socioeconomic status, and when the cancer was diagnosed, those living in sunnier areas had a lower risk of dying from lung cancer. For example, people in regions with solar radiation typical of southern England had a predicted five‑year survival of about 28%, compared with 20% for those in darker regions similar to central Scotland—a modest but meaningful gain.
What This Could Mean for Patients
Taken together, the mouse and human data suggest that UVB exposure may do more than tan the skin: it may fine-tune immune activity in the lungs in ways that can slow tumor growth. The findings do not imply that people should sunbathe recklessly, nor that sunlight is a cure for cancer. Instead, they point toward a more nuanced picture in which carefully controlled UVB—such as medical phototherapy already used for skin diseases—might one day be harnessed to support anti-cancer immunity in select patients, without broadly shutting down the immune system. Future clinical studies will be needed to test how safe, targeted light exposure could complement existing treatments while still guarding against the well-known risks of too much sun.
Citation: Maliah, A., Parikh, S., Stevenson, A.C. et al. UV-induced immune modulation in the lung niche slows cancer progression. Sci Rep 16, 8290 (2026). https://doi.org/10.1038/s41598-025-33900-z
Keywords: UVB radiation, lung cancer, melanoma metastasis, tumor immunity, sunlight exposure