Clear Sky Science · en
Analysis of factors associated with cervical cancer and precancerous lesions
Why this study matters to everyday women
Cervical cancer is one of the few cancers we can largely prevent, yet it still claims hundreds of thousands of women’s lives each year. This study from a large hospital in Hangzhou, China, follows nearly 3,000 women who had samples taken from their cervix to understand which real‑world factors are most closely tied to early cervical changes and cancer. By clarifying the roles of common infections, childbirth history, screening tests, and vaccination, the research points to practical steps women, families, and health systems can take to keep this cancer at bay.
Looking closely at the cervix
The researchers analyzed data from 2,998 women aged 16 to 76 who underwent cervical biopsy over one year. Using tissue findings, they divided women into four groups: no abnormal change, mild changes, serious precancerous changes, and cervical cancer. They also gathered information on age, pregnancies and births, contraceptive habits, smoking, whether women had received the HPV vaccine, and results from common screening tests that look for abnormal cells and high‑risk human papillomavirus (HPV), the virus known to trigger most cervical cancers. This allowed them to compare who developed more dangerous lesions and which background features these women had in common.
The central role of a common virus
HPV infection emerged as the clearest driver of dangerous cervical changes. More than 88% of all women in the study carried high‑risk HPV types, and these infections appeared in over 95% of women with serious precancerous lesions or cervical cancer. Two types, known as HPV16 and HPV18, were especially worrisome: they were present in about a quarter of women with mild changes but in roughly half of those with serious precancerous lesions and nearly two‑thirds of those with cancer. In statistical models that considered several factors at once, the severity of HPV infection strongly predicted whether a woman’s biopsy would show serious disease, confirming that persistent high‑risk HPV is the main spark for cervical cancer to develop.
Childbirth history and other everyday factors
Beyond infection, the number of times a woman had given birth was meaningfully linked to serious cervical disease. Women with more deliveries had about double the risk of precancerous or cancerous lesions compared with those with fewer births. This likely reflects repeated stretching and healing of the cervix during pregnancy and delivery, which may make it easier for HPV to enter and damage cells. In contrast, age alone, the number of pregnancies or abortions, condom use, and smoking did not show a clear statistical connection in this group, although other studies suggest they may still play supporting roles. Notably, only 13.7% of women in the study had received any HPV vaccine, highlighting a major missed opportunity for prevention.
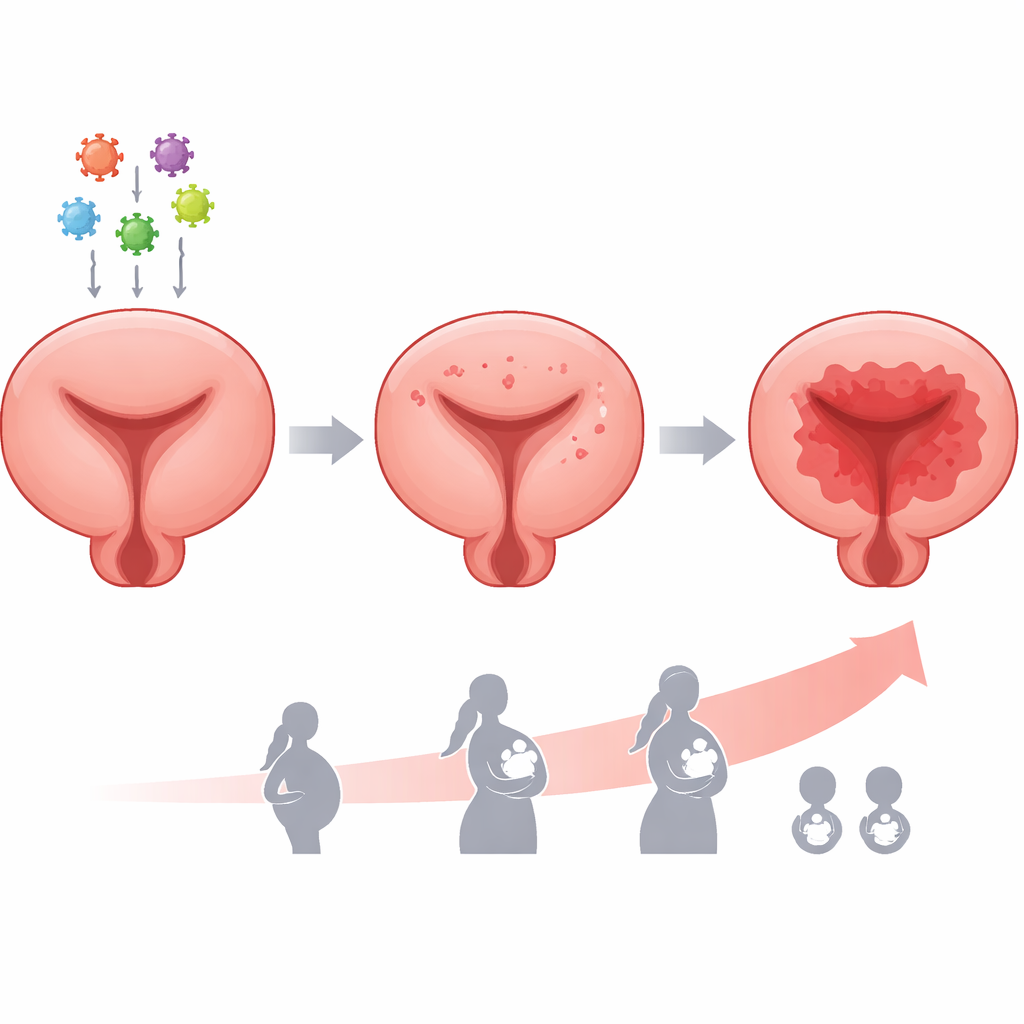
What screening tells us about early warning
The team also tested how well different screening approaches spotted serious cervical changes. A cell‑based test alone, which looks at a smear from the cervix under a microscope, detected fewer than one in five dangerous lesions. When this test was combined with HPV screening, sensitivity soared to about 98%, meaning very few high‑grade lesions were missed. In a smaller group of women who were followed for a year after biopsy, most cervical abnormalities either improved or stayed stable; only a handful worsened to more dangerous disease. These follow‑up results suggest that catching and treating precancerous lesions early can successfully slow or stop progression to cancer.
Turning findings into protection
In plain terms, this study shows that persistent infection with high‑risk HPV—especially types 16 and 18—and having many births are the key ingredients that push cervical cells from normal to precancerous to cancerous. Other suspected influences, such as age or smoking, were less obvious in this particular group. For women, the take‑home message is clear: vaccination against HPV before exposure, regular screening that includes an HPV test, and timely treatment of serious precancerous lesions can dramatically cut the risk of cervical cancer. Combined with thoughtful family planning and good sexual‑health education, these tools offer a powerful roadmap for lowering both the incidence of cervical disease and the number of lives lost to it.
Citation: Hu, D., Zhao, Y., Han, M. et al. Analysis of factors associated with cervical cancer and precancerous lesions. Sci Rep 16, 9600 (2026). https://doi.org/10.1038/s41598-025-32215-3
Keywords: cervical cancer, HPV infection, precancerous lesions, cancer screening, HPV vaccination