Clear Sky Science · en
Neuropeptides neurotensin and substance P accelerate diabetic wound healing by modulating immunity and the skin microbiome
Why slow-healing wounds matter
For many people with diabetes, a small blister or cut on the foot can turn into a stubborn, dangerous wound that refuses to close. These chronic sores, known as diabetic foot ulcers, are a leading cause of infection and amputation. The new study explores whether tiny nerve-derived molecules placed directly on the skin can help these wounds heal faster, not by killing germs like an antibiotic, but by calming runaway inflammation and gently steering the skin’s resident bacteria back toward a healthier balance.
Two tiny messengers on the skin
The researchers focused on two naturally occurring messengers called neurotensin and substance P. These molecules are made by nerve cells and are already known to influence blood flow, tissue repair, and immune responses. In diabetes, their levels in the skin tend to drop, just as wound healing becomes impaired. To test whether replacing them could help, the team created small full-thickness wounds on the backs of healthy and diabetic mice. Each day, they applied a simple saline solution, neurotensin, or substance P directly onto the wounds and carefully tracked how quickly the injured skin closed over ten days, while also examining immune cells and skin bacteria.
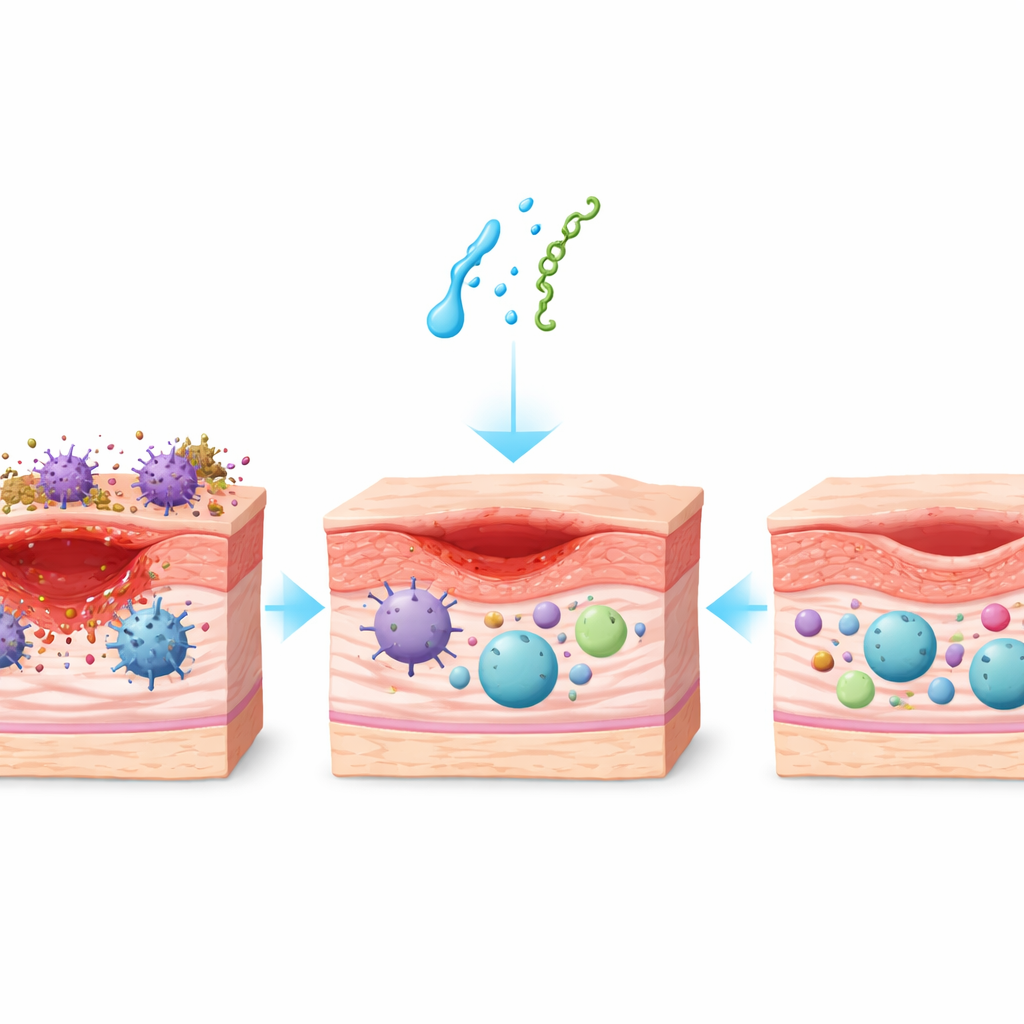
Faster closure of stubborn wounds
As expected, diabetic mice healed more slowly than healthy mice, with wounds lingering open and inflamed. When treated with either neurotensin or substance P, however, the picture changed. In both healthy and diabetic animals, wounds shrank more quickly, and the benefit was especially striking in diabetes. On average, peptide-treated diabetic wounds closed roughly a day and a half sooner than untreated diabetic wounds and even outperformed the wounds of untreated healthy mice. Substance P produced the strongest effect, trimming the time needed to reach key healing milestones such as 50% closure.
Calming the body’s overactive defenses
Slow healing in diabetes is driven in part by an immune system stuck in attack mode. The team looked closely at immune cells in the wound, focusing on macrophages—cells that can adopt a harsh, microbe-fighting “M1” state or a gentler, repair-focused “M2” state. Diabetic wounds were crowded with M1 cells and short on M2 cells, signaling ongoing inflammation. Topical neurotensin and especially substance P shifted this balance: aggressive M1 cells decreased, and pro-healing M2 cells increased, restoring a profile similar to that seen in healthy skin. Other inflammatory cells, including T cells and neutrophils, also fell back toward normal levels with treatment, indicating that the peptides helped the wound move from a chronic defensive stance into a resolution and repair phase.
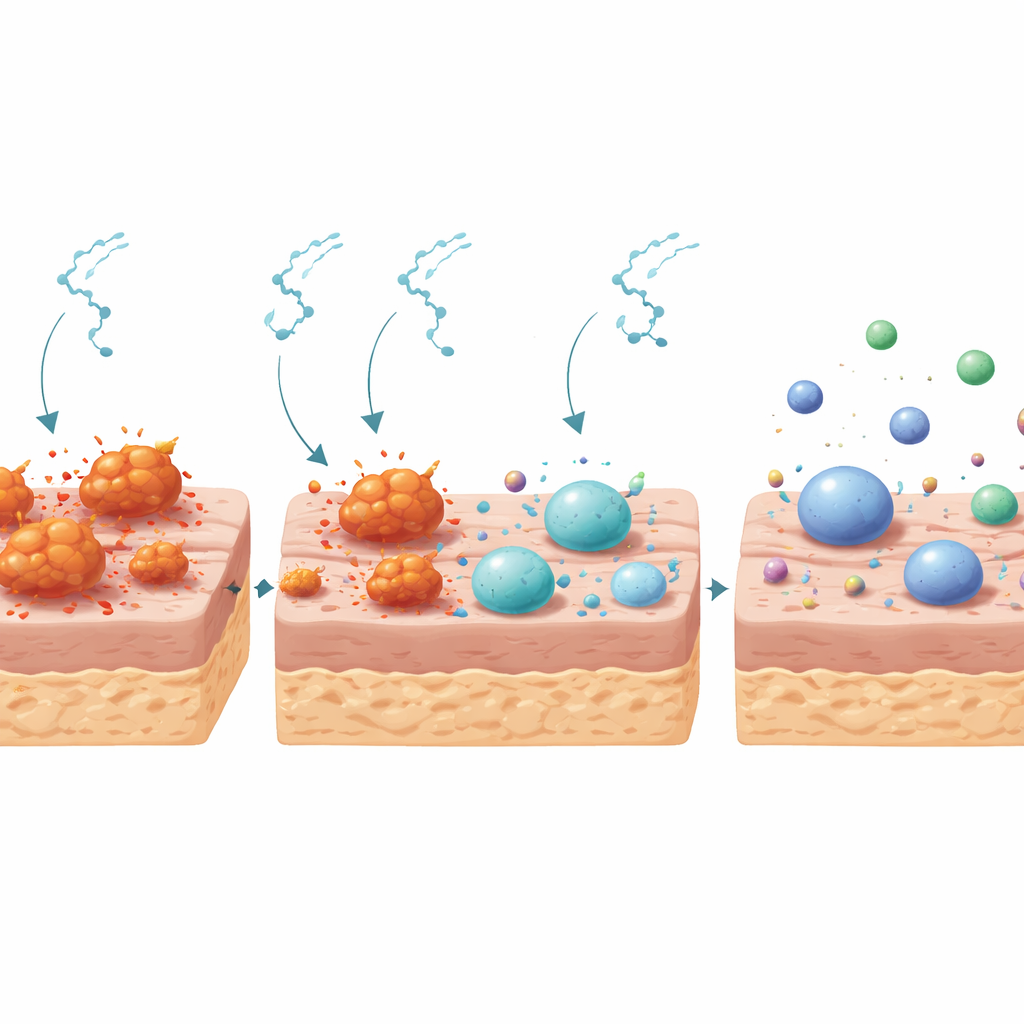
Helping friendly microbes return
The outer layer of skin is home to vast communities of bacteria that usually work with the body to maintain health. In the diabetic mice, this microbial neighborhood was distorted: a single group of bacteria, dominated by Staphylococcus, overwhelmed other species, and certain genera linked to poor healing, such as Aerococcus and Weissella, appeared only in diabetic animals. After ten days of treatment, the bacterial picture shifted. In diabetic wounds treated with substance P, the abundance of Staphylococcus and several other potentially harmful groups fell sharply, while beneficial or neutral bacteria common in non-diabetic skin, including Lactobacillus and related types, became more prominent. Overall, the treated diabetic microbiome became more evenly balanced and more closely resembled that of healthy mice, suggesting that the peptides nudged the skin ecosystem away from a chronic, infection-prone state.
Joining nerves, immunity, and microbes
Taken together, the findings point to a dual action for neurotensin and substance P. Applied as a simple topical treatment, they help diabetic wounds close faster by simultaneously dialing down excessive inflammation and reshaping the skin’s microbial residents toward a healthier mix. Rather than acting like classic antibiotics that directly kill bacteria, these neuropeptides appear to restore harmony at the interface of nerves, immune cells, and microbes. While the work was done in mice and many steps remain before use in patients, it suggests that boosting the body’s own messenger molecules could offer a new way to heal chronic diabetic wounds while reducing reliance on long courses of conventional antibiotics.
Citation: Maranha, A., Leal, E.C., Alarico, S. et al. Neuropeptides neurotensin and substance P accelerate diabetic wound healing by modulating immunity and the skin microbiome. Sci Rep 16, 9456 (2026). https://doi.org/10.1038/s41598-025-30723-w
Keywords: diabetic wound healing, skin microbiome, substance P, neuropeptides, chronic inflammation