Clear Sky Science · en
Evaluation of artificial intelligence identified ipratropium bromide for the treatment of coronavirus disease 2019
Why an asthma drug for COVID-19 matters
As the world continues to live with COVID-19, vaccines alone have not solved the problem of severe illness, especially when new variants emerge. This study explores an unexpected helper: ipratropium bromide, a long‑used inhaled medicine for asthma and chronic lung disease. Using artificial intelligence to sift through thousands of existing drugs, researchers pinpointed this familiar inhaler as a promising treatment to ease dangerous lung inflammation and blood‑clot problems seen in severe COVID-19. Their work suggests that an inexpensive, widely available drug might help protect the lungs and blood vessels from the worst complications of the disease.
Smart computers searching old drugs for new jobs
Instead of starting from scratch to invent a new medicine, the team used a commercial artificial intelligence platform called RAPTOR AI to “listen in” on how genes are switched on and off in COVID-19 patients. They collected blood samples from people with mild and severe disease, both at the time of diagnosis and later, during recovery. By reading out which genes were active in each sample, the system built a gene‑expression fingerprint of severe illness versus recovery. RAPTOR AI then compared these fingerprints with gene patterns produced by more than 23,000 chemicals tested in other experiments. The goal was simple: find drugs that could push the severe COVID-19 pattern toward the safer, recovery‑like pattern.
A familiar inhaler rises to the top
From this massive digital search, ipratropium bromide stood out as the top candidate, even outranking the antiviral drug remdesivir, which is already used in hospitals. Ipratropium is an inhaled medicine that relaxes and opens the airways by blocking certain nerve signals in the lungs. Earlier work had hinted that it could also calm inflammation and might even interfere with the virus’s ability to damage lung tissue. The AI analysis highlighted pathways linked to immune overreaction and blood‑clot formation, suggesting that ipratropium might not just help breathing but also soften the “storm” of inflammation that drives severe COVID-19.
Putting the AI prediction to the test in animals
To move beyond computer predictions, the researchers tested ipratropium in a hamster strain that develops COVID-19 symptoms resembling those in very sick human patients, including breathing trouble, fever swings, and organ damage. Animals were infected with the SARS‑CoV‑2 virus and then treated with either a neutral solution (vehicle), remdesivir, ipratropium by nebulizer, or both drugs together. In untreated infected hamsters, 70% died, losing a great deal of weight, developing intense lung inflammation, and showing signs of widespread blood clotting. In striking contrast, only 5% of the ipratropium‑treated animals died, and they lost far less weight. Their body temperature, which initially dropped as disease worsened, recovered more quickly than in the untreated group.
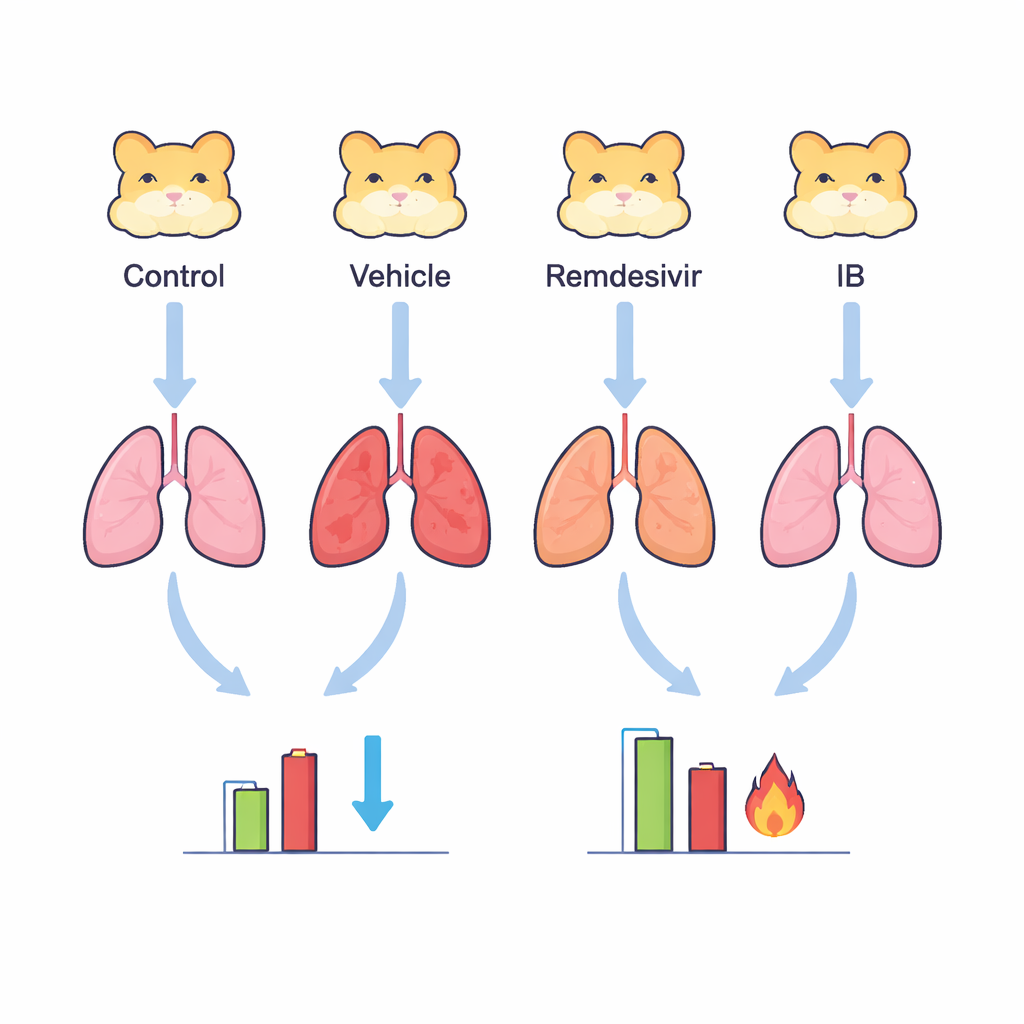
Less clotting, calmer lungs
Severe COVID-19 is notorious not only for attacking the lungs but also for triggering dangerous clots that can lead to heart attacks, strokes, and lung embolisms. The team measured blood markers linked to clotting, including D‑dimer and fibrin degradation products. These markers were much lower in animals that received ipratropium than in untreated animals, suggesting that clot formation was reduced. Levels of key inflammatory molecules in the blood, such as interleukin‑6 and tumor necrosis factor‑alpha, also dropped with ipratropium treatment. When the researchers examined lung tissue under the microscope, they saw far fewer inflammatory cells and less viral damage in the ipratropium group than in the vehicle group. In many cases, the lungs of treated animals looked close to normal.
What this could mean for future care
For non‑specialists, the key message is that a decades‑old inhaler, already familiar to many asthma and chronic lung disease patients, may do far more than simply open narrowed airways. Guided by artificial intelligence, this study shows that ipratropium bromide can strongly reduce death, clotting, and lung inflammation in an animal model of severe COVID-19, performing at least as well as, and in some ways better than, remdesivir. While more research and careful clinical trials in people are needed, the results suggest a hopeful possibility: existing, affordable inhaled medicines could become part of a broader toolkit to prevent the worst outcomes of COVID-19 and perhaps other severe lung infections.
Citation: Jung, DS., Cheon, S., Kim, CM. et al. Evaluation of artificial intelligence identified ipratropium bromide for the treatment of coronavirus disease 2019. Sci Rep 16, 6980 (2026). https://doi.org/10.1038/s41598-025-27869-y
Keywords: COVID-19 treatment, ipratropium bromide, drug repurposing, artificial intelligence in medicine, lung inflammation