Clear Sky Science · en
Polysomnography Dataset for Sleep Analysis in Ischemic Stroke Patients
Why Sleep After Stroke Deserves Attention
Many people know that sleep is important, but fewer realize how deeply it affects the brain’s ability to heal after injury. This study introduces iSLEEPS, a large new collection of detailed overnight sleep recordings from people recovering from ischemic stroke in India. By making these data freely available, the authors hope to speed up discoveries about how breathing problems during sleep influence stroke recovery and to help engineers build smarter tools that can automatically read sleep tests.
Stroke, Troubled Breathing, and a Missing Piece
Stroke is a leading cause of long‑term disability, and breathing problems during sleep—especially pauses in breathing called sleep apnea—are strikingly common in stroke survivors. These breathing disturbances can double the risk of another stroke and are linked to poorer recovery in day‑to‑day function. Doctors use an overnight test called polysomnography, which tracks brain waves, eye and muscle activity, heart rhythm, breathing, and oxygen levels, to diagnose these problems. Yet, despite its importance, there have been very few large, open datasets of such recordings from stroke patients, particularly from non‑Western countries. Existing public databases are small, focus on people without stroke, or lack the detailed markings needed to study how sleep and stroke interact.
What the iSLEEPS Collection Contains
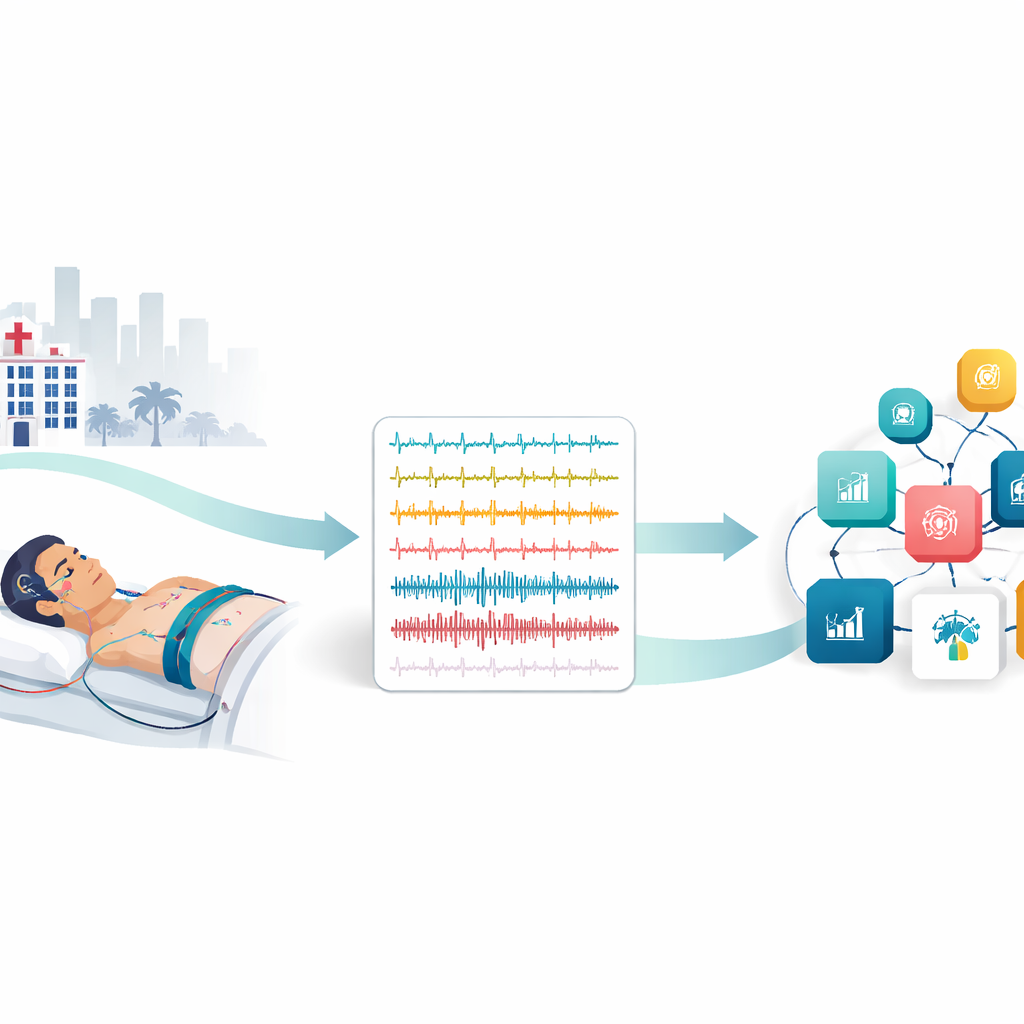
The iSLEEPS dataset fills this gap with 100 overnight recordings from adults who had an ischemic stroke within the previous month, all studied at a major neuroscience hospital in Bengaluru, India. Each participant spent a night connected to multiple sensors that captured brain waves, eye movements, muscle tone, heart rhythm, airflow, chest and belly movement, oxygen levels, snoring sounds, and body position. On average, each study lasted about eight hours, and together they add up to nearly 800 hours of data. Trained scorers, supervised by a sleep specialist, reviewed the recordings in 30‑second slices, labeling when the person was awake, in light sleep, deep sleep, or dreaming sleep, and marking breathing pauses, shallow breathing, drops in oxygen, and brief arousals.
Who the Patients Are and How Their Sleep Looks
The participants represent a real‑world mix of stroke patients: common conditions such as diabetes, heart disease, and obesity were not excluded. The average age is just over 50 years, with more men than women, reflecting the higher risk of sleep apnea in men. Analysis of the recordings shows that breathing problems during sleep are widespread in this group. Only a small minority have normal breathing, while most fall into mild, moderate, or severe apnea categories based on how many breathing disruptions occur per hour of sleep. The dataset carefully tallies different types of events—such as obstructive apnea, when the airway collapses; central apnea, when the brain briefly stops sending breathing signals; and hypopnea, a partial reduction in airflow—along with how often they happen at each severity level.
Testing the Data With Modern Algorithms
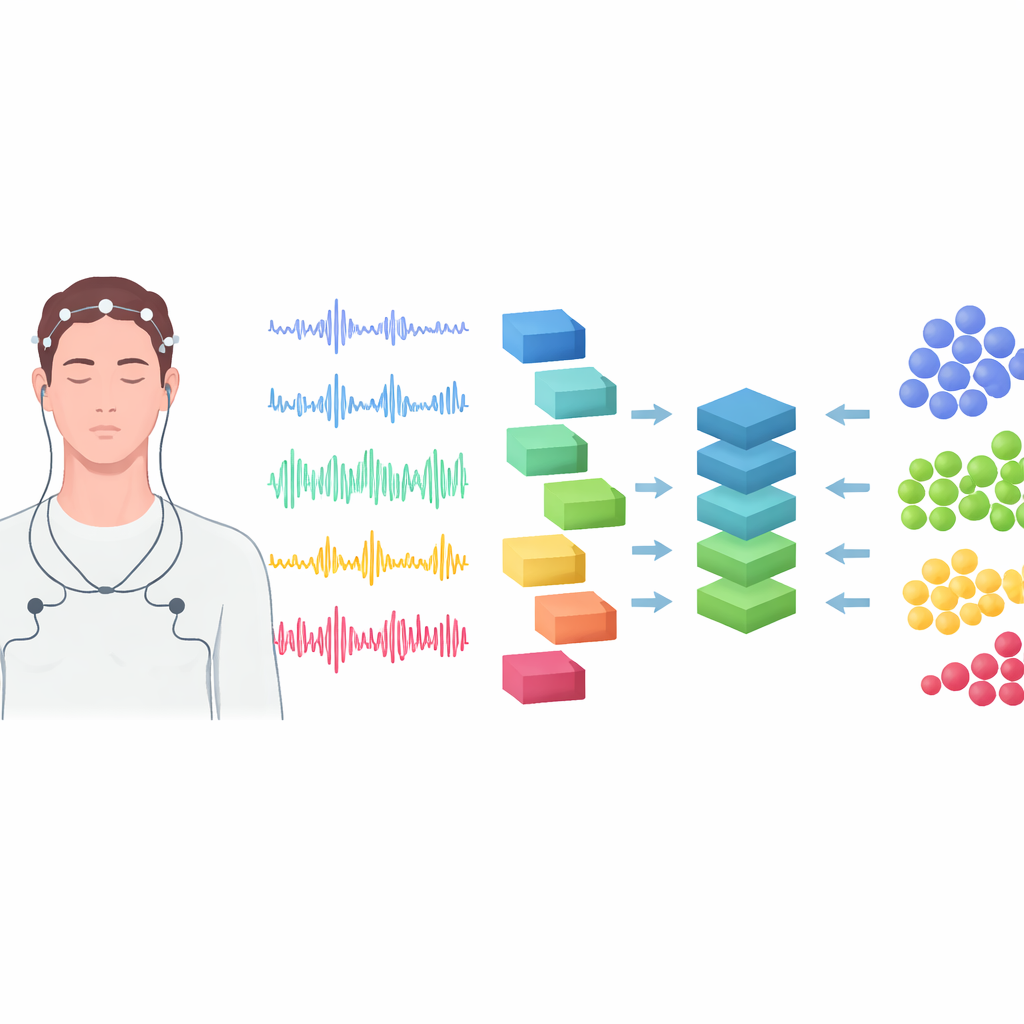
To show how iSLEEPS can be used, the researchers trained several modern deep learning models to automatically assign sleep stages from single channels of brain or eye‑movement signals. They compared a convolutional network, a long short‑term memory network, and a transformer‑based model, each designed to learn patterns in time‑series data. The algorithms were trained and tested carefully so that data from any one patient never appeared in more than one set, and performance was checked using repeated cross‑validation. Among these methods, the long short‑term memory model performed best, correctly labeling sleep stages about three‑quarters of the time. However, the results were noticeably weaker than similar models achieve in healthy volunteers, underscoring that stroke alters sleep in ways that current automated systems do not yet fully capture.
Opening the Door to Better Care
By releasing iSLEEPS as an open, well‑documented dataset—complete with anonymized recordings, detailed event markings, and basic clinical information—the authors provide a powerful new resource for scientists, clinicians, and engineers. Researchers can use it to probe how disturbed sleep and breathing shape stroke recovery, to compare patients across countries, and to build and test new algorithms that might one day screen for dangerous breathing problems automatically, even outside specialized sleep labs. For patients and families, the ultimate promise of this work is clearer diagnosis and more timely treatment of sleep problems after stroke, potentially improving both recovery and quality of life.
Citation: Maiti, S., Sharma, S.K., Mythirayee, S. et al. Polysomnography Dataset for Sleep Analysis in Ischemic Stroke Patients. Sci Data 13, 421 (2026). https://doi.org/10.1038/s41597-026-06747-w
Keywords: stroke, sleep apnea, polysomnography, sleep dataset, deep learning