Clear Sky Science · en
SexTumorDB: a comprehensive resource of sex-dependent tumor landscape at single-cell resolution
Why Men and Women Get Different Cancers
Doctors have long known that men and women do not experience cancer in the same way. Some tumors are more common in men, some in women, and they often respond differently to the same treatments. Yet, for years, most cancer research has treated the sexes as interchangeable. This article introduces SexTumorDB, a new open database that lets scientists zoom in on millions of individual cells from human tumors to uncover how biological sex shapes cancer in the body.
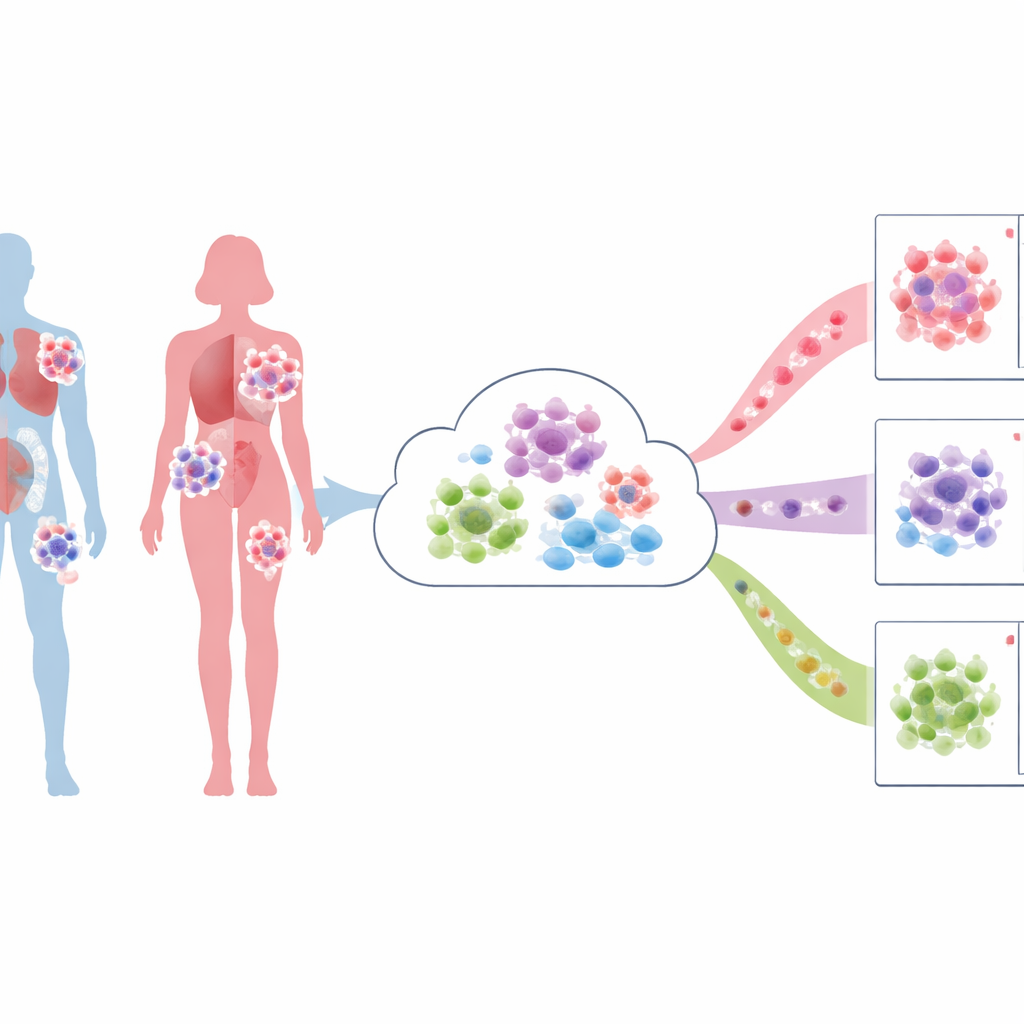
A New Map of Tumors Cell by Cell
Instead of looking at tumors as uniform lumps, SexTumorDB breaks them down into more than two million single cells. These cells come from 532 samples drawn from 13 common cancers that do not involve the reproductive organs, such as lung, liver, colon, bladder, and brain tumors. Each cell carries a readout of which genes are turned on or off, allowing researchers to see not only cancer cells but also immune cells and support cells that surround them. Crucially, every sample is linked to whether it came from a male or female patient, turning the database into a powerful tool for studying sex-based differences.
Careful Selection to Avoid Hidden Bias
To build a reliable resource, the team first combed through public cancer studies and set strict entry rules. They required single-cell or single-nucleus RNA sequencing data, clear records of donor sex, samples taken from the original tumor site, and patients who had not yet received treatment, to avoid drug-related changes. They also favored a widely used sequencing platform to reduce technical differences between studies. After this screening, they assembled data across multiple organs and disease types, including both tumors and nearby or healthy tissues, and removed samples that did not meet quality standards.
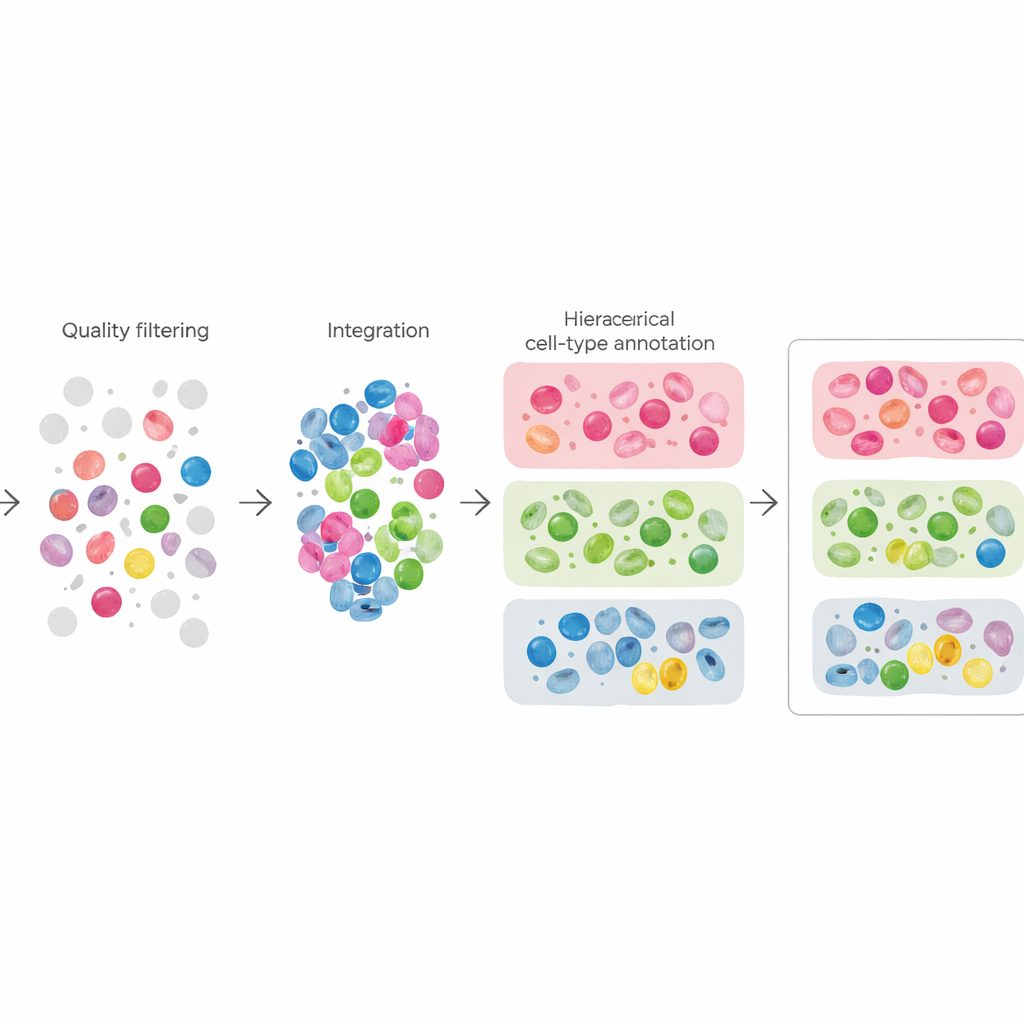
Turning Raw Data into a Common Language
The researchers then passed all datasets through a shared processing pipeline so that cells from different hospitals and studies could be compared directly. They checked the quality of each cell, filtered out damaged or ambiguous ones, and harmonized gene names. Using specialized software, they corrected for technical batch effects and projected the cells into maps where each dot represents a single cell. On top of this, they applied a three-level labeling system: every cell is first tagged as tumor, normal, immune, or stromal (support), then grouped into 33 major types such as T cells, fibroblasts, or epithelial cells, and finally annotated with more detailed subtype names drawn from original studies or manual expert review.
Ensuring Sex and Malignancy Are Correct
Because sex is central to the database, the authors double-checked the sex labels rather than simply trusting the original studies. They used well-known genes that behave differently in males and females, including genes located on the Y chromosome and a gene called XIST, which is active mainly in female cells. Across all datasets, male samples showed the expected Y-linked signatures, and female samples showed strong XIST activity, confirming that sex had been correctly assigned. To distinguish truly malignant tumor cells from lookalike normal cells, they applied a lightweight machine-learning tool and compared its results to existing labels, finding high agreement and further boosting confidence in the data.
Tools for Scientists Everywhere
Recognizing that not every laboratory has access to powerful computers or expert programmers, the team created lighter, downsampled versions of the data and built interactive web applications. These online tools let users explore tumor, immune, and stromal cells one compartment at a time, visualize how cell types differ between male and female patients, and download standardized datasets and metadata. The entire resource, along with the processing code, has been made freely available through public repositories so that others can reproduce or extend the work.
What This Means for Future Cancer Care
SexTumorDB does not provide a new drug or cure on its own, but it lays the groundwork for treatments that respect biological differences between men and women. By offering a clean, unified view of how millions of individual cells behave in male and female tumors, the database helps researchers pinpoint sex-specific weaknesses in cancer cells and in the surrounding immune system. Over time, discoveries drawn from this resource could guide more tailored screening strategies and therapies, moving cancer care closer to truly personalized medicine that takes sex into account rather than treating it as an afterthought.
Citation: Sun, R., Deng, Q. & Wang, D. SexTumorDB: a comprehensive resource of sex-dependent tumor landscape at single-cell resolution. Sci Data 13, 520 (2026). https://doi.org/10.1038/s41597-026-06707-4
Keywords: sex differences in cancer, tumor microenvironment, single-cell RNA sequencing, cancer databases, precision oncology