Clear Sky Science · en
A multi-level annotated sensor dataset of gait freezing manifestations and severity in Parkinson’s disease
Why Stopping Mid-Step Matters
For many people with Parkinson’s disease, walking is not just slower or shakier—it can suddenly stop. In an instant, their feet feel glued to the floor, even though they are desperately trying to move. This frightening event, called freezing of gait, is a leading cause of falls, injuries, and loss of independence. The paper behind this summary introduces FoG-STAR, a rich new dataset built from wearable sensors that track how people with Parkinson’s move during everyday actions. By sharing these data openly with scientists worldwide, the authors hope to speed up the development of smarter devices and algorithms that can detect, measure, and eventually help prevent these dangerous freezing episodes.
Watching Movement with Discreet Wearable Sensors
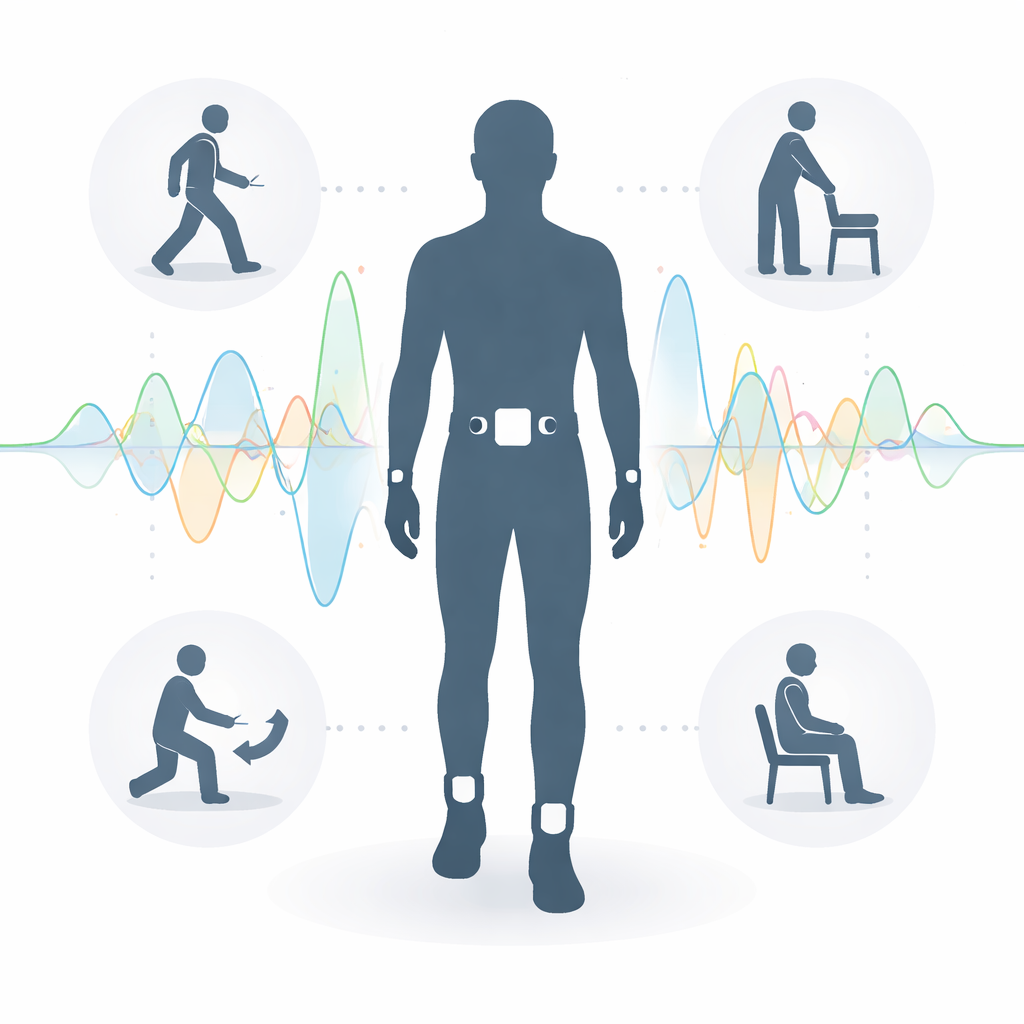
Instead of relying only on a doctor’s brief observation in the clinic, the FoG-STAR project uses four small motion sensors to follow how the body moves step by step. Twenty-two volunteers with Parkinson’s wore sensors on both ankles, on one wrist, and on the lower back, roughly where the body’s center of mass sits. Each device recorded how fast different parts of the body moved and rotated, hundreds of times per second, while participants performed common movements such as standing up, sitting down, walking ten meters, turning in place, or passing through a doorway. All sessions were recorded while the participants were in an “off-medicine” state so that freezing events would be more likely to appear. At the same time, video cameras captured every action, providing a visual reference for what the sensors were picking up.
From Raw Motion to Labeled Freezing Episodes
Collecting the signals is only half the story; the other half is understanding what they mean. Two neurologists, both experts in movement disorders, carefully reviewed the videos frame by frame. They marked when each freezing episode began and ended and described how it looked—whether the person shuffled forward with tiny steps, trembled in place with rapid leg movements, or became completely stuck without moving at all. They also labeled what the person was doing the rest of the time: walking, standing, turning, sitting, or changing posture. These detailed markings were then synchronized with the sensor data, producing a time-aligned record where every instant of motion is paired with what was happening clinically. This multi-layer description makes it possible to study freezing in context rather than as isolated blips.
Building a Resource for Smarter Algorithms
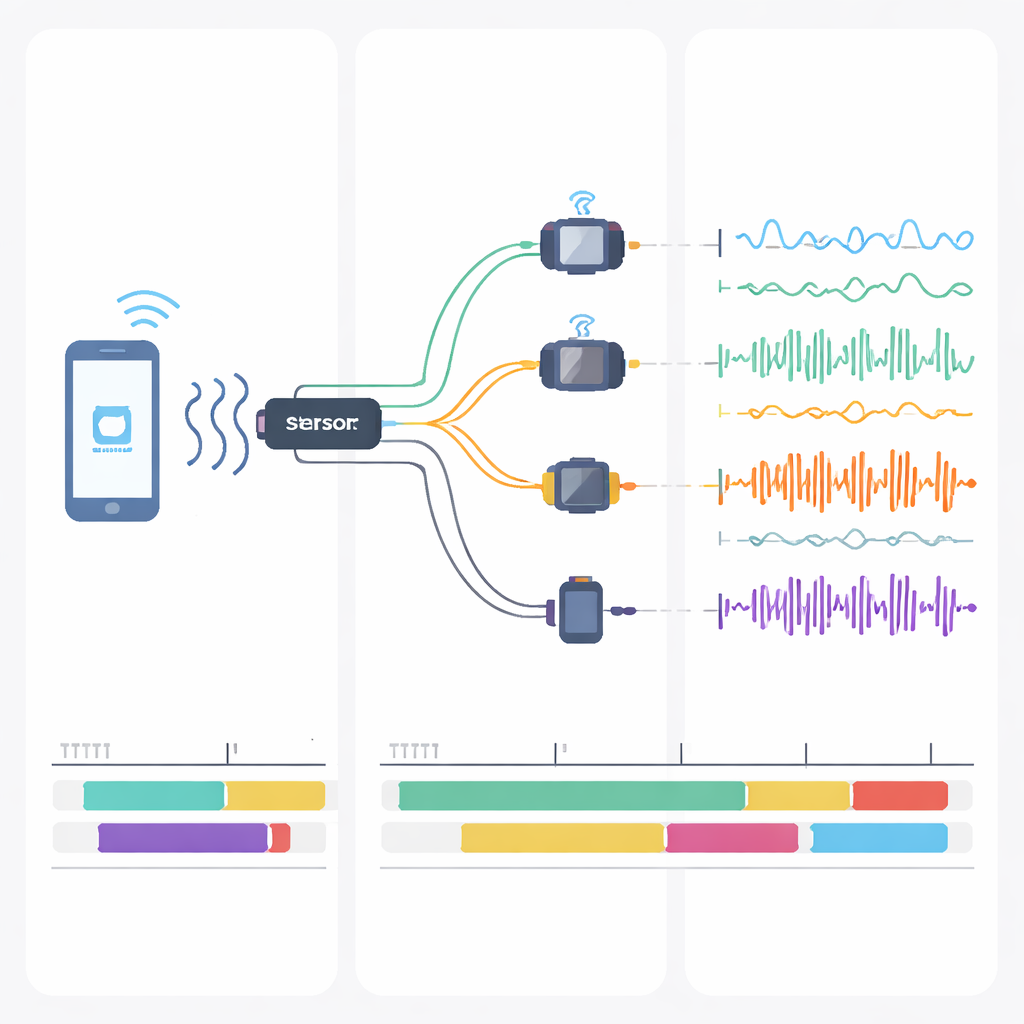
The result is an open, organized collection of 329,000 sensor samples, each linked to a subject, task, activity, and freezing label. A separate file lists each participant’s age, disease stage, movement scores, thinking ability, fear of falling, and quality of life, so researchers can explore how freezing patterns differ across patients. Early tests with machine learning models show that deep learning methods can recognize freezing episodes with high accuracy, especially when using data from ankle sensors. These models can even be trained on FoG-STAR and then adapted to work on other datasets, suggesting that FoG-STAR captures key features of how freezing appears in motion signals. The authors also describe how they handled technical issues like synchronizing multiple sensors and dealing with occasional gaps in data, giving others a roadmap for similar studies.
Limits, Caveats, and Real-World Use
Like any scientific resource, FoG-STAR has limits. The study includes only 22 people, all tested in a carefully controlled setting and all off their usual medication, so the data may not reflect the full variety of freezing seen at home or in milder disease stages. Not every participant completed every task, and the videos were reduced to ten frames per second, which means extremely brief freezing events may not be captured precisely. Still, the dataset covers a wide mix of walking patterns, turns, and posture changes, and it keeps small gaps and imperfections in the signals visible rather than smoothing them away, so researchers can decide how best to clean and interpret the data for their own purposes.
What This Means for People Living with Parkinson’s
In everyday terms, FoG-STAR is like handing the research community a detailed, time-stamped diary of how freezing of gait actually unfolds in the body, written not in words but in movement. By making this diary open and well documented, the authors give engineers, clinicians, and data scientists a common starting point for comparing new ideas and tools. Over time, such work could lead to wearable devices that warn people just before they freeze, adjust treatments to reduce freezing, or guide home-based rehabilitation exercises tailored to a person’s specific movement patterns. While FoG-STAR does not cure Parkinson’s or freezing of gait on its own, it lays crucial groundwork for technologies that might one day help people walk more safely and confidently.
Citation: Borzì, L., Demrozi, F., Bacchin, R.A. et al. A multi-level annotated sensor dataset of gait freezing manifestations and severity in Parkinson’s disease. Sci Data 13, 305 (2026). https://doi.org/10.1038/s41597-026-06645-1
Keywords: Parkinson’s disease, freezing of gait, wearable sensors, gait analysis, deep learning