Clear Sky Science · en
Mass azithromycin distribution and antibiotic resistance in the gut and nasopharynx: a cluster-randomized trial
Why giving one pill to many kids matters
In parts of West Africa, a single antibiotic, azithromycin, has been used in mass campaigns to cut the number of young children dying from infections. The strategy works—but it raises a serious worry: are we quietly breeding tougher, drug-resistant germs in children’s bodies? This study, carried out in hundreds of villages in Niger, takes a close look inside children’s guts and noses to see how repeated community-wide treatments reshape their hidden microbial world and resistance to antibiotics.
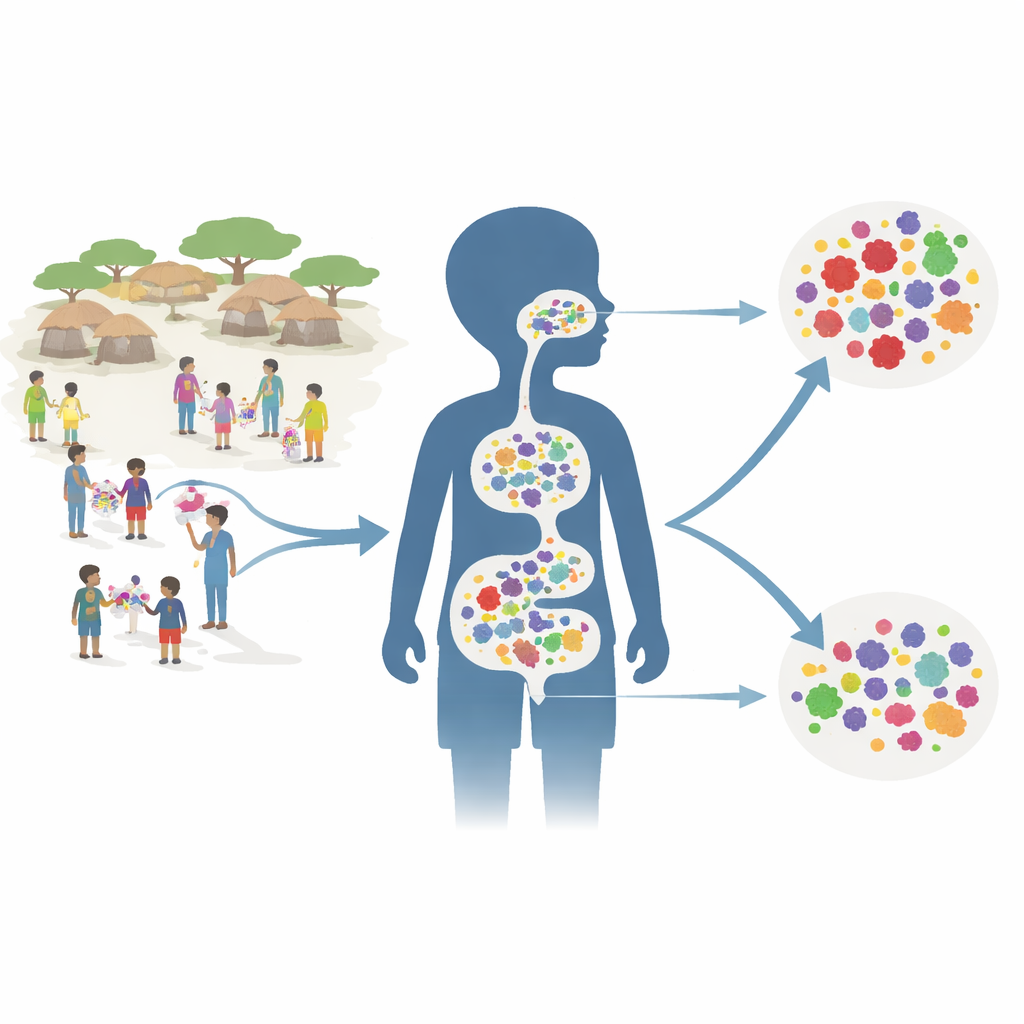
Testing a community-wide medicine plan
Researchers embedded their work within a huge trial called AVENIR, which had already shown that giving azithromycin every six months to all children aged 1 to 59 months could lower deaths in this age group. For the resistance study, they focused on 150 randomly chosen villages. Each village belonged to one of three groups: all young children received azithromycin; only infants up to 11 months received azithromycin while older toddlers and preschoolers received placebo; or all children received placebo. Two years into the program—six months after the fourth round of treatment—the team collected rectal and deep nasal swabs from about 30 children per village.
Peering into the gut and nose
Instead of growing germs in the lab, the scientists pooled the samples from each village and used modern DNA sequencing. This allowed them to catalog which bacteria were present and count genetic markers that signal resistance to different families of antibiotics. They paid special attention to macrolides—the drug family that includes azithromycin—while also scanning for resistance to many other widely used antibiotic types, such as penicillin-like drugs. The gut and the nasopharynx (the upper part of the throat behind the nose) were examined because both are major reservoirs where resistance genes can accumulate and potentially spread.
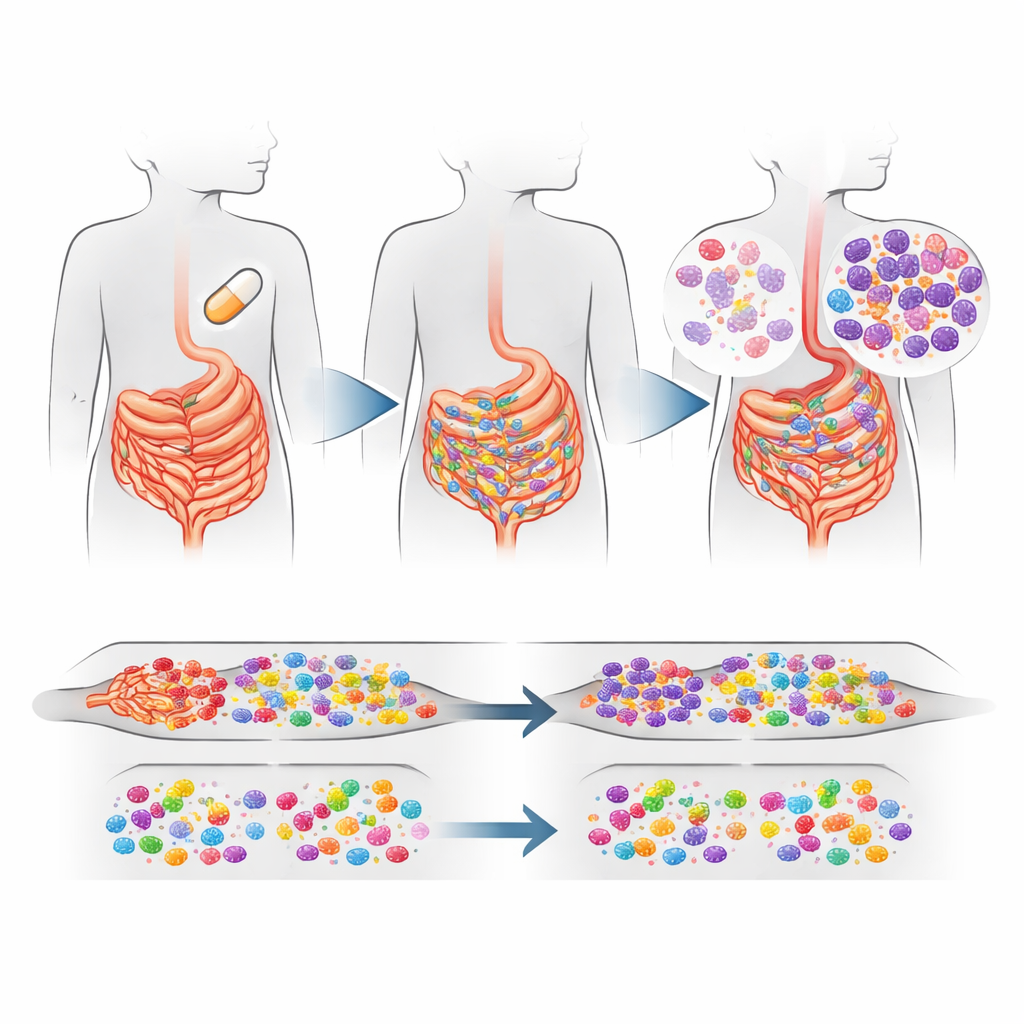
What changed inside children’s guts
The clearest signal came from the gut. Villages where all children received azithromycin had a modest but statistically reliable increase—about 16% higher overall—of macrolide resistance genes in gut bacteria compared with placebo villages. The rise was driven largely by one resistance gene, called ermF, which helps protect bacteria against macrolide drugs. This gene is often carried by common gut bacteria such as Bacteroides and Prevotella, which usually live harmlessly in the intestines but can sometimes cause disease. Interestingly, resistance genes against other major antibiotic families did not increase, and the overall mix and diversity of gut bacteria looked broadly similar between treatment groups, even though some specific species became more or less common.
What stayed the same in the nose
In contrast, the nasal passages told a quieter story. The study did not find clear, statistically firm differences in macrolide resistance genes between treatment groups in the nasopharynx, nor evidence that resistance to other antibiotic classes was being selected there. The typical nasal residents—genera such as Moraxella, Haemophilus and Streptococcus—remained dominant. A few mouth-related bacteria linked to gum disease became more common in azithromycin-treated communities, and some of these can also carry resistance genes, but the overall resistance burden in the nose did not shift in the same way as in the gut.
Balancing today’s gains with tomorrow’s risks
Taken together, the findings show that giving azithromycin to all young children in a community can save lives, but it also nudges gut bacteria toward greater resistance to this drug family, mainly through expansion of specific resistance genes like ermF. The study did not see a spillover into resistance against other antibiotic types over the two-year window, nor strong changes in the nasal reservoir, but the authors warn that resistant gut bacteria and their genes can spread over time and between people. They argue that any broad antibiotic program for childhood survival should build in careful, long-term resistance tracking so that health officials can keep weighing the immediate benefit of fewer child deaths against the slower, less visible cost of strengthening drug-resistant microbes.
Citation: Doan, T., Yan, D., Arzika, A.M. et al. Mass azithromycin distribution and antibiotic resistance in the gut and nasopharynx: a cluster-randomized trial. Nat Med 32, 859–868 (2026). https://doi.org/10.1038/s41591-026-04217-9
Keywords: azithromycin, childhood mortality, antibiotic resistance, gut microbiome, mass drug administration