Clear Sky Science · en
Implementation and evaluation of the Y-Check comprehensive adolescent health check-up intervention in Zimbabwe: a pre−post mixed-methods study
Why Teen Health Check-Ups Matter
Across the world, teenagers are living through huge physical, emotional and social changes, yet many rarely see a health worker unless they are seriously ill. This study, carried out in the city of Chitungwiza in Zimbabwe, tested a new idea: offering a one-stop health check-up designed just for adolescents, in schools and community centers. The goal was simple but ambitious—to quietly catch hidden problems, offer help on the spot, and guide young people to services that could protect their health, schooling and futures.
A New Kind of Health Visit for Young People
The program, called Y-Check, was developed by Zimbabwean researchers working with the World Health Organization. Instead of focusing on just one issue, such as eyesight or vaccines, Y-Check brought together 25 different checks and supports in a single visit. Adolescents aged 10–19 came either from primary and secondary schools or from nearby community venues. During the visit, non-clinical staff helped them register, collect a urine sample, and complete a private digital questionnaire on a tablet. This asked about their home life, mood, sleep, physical activity, substance use, sexual health and more. Simple physical measurements and lab tests followed, including height and weight, blood pressure, vision and hearing tests, dental checks and screening for anemia and some infections. 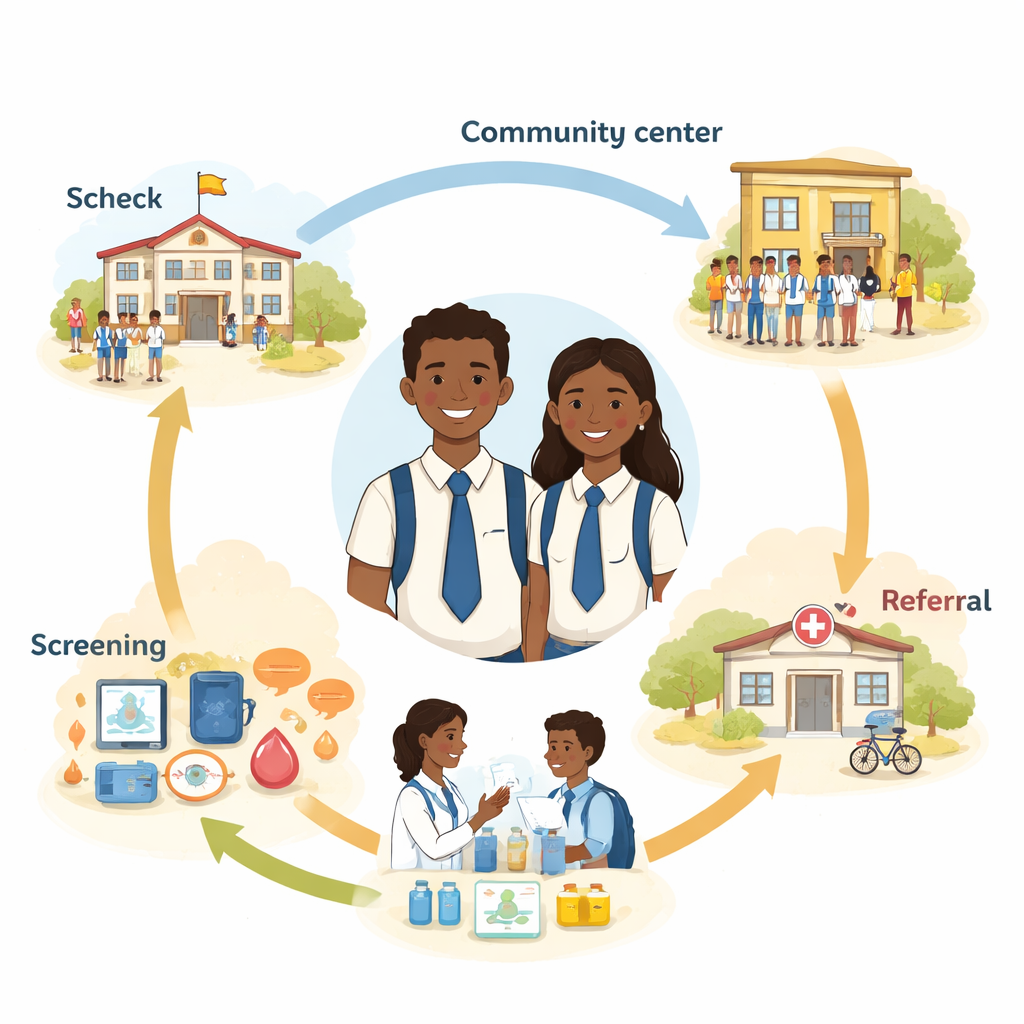
From Hidden Problems to Real Help
Behind the scenes, a custom-made app turned each young person’s answers and test results into color-coded ‘warning flags’ that a nurse reviewed. The nurse then decided whether the adolescent simply needed information and reassurance, on-the-spot treatment, or a referral to another service such as a mental health counselor, dentist or HIV clinic. Of the 2,094 adolescents who attended, nearly 9 in 10 had at least one previously untreated condition or risky behavior, ranging from psychosocial problems to high blood pressure, anemia and poor oral health. About 30% needed referral beyond what could be done immediately. Overall, 70.8% of those with an identified issue had received appropriate care or completed their referrals by the follow-up visit about six months later, and for issues that could be managed entirely on-site, success rates topped 90%.
Changes in Health, Habits and School Life
To see whether the check-ups did more than just label problems, the team invited adolescents back several months later for a follow-up survey and tests. Among those who had been underweight or anemic, thinness decreased in both age groups and anemia fell in older teens. Many who had infections or mental health difficulties at the first visit showed clear improvement by the second. Self-esteem scores rose, health-related quality of life nudged upward, and more young people reported brushing their teeth, eating fruit and being physically active. School life shifted too: younger adolescents missed fewer days of school because of illness or menstruation, and students in all age and sex groups were less likely to say that poor health was holding back their performance or participation in class.
What Worked Well—and What Was Hard
Most participants—84%—said they were very satisfied with the check-ups. They valued being listened to, getting free care and learning whether they were healthy. The digital questionnaire felt confidential and made it easier to talk about sensitive topics, though some younger pupils needed help. The study also highlighted real-world obstacles. Setting up reliable referral pathways was difficult, especially for mental health, dental problems and nutrition, where public services were limited or carried user fees. Some parents worried about blood and urine tests, or about discovering conditions they could not afford to treat. Older adolescents preferred community venues over school-based visits for privacy. The program was not cheap: excluding initial design costs, screening and caring for each adolescent cost about US$47, a significant share in a country with low per-person health spending. 
What This Means for the Future
For a lay reader, the main message is clear: many teenagers carry untreated health problems that quietly sap their well-being and school success, but a thoughtfully designed check-up can find them and make a difference. In this study, a single comprehensive visit, backed by digital tools and youth-friendly staff, improved a wide range of health, emotional and educational measures in a challenging, low-resource setting. The authors argue that if programs like Y-Check can be made more affordable and better linked to everyday health services, they could become a routine part of growing up—helping adolescents stay healthier now and laying the groundwork for stronger, more productive adults later in life.
Citation: Doyle, A.M., Nzvere, F., Manyau, S. et al. Implementation and evaluation of the Y-Check comprehensive adolescent health check-up intervention in Zimbabwe: a pre−post mixed-methods study. Nat Med 32, 494–504 (2026). https://doi.org/10.1038/s41591-025-04156-x
Keywords: adolescent health, school health programs, screening check-ups, Zimbabwe, mental health