Clear Sky Science · en
Circulating metabolites, genetics and lifestyle factors in relation to future risk of type 2 diabetes
Why your blood’s tiny molecules matter
Type 2 diabetes is often described in terms of sugar, insulin and weight. But beneath those familiar ideas lies a bustling world of hundreds of tiny molecules circulating in our blood. This study, involving more than 23,000 people followed for up to 26 years, shows that patterns of these molecules can reveal who is more likely to develop type 2 diabetes long before symptoms appear—and how genes and everyday habits like diet and exercise shape that risk.
Looking inside the body’s chemical fingerprint
Our blood carries a rich mixture of small molecules—fats, amino acids, sugars and byproducts of food and gut microbes—that together form a kind of chemical fingerprint, or metabolome. The researchers measured 469 such molecules in participants who did not yet have diabetes, then tracked who developed the disease over time. They found that levels of 235 molecules were linked to later type 2 diabetes, including 67 that had not been clearly tied to the disease before. Some fats that store or move energy, such as certain triacylglycerols and ceramides, were associated with higher risk, while other fats, like specific cholesterol esters and antioxidant-like “plasmalogens,” were linked to lower risk. Several amino acids and bile acids, as well as molecules related to coffee and gut microbe activity, also stood out.
How genes and organs help shape diabetes risk
To understand why these molecules matter, the team combined metabolite data with large-scale genetic studies. They asked which genetic variants influence the levels of diabetes-related metabolites, and whether those variants also affect diabetes itself or key traits such as insulin resistance, liver fat and blood lipids. Many of the same gene regions controlled both the metabolites and diabetes-related traits, suggesting shared biological pathways. Signals pointed strongly to organs central to metabolism, including liver, pancreas, fat tissue, thyroid and parts of the digestive tract. In other words, the blood chemistry profile appears to mirror subtle changes across several organ systems long before a person meets the diagnostic threshold for diabetes.
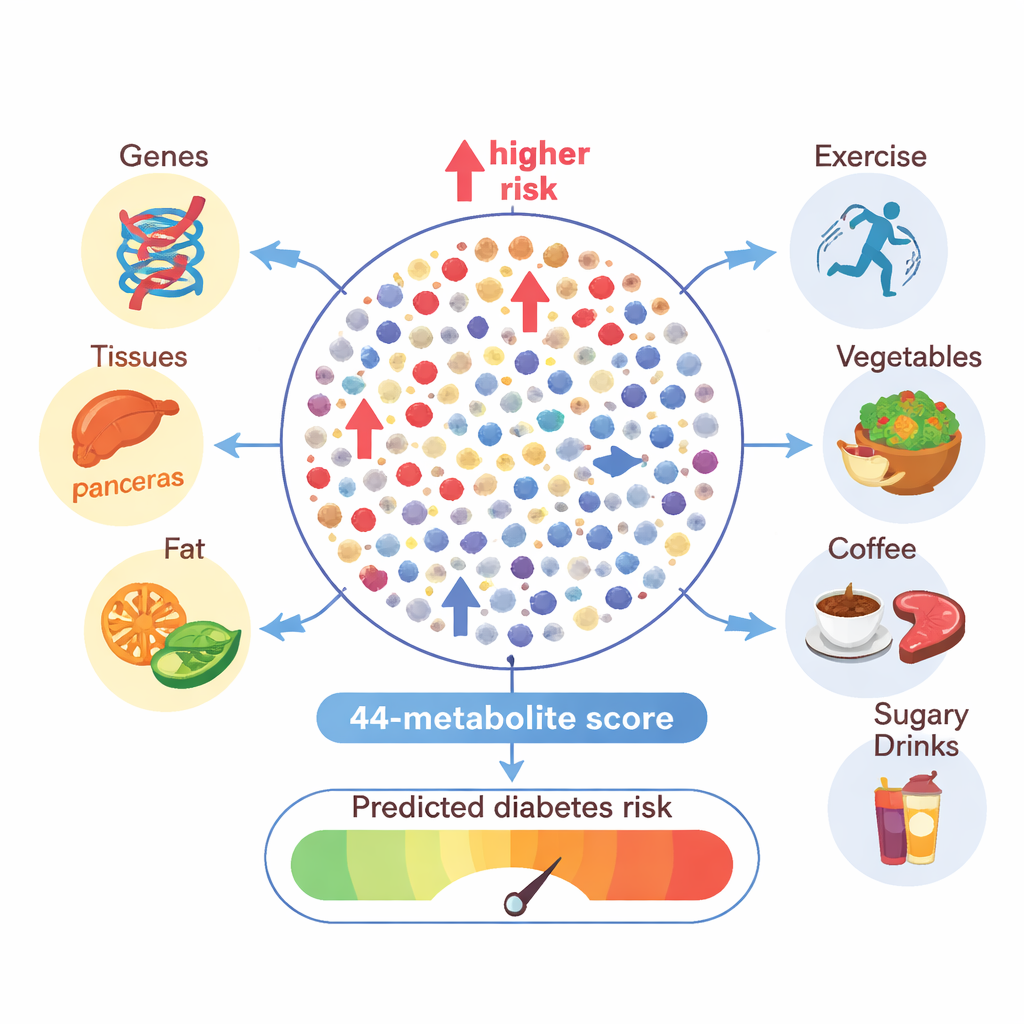
What lifestyle has to do with these hidden signals
Genes are only part of the story. The researchers also examined how body weight, physical activity and diet relate to the metabolite patterns tied to diabetes. Obesity explained more variation in diabetes-linked molecules than in other molecules, especially certain blood fats and amino acids, echoing its central role in the disease. People who were more physically active, or who consumed more vegetables, whole grains and coffee or tea, tended to have more favorable metabolite profiles—those associated with lower diabetes risk. In contrast, higher intakes of red meat and sugary drinks were linked to metabolite patterns pointing toward greater risk. Statistical analyses suggested that many of these molecules may act as messengers, partly explaining how lifestyle choices translate into changes in diabetes risk.
A 44-molecule score that flags future diabetes
Building on these insights, the team used machine learning to assemble a “metabolomic signature” of 44 key molecules that together captured much of the complexity of diabetes-related metabolism. When they tested this score in multiple independent groups, people in the highest tenth of the score had about five times the risk of developing type 2 diabetes compared with those in the lowest tenth. The score predicted future disease better than standard risk factors alone, such as age, weight, blood pressure and family history, and in many cases added useful information even beyond fasting blood sugar. The same score also tracked with lifestyle: higher body mass index and greater consumption of red meat and sugary drinks pushed the score upward, whereas more exercise and higher intakes of whole grains, coffee or tea and moderate wine pulled it down.
What this means for prevention and early action
For a layperson, the main message is that type 2 diabetes is not just about one number like blood sugar—it reflects a broad, interconnected shift in the body’s chemistry that is influenced by both genes and everyday choices. By identifying a large set of blood molecules linked to diabetes, and combining them into a practical 44-molecule score, this study moves us closer to personalized prevention: spotting high-risk individuals years in advance and monitoring how changes in diet, activity and weight improve their underlying metabolic health. While clinical use will require further testing and cost reductions, these findings highlight that small, invisible molecules in our blood can provide early warning—and a chance to act before diabetes takes hold.
Citation: Li, J., Hu, J., Yun, H. et al. Circulating metabolites, genetics and lifestyle factors in relation to future risk of type 2 diabetes. Nat Med 32, 660–670 (2026). https://doi.org/10.1038/s41591-025-04105-8
Keywords: type 2 diabetes, metabolomics, precision prevention, diet and lifestyle, genetic risk