Clear Sky Science · en
Clinical genetic variation across Hispanic populations in the Mexican Biobank
Why Genes and Geography Matter for Your Health
When doctors order genetic tests, they often lump millions of people into broad labels like “Hispanic” or “Latino.” This study shows why that shortcut can be risky. By closely examining DNA from more than 6,000 people across all 32 states of Mexico, researchers found that important health-related gene variants vary sharply from region to region. These differences can change how well drugs work, how safe they are, and who should get early screening for certain diseases—meaning that a person’s specific regional and Indigenous roots can matter just as much as any broad ethnic label.
A Nationwide Look Inside Mexican DNA
The team used the Mexican Biobank, a large collection of genetic data from 6,011 adults sampled in 898 locations, from northern deserts to the Yucatán Peninsula. Each participant was genotyped for about 1.8 million DNA markers, many of them already known to influence disease risk or drug response. Instead of treating all Mexican or Hispanic individuals as one group, the researchers measured the mix of Indigenous American, European, and African ancestry in each person, and then asked how often medically important variants appeared in each state. They found clear regional patterns that mirror Mexico’s history: southern states like Oaxaca and Chiapas carry more Indigenous ancestry on average, while northern states have a stronger European contribution.
Hidden Patterns in Drug Response Genes
When the researchers zoomed in on genes that affect how people process medications—especially painkillers and cholesterol-lowering drugs—they uncovered striking gradients across Mexico. One variant in the CYP3A4 gene, linked to fentanyl metabolism, was far more common in people with higher Indigenous ancestry and became more frequent moving from north to south. This variant tends to slow fentanyl breakdown, meaning that standard doses could be too strong for some carriers. Another variant in the SLCO1B1 gene, which controls how the body handles certain statins, was overall more common in DNA segments of European origin, but showed sharp regional jumps within the Indigenous ancestry component—reaching much higher levels in the Mayan region of Yucatán than in northern states. In some cases, the differences within Indigenous Mexican ancestry were even larger than those between entire continents such as Europe and East Asia.
Indigenous Roots and Treatable Genetic Diseases
The study did not stop at drug responses. It also examined rare but serious disease variants that professional societies consider “actionable” because early detection can change medical care. One powerful example is a harmful change in the BTD gene, which causes biotinidase deficiency—a condition that can lead to permanent neurological damage but is easily treated with vitamin supplements if caught early. This variant appeared almost exclusively in people with Indigenous ancestry from the Yucatán Peninsula, suggesting a strong Mayan origin. Its localized frequency was much higher than in Mexico City. These findings show that newborn screening and carrier testing strategies could be fine-tuned to focus more intensely on regions where certain treatable conditions are genuinely more common.
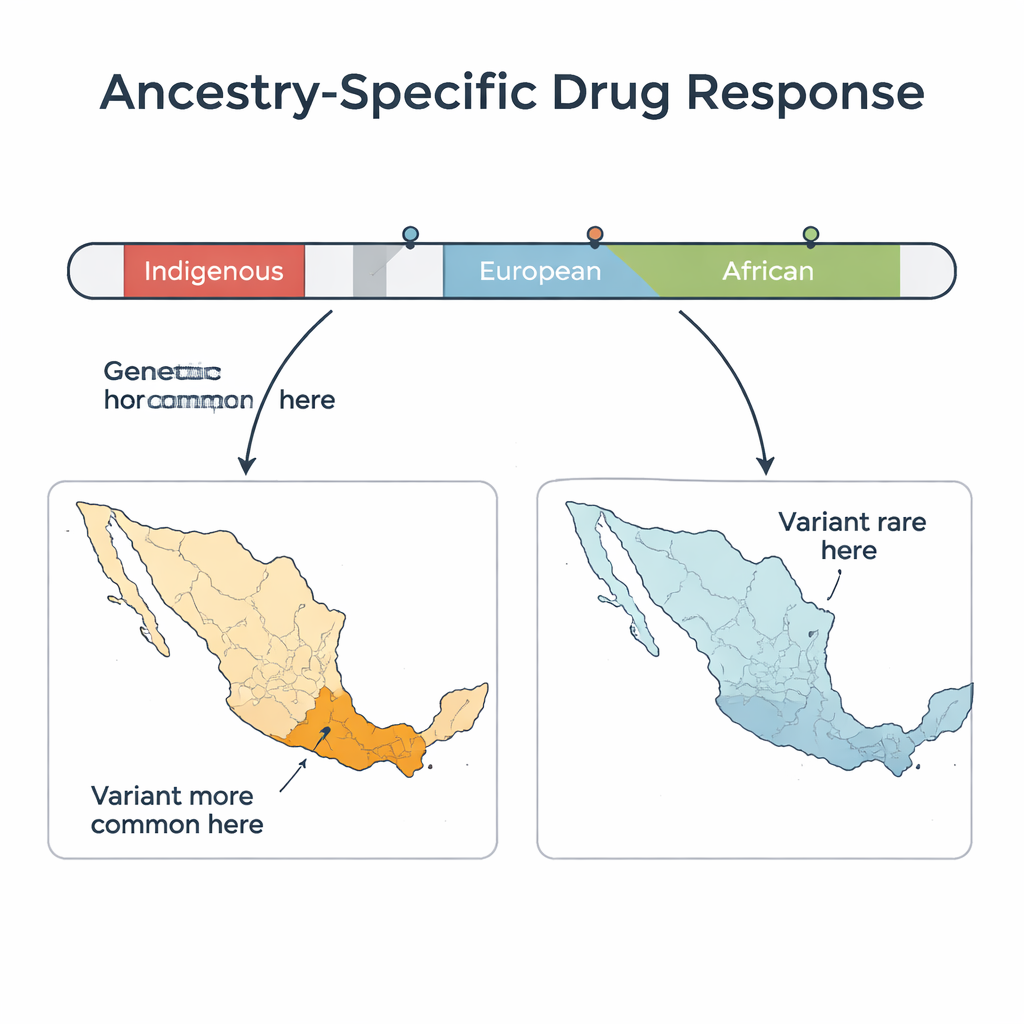
From Big Labels to Fine-Grained Precision Medicine
To help doctors and researchers use these insights, the team built MexVar, an interactive online platform that lets users look up how common a particular health-related variant is in each Mexican state and within each ancestry component. Analyses of more than 42,000 clinically relevant variants revealed that about 60% of their frequency differences are tied to ancestry, with many others shaped by geography that reflects deep, pre-Columbian population structure. The authors argue that relying on broad terms like “Hispanic” or “Latino” hides this crucial diversity and can mislead testing and treatment decisions. Instead, precision medicine in the Americas should recognize that a patient from Chiapas, one from Sonora, and one from Yucatán may all identify as Mexican or Latino, yet carry very different genetic profiles that matter for drug dosing, disease risk, and preventive care.
What This Means for Patients and Doctors
For non-specialists, the central message is simple: where your ancestors came from within a country like Mexico can strongly influence how your body handles medications and your chances of certain inherited conditions. The study shows that many clinical guidelines, built mostly on European data and broad ethnic labels, may miss important risks or benefits for people of Mexican and broader Latin American descent. Tools like the Mexican Biobank and the MexVar platform move medicine toward a future where genetic testing and treatments are tailored not just to a generic category, but to the true diversity of ancestry and geography—helping make care safer, more effective, and more equitable.
Citation: Barberena-Jonas, C., Medina-Muñoz, S.G., Cedillo-Castelán, V. et al. Clinical genetic variation across Hispanic populations in the Mexican Biobank. Nat Med 32, 725–735 (2026). https://doi.org/10.1038/s41591-025-04100-z
Keywords: pharmacogenomics, Mexican Biobank, Indigenous ancestry, precision medicine, genetic variation