Clear Sky Science · en
A minimally invasive dried blood spot biomarker test for the detection of Alzheimer’s disease pathology
A Finger-Prick Test for Brain Health
Imagine checking for early signs of Alzheimer’s disease with a simple finger-prick at home instead of a spinal tap or a brain scan. This study explores exactly that idea: whether tiny spots of dried blood, collected from a fingertip, can reliably reveal the hidden brain changes that signal Alzheimer’s long before severe memory loss appears.
Why Blood Clues Matter for Alzheimer’s
Alzheimer’s disease starts silently, often years before everyday memory problems become obvious. Today, confirming the disease usually requires expensive brain scans or a spinal fluid test, both of which are available only in specialized clinics. In the last decade, scientists have discovered blood “biomarkers” that mirror what is happening in the brain. One of the most important is a form of the tau protein called p-tau217, which rises when Alzheimer’s-type changes are underway. Two others, GFAP and NfL, reflect damage and stress in brain cells. Standard blood tests already measure these markers well, but they still depend on a needle in the arm, rapid processing, and freezers—steps that limit how widely such tests can be used.
Turning a Drop of Blood into a Lab Sample
The DROP-AD project set out to remove those hurdles by asking a simple question: can a small drop of capillary blood from a finger be dried on special paper cards and later analyzed as accurately as regular venous blood drawn from the arm? Researchers across seven European centers enrolled 337 volunteers, including people with normal thinking, mild memory problems, Alzheimer’s dementia, other forms of dementia, and adults with Down syndrome, who face a very high genetic risk of Alzheimer’s. Using fingertip pricks, staff collected dried plasma spots (for p-tau217 and NfL) and dried blood spots (for GFAP), shipped them at room temperature to a central lab, and compared the results with traditional plasma and spinal fluid tests.
How Well Do the Finger-Prick Results Match?
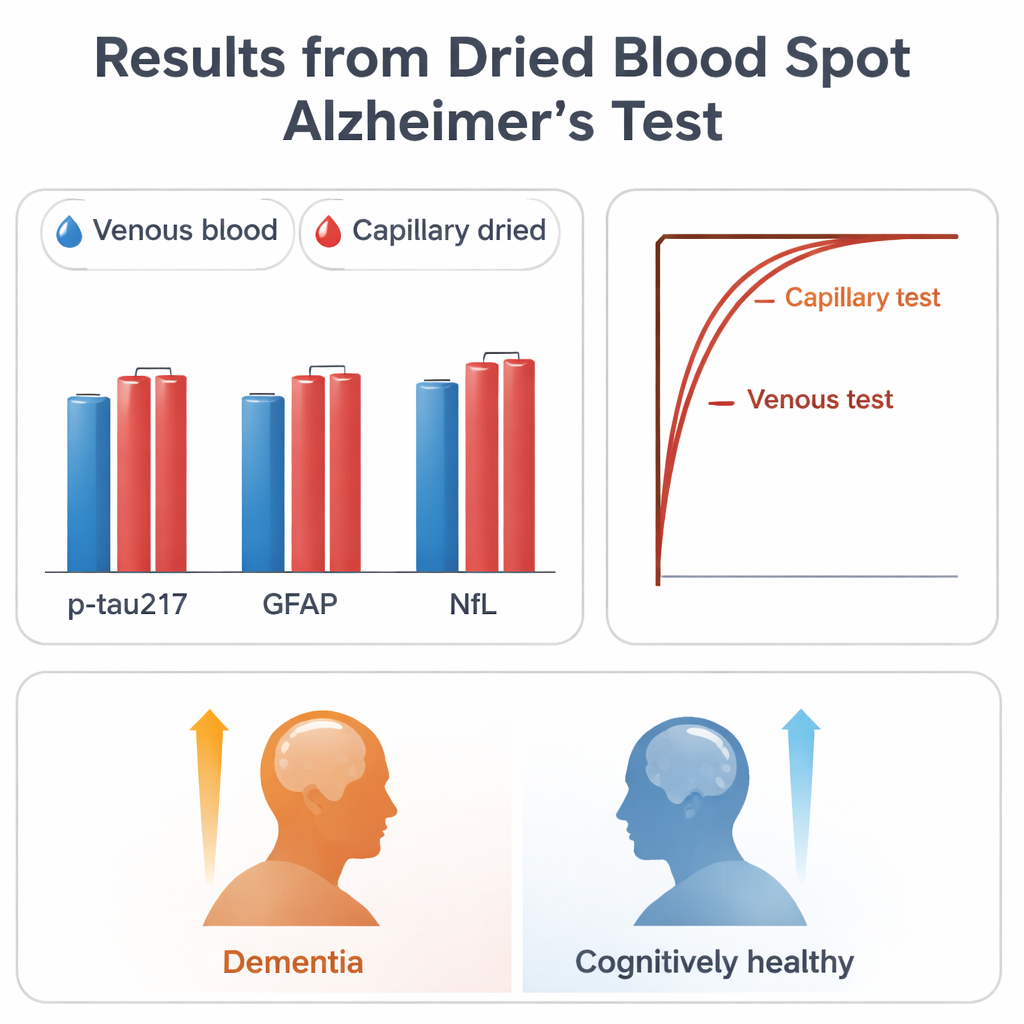
The dried finger-prick samples tracked the conventional tests surprisingly closely. Levels of p-tau217 in dried plasma spots showed a strong correlation with p-tau217 in standard plasma, and they rose stepwise from cognitively unimpaired people to those with mild cognitive impairment and then to those with Alzheimer’s dementia. When the researchers compared dried-blood p-tau217 against spinal fluid markers that define Alzheimer’s, the finger-prick test correctly distinguished people with Alzheimer’s-type changes most of the time. GFAP and NfL from dried samples also lined up well with their venous counterparts and showed expected patterns: higher levels in older individuals and in those with worse scores on a simple thinking test. Although the dried samples gave lower absolute concentrations—partly because the proteins are diluted when eluted from the paper—the relative differences between people and groups remained meaningful.
Reaching People Who Are Often Left Out
The team also tested whether this approach could help groups who are frequently underrepresented in research or for whom standard blood draws are difficult. In adults with Down syndrome, they successfully collected finger-prick samples and found clearly higher p-tau217 and GFAP levels in those with dementia compared with those without Alzheimer’s symptoms. In a small pilot, participants even collected some of their own samples after brief training, and their self-collected results closely matched those collected by professionals. These findings hint at a future in which people might contribute to Alzheimer’s research—or be screened for risk—without traveling to specialized centers.
What This Means for Patients and Families
For now, the authors caution that dried blood spot testing is not ready to guide individual medical decisions, because it is still somewhat less accurate than traditional blood and spinal fluid tests. But the study shows that a simple finger-prick can carry a great deal of information about brain health. With further refinement, such tests could make large-scale Alzheimer’s screening and monitoring more practical, cheaper, and more inclusive—opening the door to earlier diagnosis, timely treatment, and better representation of diverse communities in research.
Citation: Huber, H., Montoliu-Gaya, L., Brum, W.S. et al. A minimally invasive dried blood spot biomarker test for the detection of Alzheimer’s disease pathology. Nat Med 32, 599–608 (2026). https://doi.org/10.1038/s41591-025-04080-0
Keywords: Alzheimer’s disease, blood biomarkers, dried blood spot, early detection, Down syndrome