Clear Sky Science · en
Tirzepatide on obstructive sleep apnea-related cardiometabolic risk: secondary outcomes of the SURMOUNT-OSA randomized trial
Why this matters for people who snore
If you or someone you love snores loudly, wakes up gasping, or feels exhausted despite a full night in bed, obstructive sleep apnea may be to blame. This common condition is tightly linked to excess weight and raises the risk of heart disease, diabetes, and stroke. Researchers recently tested whether a powerful new weight‑loss medicine, tirzepatide, could not only ease sleep apnea but also improve the broader "heart and metabolism" risks that come with it.
A problem that goes beyond snoring
Obstructive sleep apnea happens when the throat repeatedly closes during sleep, cutting off airflow and oxygen. These nightly choking episodes strain the heart, drive up blood pressure, worsen blood sugar control, and disturb cholesterol and fat levels in the blood. The standard treatment, a bedside machine called CPAP that blows air through a mask, can keep the airway open but is often uncomfortable and does not reliably improve long‑term heart outcomes. Because obesity is a major cause of sleep apnea, scientists have wondered whether tackling weight directly—rather than just splinting the airway open—might deliver more complete health benefits.
A large, year‑long clinical test
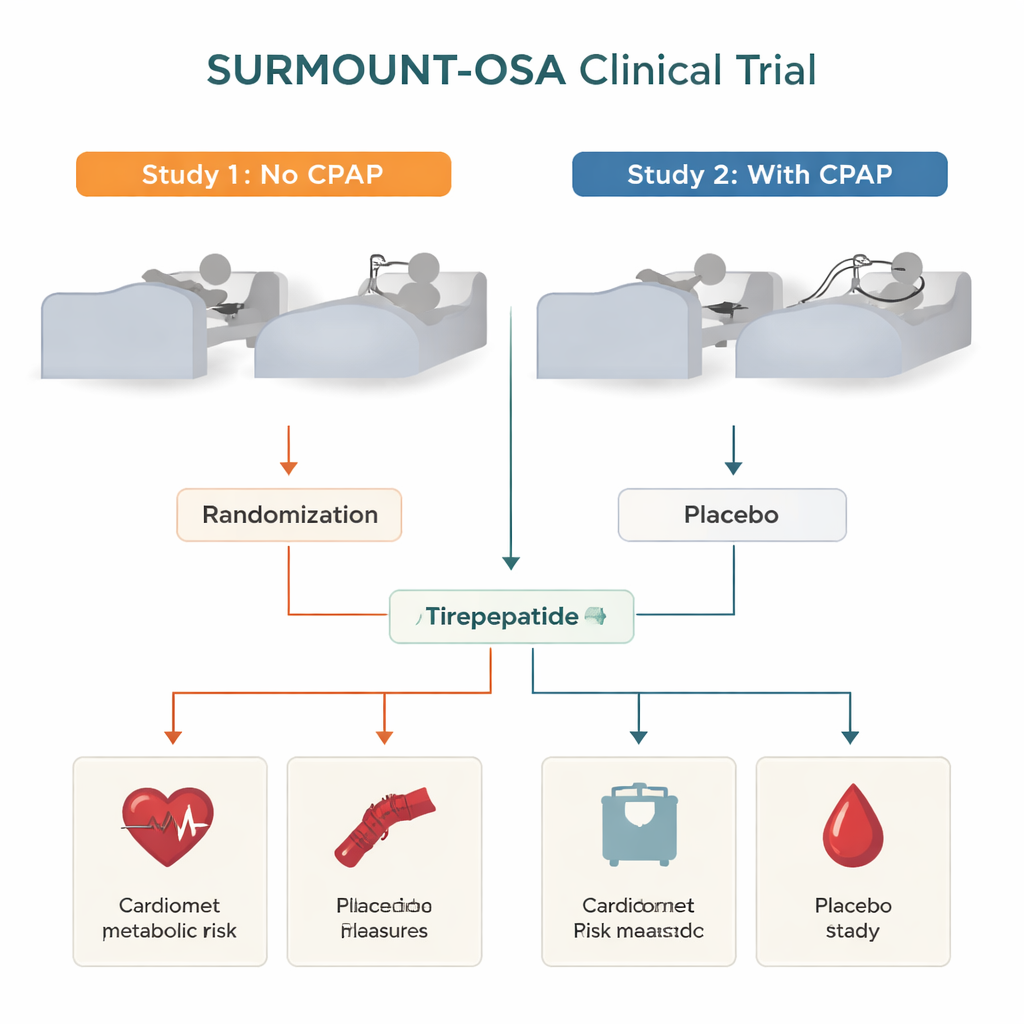
The SURMOUNT‑OSA program combined two gold‑standard, year‑long clinical trials in nearly 470 adults with moderate‑to‑severe sleep apnea and obesity. One trial enrolled people not using CPAP; the other enrolled people already on CPAP and planning to continue it. In both trials, participants were randomly assigned to weekly injections of tirzepatide, at the highest dose they could tolerate, or to placebo injections that looked the same but contained no active drug. Earlier reports from these studies showed that tirzepatide led to major weight loss and fewer breathing interruptions during sleep. The current analysis focused on a different question: how much did the drug change key measures linked to heart and metabolic disease, and were those changes driven more by losing weight, by improving sleep apnea itself, or by both?
Improvements in blood pressure and blood chemistry
After about a year, people taking tirzepatide had substantially healthier cardiometabolic profiles than those on placebo. Systolic blood pressure—the top number on a blood pressure reading—fell several points more with tirzepatide than with placebo in both trials, while the lower diastolic number improved clearly in one of the two. Markers of inflammation and metabolism also shifted in a favorable direction. A blood test called high‑sensitivity C‑reactive protein, which reflects "hidden" body‑wide inflammation, dropped sharply. Levels of triglycerides and very‑low‑density lipoprotein (fats linked to artery‑clogging plaques) fell by about one‑third, while “good” HDL cholesterol rose and overall non‑HDL cholesterol declined. Fasting insulin levels and a standard index of insulin resistance were cut nearly in half, signaling that the body’s response to insulin became much more efficient.
Untangling weight loss from better sleep
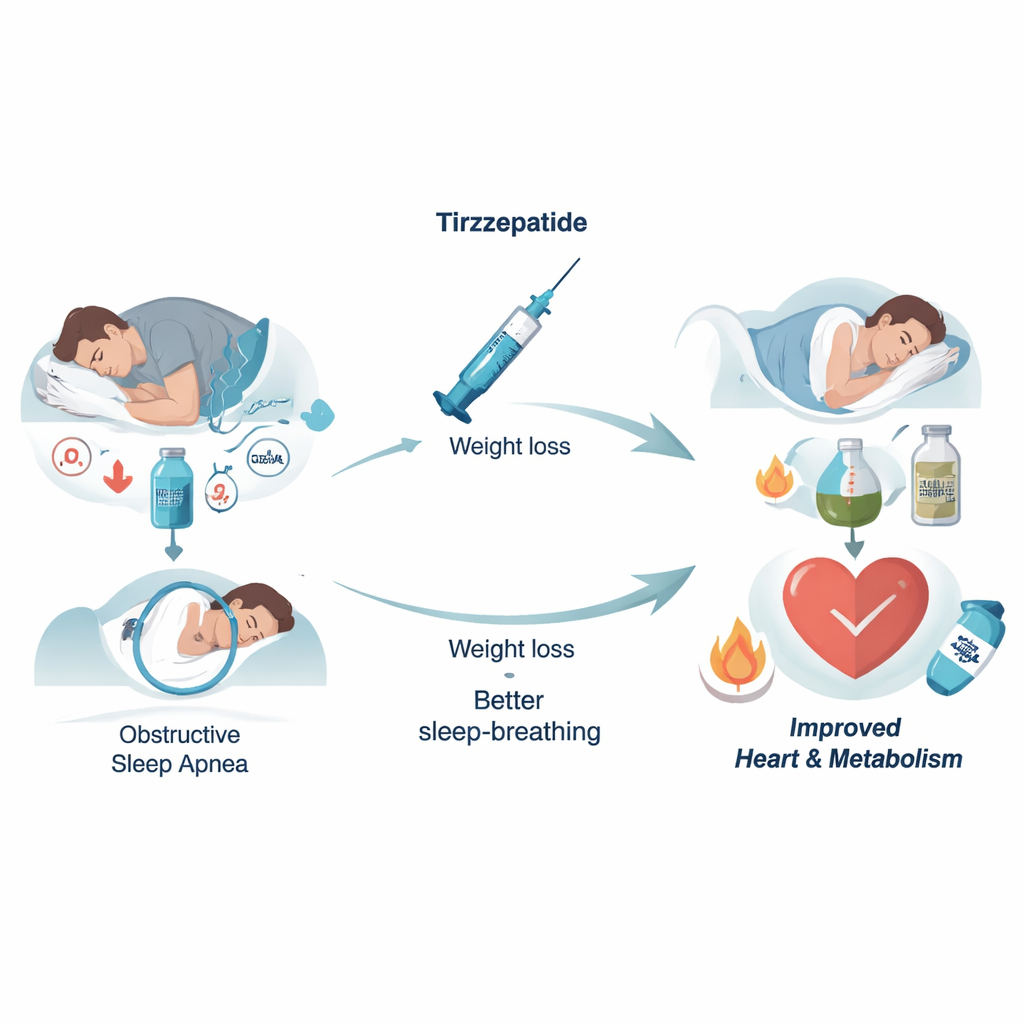
To understand what was driving these benefits, the researchers used a statistical approach called mediation analysis. They asked how much of tirzepatide’s impact on each heart‑risk marker could be explained by three changes: body weight, the number of breathing pauses per hour of sleep, and the total amount of oxygen loss during the night. For blood pressure, weight loss turned out to be the main player—changes in sleep‑breathing measures alone did not significantly explain the improvement. In contrast, for inflammation, insulin resistance, and triglycerides, both pathways mattered: losing weight and easing the oxygen drops of sleep apnea each independently contributed to better results. For one cholesterol measure, the combination of weight loss and improved sleep‑breathing together was important, even when each alone was not clearly enough.
What this means for patients and clinicians
Put simply, in people with moderate‑to‑severe sleep apnea and obesity, tirzepatide did far more than quiet snoring. It lowered blood pressure, reduced harmful blood fats, calmed inflammation, and improved the body’s handling of insulin—changes that, over time, are expected to reduce the risk of heart attacks and strokes. The analysis suggests that the best results come from tackling both problems at once: the extra weight and the breathing disorder it fuels. For many patients, that may mean combining CPAP or other airway treatments with potent weight‑loss medications such as tirzepatide, rather than relying on one or the other alone.
Citation: Malhotra, A., Grunstein, R., Azarbarzin, A. et al. Tirzepatide on obstructive sleep apnea-related cardiometabolic risk: secondary outcomes of the SURMOUNT-OSA randomized trial. Nat Med 32, 653–659 (2026). https://doi.org/10.1038/s41591-025-04071-1
Keywords: obstructive sleep apnea, tirzepatide, obesity, cardiometabolic risk, weight loss treatment