Clear Sky Science · en
Flt3L-mediated tumor cDC1 expansion enhances immunotherapy by priming stem-like CD8+ T cells in lymph nodes
Helping the Immune System Remember How to Fight Cancer
Why do some people’s tumors melt away with modern immunotherapy while others see little benefit? This study looks under the hood of the immune system to answer that question. The researchers show that by boosting a particular group of sentry cells in tumors, they can grow a reservoir of long‑lived, “stem‑like” killer T cells in nearby lymph nodes. Those cells, in turn, make standard checkpoint drugs, especially anti‑CTLA‑4 therapy, work harder and for longer.
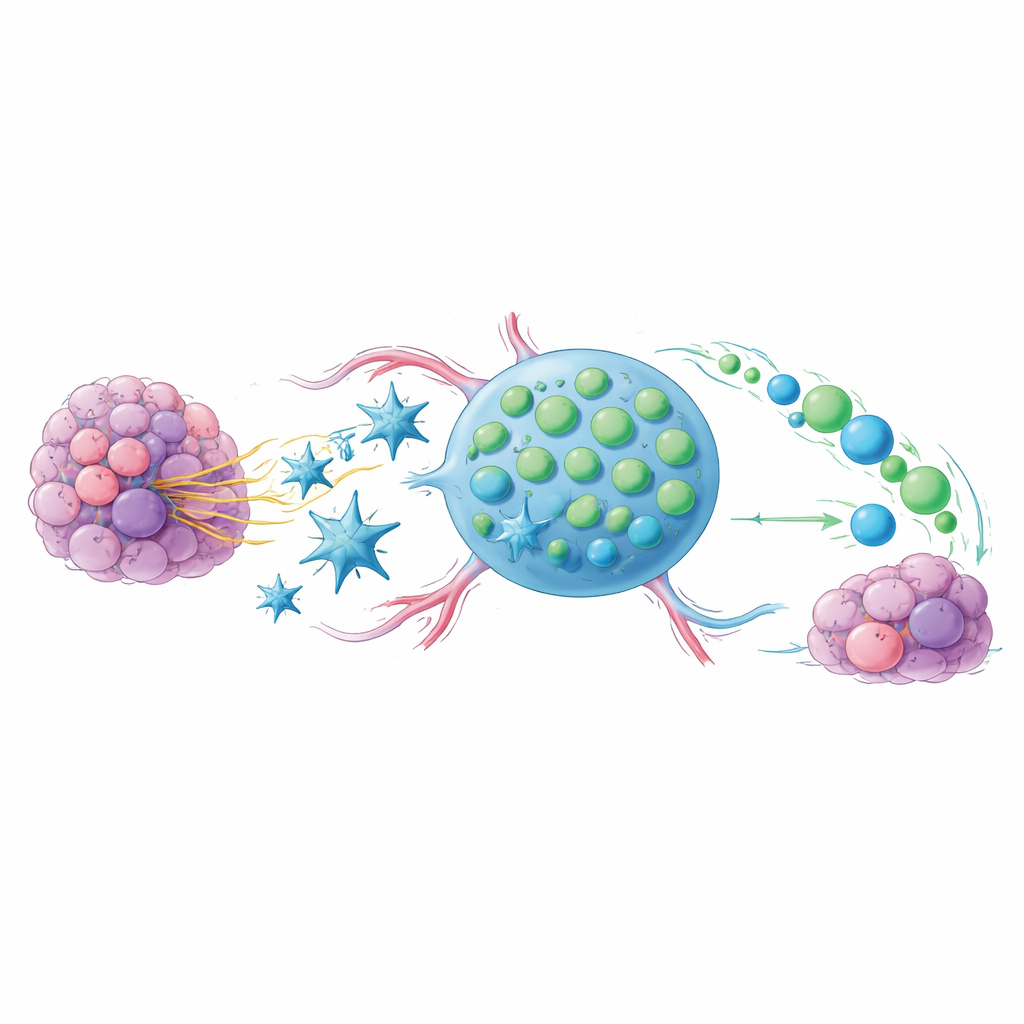
The Problem of Tired Tumor‑Fighting Cells
Checkpoint drugs such as anti‑PD‑1 and anti‑CTLA‑4 unleash immune cells against cancer, but they work well in only a fraction of patients. One clue lies in the state of CD8 T cells, the main assassins of infected or cancerous cells. When these T cells are pushed too hard for too long, they slip into a worn‑out, “exhausted” state and stop multiplying effectively. A smaller subset, however, keeps a more youthful, stem‑like character: they divide readily, spawn fresh fighters and are strongly linked to good responses in people receiving checkpoint therapy. The central question of this work is how to coax tumors and their surroundings to favor these stem‑like cells over their burned‑out cousins.
Supercharging the Tumor’s Sentry Cells
The team focused on conventional type 1 dendritic cells, a rare but powerful class of immune sentries that excel at showing tumor fragments to T cells. They used a growth signal called Flt3 ligand (Flt3L) to expand these cells inside mouse tumors, either by engineering the cancer cells to secrete it or by giving it as a drug. Single‑cell RNA sequencing revealed that Flt3L‑rich tumors contained many more dendritic cells and lymphocytes and fewer tumor cells. Within the dendritic compartment, three distinct groups expanded, including one that was highly mature and primed for travel to lymph nodes, where T cells are first trained. At the same time, CD8 T cells inside these tumors shifted away from a terminally exhausted profile toward a stem‑like or memory‑like state.
Building a Stem‑Like T Cell Reservoir in Lymph Nodes
By tracking tumor‑specific T cells and using genetic tools, the researchers showed that Flt3L treatment boosts a population of CD8 T cells bearing surface markers associated with stem‑like potential and active division. These cells depended on XCR1‑positive dendritic cells and on CCR7‑guided movement of dendritic cells from the tumor to the draining lymph node. When dendritic cells were depleted, or their migration disabled, the stem‑like T cell pool shrank. Blocking lymphocyte exit from lymph nodes had a similar effect, cutting off the supply of renewed T cells to the tumor. Molecular profiling revealed that this process relied on the transcription factor Myb and favored T cells with relatively low‑strength recognition of tumor targets, a type increasingly recognized as important for durable cancer control.
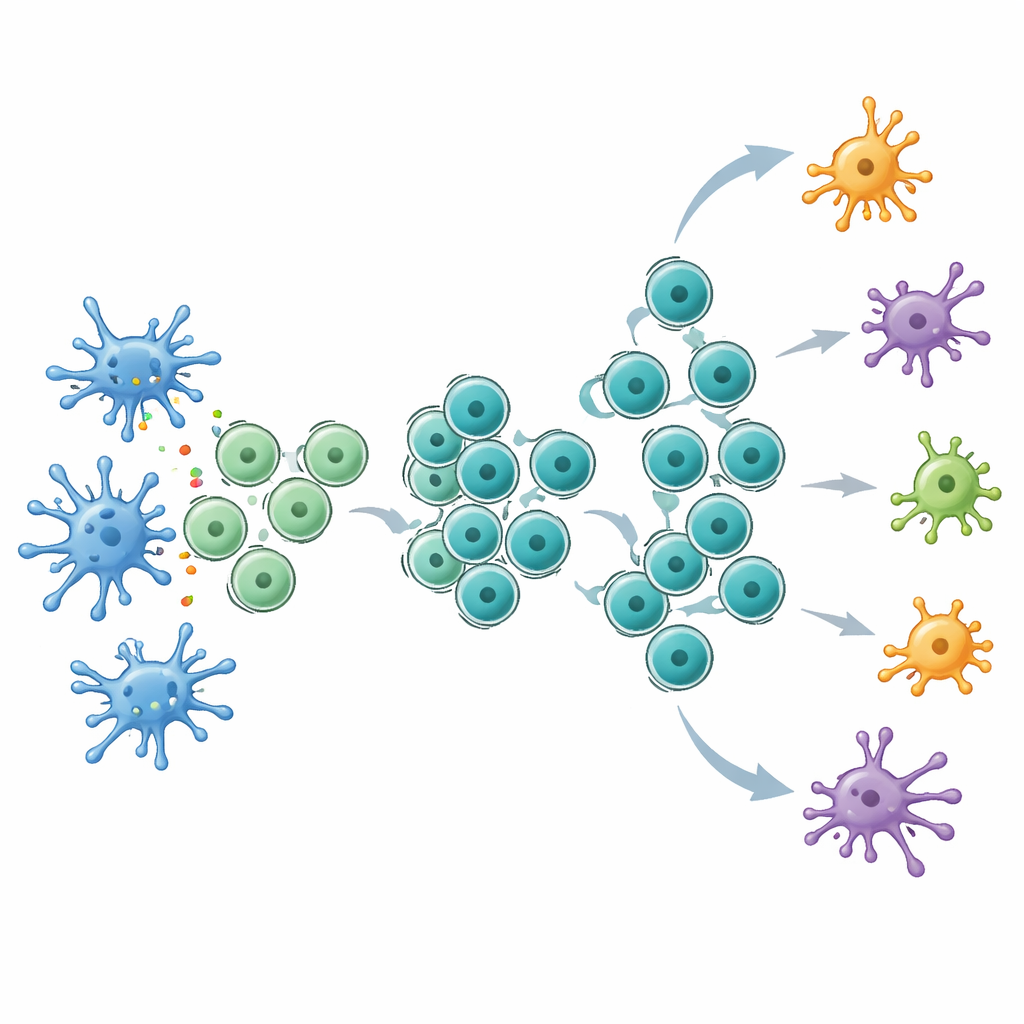
Making Checkpoint Therapy Work Harder
Armed with this expanded reservoir of stem‑like T cells, the mice responded far better to checkpoint blockade, particularly anti‑CTLA‑4 treatment. Tumors in Flt3L‑treated animals shrank more, survival improved and the blood and lymph nodes contained more tumor‑specific T cells. Within tumors, Flt3L increased stem‑like CD8 cells, while subsequent CTLA‑4 blockade appeared to drive these cells to mature into potent effectors that produced high levels of key anti‑tumor molecules. Sequencing of T cell receptors showed that the combination therapy broadened the range of T cell clones that expanded, including many subdominant ones, suggesting a more diverse attack on the cancer. Detailed single‑cell analysis uncovered a unique CD8 T cell cluster, marked by expression of the receptor for the immune messenger IL‑21, that sat midway between stem‑like and exhausted states and shared T cell receptors with both early and late populations. Blocking IL‑21 signaling weakened the benefits of combining Flt3L with anti‑CTLA‑4.
What This Means for Future Cancer Treatments
To a lay reader, the message is that successful immunotherapy depends not just on kicking the immune system harder, but on having the right kind of cells to kick. This work shows that feeding and guiding dendritic cells with Flt3L can stock nearby lymph nodes with a renewable pool of stem‑like killer T cells. When checkpoint drugs such as anti‑CTLA‑4 are then applied, they can draw on this reserve to generate waves of fresh fighters that are more numerous, more diverse and better able to control tumors. Analyses of human cancer datasets suggest that the gene signatures linked to this pathway also predict better outcomes in patients. Together, these findings point toward combination treatments that first build the right immune cell “seed stock” with agents like Flt3L, then unleash it with checkpoint drugs for stronger and more lasting cancer control.
Citation: Lai, J., Chan, C.W., Armitage, J.D. et al. Flt3L-mediated tumor cDC1 expansion enhances immunotherapy by priming stem-like CD8+ T cells in lymph nodes. Nat Immunol 27, 530–542 (2026). https://doi.org/10.1038/s41590-026-02419-4
Keywords: cancer immunotherapy, dendritic cells, stem-like CD8 T cells, checkpoint blockade, Flt3 ligand