Clear Sky Science · en
Structural divergence of lentinula edodes polysaccharides is associated with distinct anti-hyperuricemia pathways
Shiitake Mushrooms and a Growing Health Problem
High uric acid in the blood, known as hyperuricemia, is becoming more common worldwide and is best known for causing painful gout. It is also linked to kidney damage, liver problems, and chronic inflammation. Many current drugs lower uric acid effectively but can trigger serious side effects, so there is strong interest in safer, food‑based options. This study explores whether natural sugars (polysaccharides) from shiitake mushrooms (Lentinula edodes) can help control uric acid and protect organs—and how subtle differences in their molecular structure change the way they work.
Two Cousins in the Mushroom: Similar, Yet Not the Same
The researchers isolated two main polysaccharides from shiitake, named LEP20 and LEP50, using graded ethanol to separate them by size and shape. Detailed chemical tests, including chromatography and nuclear magnetic resonance, showed that both are chains of glucose, but with very different architectures. LEP20 is a (1→3)-β-D-glucan with frequent side branches, forming a more rigid, helical structure often seen in immune‑active mushroom fibers. LEP50 is a (1→4)-α-D-glucan with fewer branches, more like the starch‑type sugars we digest more readily. These structural contrasts—bond direction, branching pattern, and molecular weight—set the stage for the two compounds to act along different biological routes, even though they come from the same mushroom.
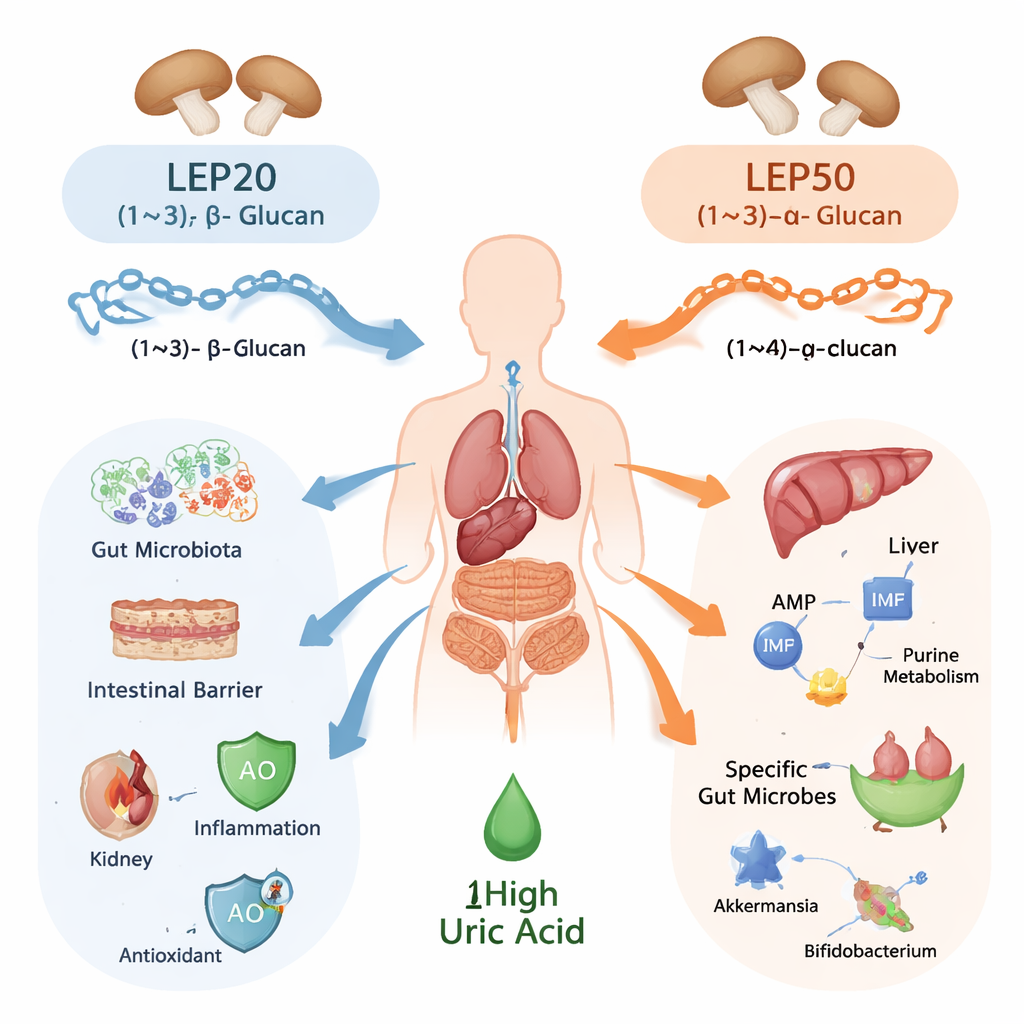
Protecting Kidneys, Liver, and Intestines
To test their effects, the team used rats treated with chemicals to mimic human hyperuricemia. Both LEP20 and LEP50 substantially lowered uric acid levels in the blood and reduced activity of xanthine oxidase, the liver enzyme that makes uric acid from purines. They also improved standard markers of kidney function (creatinine and urea nitrogen) and liver damage (AST and ALT), and tissue examinations showed less scarring, swelling, and inflammatory cell invasion in these organs. In the kidneys, both polysaccharides pushed uric acid handling in a favorable direction: they dialed down transporters that reabsorb uric acid back into the blood and boosted transporters that pump it out for excretion. LEP20 was consistently more potent than LEP50 in easing inflammation, enhancing antioxidant defenses, and restoring the microscopic structure of kidney and liver tissue.
The Gut as a Control Center
Because the gut and its microbes are now known to strongly influence uric acid and inflammation, the researchers examined the intestines in detail. Hyperuricemic rats showed damaged gut lining, weakened “tight junction” proteins that normally seal the barrier, and higher levels of inflammatory molecules. Treatment with either polysaccharide partially reversed these problems, with LEP20 again giving stronger protection. Using DNA sequencing, the team found that both compounds reshaped the gut microbiota but in distinct ways. LEP20 favored the growth of beneficial, short‑chain‑fatty‑acid‑producing bacteria such as Blautia and Lactobacillus, while suppressing potentially harmful strains. This shift raised levels of key microbial acids—especially butyrate—that are known to strengthen the gut barrier and calm inflammation. LEP50 also improved the microbiota but more strongly influenced species and functions tied to purine metabolism, the chemical pathway that generates uric acid from dietary and internal sources.
Different Roads to Lower Uric Acid
To connect these microbial changes to chemistry in the body, the team profiled hundreds of small molecules in the rats’ feces. LEP20 mainly altered fat‑related and tryptophan pathways and boosted metabolites linked to antioxidant protection and anti‑inflammatory effects. LEP50, in contrast, had a clearer impact on purine and nucleotide metabolism. Notably, it lowered hypoxanthine, a direct precursor that xanthine oxidase converts into uric acid, and increased certain bile‑acid‑related compounds that may help eliminate uric acid. When the scientists matched microbes, metabolites, and health markers, they saw that “good” bacteria and their products were associated with lower uric acid, better kidney and liver tests, and more favorable uric acid transporter patterns, while “bad” bacteria and purine breakdown products tracked with worse outcomes.
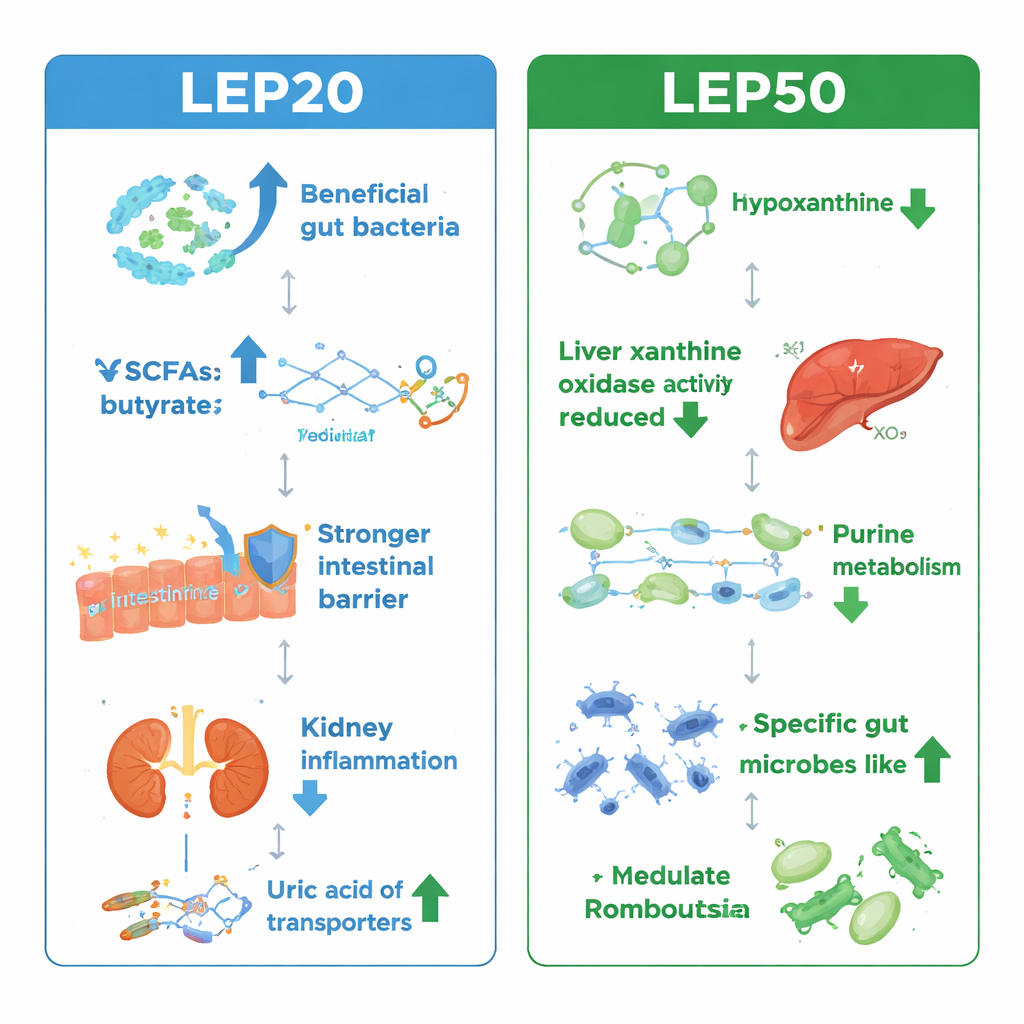
What This Means for People with High Uric Acid
Overall, the study shows that two closely related fibers from shiitake mushrooms can both ease high uric acid and protect the kidneys, liver, and gut—but they do so through different main routes. The β‑glucan‑type LEP20 leans toward reinforcing the gut barrier, quelling inflammation, and boosting antioxidant capacity via beneficial microbes and their short‑chain fatty acids. The α‑glucan‑type LEP50 more directly influences purine metabolism and uric acid production. For a layperson, the takeaway is that not all “mushroom polysaccharides” are interchangeable: their fine‑scale structure matters, shaping how they interact with the microbiome and the body’s metabolism. This understanding could guide the design of future functional foods or supplements that combine specific mushroom fibers to more safely and effectively manage hyperuricemia and related conditions.
Citation: Xiong, X., Liu, P., Liu, L. et al. Structural divergence of lentinula edodes polysaccharides is associated with distinct anti-hyperuricemia pathways. npj Sci Food 10, 64 (2026). https://doi.org/10.1038/s41538-026-00714-w
Keywords: hyperuricemia, shiitake mushroom, polysaccharides, gut microbiota, uric acid