Clear Sky Science · en
SN/VTA neuromelanin signal is associated with subclinical paranoia irrespective of familial risk for psychosis
Why Everyday Suspicion Matters
Many people occasionally feel that others are talking about them or might wish them harm, even when there is no clear evidence. These fleeting suspicious thoughts are a milder form of paranoia and are surprisingly common in the general population. The featured study asks a simple but important question: are these everyday paranoid thoughts tied to the same brain chemistry systems that underlie full-blown psychotic disorders such as schizophrenia?
The Brain’s Suspicion Switch
Scientists have long suspected that the brain chemical dopamine plays a central role in psychosis, including hallucinations and paranoid delusions. Dopamine-producing cells deep in the midbrain, in regions called the substantia nigra and ventral tegmental area, send signals to many other brain areas that help us learn from experience and update our beliefs. When this system is overactive, it may cause people to see meaning or threat where there is none, feeding into paranoid ideas. But it has been unclear whether the same system is involved in the quieter, subclinical paranoid thoughts that many people have, especially those with a family history of psychosis.
Using Brain Pigment as a Long-Term Gauge
To probe this question, the researchers turned to a special kind of MRI scan that can detect neuromelanin, a dark pigment that slowly builds up inside dopamine-producing neurons over many years. Because neuromelanin forms as a by-product of dopamine breakdown, its signal on these scans can act as a rough, noninvasive indicator of long-term dopamine activity. In this study, 102 adults took part: 25 had a parent or sibling with a psychotic disorder, and 77 had no close relatives with psychosis. None of the participants themselves had psychotic illnesses. All volunteers completed detailed questionnaires about how often they experienced paranoid thoughts, how convincing those thoughts felt, and how distressing they were.
Family History Was Not the Deciding Factor
The team first examined whether people with a first-degree relative with psychosis showed stronger neuromelanin signal than those without such a family history. After carefully accounting for age and sex, they found no meaningful differences between the two groups in the midbrain regions studied. This suggests that simply having a close relative with psychosis does not necessarily translate into a clearly higher long-term dopamine signal in these brain areas, at least in people who have not developed psychosis themselves. The authors caution that subtle differences may have gone undetected, but the results argue against a large, straightforward effect of familial risk on this measure.
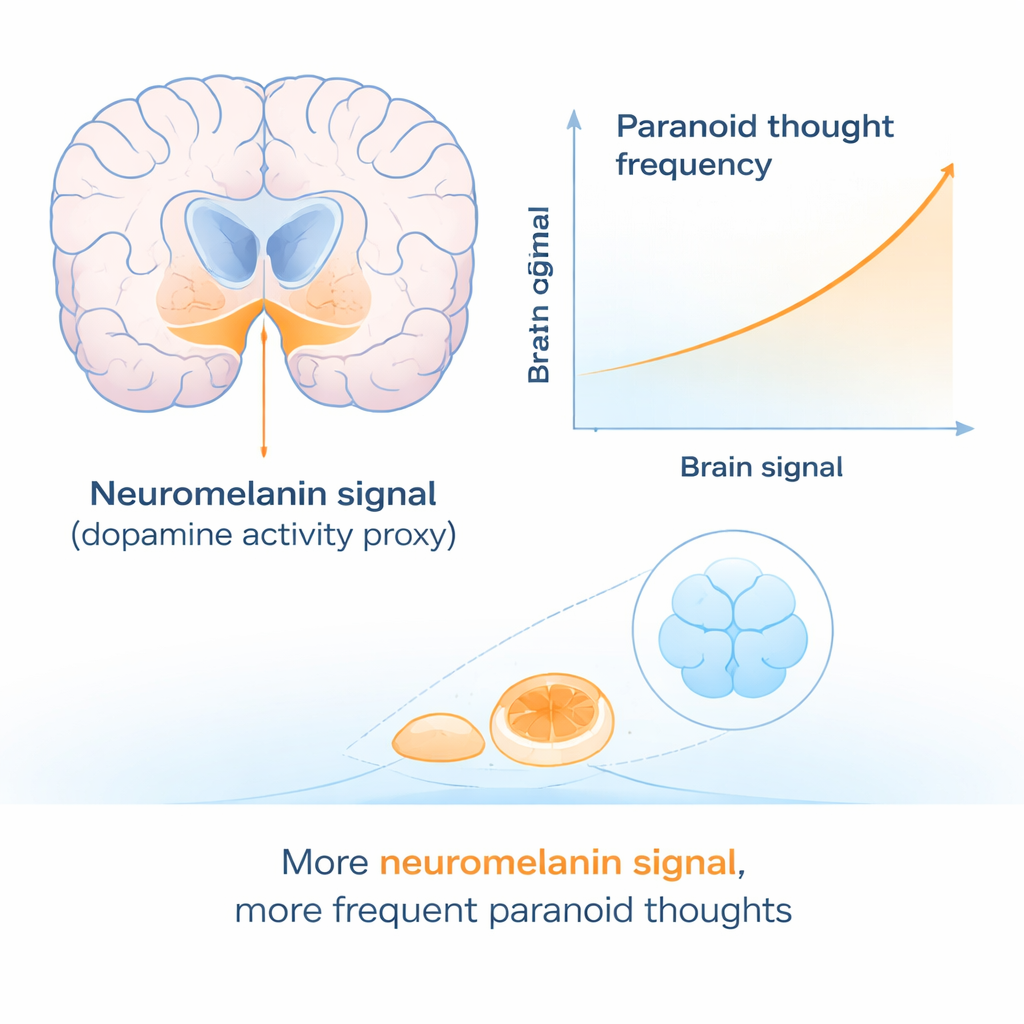
Paranoid Thoughts and Brain Signal Go Hand in Hand
Next, the researchers set aside family background and looked across all participants to see whether brain signal strength tracked with paranoid thinking. Here, a clear pattern emerged. People who reported more frequent paranoid thoughts tended to have a stronger neuromelanin signal in a specific part of the midbrain. This link appeared consistently across two different paranoia questionnaires. Intriguingly, the relationship was specific to how often paranoid thoughts occurred; it did not show up for how strongly people believed those thoughts or how upsetting they found them. That pattern hints that the dopamine system may be especially tied to the basic generation of suspicious ideas, while other factors determine whether those ideas become firmly believed and deeply distressing.
What This Means for Understanding Psychosis
For non-specialists, the take-home message is that the brain chemistry changes associated with psychosis seem to extend into everyday life. A stronger long-term dopamine signal in midbrain regions was linked to more frequent paranoid thoughts in people with and without a family history of psychosis, even though none were clinically psychotic. At the same time, this elevated signal alone did not appear to be enough to produce the fixed, distressing delusions seen in illness. The findings support the idea of a continuum: many people experience mild forms of paranoia, possibly nudged along by how their dopamine system works, but additional biological or environmental triggers are likely needed for those thoughts to harden into the severe, life-disrupting symptoms of psychotic disorders.
Citation: Hamati, R., Kanaa, N., Chidiac, B. et al. SN/VTA neuromelanin signal is associated with subclinical paranoia irrespective of familial risk for psychosis. Schizophr 12, 25 (2026). https://doi.org/10.1038/s41537-026-00731-4
Keywords: paranoia, dopamine, schizophrenia, brain imaging, neuromelanin MRI