Clear Sky Science · en
Whole-brain functional connectivity predicts ultra-high risk for psychosis status and level of functioning
Why brain wiring matters before illness starts
Psychotic disorders like schizophrenia rarely appear out of the blue. Many people first go through a phase where they are at ultra-high risk for psychosis: they may have brief or milder unusual experiences, struggle in daily life, yet never develop full-blown psychosis. This study asks a simple but crucial question: can differences in how the brain’s regions “talk” to each other at rest help identify who is in this risk state and explain why many of them have trouble with work, school, and relationships?
Peeking at the resting brain
To explore this, researchers scanned the brains of 102 young adults at ultra-high risk for psychosis and 105 healthy peers. While participants simply lay still with their eyes closed, a technique called resting-state functional MRI tracked tiny, moment-to-moment changes in blood flow across the brain. By comparing how strongly different regions’ activity rose and fell together, the team built a map of each person’s “functional connectivity” – in essence, which parts of the brain tend to fire in sync.
Finding patterns in thousands of connections
Rather than focusing on a few brain areas, the scientists looked at more than 32,000 possible connections across the whole brain. They used a modern machine-learning method (NBS-Predict) that searches for networks of connections that, taken together, can distinguish people at risk from healthy controls or can predict a person’s day-to-day functioning. This approach helps avoid being misled by random noise and instead highlights coherent subnetworks: clusters of brain regions that repeatedly show up as important across many tests of the data.
The thalamus as a busy traffic hub
A clear theme emerged: the thalamus – a deep structure that helps route information between sensory systems and higher thinking areas – acted as a central traffic hub. Compared with healthy participants, ultra-high-risk individuals showed stronger connections (“hyper-connectivity”) between thalamus and regions involved in movement and attention, as well as more cross-talk between the two hemispheres. These same hyper-connected networks tended to be linked with poorer social and occupational functioning across the entire sample, regardless of diagnosis. At the same time, ultra-high-risk participants showed weaker connections (“hypo-connectivity”) between thalamus and midline regions important for internal thought and control of attention. Across all participants, stronger connectivity in these hypo-connected networks was associated with better functioning.
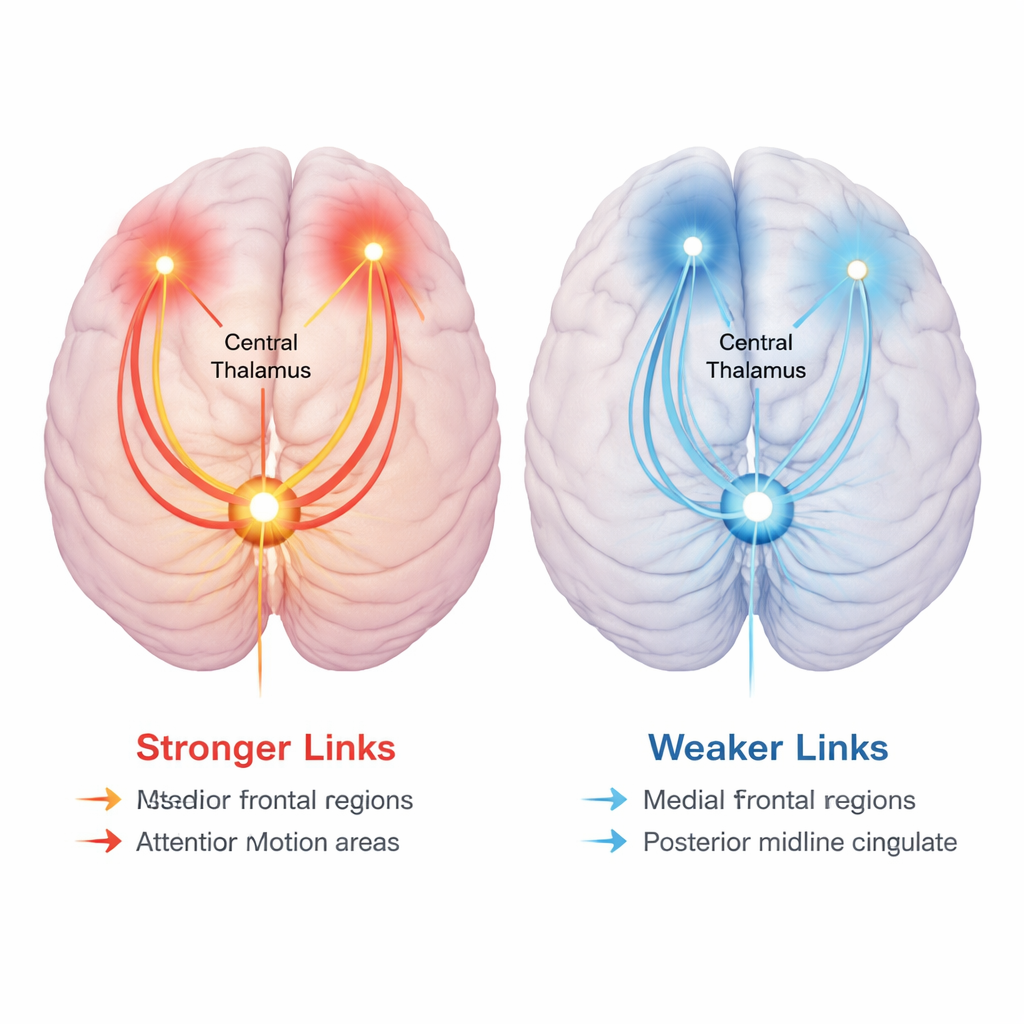
Functioning, not just future psychosis
Interestingly, the very connections that best distinguished ultra-high-risk individuals from healthy peers were also the ones that best predicted how well people were coping in everyday life. In other words, the hallmark brain patterns of being in this risk state are tied less to whether someone will definitely develop psychosis and more to how much their symptoms interfere with work, study, and social life. Within the ultra-high-risk group alone, brain connectivity did not reliably predict symptom severity or intelligence scores, underscoring that the strongest signals were about broad, cross-group differences in functioning rather than fine-grained differences within the at-risk group.
What this means for early help
For a layperson, the take-home message is that long before psychosis fully develops – and even in people who may never progress to that stage – the brain’s communication highways can already look different. In this study, the thalamus sits at the center of these changes, with some routes seemingly overused and others underused. These patterns are closely tied to how well people manage daily responsibilities and relationships. While the brain scans are not accurate enough to serve as a diagnostic test, they point to a biological signature of vulnerability that could, in the future, help clinicians identify those who need extra support and design treatments aimed at normalizing key networks rather than waiting for illness to worsen.
Citation: Ambrosen, K.S., Kristensen, T.D., Glenthøj, L.B. et al. Whole-brain functional connectivity predicts ultra-high risk for psychosis status and level of functioning. Schizophr 12, 22 (2026). https://doi.org/10.1038/s41537-025-00685-z
Keywords: psychosis risk, brain connectivity, resting-state fMRI, thalamus, social functioning