Clear Sky Science · en
Activated Hedgehog signaling in keratocytes leads to stromal stiffness and impairs corneal regeneration
Why the Clear Window of the Eye Can Turn Cloudy
The cornea is the eye’s front window, and its see-through quality is essential for sharp vision. Yet burns, trauma, and some diseases can turn this clear tissue cloudy and scarred, sometimes leading to blindness. This study asks a simple but important question: why do some corneas heal cleanly while others heal with lasting damage? The authors focus on a hidden conversation between support cells inside the cornea and the surface cells that restore the smooth, transparent coating after injury.
The Hidden Support Cells Under the Surface
Most of the cornea is made of a tough, transparent middle layer called the stroma. It is packed with orderly collagen fibers and scattered cells known as keratocytes. In healthy adult eyes, these keratocytes are quiet but busy: they maintain the collagen framework and release growth factors that nourish the surface epithelium, which is constantly renewed by stem cells at the edge of the cornea. The researchers show that, in young mice, a molecular pathway called Hedgehog is active in these keratocytes but then shuts down as the eye matures. When they genetically blocked Hedgehog signaling in adult keratocytes, the corneas looked normal, suggesting that quiescence—not ongoing activity—is the natural state for this pathway in a healthy, clear cornea.
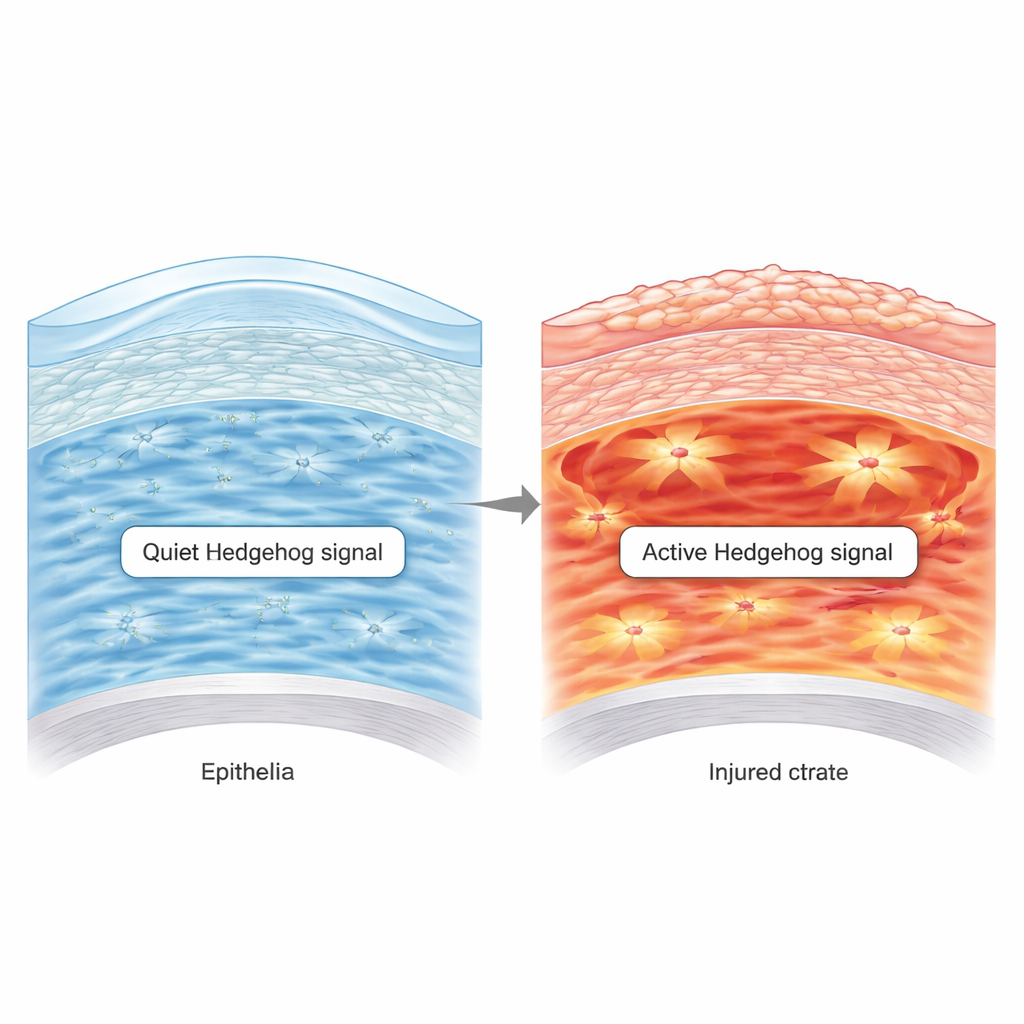
When Chemical Burns Wake Up a Sleeping Pathway
Superficial scratches on the cornea usually heal in a day or two: stem cells divide, new epithelial cells slide in, and the stroma remains largely undisturbed. Chemical burns are much more destructive. In a mouse model of alkaline burns, the team observed long-lasting defects—thin, poorly layered surface cells over a disorganized stroma. They found that Hedgehog signaling was strongly reactivated in keratocytes after chemical injury, but not after simple scraping. This surge was linked to inflammatory molecules, especially the cytokine TNF‑α, which the authors showed can directly switch on the Hedgehog program in cultured keratocytes. The results suggest that severe inflammation after a burn pushes normally quiet stromal cells into a harmful, overactive state.
From Helpful Maintainers to Rigid Scar Builders
To understand what happens when Hedgehog stays switched on, the scientists engineered mice in which keratocytes have chronically active Hedgehog signaling. Even without injury, these corneas gradually developed a thinner, stiffer stroma. Gene profiling of isolated keratocytes revealed that they were changing identity: classical keratocyte markers declined, while genes typical of fibroblasts and mesenchymal stem–like cells increased. At the same time, production of key extracellular matrix components—such as collagen and a structural protein called keratocan—dropped. Under the microscope, collagen fibrils crowded together, and mechanical testing showed that the stromal tissue became more than twice as stiff as normal. These changes turned the supportive matrix into a rigid scaffold, a hallmark of scarring tissue.
How a Stiff Bed Stops the Surface from Healing
A surprising twist in the story came from the corneal surface. In mice with chronically active Hedgehog in keratocytes, the epithelium initially closed wounds on schedule, but later failed to mature properly. The surface layer remained thin, with many immature cells and few fully differentiated, cornea‑specific cells. The team traced this defect to a mechanical signaling system in epithelial cells known as the Hippo–YAP pathway, which senses how stiff the underlying tissue is. In the stiffened stroma, Hippo signaling was switched on, which in turn shut down YAP, a protein that normally promotes healthy differentiation. When the researchers applied a small molecule that inhibits Hippo signaling, YAP activity returned and the epithelium regained near‑normal thickness and structure—even though the stroma itself stayed thin. This indicates that the rigidity of the stromal “bed” can directly govern whether the surface can rebuild itself correctly.
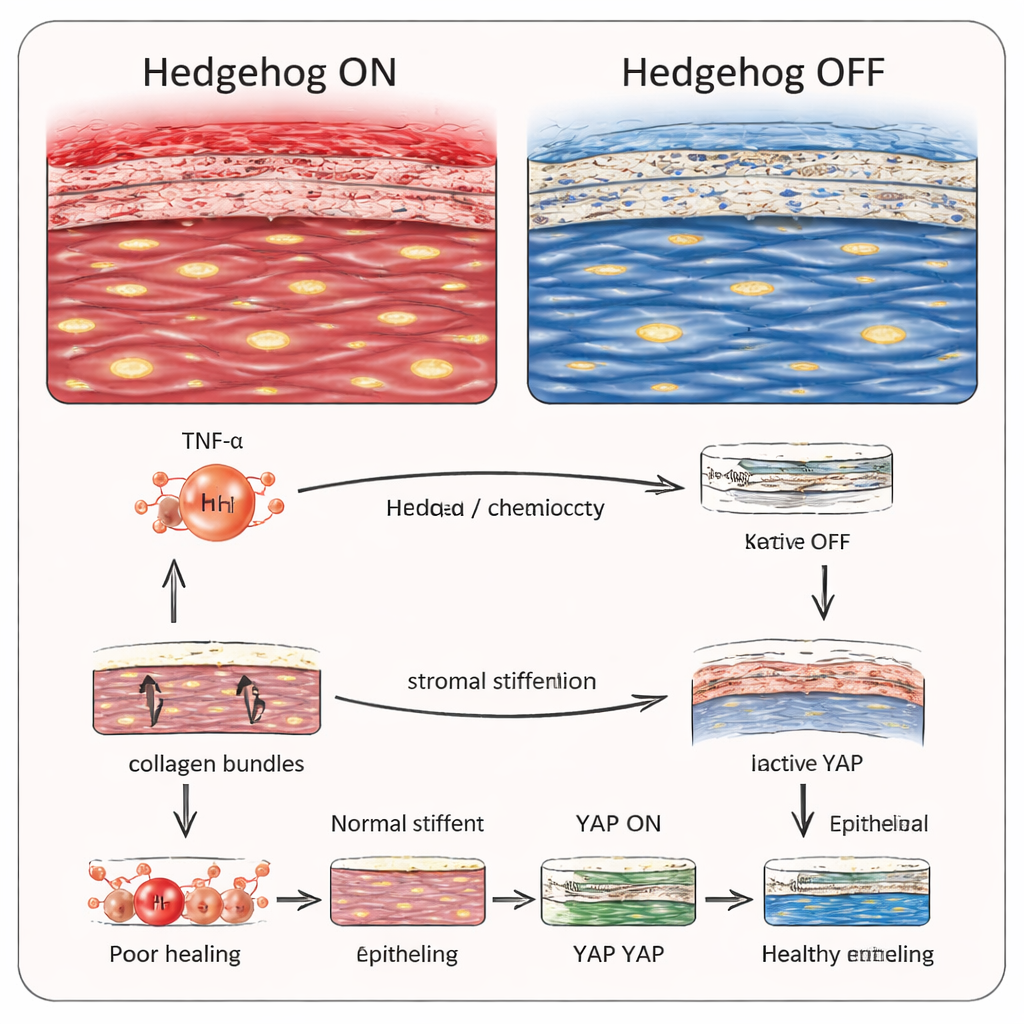
Turning Down Hedgehog to Rescue Vision
The most hopeful part of the work came from experiments that dialed Hedgehog signaling back down. In mice with genetically activated Hedgehog, treating them with a drug that blocks the pathway’s key transcription factors restored stromal organization and rescued surface cell differentiation. In separate experiments, mice that lacked a core Hedgehog component in keratocytes were protected from the usual scarring and epithelial defects after chemical burns. Finally, applying a Hedgehog‑blocking drug to the eyes of normal mice after alkaline injury markedly improved corneal structure without obvious side effects. For a lay reader, the message is that an overexcited “repair” pathway in the cornea’s support cells can actually sabotage healing by stiffening the tissue and confusing the surface cells. By carefully turning this pathway down, it may be possible to guide the cornea to heal clear rather than cloudy, offering a new avenue for treating chemical burns and possibly other conditions, such as diabetic eye disease, where wound healing is chronically impaired.
Citation: Yu, Q., Li, P., Du, Z. et al. Activated Hedgehog signaling in keratocytes leads to stromal stiffness and impairs corneal regeneration. npj Regen Med 11, 9 (2026). https://doi.org/10.1038/s41536-026-00453-2
Keywords: corneal wound healing, Hedgehog signaling, stromal stiffness, keratocytes, chemical eye injury