Clear Sky Science · en
Profiling of 5-hydroxymethylcytosine in blood reveals preferential enrichment at exon-intron junctions and predictive value for Parkinson’s disease
Why Blood Can Reveal Clues About Parkinson’s
Parkinson’s disease is best known for its tremors and movement problems, but the early biological changes that lead to these symptoms remain hard to detect. This study asks a simple, practical question with big implications: can a standard blood sample reveal subtle chemical marks on DNA that both reflect Parkinson’s biology and help distinguish people with the disease from those without it? By focusing on these DNA marks, the researchers look for a bridge between everyday environmental exposures, our genes, and the gradual breakdown of brain cells seen in Parkinson’s.
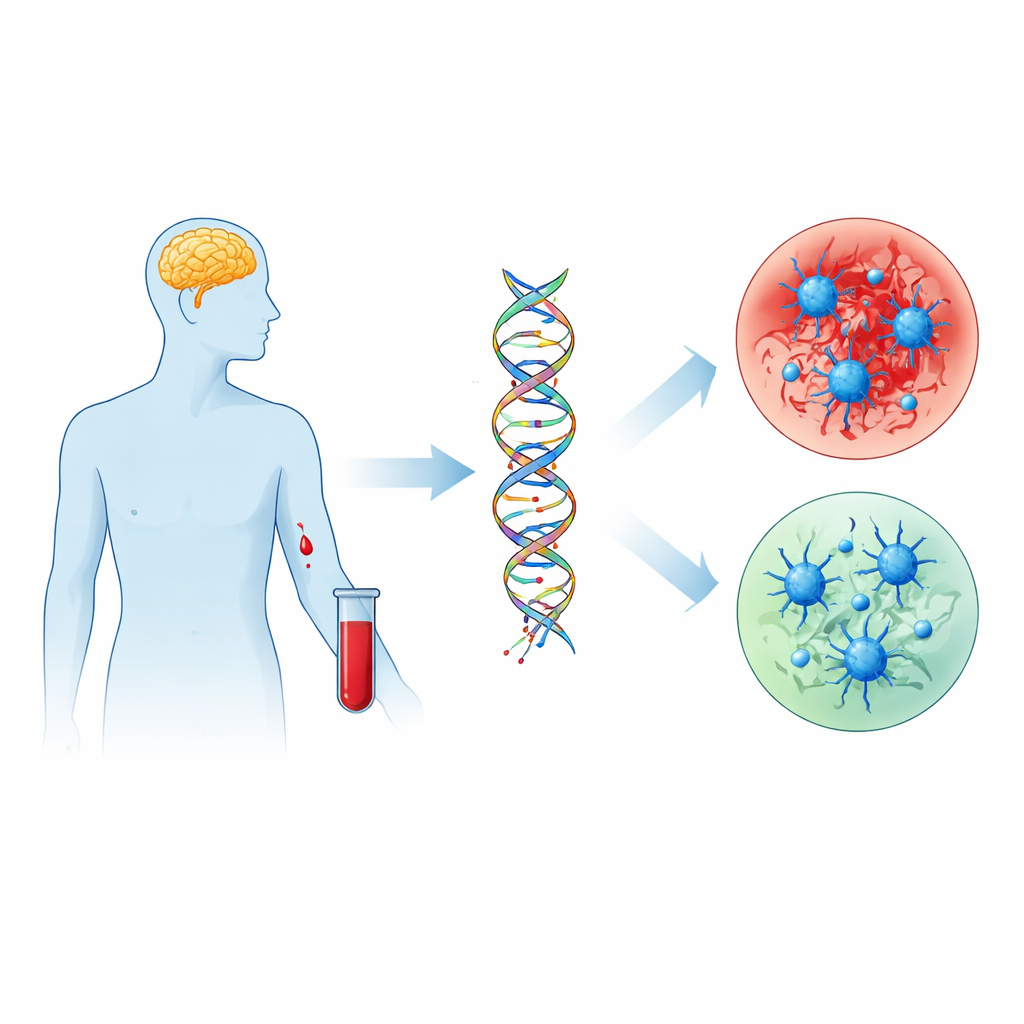
Tiny Marks on DNA as Chemical Footprints
Inside every cell, DNA carries not only genetic code but also tiny chemical tags that help control which genes are turned on or off. Two such tags, called 5-methylcytosine and 5-hydroxymethylcytosine, act like adjustable dimmer switches on gene activity. Previous work suggested that these tags change in the brains of people with Parkinson’s, but brain tissue is difficult to study in living patients. Here, the scientists turned instead to white blood cells taken from 109 people with Parkinson’s and 49 neurologically healthy volunteers. They measured the overall levels of these DNA marks and then used high-density DNA chips to map where, along the genome, the tags were altered.
A Global Drop in One Key DNA Mark
The team found a consistent reduction in the overall amount of 5-hydroxymethylcytosine in blood cells from people with Parkinson’s, while the related mark 5-methylcytosine did not differ between groups. This pattern held even after accounting for age, sex, common genetic risk variants, and Parkinson’s medications such as levodopa. A statistical model that combined age, sex, and the two DNA marks could correctly identify people with Parkinson’s about 88 percent of the time, with 5-hydroxymethylcytosine emerging as one of the most informative features. However, these global levels did not clearly track how advanced a person’s disease was, suggesting they signal the presence of Parkinson’s more than its stage.
Where the DNA Changes Prefer to Occur
Looking more closely along the genome, the researchers observed that altered DNA marks were not randomly scattered. Instead, both types of changes clustered inside genes, particularly in the stretches of DNA called introns that sit between the protein-coding pieces known as exons. Within these introns, the most strongly affected regions lay close to the boundaries where an intron meets an exon. These boundary zones are important because they guide how RNA is cut and stitched together when a gene is read, shaping which versions of a protein are produced. The study suggests that, in Parkinson’s, DNA marking is especially disturbed at these critical junctions, potentially nudging cells toward different protein variants.
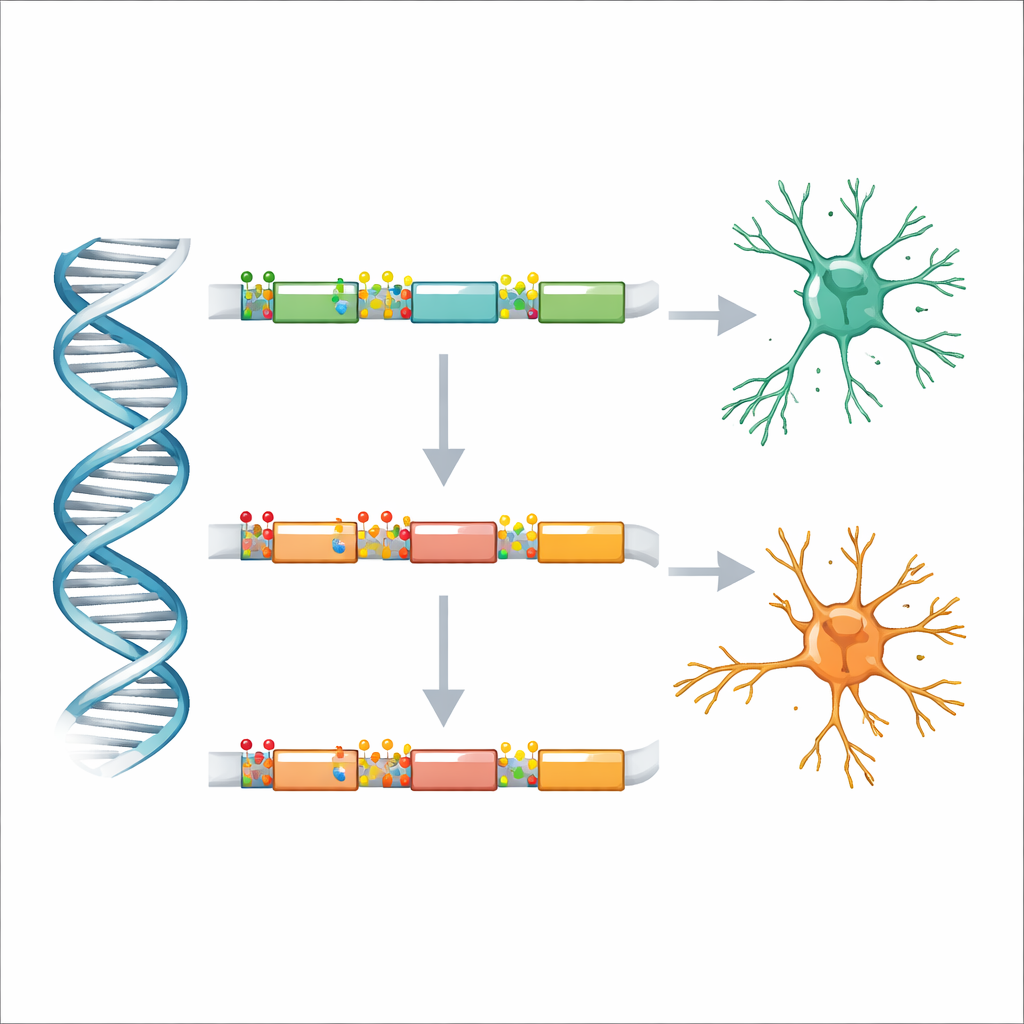
Gene Networks Involving Nerves, Blood Vessels, and Immunity
The genes sitting underneath these altered DNA marks pointed to biological systems already suspected in Parkinson’s. Regions with changed methylation were linked to nerve-cell communication, brain development, and the formation and remodeling of blood vessels. Regions with altered hydroxymethylation, in contrast, were enriched in genes involved in immune signaling and broader cell-to-cell communication. Many named genes have known roles in maintaining dopamine-producing neurons, controlling synapses, or shaping the brain’s immune and vascular environment. Together, the patterns hint that Parkinson’s may involve a coordinated shift in how genes controlling nerve function, blood flow, and immune activity are regulated.
What This Could Mean for Patients
For non-specialists, the key takeaway is that a simple blood draw can capture DNA “punctuation marks” that differ in people with Parkinson’s, and these differences are most pronounced at the junctions where genes are spliced into final messages. The study is exploratory and based on relatively small numbers, so it cannot yet prove cause and effect or support a clinical test on its own. Still, it strengthens the idea that 5-hydroxymethylcytosine in blood may serve as a convenient biomarker to flag Parkinson’s and to probe how gene regulation, immune responses, and blood vessel changes contribute to the disease. With larger follow-up studies, these chemical traces on DNA may help move diagnosis and monitoring from the brain—where sampling is difficult—to the bloodstream, where it is far more accessible.
Citation: Antczak, P., Brandt, P., Radosavljević, L. et al. Profiling of 5-hydroxymethylcytosine in blood reveals preferential enrichment at exon-intron junctions and predictive value for Parkinson’s disease. npj Parkinsons Dis. 12, 76 (2026). https://doi.org/10.1038/s41531-026-01322-x
Keywords: Parkinson’s disease, epigenetics, DNA hydroxymethylation, blood biomarkers, gene regulation