Clear Sky Science · en
Pedunculopontine-thalamic cholinergic projections in rapid eye movement sleep behaviour disorder
Why dream actions may warn of brain disease
Some people act out their dreams—kicking, shouting, or punching while still asleep. This condition, called REM sleep behavior disorder, can be more than a nighttime nuisance. Many of those who have it later develop Parkinson’s disease or a related form of dementia. The study summarized here asks whether a specific set of brain cells that use the chemical messenger acetylcholine show early damage in these patients, and whether this damage could help predict who is most likely to go on to full-blown disease.
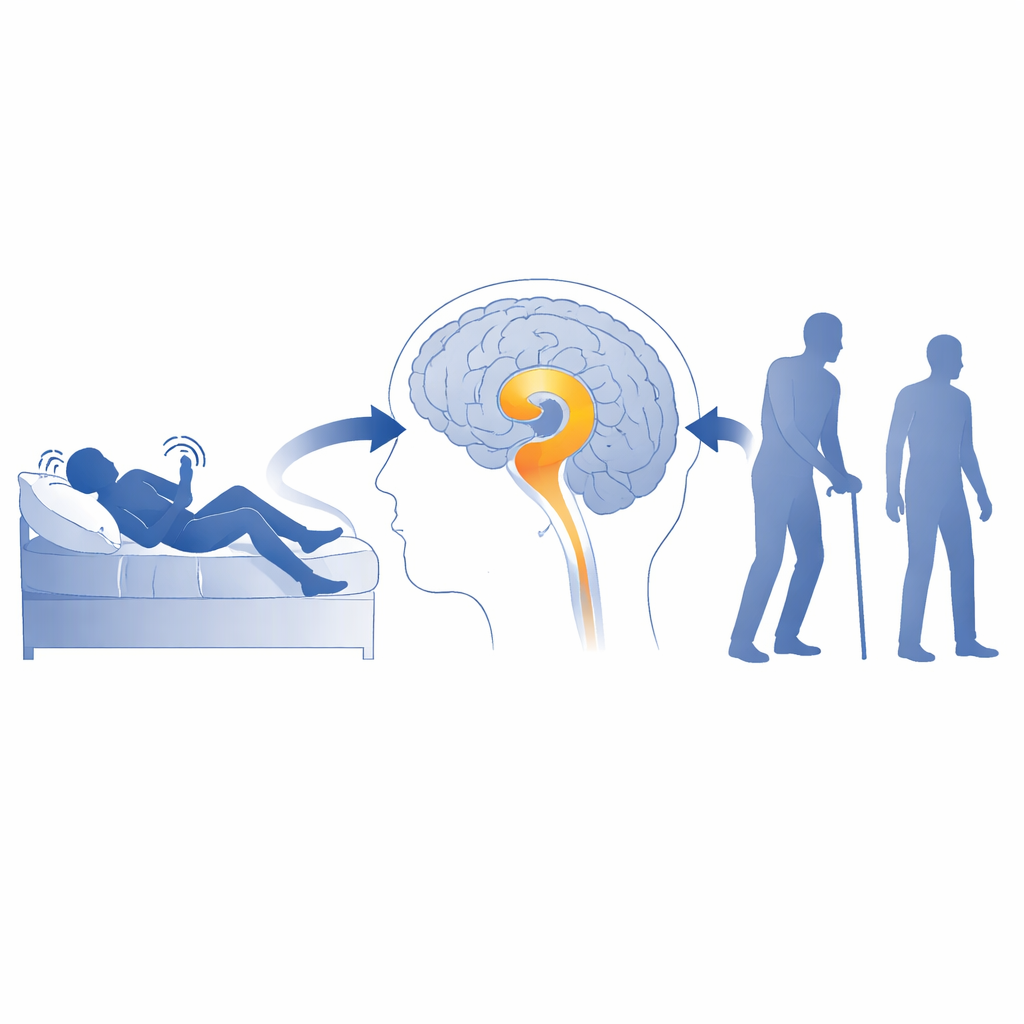
Two brain hubs that keep the mind alert
The researchers focused on two major hubs of acetylcholine-producing cells. One lies deep in the front of the brain and sends widespread branches to thinking areas of the cortex; this system is strongly linked to attention and memory and is known to degenerate in both Parkinson’s disease and Alzheimer’s disease. The second hub sits lower down in the brainstem, in a region called the pedunculopontine nucleus, which sends its signals upward to the thalamus, a relay station that helps regulate sleep, movement, and alertness. Earlier work suggested that this brainstem–thalamus route might be hit harder in Parkinson’s-related conditions than in Alzheimer’s disease, hinting that it could be a more specific early warning sign.
Scanning sleeping brains
Using data from an international project that tracks people at risk for Parkinson’s disease, the team examined brain scans from 146 people with isolated REM sleep behavior disorder and 102 similar adults without the condition. They measured the size of the front-of-brain acetylcholine hub and used diffusion imaging—an MRI method that infers the health of nerve fibers from the way water moves through tissue—to assess three sets of wiring: two pathways from the forebrain hub to the cortex, and the pathway from the brainstem hub up to the thalamus. Participants also completed a battery of thinking and memory tests and were followed for several years to see who would develop Parkinson’s disease or dementia with Lewy bodies.
Early damage in a deep sleep–movement circuit
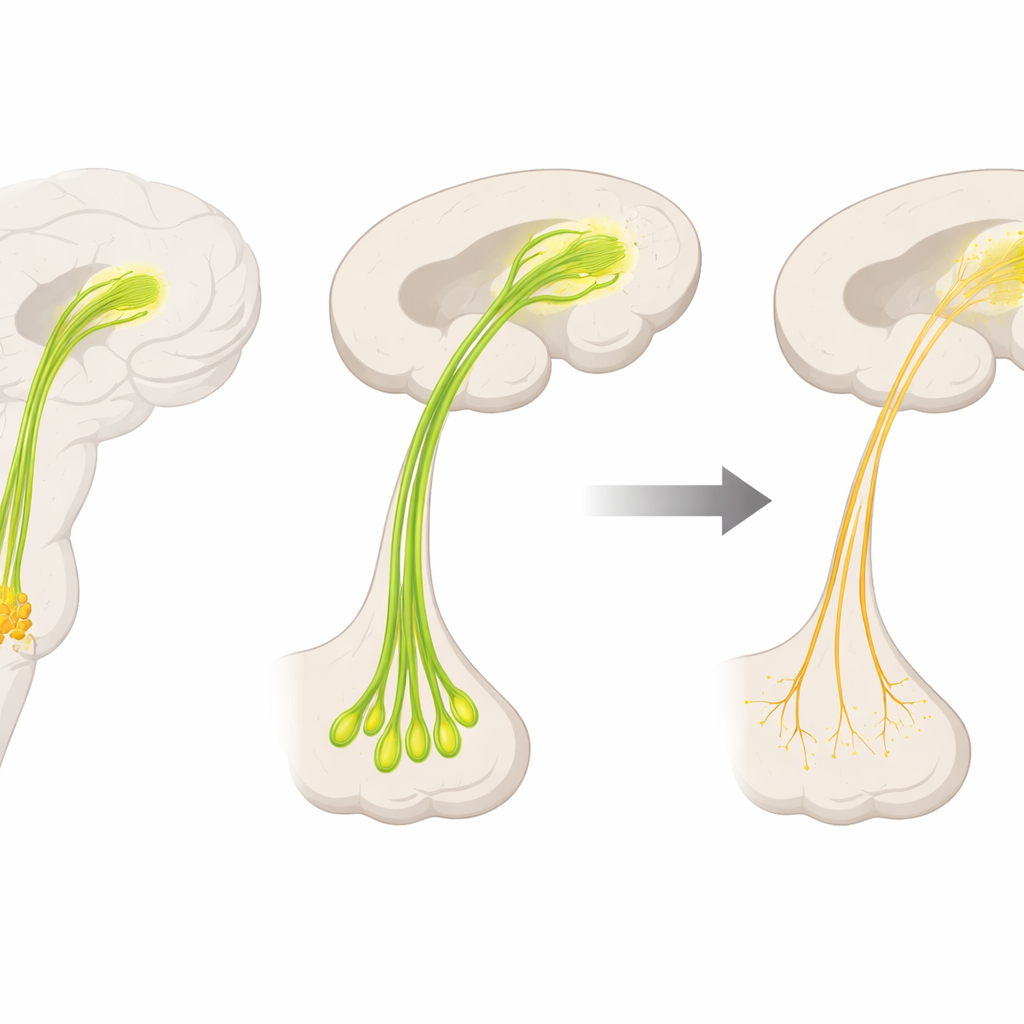
The most striking differences between patients and healthy volunteers appeared in the brainstem-to-thalamus pathway. In those with REM sleep behavior disorder, the fibers here showed signs of microstructural breakdown, especially on the left side. In contrast, the size of the front-of-brain acetylcholine hub and the integrity of its two main pathways looked similar in patients and controls, apart from a subtle sign that one of these routes might even be slightly more ordered at this very early stage. Within the patient group, however, individuals with better-preserved forebrain pathways tended to perform better on tests of attention, language, and speed of thinking, suggesting that mild wear and tear in this system is already linked to subtle cognitive changes.
Links to future decline and diagnosis
When the researchers examined changes over a year, they found that healthier forebrain pathways were associated with less decline in certain thinking skills. Most importantly, they asked whether the health of any of these acetylcholine systems could foretell who would go on to Parkinson’s disease or dementia with Lewy bodies. Over a median of about two years of follow-up, 12 patients converted to one of these diagnoses. Those with more abnormal diffusion measures along the brainstem-to-thalamus pathway had roughly double the risk of conversion compared with those with more intact fibers, while measures from the forebrain hub and its cortical pathways did not clearly predict conversion in this early dataset.
What this means for patients and future care
Taken together, the findings suggest that in people who act out their dreams, the acetylcholine pathway linking the lower brainstem to the thalamus may start to deteriorate earlier than the better-known forebrain system. This deep circuit may therefore be a particularly sensitive marker of very early Lewy body disease, and with further validation could help doctors identify which patients with REM sleep behavior disorder are at highest risk of developing Parkinson’s disease or dementia. Because the study still includes relatively few patients who have converted, and because some results weakened after adjusting for overall white matter health, larger and longer-term studies will be needed before these scans can guide individual treatment decisions. Nonetheless, the work charts a promising route toward catching brain disease years before classic symptoms appear.
Citation: Schumacher, J., Teipel, S., Storch, A. et al. Pedunculopontine-thalamic cholinergic projections in rapid eye movement sleep behaviour disorder. npj Parkinsons Dis. 12, 67 (2026). https://doi.org/10.1038/s41531-026-01311-0
Keywords: REM sleep behavior disorder, Parkinson’s disease risk, cholinergic pathways, brainstem thalamus circuit, Lewy body disease