Clear Sky Science · en
Comparative effects of medication combined with twenty rehabilitation therapies: core outcomes in 8202 parkinson’s patients
Why this matters for everyday life
Parkinson’s disease is often thought of as a problem of shaky hands, but for many of the more than eight million people living with it worldwide, the bigger challenges are staying steady on their feet, thinking clearly, and simply feeling like themselves. This study asks a practical question that patients, families, and clinicians face every day: when Parkinson’s drugs are already on board, which kinds of rehabilitation—exercise classes, brain stimulation, water therapy, tai chi, robotics, and more—seem to help most with movement, mood, and quality of life?
A big picture look at many rehab options
The researchers pulled together results from 186 clinical trials involving 8,202 people with Parkinson’s disease from 20 countries. In every trial, participants took standard Parkinson’s medication and then received one of 20 types of rehabilitation, ranging from familiar approaches like strength training and balance exercises to newer methods like virtual reality, robotic exoskeletons, and non-invasive brain stimulation. Instead of comparing just two therapies at a time, the team used a method called network meta-analysis, which allows them to weave together direct and indirect comparisons and build a single, large map of how all these options stack up against one another.
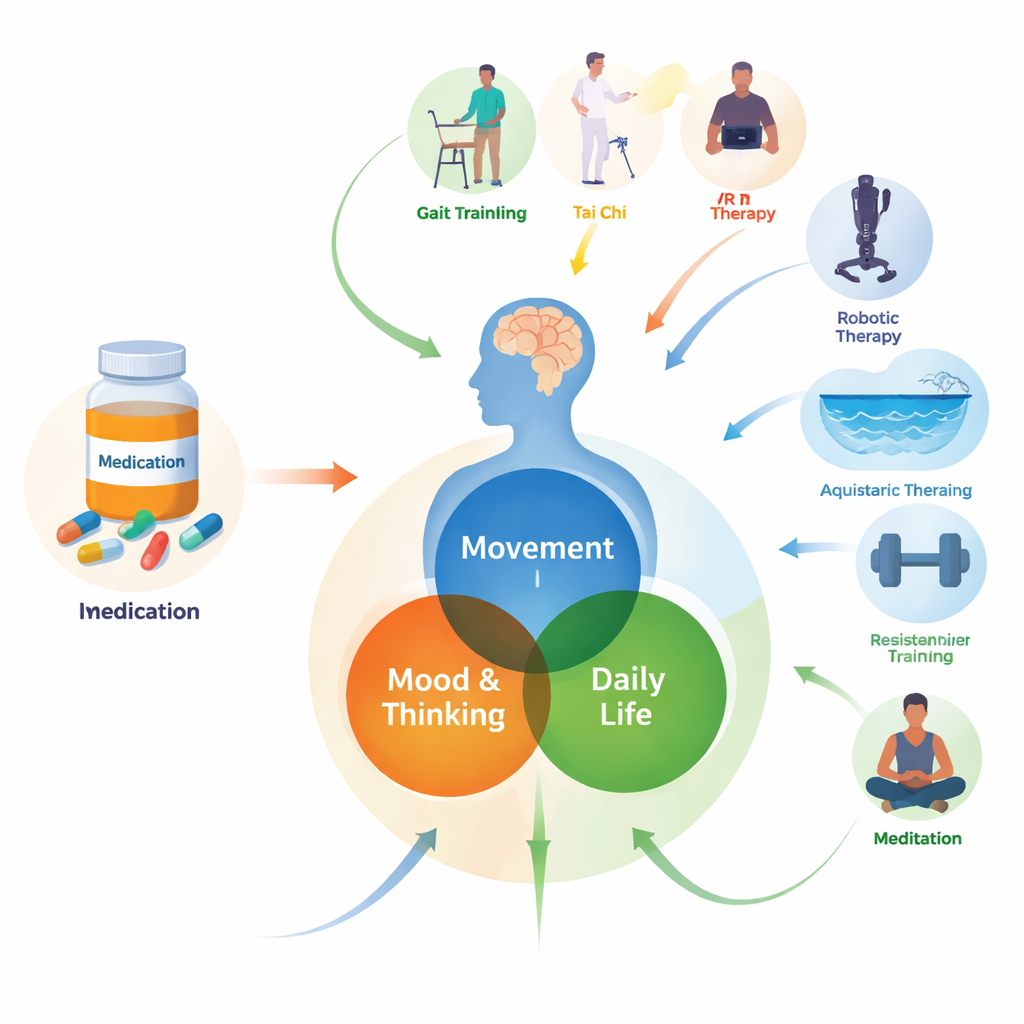
What seems to help with movement
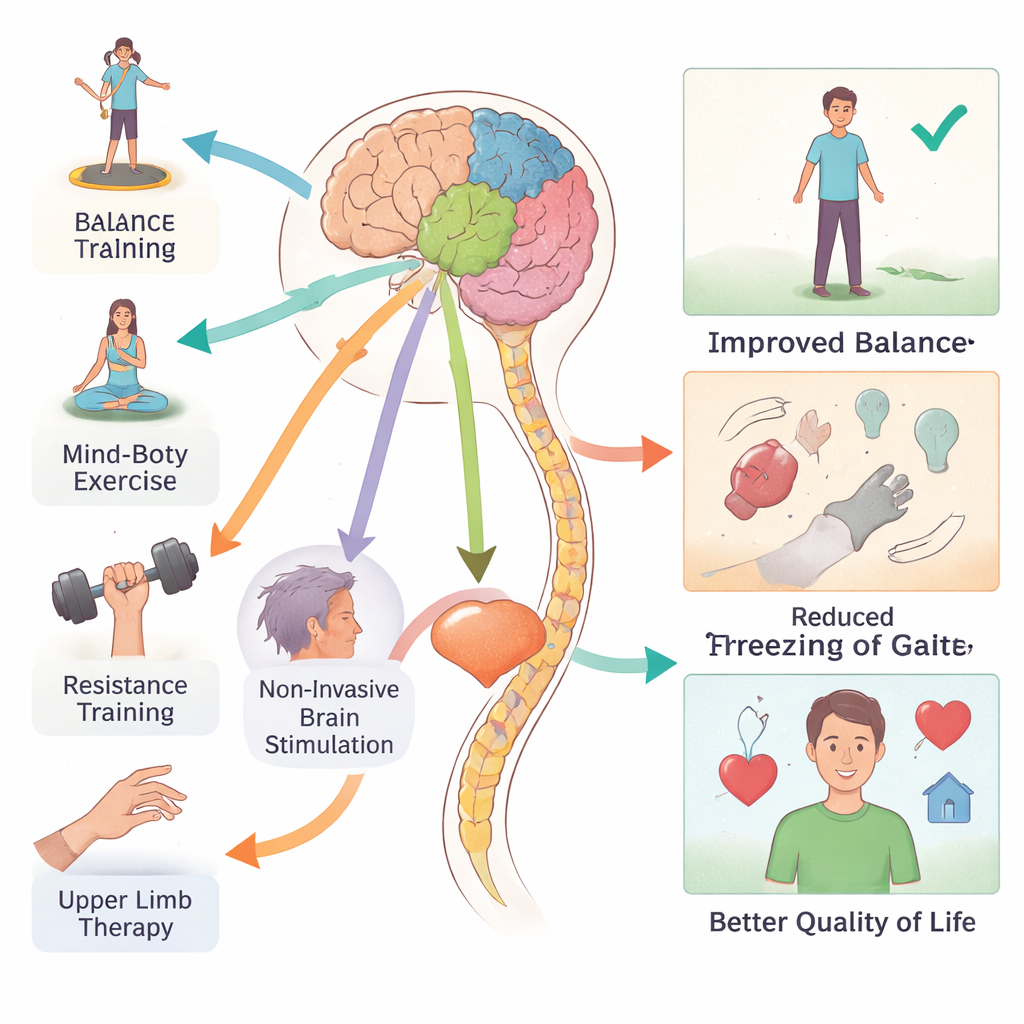
Many people with Parkinson’s struggle with balance, slowness, and episodes where their feet suddenly “freeze” while walking. The analysis suggests several combinations of drugs and rehab can meaningfully improve movement, although the strength of the evidence is modest. Traditional Chinese–style programs (including tai chi and related practices), water-based exercise, exoskeleton-assisted training, and conventional movement therapy all appeared to help balance more than usual care. Mind–body exercise programs and non-invasive brain stimulation—where weak electrical or magnetic currents are applied to the scalp—were linked to better overall motor ability. However, for the particularly disabling problem of freezing of gait, no single therapy clearly outperformed the others, highlighting how difficult this symptom remains to treat.
Thinking, mood, and the hidden burden
Parkinson’s disease affects far more than muscles. Many patients experience changes in memory, attention, and mood that can be just as disabling as tremor. Here, resistance training and non-invasive brain stimulation stood out as the most promising partners to medication for sharpening thinking skills, with art-based therapy showing potential as well. For emotional health, mind–body exercise—programs that blend movement with breathing, focus, or meditation—was the only approach that consistently eased negative mood. These findings echo growing evidence that targeted physical and mental practice can nudge brain circuits toward better function, even in a degenerative condition.
Everyday quality of life
Ultimately, people with Parkinson’s care less about test scores and more about whether they can dress themselves, leave the house safely, and enjoy time with others. When the researchers looked at measures of day-to-day well-being, therapies focused on the arms and hands and on resistance training were linked to the largest reported gains in quality of life, with cognitive–behavioral programs also showing benefits. Still, improvements were often modest, and gains in one area—such as balance—did not always translate into feeling better overall. This mismatch may reflect how complex real-life functioning is, and how slowly meaningful life changes can emerge.
How sure can we be?
Despite its size, the study comes with important caution flags. Many of the underlying trials were small, hard to blind, or varied widely in how often and how long therapies were delivered. When the authors carefully rated the strength of the evidence, most findings landed in the “low” or “very low” confidence range. Some calculated benefits were surprisingly large—bigger than what is usually seen in rehabilitation research—suggesting that statistical quirks, not just clinical effects, may be at work. The authors stress that their rankings are best viewed as a roadmap for future, better-designed trials, not as final verdicts.
What this means for patients and families
For people living with Parkinson’s, this work supports a simple but powerful message: medication alone is not enough, and carefully chosen rehabilitation can make a meaningful difference, especially for balance, strength, thinking, and mood. At the same time, there is no single “magic” therapy. The best approach is likely to be a tailored mix of exercises and brain-focused therapies, adjusted to a person’s symptoms, preferences, and access to care. As larger, more rigorous studies are done, doctors should gain clearer guidance on which combinations offer the greatest real-world payoff, bringing us closer to truly personalized rehabilitation for Parkinson’s disease.
Citation: Li, H., Lin, X., Huang, R. et al. Comparative effects of medication combined with twenty rehabilitation therapies: core outcomes in 8202 parkinson’s patients. npj Parkinsons Dis. 12, 52 (2026). https://doi.org/10.1038/s41531-026-01266-2
Keywords: Parkinson’s disease, rehabilitation, exercise therapy, brain stimulation, quality of life