Clear Sky Science · en
JAK/STAT1-interferon-ISGylation networks in breast cancer resistance to inhibitors of FOXM1 and CDK4/6
Why this matters for breast cancer treatment
Many women with estrogen receptor–positive (ER+) breast cancer now receive modern targeted drugs that slow tumor growth by halting the cell cycle. Yet, almost inevitably, tumors learn to work around these treatments and start growing again. This study asks a pressing question: when ER+ breast cancers become resistant to two major drug types—FOXM1 inhibitors and CDK4/6 inhibitors—what changes inside the cancer cells allow them to escape, and can those same changes reveal new ways to stop them?
A common survival wiring inside resistant tumors
The researchers focused on ER+ breast cancer cells that had been grown in the lab until they no longer responded to either FOXM1-blocking drugs or CDK4/6-blocking drugs such as palbociclib and abemaciclib. They found that, despite being made resistant to different drugs, these cells switched on a similar internal alarm system built around interferon signals and a protein called STAT1. This alarm leads to the production of many “interferon-stimulated genes” and a small protein called ISG15, which can be attached to other proteins like a molecular tag. Resistant cells had much higher levels of STAT1, activated STAT1, free ISG15, and ISG15-tagged proteins than their non-resistant counterparts, suggesting that this network forms a shared backbone of drug resistance.
A protective coat of molecular tags
Looking more closely, the team saw that the resistant cells not only made more ISG15 but also boosted enzymes that attach ISG15 onto other proteins, a process known as ISGylation. These enzymes—HERC5, HERC6, and UBE2L6—were strongly elevated, especially in FOXM1 inhibitor–resistant cells. Many cellular proteins, including STAT1 itself, carried ISG15 tags in resistant cells, often at higher levels than in the original drug-sensitive cells. Because adding these tags can change how long proteins last and how they behave, the buildup of ISGylated proteins appears to be part of how cancer cells toughen themselves against treatment.
Switching off the alarm weakens resistant cells
The investigators then asked whether turning down this alarm network would make resistant cells more vulnerable. They used drugs that block JAK kinases—key switches upstream of STAT1—and small interfering RNAs to reduce ISG15, HERC5, and HERC6. Blocking JAK1/2 signaling markedly lowered STAT1 activity, reduced ISG15 levels and ISGylation, and shrank the colonies formed by resistant cells, especially those resistant to FOXM1 inhibitors. Similarly, directly silencing ISG15 and its tagging enzymes decreased the overall ISGylation pattern and impaired cell survival. These experiments show that the interferon–STAT1–ISG15 system is not just a bystander but actively supports the growth and persistence of drug-resistant cancer cells.
New hope in sequential treatment strategies
One of the most encouraging findings is that the resistant cells were not stuck in a single invincible state. Breast cancer cells that had become resistant to CDK4/6 inhibitors still responded to FOXM1 inhibitors, and cells resistant to FOXM1 inhibitors could still be slowed by palbociclib or abemaciclib. In both two-dimensional cell layers and three-dimensional Matrigel cultures that better mimic tumors, switching drug classes sharply reduced cell growth and lowered the expression of genes that drive DNA copying and cell division. At the same time, patient data showed that high levels of ISG15 and its associated enzymes in ER+/HER2− tumors were linked to worse survival, underscoring the clinical relevance of this resistance wiring.
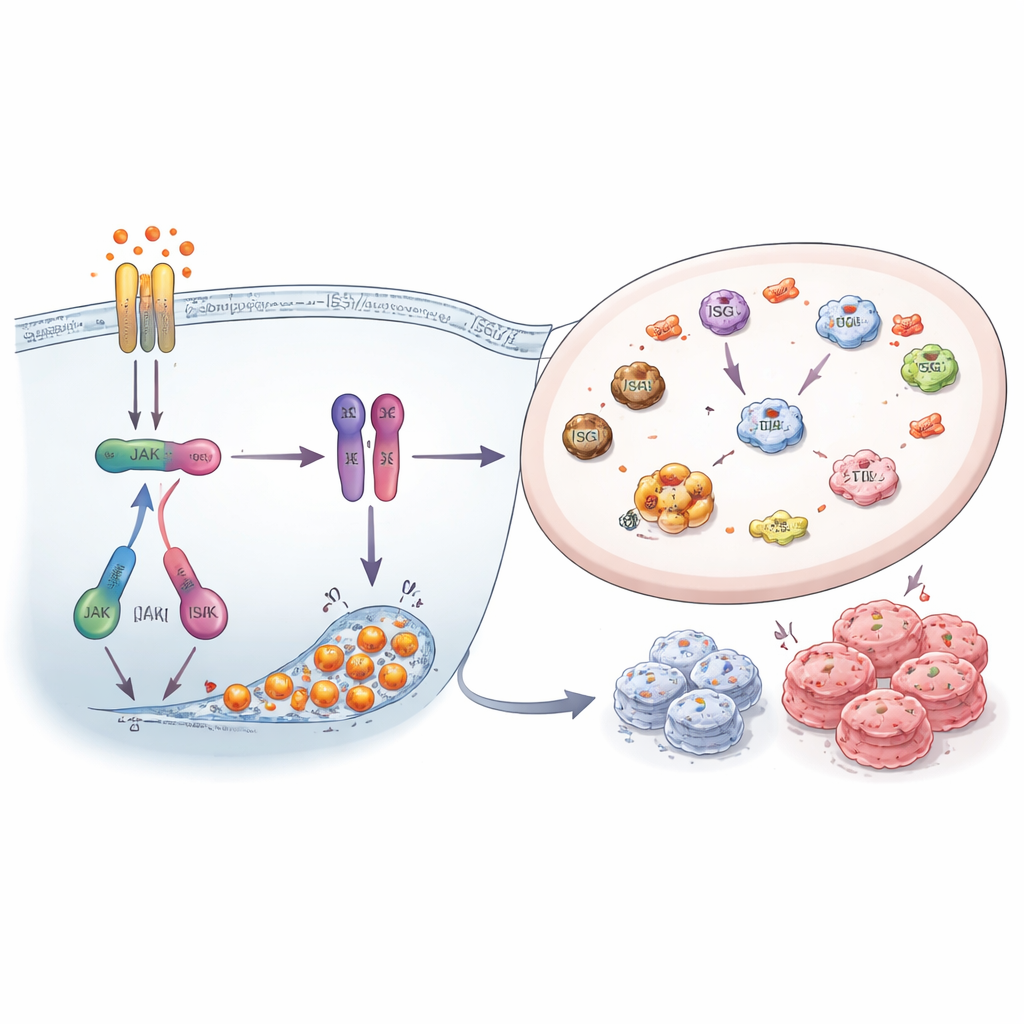
What this means for patients and future therapies
To a lay reader, the picture that emerges is that resistant ER+ breast cancers rewire themselves around a shared stress-response circuit, using interferon signals and ISG15 tags as a kind of protective armor. The good news is that this armor exposes new weak spots. Drugs that block the JAK–STAT1–ISG15 pathway, and treatment plans that sequence FOXM1 inhibitors after CDK4/6 drugs (or vice versa), may help outmaneuver resistance rather than being defeated by it. While these insights still need to be tested in clinical trials, they offer a clearer roadmap for turning an all-too-common treatment dead end into a new opportunity for control.
Citation: Ziegler, Y., Kumar, S., Saeh, C.M. et al. JAK/STAT1-interferon-ISGylation networks in breast cancer resistance to inhibitors of FOXM1 and CDK4/6. npj Breast Cancer 12, 44 (2026). https://doi.org/10.1038/s41523-026-00911-6
Keywords: ER-positive breast cancer, drug resistance, CDK4/6 inhibitors, FOXM1 inhibitors, interferon signaling