Clear Sky Science · en
Restoration of ethanol-induced Bifidobacterium pseudocatenulatum depletion ameliorates alcohol-associated liver disease
Why Your Gut Matters When You Drink
Many people know that heavy drinking can damage the liver, but fewer realize that the story begins in the gut. This study explores how changes in intestinal bacteria caused by alcohol may drive liver disease—and how a specific “good” bacterium, Bifidobacterium pseudocatenulatum, could help turn the tide. The findings hint at future probiotic treatments that might one day support people at risk of alcohol‑associated liver damage.
A Link Between Drinking, Gut Germs, and Liver Harm
Alcohol‑associated liver disease, which ranges from fatty liver to cirrhosis, kills millions worldwide each year. The researchers started by examining stool and blood samples from 127 men: healthy volunteers, patients with alcohol‑related liver disease, and patients with hepatitis B–related liver problems. Using genetic fingerprinting of gut microbes, they found that people with alcohol‑related liver disease had a disturbed gut ecosystem, with fewer helpful bacteria and more potentially harmful ones. One of the most depleted groups was Bifidobacterium, a family of bacteria often found in probiotic foods and supplements.
Finding a Helpful Gut Ally
From the stools of healthy donors, the team isolated three Bifidobacterium strains and tested them in mice fed an alcohol‑containing liquid diet that mimics human drinking patterns. Only one strain—Bifidobacterium pseudocatenulatum—strongly reduced two key blood markers of liver injury and lowered fat buildup in the liver. Genetic analysis of this strain showed that it carried many genes involved in processing fats and carbohydrates, suggesting it might reshape metabolism in helpful ways. This made B. pseudocatenulatum the focus of a deeper investigation.
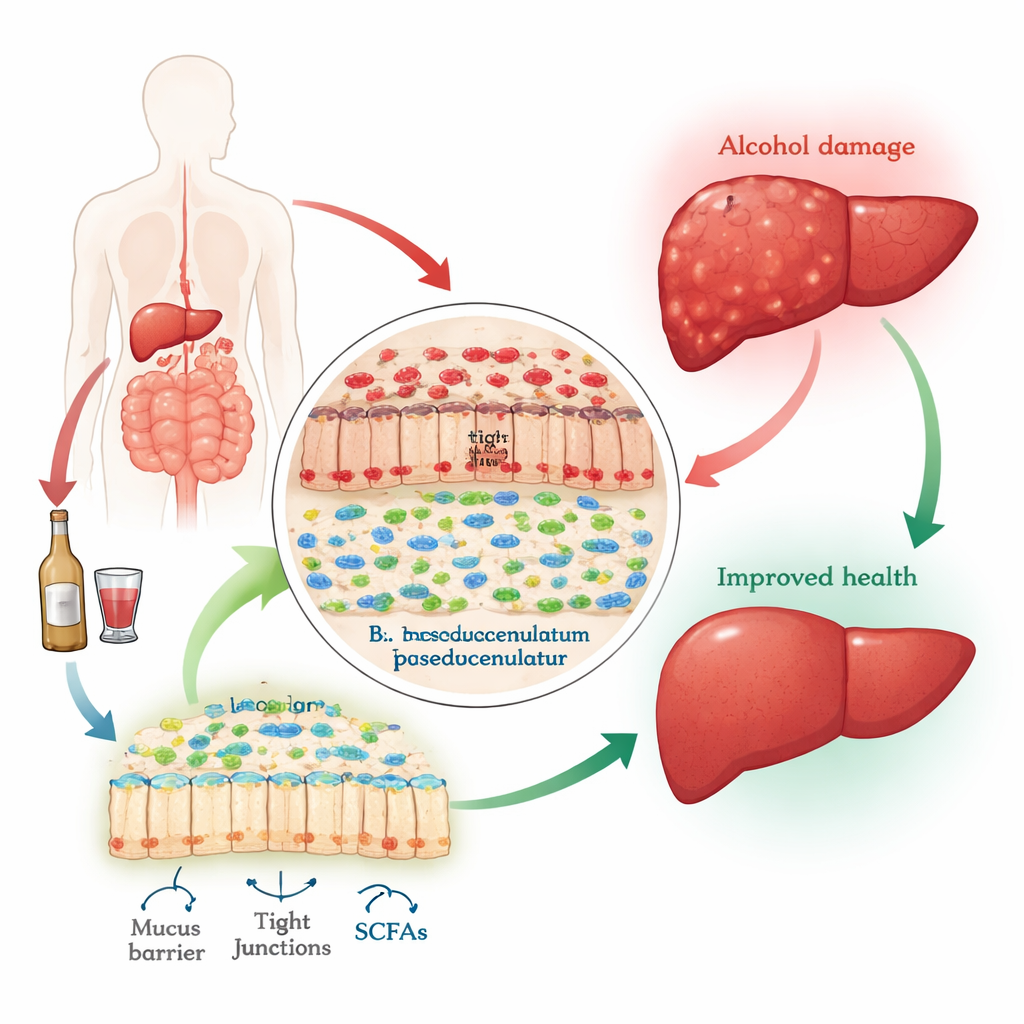
Protecting the Liver in an Alcohol‑Fed Mouse
Mice were fed an alcohol‑rich diet for eight weeks, with some also receiving daily doses of B. pseudocatenulatum by mouth. In animals given alcohol alone, the liver became enlarged, pale, and packed with fat droplets, and blood tests showed high levels of enzymes that leak from damaged liver cells. Their intestines also showed thinning of the mucus layer, frayed surface cells, and leaky junctions between cells, allowing bacterial products to seep into the bloodstream and stoke inflammation. In contrast, mice that received the probiotic had smaller livers, less fat accumulation, and lower liver enzyme levels. Microscopic exams revealed that their gut lining was more intact, the mucus layer thicker, and the tight junction proteins better preserved.
Rebalancing Gut Communities and Chemical Signals
The probiotic did not simply plug leaks in the gut wall; it also reshaped the gut community and the chemicals it produces. In alcohol‑fed mice, harmful groups such as Escherichia–Shigella and other inflammatory bacteria flourished, while beneficial genera like Bifidobacterium and Blautia shrank. Adding B. pseudocatenulatum reversed many of these shifts, enriching friendly bacteria and trimming back trouble‑makers. When the team measured hundreds of small molecules in the feces, they found that alcohol disrupted pathways for processing sugars, fats, and bile acids. Probiotic treatment nudged these pathways back toward a healthier pattern and boosted short‑chain fatty acids—small fermentation products, such as acetate, propionate, and butyrate, that serve as fuel for gut cells and signaling molecules for the liver and immune system.
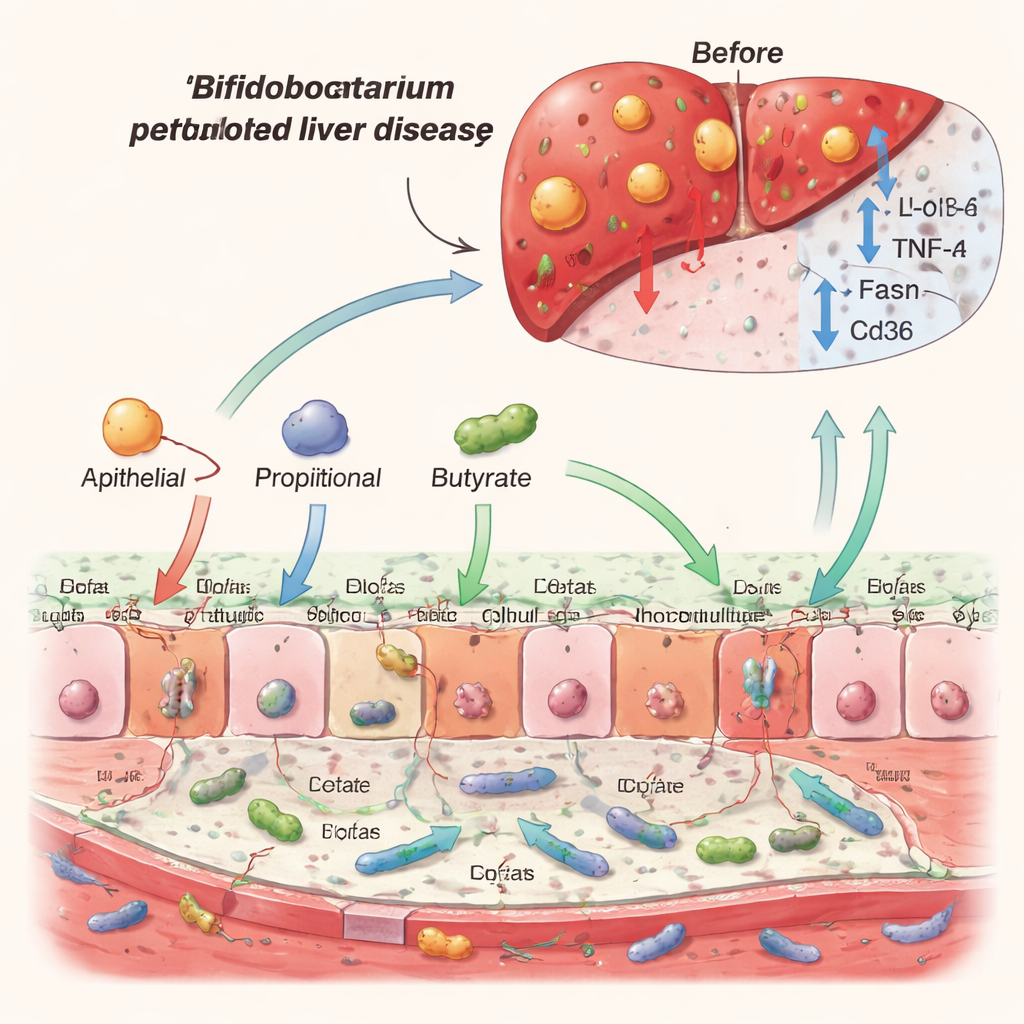
Dialing Down Inflammation and Fat Production
Inside the liver, alcohol ramped up genes involved in making and importing fat, and it increased inflammatory messengers that attract immune cells and can damage tissue over time. Mice given B. pseudocatenulatum showed the opposite trend: genes that drive fat synthesis and uptake were turned down, and many inflammatory signals were reduced. At the same time, receptors that sense bacterial toxins were more carefully regulated, both in the gut and the liver, suggesting that the probiotic helps the body respond more calmly to constant microbial chatter from the intestine. Safety tests showed no obvious side effects in the treated animals, supporting the idea that this human‑derived strain could be suitable for further development.
What This Could Mean for People Who Drink
To a layperson, the takeaway is that heavy drinking appears to injure the liver not only directly but also indirectly, by disturbing the protective community of microbes and the barrier lining the gut. In this mouse study, restoring a single missing ally, Bifidobacterium pseudocatenulatum, helped patch the gut, cool inflammation, and lighten the fat load on the liver. While only rigorous clinical trials can reveal whether this approach will work in people, the work points toward a future in which targeted probiotics may become part of the toolkit for preventing or treating alcohol‑associated liver disease.
Citation: Li, Y., Yang, L., Xu, H. et al. Restoration of ethanol-induced Bifidobacterium pseudocatenulatum depletion ameliorates alcohol-associated liver disease. npj Biofilms Microbiomes 12, 47 (2026). https://doi.org/10.1038/s41522-026-00913-z
Keywords: alcohol-associated liver disease, gut microbiome, Bifidobacterium, probiotics, short-chain fatty acids